Abstract
Glial fibrillary acidic protein (GFAP) has been suggested as a biomarker for reactive astrogliosis. We measured the levels of plasma GFAP by Simoa in 60 patients with PD with normal cognition, 63 with mild cognitive impairment (PD-MCI), 24 with dementia (PDD) and 15 healthy controls. A subgroup of patients with PD-MCI (n = 31) was followed up for 4.1 ± 2.3 years. Compared with healthy controls, plasma GFAP levels were elevated in patients with PDD (adjusted P < 0.001) and PD-MCI (adjusted P = 0.013) and were negatively correlated with the Mini Mental State Examination (MMSE) score in PD participants. Plasma GFAP predicted MCI-to-dementia conversion with an AUC of 0.90, higher than NfL, Tau and pTau181. Our results support that plasma GFAP has potential value for distinguishing patients with PDD, and predicting MCI-to-dementia conversion in PD.
Similar content being viewed by others
Introduction
Parkinson’s disease (PD) is a neurodegenerative disease with complex molecular and clinical characteristics1. Cognitive impairment, including mild cognitive impairment (PD-MCI) and dementia (PDD), is a prevalent non-motor symptom of PD1,2.
Growing evidence indicates that neuroinflammatory processes such as reactive astrogliosis contribute to PD development3,4. Glial fibrillary acidic protein (GFAP) is an intermediate filament protein that is primarily expressed in astrocytes of the central nervous system. When the nervous system is injured, astrocytes rapidly release GFAP into the bloodstream5. A few studies have examined serum GFAP in PD, finding elevated serum levels of GFAP compared to controls6,7. However, there is a lack of studies investigating GFAP in PD from a cognitive perspective. Whether GFAP can be used as a potential biomarker to predict cognitive progression of PD is unknown. Here, we evaluated plasma GFAP levels to investigate differences in patients with PD with normal cognition (PD-NC), PD-MCI and PDD. We also investigated possible correlations between levels of GFAP and cognitive scores, as well as progression to dementia. Furthermore, we compared levels of plasma GFAP with three other neuronal blood markers, that is, neurofilament light chain (NfL), Tau and pTau181.
Results
The demographic information of the study participants is presented in Table 1, and detailed observations of cognitive performance are reported in Supplementary Table 1. Increased Movement Disorders Society Unified Parkinson’s Disease Rating Scale part III (MDS UPDRS-III) scores were observed in the PDD group compared to the PD-NC group (adjusted P < 0.05). As expected, performance on the Mini Mental State Examination (MMSE) was worse in the PDD group as compared to age-matched healthy control subjects (HCs), PD-NC and PD-MCI groups (all adjusted P < 0.001).
Age was significantly correlated with plasma GFAP (r = 0.158, P = 0.044) in all participants. We observed no significant correlation between plasma GFAP and disease duration (r = 0.019, P = 0.816), Hoehn and Yahr (H&Y) stage (r = 0.160, P = 0.063), or levodopa equivalent dose (LED, r = 0.049, P = 0.558) in all participants. Furthermore, in all participants, sex did not significantly affect plasma GFAP levels (Mann–Whitney U = 2899, P = 0.278). For these reasons, we included age as a covariate in the statistical comparison of the study groups.
After adjusting for age, we found that plasma GFAP was significantly elevated in the PDD group compared to the HCs (adjusted P < 0.001), PD-NC (adjusted P < 0.001) and PD-MCI (adjusted P < 0.001) groups. Moreover, plasma GFAP was significantly increased in the PD-MCI group compared to the HCs (adjusted P = 0.009, Fig. 1a).
