Abstract
For decades, the systemic treatment of localized triple negative breast cancer (TNBC) has exclusively relied on chemotherapy. Recent advancements, however, are rapidly reshaping the treatment algorithms for this disease. The addition of pembrolizumab to neoadjuvant chemotherapy has indeed shown to significantly improve event-free survival for stage II–III TNBC, leading to its establishment as new standard of care in this setting. This landmark advancement has however raised several important scientific questions. Indeed, we desperately need strategies to identify upfront patients deriving benefit from the addition of immunotherapy. Moreover, the best integration of pembrolizumab with further recent advancements (capecitabine, olaparib) is yet to be defined. Lastly, extensive efforts are needed to minimize the impact on patients of immune-related adverse events and financial toxicity. The next decade of clinical research will be key to overcome these challenges, and ultimately learn how to optimally integrate immunotherapy in the treatment landscape of TNBC.
Similar content being viewed by others
Introduction
Triple negative breast cancer (TNBC) has long been a challenging disease to treat due to its aggressive behavior and the lack of actionable targets1. It is commonly diagnosed at a younger age compared with other breast cancer (BC) subtypes, and has a poor prognosis in case of metastatic relapse, with a median overall survival (OS) of less than two years2. Thus, intensive treatment strategies have been developed, to reduce the odds of recurrence after tumor removal. Poly-chemotherapy remains the standard treatment for early TNBC, most often administered preoperatively to assess tumor sensitivity and adapt post-operative systemic treatment accordingly3. Indeed, patients with residual disease after neoadjuvant chemotherapy are at the highest risk of recurrence4 and derive a significant benefit from the addition of adjuvant capecitabine5. Conversely, only follow up is recommended for patients achieving pathological complete response (pCR) at surgery, despite the fact that the risk of relapse remains clinically relevant. Multiple novel agents have been tested in the last decades to improve the prognosis of early TNBC, with none entering clinical practice, except for the recent approval of adjuvant olaparib for the subset of high-risk TNBC patients harboring germline BRCA1 or BRCA2 pathogenic variants6. However, the emergence of cancer immunotherapy is now revolutionizing the way we treat this disease.
The rise of immunotherapy for TNBC
Despite lacking canonical targets for biologic treatment, TNBC is characterized by a relatively high tumor mutational burden (TMB) compared to other subtypes of BC, a feature which has been linked with increased responsiveness to immunotherapy with immune-checkpoint inhibitors (ICIs)7. Indeed, checkpoint inhibition with atezolizumab (now withdrawn in the U.S.) and with pembrolizumab has been approved for advanced-stage, PD-L1 positive TNBC based on the improvement in outcomes observed when combined with frontline chemotherapy8,9. Notably, evidence suggest a superior efficacy of ICIs in TNBC when administered early in the disease course, possibly due to the progression of immune escape mechanisms during the advancement of disease10,11. From this perspective, there was strong rationale for ICI administration to the earliest possible time in the disease course, namely before surgical resection. Results from several randomized trials designed with this purpose are now available, igniting a rapid change of practice in early TNBC.
Of five main randomized trials testing the addition of an anti-programmed cell death-1 (PD-1)/programmed cell death ligand-1 (PD-L1) agent to neoadjuvant chemotherapy12,13,14,15,16, three showed an improvement in pCR rate with immunotherapy12,13,14,17 (Table 1). Furthermore, long-term analyses have recently also demonstrated a survival benefit with this strategy. First, long-term results of the randomized GeparNuevo phase 2 trial were presented at 2021 ASCO Annual Meeting: although the trial has not met its primary endpoint of improving pCR15, the addition of durvalumab to neoadjuvant chemotherapy for high-risk TNBC patients ultimately improved 3-year invasive disease-free survival (iDFS) from 76.9% to 84.9% (HR = 0.54, p = 0.0559) and OS from 83.1% to 95.1% (HR = 0.26, p = 0.0076)18. These results, although suggestive of a benefit, required confirmation, since the trial was not powered to detect survival differences. More recently, the ESMO Virtual Plenary presentation of the mature event-free survival (EFS) results from the KEYNOTE-522 trial brought key new data in this setting, demonstrating that adding checkpoint inhibition in the early stage setting does in fact improve long-term outcomes19.
