Abstract
Non-motor symptoms (NMS) are common among patients with Parkinson’s disease and reduce patients’ quality of life (QOL). However, there remain considerable unmet needs for NMS management. Three monoamine oxidase B inhibitors (MAO-BIs), selegiline, rasagiline, and safinamide, have become commercially available in many countries. Although an increasing number of studies have reported potential beneficial effects of MAO-BIs on QOL and NMS, there has been no consensus. Thus, the primary objective of this study was to provide an up-to-date systematic review of the QOL and NMS outcomes from the available clinical studies of MAO-BIs. We conducted a literature search using the PubMed, Scopus, and Cochrane Library databases in November 2021. We identified 60 publications relevant to this topic. Overall, rasagiline and safinamide had more published evidence on QOL and NMS changes compared with selegiline. This was likely impacted by selegiline being introduced many years prior to the field embarking on the study of NMS. The impact of MAO-BIs on QOL was inconsistent across studies, and this was unlikely to be clinically meaningful. MAO-BIs may potentially improve depression, sleep disturbances, and pain. In contrast, cognitive and olfactory dysfunctions are likely unresponsive to MAO-BIs. Given the paucity of evidence and controlled, long-term studies, the effects of MAO-BIs on fatigue, autonomic dysfunctions, apathy, and ICD remain unclear. The effects of MAO-BIs on static and fluctuating NMS have never been investigated systematically. More high-quality studies will be needed and should enable clinicians to provide personalized medicine based on a non-motor symptom profile.
Similar content being viewed by others
Introduction
Three monoamine oxidase B inhibitors (MAO-BIs) are now commercially available in many countries for the management of motor symptoms in patients with Parkinson’s disease (PD). Selegiline and rasagiline are irreversible MAO-BIs, while safinamide is a reversible MAO-BI1. These MAO-BIs possess distinct pharmacological profiles (i.e., potency, MAO-B/MAO-A selectivity, and pharmacokinetics). In addition, safinamide modulates voltage-sensitive sodium and calcium channels activity and reduces glutamate release2,3.
The results of large clinical trials have been reported since the 1990s for selegiline, since the 2000s for rasagiline, and since the 2010s for safinamide. Notably, selegiline was largely studied before the field embarked on defining non-motor symptoms (NMS) of PD and developing specific and applicable scales. Recognition of NMS has also evolved over recent years4,5. Many double-blind, placebo-controlled randomized controlled studies (RCTs) revealed the beneficial effects of MAO-BIs on motor symptoms and wearing-off compared with placebo1,6,7. These findings are corroborated by meta-analyses8,9,10. The superiority of one MAO-BI over others remains undetermined because there have been no high-quality direct comparative trials among the MAO-BIs.
NMS of PD include depression, anxiety, sleep disturbances, fatigue, pain, and cognitive and autonomic dysfunctions, and underpin the entire course from the prodromal to late stage5,11. Past studies revealed that NMS were more relevant than motor symptoms in quality of life (QOL)12,13. A review on level 1 evidence for treatment of NMS by the Movement Disorders Society was published in 2019 and suggested that there remain considerable unmet needs for NMS management5. Although an increasing number of MAO-BI studies have reported QOL or NMS outcomes, to the best of our knowledge, no reviews have systematically summarized those results. Thus, this systematic review aimed (1) to summarize QOL and NMS outcomes from clinical studies of MAO-BIs, (2) to guide clinicians to select MAO-BIs based on a patient’s symptom profile, and (3) to facilitate future investigations on these issues.
Results
Literature search
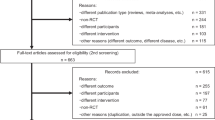
The systematic literature search revealed 1850 records (Fig. 1). By performing duplicate removal, title/abstract screening, full-text assessments, and hand searches, we identified 60 clinical studies which met the eligibility criteria. Most studies enrolled either early PD patients or advanced PD patients experiencing wearing-off, whereas a minority of studies focused on specific populations: patients with sleep disturbances (three studies)14,15,16, depression (two studies)17,18, mild cognitive impairment (MCI) (two studies)19,20, freezing of gait (two studies)21,22, fatigue (one study)23, urinary symptoms (one study)24, high non-motor burden (one study)25, or RBD (one study)26. There are only five double-blind, placebo-controlled RCTs that investigated non-motor outcomes as the primary outcomes (rasagiline for MCI19,20, rasagiline for depression17, rasagiline for fatigue23, and rasagiline for sleep disturbances)14. The remaining studies are RCTs reporting QOL or non-motor results as the secondary outcomes or open-label studies. In the following paragraphs, QOL and NMS outcomes in the literature will be systematically summarized along with Tables 1–7.
Quality of life (Table 1)
The Parkinson’s Disease Questionnaire-39 (PDQ-39) was most commonly used to estimate the changes in QOL after MAO-BI administration27. Eight double-blind, placebo-controlled RCTs reported the effects of rasagiline on QOL based on PDQ-39: three RCTs for patients with early PD28,29,30, two for those with advanced PD31,32, one for those with moderate depression17, one for those with moderate to severe fatigue23, and one for those with sleep disturbances14. Of these studies, only two studies reported significant benefits of rasagiline on QOL at 12–26 weeks (one RCT on advanced PD patients and another RCT for those with moderate to severe fatigue)23,31. Based on the results from the RCTs, effect sizes for rasagiline 1 mg and 0.5 mg were trivial to small (0.05–0.27) and trivial (0.03), respectively. Two Chinese RCTs (one for early PD and one for advanced PD) found significant benefits of rasagiline on QOL based on the EuroQol 5 dimensions (EQ-5D) despite the non-significant results based on the PDQ-3930,32. Two old RCTs evaluated QOL outcomes based on the PDQUALIF scale33,34; significant improvement in the PDQUALIF scale was observed not in early PD patients but in advanced PD patients. In addition, open-label studies reported significant35 or non-significant21,36 benefits of rasagiline based on the PDQ-39.
All the studies of safinamide enrolled advanced PD patients37,38,39,40,41,42,43,44,45,46 except for one study for those with high non-motor burden (defined as the NMS Scale (NMSS) ≥ 40)25. RCTs and open-label studies using safinamide 100 mg reported positive or negative QOL outcomes with safinamide25,37,38,39,40,42,43,45,46, whereas all the studies using safinamide 50 mg reported negative outcomes37,39,40,44. Based on the PDQ-39 outcomes from the RCTs, effect sizes for safinamide 100 mg and 50 mg were small (0.22–0.23) and trivial (0.11–0.15), respectively.
Collectively, a minority of the RCTs (rasagiline or safinamide vs. placebo) for advanced PD patients reported statistically significant QOL improvement. There have been no selegiline studies reporting QOL outcomes. The clinical impact of the QOL changes will be discussed later.