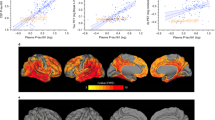
a Plasma GFAP levels in healthy controls (n = 15) and patients with PD-NC (n = 60), PD-MCI (n = 63) and PDD (n = 24). Groups were compared by a generalized linear model after adjusting for age. Boxes show the median and IQR, and whiskers are the minimum and maximum. Dots are single values. b Correlation analysis of plasma GFAP with plasma NfL, Tau and pTau181 using Spearman’s partial correlation including age as a covariate. The correlation coefficient r is given in the heat map. c Baseline levels of plasma GFAP, NfL, Tau and pTau181 in PD patients with MCI stable (n = 21) and conversion to dementia (converter, n = 10) during the whole follow-up period. Groups were compared by the Mann–Whitney U test. Boxes show the median and IQR, and whiskers are the minimum and maximum. Dots are single values. d Receiver operating characteristic (ROC) curve analysis indexed the efficiency of plasma GFAP for the differential diagnosis of Parkinson’s disease subgroups stratified according to cognitive status. e ROC curve analysis for baseline levels of plasma GFAP, NfL, Tau, and pTau181 to predict MCI-to-dementia conversion during the next 4.1 ± 2.3 years. *p < 0.05, **p < 0.01, ***p < 0.001. HCs healthy controls, PD-NC Parkinson’s disease with normal cognition, PD-MCI Parkinson’s disease with mild cognitive impairment, PDD Parkinson’s disease dementia, AUC area under the curve.
To evaluate whether plasma GFAP was correlated with performance on the MMSE, we used Spearman’s partial correlation including age as a covariate. A significant correlation between plasma GFAP and MMSE score was detected in all participants with PD (r = −0.584, P < 0.001). Furthermore, significant correlations between plasma GFAP and MMSE scores were detected in the PD-MCI (r = −0.313, P = 0.013) and PDD groups (r = −0.506, P = 0.014), but not observed in the PD-NC group (r = −0.128, P = 0.335). The correlations between GFAP and other neuropsychological tests are shown in Supplementary Table 2.
Next, we studied the relationship between plasma GFAP and three other plasma biomarkers, NfL, Tau and pTau181. Plasma GFAP showed a significant moderate correlation with plasma NfL (r = 0.585, P < 0.001) and pTau181 (r = 0.413, P < 0.001) in all PD participants (Fig. 1b).
A subgroup of patients with PD-MCI (n = 31) was clinically followed up for 4.1 ± 2.3 years. Twenty-one PD subjects showed stable MCI during the whole follow-up period whereas 10 PD patients with MCI progressed to dementia (converter). Plasma GFAP at baseline was significantly higher in converters than in patients with stable MCI (P < 0.01). None of the other three biomarkers (NfL, Tau and pTau181) showed significant differences between stable MCI and converters (Supplementary Table 3 and Fig. 1c).
ROC curve analysis revealed that plasma GFAP allowed a reliable differential diagnosis between PDD and PD-NC (AUC = 0.79), PD-MCI (AUC = 0.74) or PD with non-dementia (including both PD-NC and PD-MCI, AUC = 0.77) (Fig. 1d). Plasma GFAP was unsuitable to discriminate PD-MCI and PD-NC.
Furthermore, we investigated the predictive value of plasma GFAP, NfL, Tau and pTau181 for MCI to dementia conversion in PD. Plasma GFAP at baseline had a high accuracy for separating patients with stable MCI and MCI to dementia conversion (AUC = 0.90) after an average follow-up of 4.1 ± 2.3 years, with a sensitivity of 90% and specificity of 81% at an optimal cut-off of 100.2 pg/mL. The other three biomarkers showed lower performance in discriminating the two groups of patients (Fig. 1e).
Discussion
In the present study, we found increased plasma GFAP levels in PD patients with dementia as well as MCI, compared to controls. Plasma GFAP showed a significantly negative correlation with the MMSE score in the PD participants. Furthermore, we suggest that plasma GFAP may be a potential biomarker for predicting the progression of MCI to dementia in PD.
Previous studies have demonstrated the presence of reactive astrogliosis in PD progression, but their role in the pathophysiology is not fully understood3,4. GFAP is a major structural component of fibrillary astrocytes and has proven to be one of the most common reactive astrocytic markers5. In this study, we found that levels of plasma GFAP increased in patients with PDD, and the increase was also observed in patients with PD-MCI. Plasma GFAP was negatively correlated with MMSE scores in the PDD and PD-MCI groups; however, no significant correlation was observed in the PD-NC group. Our study might indicate the presence of reactive astrogliosis in the early phase of cognitive impairment in PD.
