Abstract
Children with preschool wheeze regularly attend UK emergency departments. There is no international consensus on any specific personalised management approach. This paper describes the first attempt to co-design patient-centred outcomes with families. Preschool wheezers’ parents participated in semi-structured interviews and focus-group discussions to air their concerns and identify potential additional support. Fifty-seven families participated in these interviews. From these, themes were defined through qualitative content analysis. Parental experience was mapped to the patient pathway and seven important personalised outcomes were described. These can be used to inform a tool which following further validation could potentially support management of children with preschool wheeze and provide an additional patient focused clinical outcome measure in audit and research.
Similar content being viewed by others
Introduction
Chronic respiratory conditions are major causes of morbidity and mortality in childhood. Such children may have impaired physical, emotional, and general well-being. Their illness and associated stressors can have a great impact on their caregivers, especially when recurrent hospitalisations are required1.
Recurrent wheeze in preschool children is one of the most common respiratory conditions. Wheezing disorders in toddlers constitute one-third of the presentations of respiratory disorders in this age group and are associated with increased healthcare costs, loss of time from work in parents and impaired quality of life for the carers and/or the family2,3 The prevalence of preschool wheeze varies between countries. A recently published European study describes the differences in prevalence during the second year of life in nine European countries with UK having the second highest prevalence4.
In the UK, the last published national audit shows that the number of hospital admissions for preschool children with wheeze remained steadily high in the previous decade5 Recently, the first UK study looking at exacerbation rates in a general asthma population between the years 2007 and 2015 showed that the patients with the most frequent exacerbations were the group of children under 5 years old6 In Canada, the annual rate of emergency department visits is 23–42 per 1000 for preschool children with wheeze, compared with less than 15 per 1000 for those aged above six years old7 There is a similar pattern for the rate of hospital admissions.
A recent Australian study shows that nearly a third of children who present at the emergency department with a wheeze attack are discharged within 4 h and more than 40% are discharged within 7 h8, which has been reported in other studies9,10 The brevity of stay highlights that a significant number of preschool wheezers need not have sought clinical review at a secondary care setting. If we can understand why parents often seek hospital advice unnecessarily, more meaningful interventions for these patients can potentially be designed.
Patient-reported outcome measures (PROMs) are tools measuring outcomes that matter to patients. Many have been developed over the past 30 years but few are used routinely in clinical practice. Evidence shows that the systematic use of PROMs leads to better communication and decision making by doctors and patients and improves patient satisfaction and outcomes of care11 However, there are no UK PROMs for preschool children with wheeze, potentially impairing parental communication with doctors and coordination of their child’s care. We also contacted experts in management of preschool wheeze in eight different countries (UK, US, Argentina, Greece, Australia, Italy, Singapore, India) in order to identify whether any PROMs are used routinely in each country for the management of these children. We found that no PROMs have been routinely introduced in these countries either12 There are two instruments attempting to assess the severity of preschool wheeze attacks and the main parental concerns during the episode13,14 Although these instruments demonstrate how families feel during acute attacks, they do not capture the changes in quality of their life over time and are not co-designed with families as would a PROM tool15 Therefore, a PROM would potentially add significantly in the management of these children.
This paper describes the main co-developed personalised outcomes for preschool children with wheeze.
Results
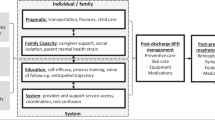
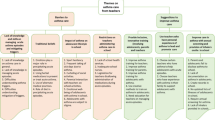
The majority of parents were women (96%) with a mean age of 30.7 years (standard deviation (SD) 4.7). Based on parents’ narratives around their first experience of having a wheezing child, a process map was created to illustrate parents’ journey (Fig. 1)16 Parental emotions were mapped in a chart (Fig. 2) and seven main outcomes were identified through discussions. Notably, while most of the journey engendered a mix of emotions, both positive and negative, parents describe only negative emotions (stress, anger and fear) when they are at home and need to manage their wheezy child.
Process map describing patients’ journey during the first episode of wheeze they recall needing to seek for medical support—the red colour indicates admission with acute wheeze and the green colour indicates discharge—the number of parents who have described each journey are added next to each arrow
Personalised outcomes deriving from thematic analysis are:
a. Sense of reassurance
Parents value significantly having a sense of reassurance. This applies to both cognitive (knowing more) and affective (doctors feel for what they are going through) reassurance17.
Parent: “more knowledge around the condition would provide reassurance”
Parent: “would feel less anxious if the team was more supportive”
b. Less time off work
Parents feel that it is important to have less time off, and less impact on, work.
Parent: “needs time free for work”
Parent: “I need to be able to concentrate at work”
c. Family quality time
Improved family quality time is something that parents feel they miss.