Depression and anxiety (Table 2)
The ACCORDO study, a multicenter, double-blind, placebo-controlled RCT, enrolled non-demented PD patients with moderately severe depressive symptoms (Beck Depression Inventory, BDI ≥ 15)17. Compared with placebo, rasagiline 1 mg led to a significantly larger reduction in the BDI scores at 4 weeks (effect size, 1.01) without a significant between-group difference at 12 weeks. Another multicenter, double-blind, placebo-controlled RCT enrolled 30 PD patients with moderate to severe fatigue23. In parallel with fatigue improvement, rasagiline 1 mg showed a significantly greater reduction of the BDI scores than placebo (5.5 vs. 0.5 points, P = 0.018). In contrast, significant improvement in anxiety was not observed based on the State-Trait Anxiety Inventory. Significant benefits of rasagiline on depressive symptoms over placebo were not observed in RCTs either for early PD patients or those with MCI19,34,47. Seven studies assessed the impact on anxiety and depressive symptoms according to the PDQ-39 emotional well-being subscore17,21,29,30,31,32,36; a minority of studies for either early or advanced PD patients reported significant benefits of rasagiline29,31.
In a multicenter, double-blind, placebo-controlled RCT38 and two open-label prospective studies43,44, safinamide 100 mg for advanced PD patients did not significantly ameliorate depression at 6 months. However, in the Study 016 and its extension study (Study 018), significant benefits on the Hamilton Depression Scale (HAMD) and PDQ-39 emotional well-being subscore over placebo were observed with safinamide 100 mg but not with the 50 mg dose37,39. Furthermore, a post hoc analysis of these two studies confirmed the beneficial effects of safinamide 100 mg on depression48. Interestingly, compared with the placebo group, significantly fewer patients in the safinamide group experienced depression as adverse events during the 2-year follow-up48. Also, open-label studies on patients with either depressive symptoms18 or high non-motor burden25 reported prominent improvement in depression with safinamide based on the HAMD or BDI-II, respectively. The Study 016, its post hoc analysis, and an open-label study observed significant improvement in the PDQ-39 emotional well-being subscore37,48. However, none of the two open-label prospective studies found significant benefits of safinamide on anxiety43,44,45.
Five double-blind, placebo-controlled RCTs for early PD patients reported the effects of selegiline on depressive symptoms using either the HAMD or BDI. Two small RCTs reported negative results49,50, whereas three large RCTs suggested a positive impact of selegiline 10 mg on depressive symptoms with trivial to moderate effect sizes (0.10 and 0.67)51,52,53.
Taken together, rasagiline, safinamide, and selegiline may potentially improve depressive symptoms. In contrast, no studies demonstrated significant benefits of MAO-BIs on anxiety.
Sleep disturbances (Table 3)
Two large multicenter, double-blind, placebo-controlled RCTs for early PD patients reported non-significant effects of rasagiline 1 mg on sleep disturbances at 18–26 weeks based on the PDQUALIF sleep subscore or Scales for Outcomes in PD (SCOPA) daytime sleepiness score28,54. Similarly, one small multicenter, double-blind, placebo-controlled RCT for PD patients with moderate to severe fatigue demonstrated non-significant effects of rasagiline 1 mg on sleep disturbances based on the Parkinson’s Disease Sleep Scale (PDSS) at 12 weeks23. One single-center, double-blind, placebo-controlled RCT enrolled 20 PD patients with sleep disturbances14. Rasagiline 1 mg led to significantly better sleep maintenance as assessed by polysomnography (effect size, 0.71), with significantly decreased wake time after sleep onset, number of arousals, and percentage of light sleep. Although daytime sleepiness, as measured by the Epworth Sleepiness Scale (ESS), improved significantly with rasagiline (effect size, 0.19), there was no significant change in the PDSS-2. The authors found no correlations of polysomnographic sleep parameters or PDSS-2 score with changes in motor function14. Open-label studies reported positive15,55,56 or non-significant57 effects of rasagiline on sleep disturbances.
Six open-label studies have reported the impact of safinamide on sleep disturbances25,26,43,44,45,57. Most studies employed the PDSS-2 and ESS; however, the outcomes were inconsistent. An open-label cross-over study enrolled 30 PD patients with RBD26. Interestingly, safinamide 50 mg alleviated RBD as assessed by polysomnography and questionnaires at 3 months. This study is the only one investigating the effects of MAO-BIs on RBD.
In a large multicenter, double-blind, placebo-controlled RCT for advanced PD patients, orally disintegrating selegiline 1.25–2.5 mg did not prolong asleep time based on patient diaries58. A single-center, open-label, retrospective study analyzed the effects of selegiline 10 mg on excessive daytime sleepiness at 3 months16. The authors reported significant alleviation of excessive daytime sleepiness based on the ESS with a large effect size (1.21). This benefit was accompanied by improved self-perceived quality of sleep. In a single-center, open-label, prospective study, switching from selegiline 7.5 mg to rasagiline 1 mg led to an improvement in sleep disturbances based on the PDSS15. However, the results should be cautiously interpreted because of the potential effect of patients’ expectations of treatment benefits.
In summary, no RCTs showed significant benefits of MAO-BIs based on the sleep-specific rating scales. However, one RCT using polysomnography and some open-label studies reported positive effects of MAO-BIs on sleep disturbances.
Pain (Table 4)
All the rasagiline studies (6 large RCTs and 1 small open-label study) reported pain outcomes based on the PDQ-39 bodily discomfort subscore17,21,29,30,31,32,36. The two large RCTs for advanced PD patients showed significant benefits of rasagiline 1 mg on pain at 16–26 weeks (effect size, incalculable)31,32. Alleviation of pain with rasagiline 0.5 mg was numerically smaller and did not reach statistical significance31. Two large RCTs for early PD patients did not find significant benefits of rasagiline 1 mg on pain29,30.
In a large double-blind, placebo-controlled RCT, advanced PD patients were randomized to safinamide 100 mg, 50 mg, or placebo for 24 weeks37. Compared with placebo, only patients taking safinamide 100 mg experienced significant amelioration of pain based on the PDQ-39 bodily discomfort subscore. Similar results were observed in another large RCT for advanced PD patients, although the outcomes did not reach statistical significance59. Furthermore, small open-label studies and post hoc analyses of large RCTs for advanced PD patients support the efficacy of safinamide 100 mg on pain25,46,60. Two open-label studies reported detailed outcomes based on the King’s PD pain scale, suggesting that safinamide 100 mg improves fluctuation-related pain43,61. Collectively, safinamide 100 mg possibly ameliorates pain, especially fluctuation-related pain, with trivial to small effect size (0.16–0.41).