Importantly, the capacity to predict the timeframe of disease progression is a critical issue in clinical practice and clinical trials. We next investigated whether plasma GFAP could predict more rapid cognitive decline in PD. In the subgroup of patients with PD-MCI who were clinically followed up for an average of 4.1 years, baseline plasma GFAP was significantly higher in patients who developed dementia than in those who remained stable with MCI. Meanwhile, the other three biomarkers, NfL, Tau and pTau181, which are related to neuronal injury and neurodegeneration, did not differ significantly between stable MCI and converters. With an AUC of 0.90, plasma GFAP levels separate patients with stable MCI and converters. Although the results need to be confirmed with a larger sample size, it is worth noting that plasma GFAP measurement may be useful as a marker for predicting the transition from MCI to dementia in PD. This might be helpful for patient classification in clinical trials or as a follow-up marker.
This study has several limitations. First, our study used clinical diagnosis in the absence of neuropathological confirmation. However, patients were well characterized, and most of the patients were followed over time to acquire as accurate a clinical diagnosis as possible. Second, the number of participants in the study is limited. The results therefore need to be reproduced in larger cohorts. Finally, MMSE scores exhibit ceiling/floor effects. More sensitive scales of global cognitive abilities would need to be applied to further investigate the relationship of GFAP with cognitive function.
In conclusion, we demonstrate that the levels of plasma GFAP are elevated in PD patients with cognitive impairment, but not in PD patients with normal cognition. We suggest that plasma GFAP might have prognostic value for predicting MCI-to-dementia conversion in PD.
Methods
Participants and controls
The study participants were recruited from the Movement Disorders Clinics at Huashan Hospital, Fudan University, between April 2013 and October 2021. Patients with PD-NC (n = 60), PD-MCI (n = 63), PDD (n = 24), and HCs (n = 15) were enrolled. PD subjects were diagnosed according to the UK Brain Bank criteria8. All HCs had a negative history of neurological or psychiatric disorders. A subgroup of patients with PD-MCI (n = 31) was clinically followed up for 4.1 ± 2.3 years (mean ± SD) after sample collection (baseline), and the details are presented in Supplementary Fig. 1 and Supplementary Table 4. The clinical and neuropsychological features were assessed annually. Ethics approval for the study was received from the Institutional Review Board at Huashan Hospital (approval numbers: 2011-174-2). All participants provided written informed consent in accordance with the Declaration of Helsinki.
Clinical and neuropsychological assessments
Patients underwent clinical assessment at least 12 h off anti-parkinsonian medications. Disease severity was evaluated using the MDS UPDRS-III and the H&Y scale9. The Beck Depression Inventory (BDI) was performed to evaluate depression10. The dosage of antiparkinsonian drugs was converted into a total daily LED11.
The MMSE was performed to assess global cognitive function12. A full set of neuropsychological tests for five specific cognitive domains were carried out as follows: (1) Symbol Digit Modality Test (SDMT) and Trail Making Test A (TMT-A) for attention and working memory13,14, (2) Trail Making Test B (TMT-B) and Stroop Color-Word Test (CWT) for executive function15,16, (3) Animal Fluency Test (AFT) and Boston Naming Test (BNT) for language16, (4) Auditory Verbal Learning Test (AVLT) and Rey-Osterrieth Complex Figure Test (CFT-delay) for memory17,18, (5) Rey-Osterrieth Complex Figure Test (CFT-copy) and Clock Drawing Test (CDT) for visuospatial function18,19.
PDD was diagnosed according to the MDS criteria20. The MDS Task Force Level 2 was applied for PD-MCI diagnosis21. The PD patients who were excluded from PD-MCI and PDD were defined as PD-NC.
Plasma sample collection and storage
After a 12 h overnight fast, blood samples were collected in the morning in EDTA Vacutainer tubes (BD). EDTA blood were briefly stored on ice and then was centrifuged at 2000 × g for 15 min within 30 min after collection. Plasma supernatant was collected, divided into aliquots (200 µl/tube), and frozen at − 80 °C until further use.