Parent: “I would like to have more relaxing days with the kids”
Parent: need “better family time”
d. Parental mental health well-being
Parents feel they need to maintain their mental-health wellbeing.
Parent: “I can’t stay calm and I feel always stressed”
Parent: “since he started having the wheeze I feel depressed”
e. School readiness
Parents are concerned that they need to have some time to focus on their child’s development.
Parent: “my niece is far more advanced than him”
These outcomes are further described in Table 1 below.
f. Sense of expertise
The need for an improved sense of expertise is highlighted by many parents.
Parent: need for further “knowledge about the disease”
Parent: wanting to know how to navigate the healthcare services, knowing “where to go and what to do” when her child becomes wheezy
g. More coordinated care
The most commonly suggested outcome points to the way healthcare services are designed and has to do with improved coordination of care.
Parent: “I would like one single plan not ten”
Parent: “I would like a plan for his management that doesn’t change all the time”.
Discussion
This is the first study attempting to co-design personalised outcomes in preschool children with recurrent wheeze. These findings will inform the design of a tool that can be used in management of these patients and as another outcome in randomised controlled clinical trials.
A strength of this study is its use of an open survey tool to elicit parental feelings, unlike others who have used preselected criteria14 Although the study population was small, it is one of the largest described compared with similar studies14 Although we made every effort to recruit from varied settings, there should be caution in extrapolating the findings, in particular to tertiary care. Further work is required to design and validate an instrument based on these outcomes which could be subsequently tested in a larger population.
Our study highlighted coordination of care and communication between healthcare professionals as one of the main concerns of families. Suggested management plans often differed significantly between healthcare professionals, leading to inconsistent information being given to parents, potentially leading to poor continuity of care.
Parents highlighted the importance of health literacy, in particular how they can assess severity during an attack, and the navigation of healthcare services. It is important for parents to know when to escalate their child’s management and to choose the appropriate healthcare setting. Knowledge reduces stress and anxiety levels. It is especially challenging for immigrant parents to know where to turn for help when concerned enough to leave home. Although the increasing use of digital health aims to educate users, including non-native residents, around healthcare services18, many families remain confused. Also, parents value significantly having a sense of reassurance. This applies to both cognitive (knowing more) and affective (doctors feel for what they are going through) reassurance17.
Finally, quality family time and parents’ working schedules are severely affected by ill health in children. Measuring this aspect as a specific outcome will be helpful.
We have determined seven outcomes which may be important to parents of children with preschool wheeze. The next steps are to develop a formal score and test its sensitivity to intervention.
Methods
Parents of preschool children with a history of at least one episode of recurrent wheeze were recruited in three different settings—emergency department, children’s ambulatory unit of Imperial College NHS Trust and general practices in the surrounding area that are part of Connecting Care for Children model (https://www.cc4c.imperial.nhs.uk/). The recruitment was either during opportunistic visits of the research team members to the emergency department and the children’s ambulatory unit or by general practitioner led identification, information and recruitment. Similar numbers of participants were interviewed at an emergency department (n = 24) and at a primary care or “supporting primary care” setting (n = 33). It is of note that 10 out of the 24 parents interviewed at an emergency department declared that their children are followed up in tertiary care clinics because of severe episodes of recurrent wheeze. Therefore parents of children with mild, moderate and severe forms of the condition are represented.
Parents, who consented to being contacted again, were invited to participate in two workshops held in a focus group format. The first explored (n = 11) further personalised outcomes, and the second (n = 9) refined and finally agreed the outcomes. All workshop participants had been interviewed by members of the team; eight out of the nine participants in the second workshop had participated in the first workshop. It is of note that both in semi-structured interviews and in focus group discussions parents were not given a list of questions describing their emotions, which we note was done in previous study published aiming to develop a relevant tool14 Feelings were not specifically named, but we aimed to highlight these by analysis of the in-depth discussions.
Main demographic data were analysed quantitatively. Each question was used to organise acquired data into categories (codes). Focus group discussions were not further segmented for analysis. All coding was carried out by two researchers independently (EK and HM) and coding consistency was compared and cross-checked for accuracy until a consensus was reached. Themes were identified from the coding. Inductive thematic saturation was reached. Themes were presented using continuous text with direct quotations to illustrate results. In addition, absolute frequencies and descriptive group comparisons were performed. NVivo 11.0 software was used for the building of the coding and the segmentation of units of coding but not for the presentation of the data.
Reporting Summary
Further information on experimental design is available in the Nature Research Reporting Summary linked to this article.
Data availability
The authors declare that [the/all other] data supporting the findings of this study are available within the paper [and its supplementary information files].