Collectively, rasagiline and safinamide might improve pain, especially in patients with more advanced disease stages. Note that no selegiline studies have reported pain outcomes.
Fatigue (Table 5)
A large multicenter, double-blind, placebo-controlled RCT for early PD patients reported a significant difference in fatigue favoring rasagiline compared with placebo at 36 weeks62. However, the effect sizes were trivial (0.03 and 0.02 for rasagiline 1 and 2 mg, respectively). In a small multicenter, double-blind, placebo-controlled RCT for PD patients with moderate to severe fatigue, fatigue significantly improved with rasagiline 1 mg at 12 weeks (effect size, incalculable)23.
Three open-label prospective studies of safinamide reported contrasting findings. One study showed significant alleviation of fatigue with a large effect size (0.97)44, while the other two reported non-significant results25,45.
Taken together, the number of studies reporting fatigue outcomes remains scarce, and the impact of MAO-BIs on fatigue appears inconsistent across studies.
Autonomic dysfunctions (Table 6)
A large RCT for early PD patients found no significant benefits of rasagiline on urinary symptoms based on the PDQUALIF urinary function subscore at 26 weeks54. In a small single-center, open-label, prospective study, urodynamic evaluations revealed a significant gain in volume variables after the 2-month administration of rasagiline 1 mg63.
In a small single-center, open-label, prospective study for advanced PD patients, safinamide 50 mg ameliorated overall autonomic symptoms based on the SCOPA-Autonomic at 6 months44. The result for each domain was not reported. A large single-center, open-label, retrospective study showed that safinamide 100 mg reduced the SCOPA-Autonomic urinary problems subscore at 3 months24. The benefits were driven mainly by alleviating incontinence, urgency, daily frequency, and nocturia. A multicenter, open-label, prospective study on PD patients with high non-motor burden reported the effects of safinamide 100 mg on autonomic symptoms using the NMSS subscore25. Significant improvement was observed not in cardiovascular and sexual symptoms domains but in gastrointestinal and urinary symptoms domains.
In summary, the effects of MAO-BIs on various autonomic symptoms remain unclear because of the scarcity of data.
Cognitive dysfunctions
A total of 29 studies tested the effects of MAO-BIs on cognitive functions using various assessment batteries (Supplementary Table 2). No studies for either early or advanced PD patients found significant benefits in global cognition based on the Mini Mental State Examination (MMSE), Montreal Cognitive Assessment (MoCA), or SCOPA-Cognition20,22,28,38,44,45,52,64,65,66. Likewise, except for the following ones, most studies did not find beneficial effects of MAO-BIs using domain-specific cognition assessment batteries.
Two multicenter, double-blind, placebo-controlled RCTs investigated the effects of rasagiline 1 mg on cognitive functions in PD patients with MCI19,20. One RCT assessed the effects of rasagiline on global cognition and cognition-related instrumental activities of daily living based on the SCOPA-Cognition, MoCA, and Penn Daily Activities Questionnaire but failed to show significant benefits20. The other RCT reported the effects of rasagiline on various cognitive domains: attention, executive functions, memory, visuospatial functions, and language19. Although digit span–backward and verbal fluency total scores showed significantly better outcomes in rasagiline compared with placebo, the additional analysis showed significant benefits of rasagiline only in the attentional domain.
Two single-center open-label prospective studies from the same group investigated the effects of MAO-BIs in PD patients with wearing-off67,68. The unique point of these studies was that cognitive assessments were performed 20 min before the second scheduled daily dose of levodopa. Consequently, executive functions improved with either rasagiline or safinamide.
Collectively, MAO-BIs are unlikely to improve global cognition but might have the potential to improve fluctuation-related cognitive dysfunctions.
Miscellaneous: apathy, olfactory dysfunctions, and ICD (Table 7)
In a small single-center, open-label, prospective study for advanced PD patients, significant improvement in apathy was observed 6 months after administrating safinamide 50 mg with a moderate effect size (0.58)44. Conversely, multicenter RCTs did not find significant benefits of rasagiline on apathy17,23. Two double-blind, placebo-controlled RCTs tested the effects of rasagiline 1 mg on olfactory functions with non-significant benefits28,69. A single-center, open-label, prospective study reported no significant impact of safinamide 50 mg on ICD based on the Questionnaire for ICD in PD rating scale (QUIP-RS)44.
Discussion
This systematic review summarized the QOL and NMS outcomes drawn from the available clinical studies of MAO-BIs. The impact of MAO-BIs on QOL was inconsistent across studies, and this was unlikely to be clinically meaningful. Overall, rasagiline and safinamide had more evidence supporting improvements in NMS when compared with selegiline. MAO-BIs potentially improve depression, sleep disturbances, and pain (particularly pain related to motor fluctuations). In contrast, MAO-BIs are unlikely to improve cognitive and olfactory dysfunctions. Given the paucity of evidence, the effects of MAO-BIs on fatigue, autonomic dysfunctions, apathy, and ICD remain unknown. As the recent review on NMS treatment by the Movement Disorders Society demonstrated, there still remain significant unmet needs in this field5. Thus, the potential roles of MAO-BIs in the treatment of NMS will be discussed in the following paragraphs.
A subset of RCTs for advanced PD patients demonstrated statistically significant benefits of rasagiline or safinamide on QOL, with trivial to small effect sizes23,31,37,38,39,41. The minimal clinically important difference (MCID) is the smallest difference in scores that are subjectively meaningful to patients. The MCID threshold for the PDQ-39 summary index was reported to be −4.72 (improvement) and +4.22 (worsening)70. No MAO-BI studies demonstrated improvement of the PDQ-39 summary index larger than this MCID threshold. Thus, the impact of MAO-BI on overall QOL may not be clinically meaningful.