Measurement of GFAP, NfL, Tau, and p-Tau181 in plasma
Plasma EDTA samples were thawed and centrifuged at 10,000 × g for 5 min at room temperature. Plasma GFAP, NfL, and Tau were measured using the HD-X Neurology 4-Plex B Kit, and plasma pTau181 was detected using the HD-X Simoa pTau181 V2 Advantage Kit. These two kits were all 2-step digital immunoassays. Assay calibrants provided in the kit were added in 96-well plates together with samples to make standard curves. Beads were vortex for 30 s immediately before loading reagents (Bead Reagent, Sample Diluent, Detector Reagent, and SBG Reagent). Samples were detected with the Quanterix Simoa HD-X analyzer using the standard 4x Dilution setup, and assay calibrants were run neat in triplicates. The concentration of GFAP, NfL, Tau, and pTau181 in unknown samples is interpolated from corresponding standard curve obtained by logistical regression fittings. GFAP, NfL, and Tau measurements of all patients were performed on the same day, and so did the pTau181 analysis. Samples were randomized, blinded, and measured using a batch of reagents from the same lot. All assays showed good analytical performance. The within-run variations and between-run variations ranged consistently below 15%.
Statistical analysis
Categorical variables, including sex and H&Y stage, were assessed by performing the chi-square test. Demographic parameters between groups were evaluated using one-way ANOVA followed by Bonferroni’s corrected post hoc comparisons (for parametric data) and or Kruskal‒Wallis test followed by Dunn’s corrected post hoc comparisons (for non-parametric data). Correlation between plasma GFAP and demographic information, including age, disease duration, H&Y stage and LED, was performed with Spearman’s correlation analysis. The generalized linear model (GLM) was used to compare the levels of plasma GFAP, NfL, Tau, and pTau181 between groups after adjusting for age. Correlation analysis of plasma GFAP with MMSE score and other biomarkers using Spearman’s partial correlation including age as a covariate. Baseline levels of plasma GFAP, NfL, Tau, and pTau181 in patients with stable MCI and MCI-to-dementia converters were compared by the Mann–Whitney U test. The diagnostic performance of biomarkers was compared using receiver operating characteristic (ROC) curve analysis and cut-offs calculated by maximizing the Youden index. Statistical analysis was performed with IBM SPSS Statistics (version 26.0) and R (version 4.1.2). A p value < 0.05 was regarded as significant.
Reporting summary
Further information on research design is available in the Nature Research Reporting Summary linked to this article.
Data availability
The data used for this work are available from the corresponding authors upon reasonable requests. Restrictions may be applied to sensitive data for privacy preservation.
References
Hely, M. A., Reid, W. G., Adena, M. A., Halliday, G. M. & Morris, J. G. The Sydney multicenter study of Parkinson’s disease: the inevitability of dementia at 20 years. Mov. Disord. 23, 837–844 (2008).
Muslimovic, D., Post, B., Speelman, J. D. & Schmand, B. Cognitive profile of patients with newly diagnosed Parkinson disease. Neurology 65, 1239–1245 (2005).
Croisier, E. & Graeber, M. B. Glial degeneration and reactive gliosis in alpha-synucleinopathies: the emerging concept of primary gliodegeneration. Acta Neuropathol. 112, 517–530 (2006).
Rizor, A., Pajarillo, E., Johnson, J., Aschner, M. & Lee, E. Astrocytic oxidative/nitrosative stress contributes to parkinson’s disease pathogenesis: the dual role of reactive astrocytes. Antioxidants 8, 265(2019).
Liddelow, S. A. & Barres, B. A. Reactive astrocytes: production, function, and therapeutic potential. Immunity 46, 957–967 (2017).
Su, W., Chen, H. B., Li, S. H. & Wu, D. Y. Correlational study of the serum levels of the glial fibrillary acidic protein and neurofilament proteins in Parkinson’s disease patients. Clin. Neurol. Neurosurg. 114, 372–375 (2012).
Oeckl, P. et al. Glial fibrillary acidic protein in serum is increased in Alzheimer’s disease and correlates with cognitive impairment. J. Alzheimers Dis. 67, 481–488 (2019).
Hughes, A. J., Daniel, S. E., Kilford, L. & Lees, A. J. Accuracy of clinical diagnosis of idiopathic Parkinson’s disease: a clinico-pathological study of 100 cases. J. Neurol. Neurosurg. Psychiatry 55, 181–184 (1992).
Goetz, C. G. et al. Movement disorder society-sponsored revision of the unified Parkinson’s Disease Rating Scale (MDS-UPDRS): scale presentation and clinimetric testing results. Mov. Disord. 23, 2129–2170 (2008).