KEYNOTE-522 was a phase 3 trial in which 1174 stage II–III TNBC patients were randomized to neoadjuvant chemotherapy with paclitaxel-carboplatin followed by doxorubicin-cyclophosphamide, with or without the addition of pembrolizumab; after surgery, patients received adjuvant pembrolizumab (or placebo) for up to nine cycles. Primary endpoints were pCR rate and EFS in the intention-to-treat (ITT) population. pCR results were published in early 2020, showing that among the first 602 patients randomized in the study the addition of pembrolizumab significantly increased pCR rate in the ITT (64.8% vs 51.2%, delta 13.6%; 95%CI, 5.4 to 21.8; p < 0.001), and an initial trend toward an EFS improvement was also observed12. That trend became a clear, statistically significant difference at the last update of the study results, which included 1174 randomized patients: with 37 months of follow up, 15.7% of the patients in the pembrolizumab arm and 23.8% in the placebo arm have experienced an EFS event (HR = 0.63, p = 0.0003)19. Three-year EFS rate was 84.5% with pembrolizumab versus 76.8% with placebo, showing a striking similarity with iDFS results from GeparNuevo18,19. Most EFS events were distant recurrences, leading to a 3-year distant-progression or distant-recurrence free survival of 87% with pembrolizumab versus 80.7% with placebo (HR = 0.61) and a clinically relevant, although not statistically significant difference in 3-year OS (89.7% vs 86.9%, HR = 0.72, p = 0.032)19. Intriguingly, the analysis of pCR rates among all 1174 patients at the third interim analysis showed a smaller delta between arms compared to the first analysis (63% vs 55.6%, delta 7.5%, 95%CI, 1.6 to 13.4)20, highlighting that differences in pCR rates can effectively translate into meaningful EFS benefits with immunotherapy. The addition of pembrolizumab led to an increase in immune-related adverse events (irAEs), with a rate of grade 3-5 irAEs of 14.9% (vs 2.1% in the control arm) and 10.9% of the events leading to any drug discontinuation (vs 2.6% in the control arm)19. Based on these compelling results, on July 26, 2021 the Food and Drugs Administration (FDA) approved pembrolizumab for high-risk, early-stage TNBC in combination with chemotherapy as neoadjuvant treatment, and then continued as a single agent as adjuvant treatment after surgery21.
Identifying responders to immunotherapy: current status and future perspectives
KEYNOTE-522 results prompted a rapid change in clinical practice, leading to the FDA approval of the first immunotherapy agent for early-stage TNBC. This landmark achievement, however, has raised a multitude of scientific questions, requiring a new set of prospective clinical trials.
Indeed, every effort should be dedicated to identifying responders to pembrolizumab upfront, in order to tailor immunotherapy addition upon risk of relapse and immunological background. In this framework, subgroup analyses in KEYNOTE-522 did not highlight any biomarker solidly predicting the benefit of pembrolizumab19. In particular, despite PD-L1 expression being an established predictive biomarker in the advanced setting, it did not differentiate responders from non-responders in the early setting, with both PD-L1-negative and PD-L1-positive patients deriving a benefit from pembrolizumab addition19. It is however important to mention that the PD-L1 threshold adopted in the subgroup analyses of KEYNOTE-522 (CPS ≥ 1) may not be the optimal one, since a threshold of CPS ≥ 10 is currently used for patients selection in the metastatic setting, warranting this additional analysis in the future. A consistent benefit with pembrolizumab was also observed regardless of tumor size, carboplatin schedule, age and performance status19. Lastly, despite node positive patients appeared to derive greater benefit in terms of pCR from pembolizumab addition12, no difference in terms of EFS benefit were observed depending on nodal status at the survival analysis19.
Although standard parameters did not help in selecting patients for immunotherapy, novel promising biomarkers have recently emerged in this field. For instance, the detection of circulating tumor DNA (ctDNA) is emerging as a relevant prognostic factor across oncological diseases, including BC22,23. In the I-SPY2 trial, early BC patients receiving neoadjuvant treatment achieved outstanding disease outcomes with chemotherapy if no ctDNA could be detected at baseline, raising the question if any treatment escalation is required in this population24. Moreover, the presence in the tumor bed of tumor infiltrating lymphocytes (TILs) was shown to harbor a strong prognostic value for early TNBC, with tumors enriched in TILs showing excellent long-term prognosis with (neo)adjuvant chemotherapy25 and even in the absence of treatments26. Of note, when assessed in GeparNuevo trial, the presence of TILs appeared to predict benefit both in the durvalumab-containing arm and in the placebo arm, questioning the use of this biomarker alone to select patients for immunotherapy. Gains in CD274 gene (which encodes for PD-L1) were recently found to be common in TNBC, and associated with benefit to maintenance durvalumab in the advanced setting, warranting the study of this biomarker in the early setting for its promising predictive value27. The expression of Major Histocompatibility (MHC)-II complex on tumor cells was also retrospectively found to identify TNBC patients deriving benefit from the addition of immunotherapy to neoadjuvant chemotherapy in the I-SPY2 trial28. Lastly, evidence regarding the role of MHC I loss in immune-evasion is emerging for multiple tumor types29, warranting additional study in the field of breast cancer.