Depression and anxiety are among the most common NMS in PD and are key determinants of QOL71. Past studies showed beneficial effects of rasagiline 1 mg23, safinamide 100 mg37,39,48, and selegiline 10 mg51,52,53 for depressive symptoms, although the results were inconsistent across studies. Of note, most RCTs of MAO-BIs excluded patients with clinically-relevant depression or patients on concurrent antidepressants for safety reasons19,34,37,38,39,47,48,49,51,52,53,64,65, possibly in some studies accounting for non-significant results. A multicenter, double-blind, placebo-controlled RCT (ACCORDO) evaluated the effects of rasagiline 1 mg on depressive symptoms in depressive PD patients17. The primary efficacy variable, the BDI scores, improved significantly in the rasagiline group compared with placebo at 4 weeks (effect size, 1.01), without a significant between-group difference at 12 weeks. In the afore-mentioned review on NMS treatment by the Movement Disorders Society, pramipexole was the only parkinsonian medication, classified as “efficacious” for depressive symptoms5. This was mainly based on the positive results from a multicenter, double-blind, placebo-controlled RCT for PD patients with depressive symptoms, where the BDI scores decreased significantly in the pramipexole group compared with placebo at 12 weeks (−5.9 ± 0.5 vs. −4.0 ± 0.5, P = 0.01)72. The results from the ACCORDO and the above-mentioned pramipexole study seem comparable. The negative results for the ACCORDO study might be partly explained by large placebo effects at 12 weeks (rasagiline 1 mg −5.40 ± 0.79 vs. placebo −4.43 ± 0.73, P = 0.368), as patients with depression are known to show high response rates to placebo73. Another issue will be the safety of co-administrating MAO-BIs and antidepressants. A few studies for large PD cohorts did not observe serotonin syndrome despite the combined therapy18,74,75. Although serotonin syndrome seems rare, the long-term safety of the combined therapy needs to be clarified because of the potentially fatal nature of the serotonin syndrome. Finally, three studies using either rasagiline or safinamide assessed anxiety, and all three had negative results19,22,23. The positive effects of MAO-BIs on anxiety, therefore, remain unproven.
Nocturnal sleep disturbances include difficulty initiating sleep, difficulty maintaining sleep, and early morning awakenings; another issue for PD patients is excessive daytime sleepiness76. A small placebo-controlled RCT for PD patients with sleep disturbances demonstrated, using polysomnography, significantly better sleep maintenance with rasagiline 1 mg with statistically non-significant improvement in sleep efficacy by 9.3%14. However, other studies of rasagiline, safinamide, or selegiline reported contrasting findings presumably because sleep disturbances in PD patients are multifactorial: e.g., nocturnal hypokinesia, nocturia, pain, muscle cramps, restless legs syndrome, RBD, or adverse effects of medications76. Therefore, treatment options should be tailored to the putative etiology of patients’ sleep disturbances. In the review on NMS treatment by the Movement Disorders Society5, no treatment options were classified as “efficacious” for sleep disturbances, and rotigotine was the only parkinsonian medication that was classified as “likely efficacious.” A small placebo-controlled RCT assessed the impact of rotigotine on nocturnal sleep using polysomnography in advanced PD patients with sleep disturbances77. Consequently, rotigotine administration led to significantly larger improvement in sleep efficacy as compared with placebo (8.0% vs. 0.5%, P < 0.001). In other studies, ropinirole and rotigotine have been shown to improve nocturnal sleep disturbances mainly by improving nocturnal motor symptoms78,79,80. MAO-BIs potentially improve sleep disturbances through a similar mechanism; however, this remains speculative.
Multiple etiologies of pain in PD patients have been suggested: fluctuation-related, central, musculoskeletal, or neuropathic pain81. However, in the review on NMS treatment by the Movement Disorders Society5, no treatment options were labeled as “efficacious” or “likely efficacious” for pain. Rasagiline and safinamide have been beneficial for pain in advanced PD patients31,32,37. Detailed investigations on pain, based on the King’s PD pain scale, have suggested that fluctuation-related pain responded best to safinamide 100 mg43,61. Similarly, dopamine agonizts such as ropinirole or apomorphine have been reported to improve fluctuation-related pain82,83. Therefore, compared with patients with early PD, those with advanced PD might benefit more from long-acting dopaminergic agents (e.g., MAO-BIs or dopamine agonizts) in pain relief.
Accumulating evidence suggests that MAO-BIs are unlikely to improve cognitive and olfactory dysfunctions20,22,28,38,44,45,52,64,65,66,69. The limited available evidence did not allow us to determine the effects of MAO-BIs on fatigue, autonomic dysfunctions, apathy, and ICD. Note that selegiline suppressed cardiovascular autonomic responses84,85 and could result in orthostatic hypotension86,87,88. Clinicians should be aware of this potential adverse effect, as it may increase the risk of falling89. The pathophysiology of NMS remains uncertain but may involve both dopaminergic and non-dopaminergic dysfunctions11. Further clinical and preclinical investigations will be required.
There are several possible mechanisms for MAO-BIs improving NMS. MAO-BIs may improve nocturnal sleep disturbances or pain by improving motor symptoms and motor fluctuations90. Other NMS might improve through alleviation of non-motor fluctuations91. Open-label studies have suggested that executive dysfunctions related to non-motor fluctuations improved with MAO-BIs67,68. Future studies should investigate the effects of MAO-BIs specifically on NMS with or without fluctuations. The Non-Motor Fluctuation Assessment Questionnaire (NoMoFA) was recently validated and should be helpful to capture static and fluctuating NMS92. In addition, the effects of MAO-BIs on MAO-A, which metabolizes catecholamines and serotonin, might account for part of the effects of MAO-BIs1.
Another potential mechanism of action exclusively for safinamide is the modulation of overactive glutamatergic tone2,3. Increasing evidence from preclinical and clinical studies supports the importance of glutamatergic transmission in motor and NMS of PD93. Since safinamide 50 mg completely inhibits MAO-B activity, additional benefits with safinamide 100 mg might be due to non-dopaminergic mechanisms1. Interestingly, post hoc analysis of a large placebo-controlled RCT reported that safinamide 100 mg might improve dyskinesia94. This effect was analogous to the dyskinesia-suppressing effects of amantadine, an NMDA glutamate receptor antagonist95. In addition, a large RCT demonstrated that safinamide 100 mg improved depressive symptoms and pain with greater effect sizes compared with safinamide given at 50 mg39. The clinical relevance of dopaminergic and non-dopaminergic effects of safinamide needs further exploration.
We would like to highlight the limitations of the current study. First, most studies included were RCTs reporting QOL or non-motor results as the secondary outcomes or open-label studies. Therefore, the outcomes should be cautiously interpreted. Second, considerable inconsistency exists among studies. The variation in the inclusion criteria, assessment batteries, follow-up periods, and numbers of participants may account for the highly variable outcomes. Note that QOL or NMS assessment batteries used in some studies were not recommended for PD patients96,97,98,99,100,101. Genetic diversity may also have an effect on the variability of outcomes, as polymorphisms of MAO-A, MAO-B, and catechol-o-methyltransferase (COMT) have been associated with the occurrence of motor fluctuations in PD patients and psychiatric symptoms in non-PD populations102,103,104. Third, as most studies reported relatively short-term outcomes, longer-term data are warranted. Finally, another important thing to discuss is how to determine the impact of the various interventions. MCID avoids the issue of mere statistical significance and provides a threshold at which results are clinically meaningful. To the best of our knowledge, MCID for non-motor assessment batteries has not been studied in PD patients, except for the PDSS-2105. Alternatively, we calculated effect sizes to estimate the clinical relevance of interventions despite criticism about this method106. Unfortunately, required data were missing in some studies. Standardized reporting of the results, including numbers of patients and, mean scores with SD at baseline and post-intervention, will be essential as these data are also needed for future meta-analyses.