Beck, A. T., Steer, R. A., Ball, R. & Ranieri, W. Comparison of beck depression inventories -IA and -II in psychiatric outpatients. J. Pers. Assess. 67, 588–597 (1996).
Tomlinson, C. L. et al. Systematic review of levodopa dose equivalency reporting in Parkinson’s disease. Mov. Disord. 25, 2649–2653 (2010).
Hoops, S. et al. Validity of the MoCA and MMSE in the detection of MCI and dementia in Parkinson disease. Neurology 73, 1738–1745 (2009).
Sheridan, L. K. et al. Normative Symbol Digit Modalities Test performance in a community-based sample. Arch. Clin. Neuropsychol. 21, 23–28 (2006).
Zhao, Q. et al. The Shape Trail Test: application of a new variant of the Trail making test. PLoS ONE 8, e57333 (2013).
Steinberg, B. A., Bieliauskas, L. A., Smith, G. E. & Ivnik, R. J. Mayo’s older americans normative studies: age- and IQ-adjusted norms for the trail-making test, the stroop test, and MAE controlled oral word association test. Clin. Neuropsychol. 19, 329–377 (2005).
Lucas, J. A. et al. Mayo’s older african americans normative studies: norms for boston naming test, controlled oral word association, category fluency, animal naming, token test, WRAT-3 reading, trail making test, stroop test, and judgment of line orientation. Clin. Neuropsychol. 19, 243–269 (2005).
Guo, Q., Zhao, Q., Chen, M., Ding, D. & Hong, Z. A comparison study of mild cognitive impairment with 3 memory tests among Chinese individuals. Alzheimer Dis. Assoc. Disord. 23, 253–259 (2009).
Caffarra, P., Vezzadini, G., Dieci, F., Zonato, F. & Venneri, A. Rey-Osterrieth complex figure: normative values in an Italian population sample. Neurol. Sci. 22, 443–447 (2002).
Guo, Q., Fu, J., Yuan, J., Zhao, Q. & Hong, Z. A study of validity of a new scoring system of clock drawing test. Chin. J. Neurol. 41, 234–237 (2008).
Dubois, B. et al. Diagnostic procedures for Parkinson’s disease dementia: recommendations from the movement disorder society task force. Mov. Disord. 22, 2314–2324 (2007).
Litvan, I. et al. Diagnostic criteria for mild cognitive impairment in Parkinson’s disease: Movement Disorder Society Task Force guidelines. Mov. Disord. 27, 349–356 (2012).
Acknowledgements
The study was supported by National Health Commission of China (Pro20211231084249000238), Shanghai Municipal Science and Technology Major Project (2018SHZDZX01 and 21S31902200), and National Natural Science Foundation of China (82171421 and 91949118).
Author information
Authors and Affiliations
Contributions
Conceptualization: J.W., J.J.W., and H.Y. Methodology: Y.T., L.H., and S.L. Organization and data acquisition: Y.T., L.H., S.L, T.H., Z.X., Y.F., and X.L. Statistical analysis: Y.T., L.H., and S.L. Writing, original draft: Y.T., L.H., and S.L. Review and Critique: J.W., J.J.W., and H.Y. These co-first authors contributed equally: Y.T., L.H., and S.L.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Tang, Y., Han, L., Li, S. et al. Plasma GFAP in Parkinson’s disease with cognitive impairment and its potential to predict conversion to dementia. npj Parkinsons Dis. 9, 23 (2023). https://doi.org/10.1038/s41531-023-00447-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41531-023-00447-7
This article is cited by
-
Mapping dynamic molecular changes in hippocampal subregions after traumatic brain injury through spatial proteomics
Clinical Proteomics (2024)
-
Plasma GFAP as a prognostic biomarker of motor subtype in early Parkinson’s disease
npj Parkinson's Disease (2024)
-
P-tau217 and other blood biomarkers of dementia: variation with time of day
Translational Psychiatry (2024)
-
Cerebrospinal fluid GFAP is a predictive biomarker for conversion to dementia and Alzheimer’s disease-associated biomarkers alterations among de novo Parkinson’s disease patients: a prospective cohort study
Journal of Neuroinflammation (2023)
-
Associations of Alzheimer's-related plasma biomarkers with cognitive decline in Parkinson's disease
Journal of Neurology (2023)