Besides baseline biomarkers, one established dynamic biomarker, namely the achievement of pCR after neoadjuvant treatment, showed a critical value in KEYNOTE-522. Indeed, a major absolute benefit in terms of EFS was observed among patients not achieving pCR, with a 10% improvement in 3-year EFS (from 56.8% to 67.4%) for patients receiving pembrolizumab, whereas only a 2% difference was observed in those patients achieving pCR. This finding - together with the results of GeparNuevo showing survival outcomes similar to KEYNOTE-522 with immunotherapy administered only before surgery18—support the experimental testing of strategies to de-escalate adjuvant immunotherapy in patients achieving pCR with chemo-immunotherapy. Nonetheless, until prospective evidence is available, current standards of care should include the adjuvant administration of pembrolizumab to all patients receiving it in the neoadjuvant setting without experiencing concerning irAEs. Moreover, when comparing EFS curves from patients achieving pCR in the two arms, it is important to stress the fact that the addition of pembrolizumab led to more patients achieving pCR, ultimately enriching the population of patients achieving a favorable EFS.
Noteworthy, extensive efforts will also be required to expand access to pembrolizumab to populations which were not included in KEYNOTE-522 but which are likely to derive benefit. Such is the case of ER-low patients (ER 1–9%), a population that was excluded from KEYNOTE-522 since not formally meeting the definition of TNBC, but which shares biology and dismal prognosis with canonical TNBC30,31, and could theoretically share the same benefit from the addition of immunotherapy.
Integrating immunotherapy into an expanding arsenal of treatment options
One additional major challenge emerging from KEYNOTE-522 data is the optimal integration of pembrolizumab with other practice changes happening in the last few years. Indeed, since the design and initiation of the trial, two drugs have shown to significantly improve outcomes for TNBC patients at the highest risk of relapse, namely those not achieving pCR after neoadjuvant treatment4. First, the addition of 6-8 cycles of capecitabine in this high-risk cohort of patients showed to relevantly improve DFS and OS in the CREATE-X trial, rapidly reshaping treatment guidelines for TNBC5. More recently, the addition of one year of olaparib for BRCA1- or BRCA2-mutated TNBC patients not achieving pCR after neoadjuvant treatment showed a benefit in DFS and an initial trend in OS improvement in the OlympiA trial6. Neither of these two drugs were allowed in the KEYNOTE-522 trial, where all patients in the study arm received pembrolizumab alone as adjuvant treatment, regardless of residual disease at surgery12. Nonetheless, pragmatism is warranted in clinical practice, in order to derive the maximum benefit from the currently available therapies. In this framework, adjuvant treatment for patients with residual disease may be tailored according to residual cancer burden, overall recurrence risk and germline BRCA status. Therefore, for those patients appearing at the highest risk of recurrence, the addition of adjuvant capecitabine to pembrolizumab is reasonable; adjuvant olaparib ± pembrolizumab could be instead considered for high-risk BRCA-mutant patients. For both regimens we have indeed available data suggesting the safety of combining pembrolizumab with either capecitabine32 or olaparib33. Conversely, for patients with low residual cancer burden and low overall risk of recurrence, continuing pembrolizumab alone may be a reasonable option, if no concerning immune-related toxicities were experienced during neoadjuvant treatment.