In conclusion, MAO-BIs may potentially improve depression, sleep disturbances, and pain. In contrast, MAO-BI administration may not lead to clinically-meaningful improvement in QOL or cognitive and olfactory dysfunctions. The effects of MAO-BIs on other NMS remain unclear. If NMS is related to poor motor symptoms, or if NMS fluctuates along with blood levodopa concentration, the NMS may be more likely to improve with MAO-BIs. With the increasing number of treatment options available, it will be important to compare the efficacy of MAO-BIs with other options, such as dopamine agonizts and COMT inhibitors. Especially, the effects of these agents on static and fluctuating NMS should be investigated in future studies. Non-dopaminergic effects of safinamide are also of great interest. Ideally, clinicians should be able to provide personalized medicine based on patients’ symptoms and genetic profiles. By drawing attention to the gaps in knowledge, we hope to encourage researchers to conduct high-quality research exploring the efficacy of MAO-BIs and other agents on NMS for persons living with PD.
Methods
Search strategy
We conducted a systematic literature search from January 1990 to November 2021 using the PubMed, Scopus, and Cochrane Library databases according to the Preferred Reporting Items for Systematic Reviews and Meta-analysis (PRISMA) guidelines. The search terms included Parkinson’s disease, Parkinson disease, selegiline, rasagiline, and safinamide. The search syntax is provided in Supplementary Material. Two investigators (TT and YS) independently screened all records for duplicates and then performed title/abstract screening and full-text assessments based on the eligibility criteria below. Disagreements were resolved through review of the primary study and expert discussion.
Eligibility criteria and calculation of effect sizes
The inclusion criteria for this systematic review were: (1) clinical studies on patients with Parkinson’s disease (n ≥ 10), (2) reporting the effects of selegiline, rasagiline, or safinamide on NMS or QOL using symptom-specific assessment batteries or objective measures, and (3) written in English. NMS included the following ones: depression, anxiety, sleep disturbances, fatigue, pain, autonomic dysfunctions, olfactory dysfunctions, cognitive dysfunctions, apathy, psychosis, impulse control disorders (ICD), and rapid eye movement sleep behavior disorders (RBD). Conference papers, review articles, and meta-analyses were excluded. “Real-world” studies were excluded because uncontrolled factors hindered the estimation of the impact of MAO-BIs. We reviewed the reference lists of included publications to find additional publications.
By using mean values and standard deviations (SD) at baseline (meanT1 and SDT1) and mean values after intervention (meanT2) for the scales of interest, we calculated effect sizes according to the following formula: Effect size = [(meanT2 − meanT1)/SDT1]. When the publications lacked required values, effect sizes were shown as “incalculable.” Based on the values, effect sizes were considered trivial (< 0.2), small (0.20–0.49), moderate (0.50–0.79), or large (≥0.8)106.
Quality assessments
We assessed the study quality of the included studies using a PD-specific assessment form designed by den Brok et al., which was based on the Newcastle–Ottawa quality assessment scale (Supplementary Table 1)107.
Data availability
All data relevant to the study are included in the article or uploaded as supplementary information.
References
Alborghetti, M. & Nicoletti, F. Different generations of type-B monoamine oxidase inhibitors in Parkinson’s disease: From bench to bedside. Curr. Neuropharmacol. 17, 861–873 (2019).
Sciaccaluga, M. et al. Effects of safinamide on the glutamatergic striatal network in experimental Parkinson’s disease. Neuropharmacology 170, 108024 (2020).
Morari, M. et al. Safinamide differentially modulates in vivo glutamate and GABA release in the rat hippocampus and basal ganglia. J. Pharmacol. Exp. Ther. 364, 198–206 (2018).
Langston, J. W. The Parkinson’s complex: Parkinsonism is just the tip of the iceberg. Ann. Neurol. 59, 591–596 (2006).
Seppi, K. et al. Update on treatments for nonmotor symptoms of Parkinson’s disease-an evidence-based medicine review. Mov. Disord. 34, 180–198 (2019).
Tábi, T., Vécsei, L., Youdim, M. B., Riederer, P. & Szökő, É. Selegiline: A molecule with innovative potential. J. Neural Transm. 127, 831–842 (2020).
Abbruzzese, G., Barone, P., Lopiano, L. & Stocchi, F. The current evidence for the use of safinamide for the treatment of Parkinson’s disease. Drug Des. Devel. Ther. 15, 2507–2517 (2021).
Giossi, R. et al. Overall efficacy and safety of safinamide in Parkinson’s disease: A systematic review and a meta-analysis. Clin. Drug Investig. 41, 321–339 (2021).
Binde, C. D., Tvete, I. F., Gåsemyr, J., Natvig, B. & Klemp, M. A multiple treatment comparison meta-analysis of monoamine oxidase type B inhibitors for Parkinson’s disease. Br. J. Clin. Pharmacol. 84, 1917–1927 (2018).
Chang, Y., Wang, L. B., Li, D., Lei, K. & Liu, S. Y. Efficacy of rasagiline for the treatment of Parkinson’s disease: An updated meta-analysis. Ann. Med. 49, 421–434 (2017).
LeWitt, P. A. & Chaudhuri, K. R. Unmet needs in Parkinson disease: Motor and non-motor. Parkinsonism Relat. Disord. 80, S7–S12 (2020).
Skorvanek, M. et al. Relationship between the MDS-UPDRS and quality of life: A large multicenter study of 3206 patients. Parkinsonism Relat. Disord. 52, 83–89 (2018).
Prakash, K. M., Nadkarni, N. V., Lye, W. K., Yong, M. H. & Tan, E. K. The impact of non-motor symptoms on the quality of life of Parkinson’s disease patients: A longitudinal study. Eur. J. Neurol. 23, 854–860 (2016).
Schrempf, W. et al. Rasagiline improves polysomnographic sleep parameters in patients with Parkinson’s disease: a double-blind, baseline-controlled trial. Eur. J. Neurol. 25, 672–679 (2018).
Müller, T., Hoffmann, J. A., Dimpfel, W. & Oehlwein, C. Switch from selegiline to rasagiline is beneficial in patients with Parkinson’s disease. J. Neural Transm. 120, 761–765 (2013).