References
Peterson-Carmichael, S. L. & Cheifetz, I. M. The chronically critically ill patient: pediatric considerations. Respir. Care 57, 993–1002 (2012). Discussion 1002–1003.
Kuehni, C. E., Strippoli, M. P., Low, N., Brooke, A. M. & Silverman, M. Wheeze and asthma prevalence and related health-service use in white and south Asian pre-school children in the United Kingdom. Clin. Exp. Allergy 37, 1738–1746 (2007).
Stevens, C. A., Turner, D., Kuehni, C. E., Couriel, J. M. & Silverman, M. The economic impact of preschool asthma and wheeze. Eur. Respir. J. 21, 1000–1006 (2003).
Selby, A. et al. Prevalence estimates and risk factors for early childhood wheeze across Europe: the EuroPrevall birth cohort. Thorax 73, 1049–1061 (2018).
Davies, G., Paton, J. Y., Beaton, S. J., Young, D. & Lenney, W. Children admitted with acute wheeze/asthma during November 1998–2005: a national UK audit. Arch. Dis. Child. 93, 952–958 (2008).
Bloom, C. I. et al. Exacerbation risk and characterisation of the UK’s asthma population from infants to old age. Thorax 73, 313–320 (2018).
Ducharme, F. M., Tse, S. M. & Chauhan, B. Diagnosis, management, and prognosis of preschool wheeze. Lancet 383, 1593–1604 (2014).
Foster, S. J., Cooper, M. N., Oosterhof, S. & Borland, M. L. Oral prednisolone in preschool children with virus-associated wheeze: a prospective, randomised, double-blind, placebo-controlled trial. Lancet Respir. Med. 6, 97–106 (2018).
Abaya, R. et al. Improving efficiency of pediatric emergency asthma treatment by using metered dose inhaler. J. Asthma 1–8 (2018).
Staggs, L. et al. Evaluating the length of stay and value of time in a pediatric emergency department with two models by comparing two different albuterol delivery systems. J. Med. Econ. 15, 704–711 (2012).
Greenhalgh, J. & Meadows, K. The effectiveness of the use of patient-based measures of health in routine practice in improving the process and outcomes of patient care: a literature review. J. Eval. Clin. Pract. 5, 401–416 (1999).
Makrinioti, H., Klaber, R. & Watson, M. Around the world: preschool wheeze. Lancet Respir. Med. 5, 688–689 (2017).
Ducharme, F. M. et al. Asthma Flare-up Diary for Young Children to monitor the severity of exacerbations. J. Allergy Clin. Immunol. 137, 744–749 e746 (2016).
Jensen, M. E. et al. Caregiver’s functional status during a young child’s asthma exacerbation: a validated instrument. J. Allergy Clin. Immunol. 137, 782–788 e786 (2016).
Reeve, B. B. et al. ISOQOL recommends minimum standards for patient-reported outcome measures used in patient-centered outcomes and comparative effectiveness research. Qual. Life. Res. 22, 1889–1905 (2013).
Trebble, T. M., Hansi, N., Hydes, T., Smith, M. A. & Baker, M. Process mapping the patient journey: an introduction. BMJ 341, c4078 (2010).
Pincus, T. et al. Cognitive and affective reassurance and patient outcomes in primary care: a systematic review. Pain 154, 2407–2416 (2013).
Rohan, A. J., Fullerton, J., Escallier, L. A. & Pati, S. Creating a novel online digital badge-awarding program in patient navigation to address healthcare access. J. Nurses Prof. Dev. 33, 106–112 (2017).
Acknowledgements
This article presents independent research commissioned by the National Institute for Health Research (NIHR) under the Collaborations for Leadership in Applied Health Research and Care (CLAHRC) programme for North West London. The views expressed in this publication are those of the author(s) and not necessarily those of the NHS, the NIHR or the Department of Health. Makrinioti is a recipient of an Imperial Charity project grant.
Author information
Authors and Affiliations
Contributions
M. H. was leading the conduct of the study, the data collection, the analysis and the manuscript composition. K. E. assisted the data collection and the qualitative content analysis. H. B. assisted the qualitative content analysis. C. M. and K. R. assisted the supervision of data collection and the revision of the manuscript. B. M. assisted the supervision of data collection and the revision of the manuscript. G. C. guided the data collection and the qualitative analysis. W. M. co-designed the study, supervised the study’s progress and reviewed the manuscript. B. A. supervised the study, had the overview of its direction and reviewed the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Heidi, M., Emily, K., Benjamin, H. et al. Patient reported outcomes for preschool children with recurrent wheeze. npj Prim. Care Respir. Med. 29, 7 (2019). https://doi.org/10.1038/s41533-019-0120-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41533-019-0120-3