Gallazzi, M. et al. Selegiline reduces daytime sleepiness in patients with Parkinson’s disease. Brain Behav. 11, e01880 (2021).
Barone, P. et al. A randomized clinical trial to evaluate the effects of rasagiline on depressive symptoms in non-demented Parkinson’s disease patients. Eur. J. Neurol. 22, 1184–1191 (2015).
Peña, E. et al. Impact of SAfinamide on depressive symptoms in Parkinson’s disease patients (SADness-PD study): A multicenter retrospective study. Brain Sci. 11, 232 (2021).
Hanagasi, H. A. et al. The effects of rasagiline on cognitive deficits in Parkinson’s disease patients without dementia: A randomized, double-blind, placebo-controlled, multicenter study. Mov. Disord. 26, 1851–1858 (2011).
Weintraub, D. et al. Rasagiline for mild cognitive impairment in Parkinson’s disease: A placebo-controlled trial. Mov. Disord. 31, 709–714 (2016).
Cibulcik, F. et al. Effects of rasagiline on freezing of gait in Parkinson’s disease—an open-label, multicenter study. Biomed. Pap. Med. Fac. Univ. Palacky. Olomouc Czech. Repub. 160, 549–552 (2016).
Rahimi, F., Roberts, A. C. & Jog, M. Patterns and predictors of freezing of gait improvement following rasagiline therapy: A pilot study. Clin. Neurol. Neurosurg. 150, 117–124 (2016).
Lim, T. T. et al. Rasagiline for the symptomatic treatment of fatigue in Parkinson’s disease. Mov. Disord. 30, 1825–1830 (2015).
Gómez-López, A. et al. SURINPARK: Safinamide for urinary symptoms in Parkinson’s disease. Brain Sci. 11, 57 (2021).
Santos García, D. et al. Safinamide improves non-motor symptoms burden in Parkinson’s disease: An open-label prospective study. Brain Sci. 11, 316 (2021).
Plastino, M. et al. Effects of safinamide on REM sleep behavior disorder in Parkinson disease: A randomized, longitudinal, cross-over pilot study. J. Clin. Neurosci. 91, 306–312 (2021).
Jenkinson, C., Fitzpatrick, R., Peto, V., Greenhall, R. & Hyman, N. The Parkinson’s Disease Questionnaire (PDQ-39): Development and validation of a Parkinson’s disease summary index score. Age Ageing 26, 353–357 (1997).
Hauser, R. A. et al. Randomized, controlled trial of rasagiline as an add-on to dopamine agonists in Parkinson’s disease. Mov. Disord. 29, 1028–1034 (2014).
Hattori, N. et al. Rasagiline monotherapy in early Parkinson’s disease: A phase 3, randomized study in Japan. Parkinsonism Relat. Disord. 60, 146–152 (2019).
Zhang, Z. et al. Efficacy and safety of rasagiline in Chinese patients with early Parkinson’s disease: a randomized, double-blind, parallel, placebo-controlled, fixed-dose study. Transl. Neurodegener. 7, 32 (2018).
Hattori, N. et al. Efficacy and safety of adjunctive rasagiline in Japanese Parkinson’s disease patients with wearing-off phenomena: A phase 2/3, randomized, double-blind, placebo-controlled, multicenter study. Parkinsonism Relat. Disord. 53, 21–27 (2018).
Zhang, Z. et al. Adjunct rasagiline to treat Parkinson’s disease with motor fluctuations: a randomized, double-blind study in China. Transl. Neurodegener. 7, 14 (2018).
Parkinson Study Group. A randomized placebo-controlled trial of rasagiline in levodopa-treated patients with Parkinson disease and motor fluctuations: the PRESTO study. Arch. Neurol. 62, 241–248 (2005).
Parkinson Study Group. A controlled trial of rasagiline in early Parkinson disease: The TEMPO Study. Arch. Neurol. 59, 1937–1943 (2002).
Hattori, N. et al. Long-term, open-label, phase 3 study of rasagiline in Japanese patients with early Parkinson’s disease. J. Neural Transm. 126, 299–308 (2019).
Hattori, N. et al. Long-term safety and efficacy of adjunctive rasagiline in levodopa-treated Japanese patients with Parkinson’s disease. J. Neural Transm. 126, 289–297 (2019).
Borgohain, R. et al. Randomized trial of safinamide add-on to levodopa in Parkinson’s disease with motor fluctuations. Mov. Disord. 29, 229–237 (2014).
Schapira, A. H. et al. Assessment of safety and efficacy of safinamide as a levodopa adjunct in patients with Parkinson disease and motor fluctuations: A randomized clinical trial. JAMA Neurol. 74, 216–224 (2017).
Borgohain, R. et al. Two-year, randomized, controlled study of safinamide as add-on to levodopa in mid to late Parkinson’s disease. Mov. Disord. 29, 1273–1280 (2014).
Hattori, N. et al. Efficacy and safety of safinamide as an add-on therapy to L-DOPA for patients with Parkinson’s disease: A randomized, double-blind, placebo-controlled, phase II/III study. Parkinsonism Relat. Disord. 75, 17–23 (2020).
Cattaneo, C., Jost, W. H. & Bonizzoni, E. Long-term efficacy of safinamide on symptoms severity and quality of life in fluctuating Parkinson’s disease patients. J. Parkinsons. Dis. 10, 89–97 (2020).
Tsuboi, Y. et al. Long-term safety and efficacy of safinamide as add-on therapy in levodopa-treated Japanese patients with Parkinson’s disease with wearing-off: Results of an open-label study. J. Neurol. Sci. 416, 117012 (2020).
Grigoriou, S. et al. Effects of safinamide on pain in patients with fluctuating Parkinson’s disease. Brain Behav. 11, e2336 (2021).
De Micco, R. et al. Effects of safinamide on non-motor, cognitive, and behavioral symptoms in fluctuating Parkinson’s disease patients: a prospective longitudinal study. Neurol. Sci. 43, 357–364 (2022).
Bianchi, M. L. E., Riboldazzi, G., Mauri, M. & Versino, M. Efficacy of safinamide on non-motor symptoms in a cohort of patients affected by idiopathic Parkinson’s disease. Neurol. Sci. 40, 275–279 (2019).
Geroin, C. et al. Effects of safinamide on pain in Parkinson’s disease with motor fluctuations: An exploratory study. J. Neural Transm. 127, 1143–1152 (2020).
Stern, M. B. et al. Double-blind, randomized, controlled trial of rasagiline as monotherapy in early Parkinson’s disease patients. Mov. Disord. 19, 916–923 (2004).
Cattaneo, C. et al. Long-term effects of safinamide on mood fluctuations in Parkinson’s disease. J. Parkinsons. Dis. 7, 629–634 (2017).
Dalrymple-Alford, J. C., Jamieson, C. F. & Donaldson, I. M. Effects of selegiline (deprenyl) on cognition in early Parkinson’s disease. Clin. Neuropharmacol. 18, 348–359 (1995).
Hietanen, M. H. Selegiline and cognitive function in Parkinson’s disease. Acta Neurol. Scand. 84, 407–410 (1991).
Shoulson, I. An interim report of the effect of selegiline (L-deprenyl) on the progression of disability in early Parkinson’s disease. The Parkinson Study Group. Eur. Neurol. 32(Suppl 1), 46–53 (1992).
Pålhagen, S. et al. Selegiline slows the progression of the symptoms of Parkinson disease. Neurology 66, 1200–1206 (2006).
Allain, H., Cougnard, J. & Neukirch, H. C. Selegiline in de novo parkinsonian patients: The French selegiline multicenter trial (FSMT). Acta Neurol. Scand. Suppl. 136, 73–78 (1991).
Biglan, K. M. et al. Rasagiline improves quality of life in patients with early Parkinson’s disease. Mov. Disord. 21, 616–623 (2006).
Panisset, M. et al. Open-label study of sleep disturbances in patients with Parkinson’s disease treated with rasagiline. Can. J. Neurol. Sci. 43, 809–814 (2016).
Schettino, C. et al. Rasagiline for sleep disorders in patients with Parkinson’s disease: A prospective observational study. Neuropsychiatr. Dis. Treat. 12, 2497–2502 (2016).
Liguori, C., Stefani, A., Ruffini, R., Mercuri, N. B. & Pierantozzi, M. Safinamide effect on sleep disturbances and daytime sleepiness in motor fluctuating Parkinson’s disease patients: A validated questionnaires-controlled study. Parkinsonism Relat. Disord. 57, 80–81 (2018).
Waters, C. H. et al. Zydis selegiline reduces off time in Parkinson’s disease patients with motor fluctuations: A 3-month, randomized, placebo-controlled study. Mov. Disord. 19, 426–432 (2004).
Tsuboi, Y. et al. Effects of safinamide adjunct therapy on pain in patients with Parkinson’s disease: Post hoc analysis of a Japanese phase 2/3 study. J. Neurol. Sci. 429, 118070 (2021).
Cattaneo, C., Kulisevsky, J., Tubazio, V. & Castellani, P. Long-term efficacy of safinamide on Parkinson’s disease chronic pain. Adv. Ther. 35, 515–522 (2018).
Santos García, D. et al. Pain improvement in Parkinson’s disease patients treated with safinamide: Results from the SAFINONMOTOR study. J. Pers. Med. 11, 798 (2021).
Stocchi, F. & ADAGIO investigators. Benefits of treatment with rasagiline for fatigue symptoms in patients with early Parkinson’s disease. Eur. J. Neurol. 21, 357–360 (2014).
Brusa, L. et al. Rasagiline effect on bladder disturbances in early mild Parkinson’s disease patients. Parkinsonism Relat. Disord. 20, 931–932 (2014).
Stocchi, F. et al. A randomized, double-blind, placebo-controlled trial of safinamide as add-on therapy in early Parkinson’s disease patients. Mov. Disord. 27, 106–112 (2012).
Schapira, A. H. et al. Long-term efficacy and safety of safinamide as add-on therapy in early Parkinson’s disease. Eur. J. Neurol. 20, 271–280 (2013).
Pålhagen, S. et al. Selegiline delays the onset of disability in de novo parkinsonian patients. Swedish Parkinson study group. Neurology 51, 520–525 (1998).
Rinaldi, D., Assogna, F., Sforza, M., Tagliente, S. & Pontieri, F. E. Rasagiline for dysexecutive symptoms during wearing-off in Parkinson’s disease: A pilot study. Neurol. Sci. 39, 141–143 (2018).
Rinaldi, D. et al. Safinamide improves executive functions in fluctuating Parkinson’s disease patients: an exploratory study. J. Neural Transm. 128, 273–277 (2021).
Haehner, A. et al. Effects of rasagiline on olfactory function in patients with Parkinson’s disease. Mov. Disord. 28, 2023–2027 (2013).
Horváth, K. et al. Changes in quality of life in Parkinson’s disease: How large must they be to be relevant? Neuroepidemiology 48, 1–8 (2017).
Balestrino, R. & Martinez-Martin, P. Neuropsychiatric symptoms, behavioural disorders, and quality of life in Parkinson’s disease. J. Neurol. Sci. 373, 173–178 (2017).
Barone, P. et al. Pramipexole for the treatment of depressive symptoms in patients with Parkinson’s disease: A randomised, double-blind, placebo-controlled trial. Lancet Neurol. 9, 573–580 (2010).
Zis, P. & Mitsikostas, D. D. Nocebo responses in brain diseases: A systematic review of the current literature. Int. Rev. Neurobiol. 139, 443–462 (2018).
Panisset, M. et al. Serotonin toxicity association with concomitant antidepressants and rasagiline treatment: Retrospective study (STACCATO). Pharmacotherapy 34, 1250–1258 (2014).
Smith, K. M., Eyal, E. & Weintraub, D. Combined rasagiline and antidepressant use in Parkinson disease in the ADAGIO study: Effects on nonmotor symptoms and tolerability. JAMA Neurol. 72, 88–95 (2015).
Zuzuárregui, J. R. P. & During, E. H. Sleep issues in Parkinson’s disease and their management. Neurotherapeutics 17, 1480–1494 (2020).
Pierantozzi, M. et al. Rotigotine may improve sleep architecture in Parkinson’s disease: A double-blind, randomized, placebo-controlled polysomnographic study. Sleep. Med. 21, 140–144 (2016).
Ray Chaudhuri, K. et al. Improvements in nocturnal symptoms with ropinirole prolonged release in patients with advanced Parkinson’s disease. Eur. J. Neurol. 19, 105–113 (2012).
Trenkwalder, C. et al. Rotigotine effects on early morning motor function and sleep in Parkinson’s disease: a double-blind, randomized, placebo-controlled study (RECOVER). Mov. Disord. 26, 90–99 (2011).
Bhidayasiri, R. et al. Rotigotine for nocturnal hypokinesia in Parkinson’s disease: Quantitative analysis of efficacy from a randomized, placebo-controlled trial using an axial inertial sensor. Parkinsonism Relat. Disord. 44, 124–128 (2017).
Buhmann, C., Kassubek, J. & Jost, W. H. Management of pain in Parkinson’s disease. J. Parkinsons. Dis. 10, S37–S48 (2020).
Kassubek, J. et al. Rotigotine transdermal system and evaluation of pain in patients with Parkinson’s disease: A post hoc analysis of the RECOVER study. BMC Neurol. 14, 42 (2014).
Factor, S. A., Brown, D. L. & Molho, E. S. Subcutaneous apomorphine injections as a treatment for intractable pain in Parkinson’s disease. Mov. Disord. 15, 167–169 (2000).
Haapaniemi, T. H. et al. Levodopa, bromocriptine, and selegiline modify cardiovascular responses in Parkinson’s disease. J. Neurol. 247, 868–874 (2000).
Turkka, J., Suominen, K., Tolonen, U., Sotaniemi, K. & Myllylä, V. V. Selegiline diminishes cardiovascular autonomic responses in Parkinson’s disease. Neurology 48, 662–667 (1997).
Stryjer, R., Klein, C., Treves, T. A. & Rabey, J. M. The effects of acute loading with levodopa and levodopa with selegiline on blood pressure and plasma norepinephrine levels in chronic Parkinson’s disease patients. Acta Neurol. Scand. 111, 89–94 (2005).
Churchyard, A., Mathias, C. J. & Lees, A. J. Selegiline-induced postural hypotension in Parkinson’s disease: A longitudinal study on the effects of drug withdrawal. Mov. Disord. 14, 246–251 (1999).
Pursiainen, V., Korpelainen, T. J., Haapaniemi, H. T., Sotaniemi, A. K. & Myllylä, V. V. Selegiline and blood pressure in patients with Parkinson’s disease. Acta Neurol. Scand. 115, 104–108 (2007).
Heitterachi, E., Lord, S. R., Meyerkort, P., McCloskey, I. & Fitzpatrick, R. Blood pressure changes on upright tilting predict falls in older people. Age Ageing 31, 181–186 (2002).
Bhidayasiri, R. & Trenkwalder, C. Getting a good night sleep? The importance of recognizing and treating nocturnal hypokinesia in Parkinson’s disease. Parkinsonism Relat. Disord. 50, 10–18 (2018).
Martínez-Fernández, R., Schmitt, E., Martinez-Martin, P. & Krack, P. The hidden sister of motor fluctuations in Parkinson’s disease: A review on nonmotor fluctuations. Mov. Disord. 31, 1080–1094 (2016).
Kleiner, G. et al. Non-motor fluctuations in Parkinson’s disease: Validation of the non-motor fluctuation assessment questionnaire. Mov. Disord. 36, 1392–1400 (2021).
Pagonabarraga, J., Tinazzi, M., Caccia, C. & Jost, W. H. The role of glutamatergic neurotransmission in the motor and non-motor symptoms in Parkinson’s disease: Clinical cases and a review of the literature. J. Clin. Neurosci. 90, 178–183 (2021).
Cattaneo, C., Ferla, R., La, Bonizzoni, E. & Sardina, M. Long-term effects of safinamide on dyskinesia in mid- to late-stage Parkinson’s disease: A post-hoc Analysis. J. Parkinsons. Dis. 5, 475–481 (2015).
Ory-Magne, F. et al. Withdrawing amantadine in dyskinetic patients with Parkinson disease: The AMANDYSK trial. Neurology 82, 300–307 (2014).
Martinez-Martin, P. et al. Health-related quality-of-life scales in Parkinson’s disease: Critique and recommendations. Mov. Disord. 26, 2371–2380 (2011).
Schrag, A. et al. Depression rating scales in Parkinson’s disease: Critique and recommendations. Mov. Disord. 22, 1077–1092 (2007).
Leentjens, A. F. et al. Anxiety rating scales in Parkinson’s disease: Critique and recommendations. Mov. Disord. 23, 2015–2025 (2008).
Högl, B. et al. Scales to assess sleep impairment in Parkinson’s disease: Critique and recommendations. Mov. Disord. 25, 2704–2716 (2010).
Perez-Lloret, S. et al. Rating scales for pain in Parkinson’s disease: Critique and recommendations. Mov. Disord. Clin. Pract. 3, 527–537 (2016).
Skorvanek, M. et al. Global scales for cognitive screening in Parkinson’s disease: Critique and recommendations. Mov. Disord. 33, 208–218 (2018).
Soraya, G. V. et al. Polymorphisms of the dopamine metabolic and signaling pathways are associated with susceptibility to motor levodopa-induced complications (MLIC) in Parkinson’s disease: A systematic review and meta-analysis. Neurol Sci. https://doi.org/10.1007/s10072-021-05829-4 (2022).
Madzarac, Z. et al. The associations between COMT and MAO-B genetic variants with negative symptoms in patients with schizophrenia. Curr. Issues Mol. Biol. 43, 618–636 (2021).
Yen, J. Y. et al. Roles of hostility and depression in the association between the MAOA gene polymorphism and internet gaming disorder. Int. J. Env. Res. Public Heal. 18, 6910 (2021).
Horváth, K. et al. Minimal clinically important difference on Parkinson’s disease sleep scale 2nd version. Parkinsons Dis. 2015, 970534 (2015).
Middel, B. & van Sonderen, E. Statistical significant change versus relevant or important change in (quasi) experimental design: Some conceptual and methodological problems in estimating magnitude of intervention-related change in health services research. Int. J. Integr. Care 2, e15 (2002).
den Brok, M. et al. Apathy in Parkinson’s disease: A systematic review and meta-analysis. Mov. Disord. 30, 759–769 (2015).
Cattaneo, C., Barone, P., Bonizzoni, E. & Sardina, M. Effects of safinamide on pain in fluctuating Parkinson’s disease patients: A post hoc analysis. J. Parkinsons. Dis. 7, 95–101 (2017).
Acknowledgements
This study was supported by AMED under Grant Number JP21km0908001 and Nagoya University Research Fund. We would like to acknowledge the Parkinson’s Foundation Center of Excellence at the University of Florida Norman Fixel Institute for Neurological Diseases.
Author information
Authors and Affiliations
Contributions
T.T. conceived and designed the study. T.T. and Y.S. performed the systematic search and constructed the tables. T.T. wrote the first draft. Inclusions and exclusions of the identified studies from the current systematic review were discussed among T.T., Y.S., A.R.Z., and M.S.O. K.H., M.H., M.S., K.H., A.R.Z., M.S.O., and M.K. reviewed and revised the draft. All authors hold accountability for all aspects of the work.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Tsuboi, T., Satake, Y., Hiraga, K. et al. Effects of MAO-B inhibitors on non-motor symptoms and quality of life in Parkinson’s disease: A systematic review. npj Parkinsons Dis. 8, 75 (2022). https://doi.org/10.1038/s41531-022-00339-2
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41531-022-00339-2