Important new data has also recently emerged on neoadjuvant chemotherapy for TNBC. The BrighTNess trial, assessing the addition of veliparib plus carboplatin or carboplatin alone to standard neoadjuvant chemotherapy for high-risk stage II–III TNBC, has previously shown that the addition of carboplatin (but not veliparib) to anthracyclines and taxanes significantly improve pCR rates34. Survival results from this trial were recently presented at ESMO Congress 2021: the addition of carboplatin significantly improved 4-year EFS (79.3% vs 68.5%, HR = 0.57, 95%CI 0.36‒0.91, P = 0.018), whereas no benefit was observed with the addition of veliparib35. These results appear to confirm a long-term benefit of adding carboplatin, although it’s still unclear whether the same benefit is retained when adding ICIs: indeed, a survival benefit was also observed in the GeparNuevo trial, which did not include carboplatin in the neoadjuvant regimen18. In this setting, the inclusion of carboplatin appears reasonable in fit, high-risk, stage II–III TNBC patients, but new research efforts to clarify the need for platinum in the presence of pembrolizumab are urgently required, to understand if more flexibility is acceptable regarding the backbone chemotherapy regimen. Similarly, efforts will be needed to clarify if there is any role for associating dose-dense chemotherapy regimens to immunotherapy, based on the benefits observed with this strategy in prior trials36.
The flip side of the coin: immune-related toxicities and accessibility issues
The price of improving patients’ outcomes with the addition of immunotherapy is the risk of irAEs beyond the toxicities of traditional chemotherapy37. The most common irAEs observed in KEYNOTE-522 were infusion reactions (18%), thyroid impairment (15.1%, hypothyroidism; 5.2% hyperthyroidism), skin toxicities (5.7%), pneumonitis (2.2%), hypophysitis (1.9%), colitis (1.7%) and hepatitis (1.4%) in combined neoadjuvant and adjuvant phases. Importantly, some of these are expected to be irreversible38, permanently conditioning the quality of life of patients in this curable setting. Additionally, concern on the impact of immunotherapy on fertility exist, particularly since TNBC often occurs in pre-menopausal patients39. In this regards, appropriate training of clinicians in the early identification and management of irAEs will be key for the mitigation of immunotherapy side effects. Concomitantly, these risks should be discussed with patients upfront, to provide a clear overview of the risks/benefits balance of adding immunotherapy to chemotherapy for the treatment of their tumor.
Besides immune-related toxicities, another major issue is the economic challenge represented by implementing high-priced drugs in the treatment algorithm of TNBC. Differences in the care and outcomes of patients with cancer arise or worsen with the discovery of new and more effective approaches to cancer treatment. By leading to the FDA approval of immunotherapy in the curative setting for TNBC, KEYNOTE-522 established itself as the archetype of the rapidly expanding use of immunotherapy across the spectrum of disease stages and as the epitome of the emerging disparities in access to these highly effective, but expensive, treatments40 Furthermore, clinical guidelines for BC often fail to appropriately consider health-system context or to provide adaptable guidance and are often incoherent with national cancer policies41. As a result, the design and implementation of effective and integrated multilevel interventions will be required to reduce barriers to equal access to immunotherapy and to equitably provide patients with the opportunity for longer and better-quality survival40.
Research agenda for the next decade
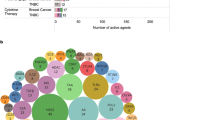
The introduction of immunotherapy marks a revolution in the treatment of early-stage TNBC. KEYNOTE-522 has shown that, by unleashing anti-cancer immune responses through ICIs, long-term benefits can be obtained for the treatment of this aggressive BC subtype. However, it represents a starting point rather than a finish line, and additional efforts will be required precisely implement immunotherapy for the treatment of TNBC (Fig. 1).
Abbreviations: IO, immunotherapy, TNBC, triple negative breast cancer; TMB, tumor mutational burden; ADC, antibody-drug conjugate; ER, estrogen receptor; CD, cluster of differentiation; TILs, tumor infiltrating lymphocytes; PD-L1, Programmed death-ligand 1; HLA, human leukocyte antigen; PD-1, Programmed cell death protein 1; A, adenosine; T, thymine; C, cytosine; G, guanine; BRCA, BReast CAncer gene; EFS, event-freee survival; RD, residual disease; me1, mono-methylated form; BC, breast cancer. Created with biorender.com.
First, biomarkers are desperately needed to optimally identify patients requiring the addition of ICIs to chemotherapy. In this regard, although PD-L1 expression determined with the 22C3 assay did not appear to differentiate responders in KEYNOTE-522, further immune-based biomarkers should be deeply investigated, including different assays and thresholds of PD-L1 expression, the presence of TILs, TMB, the value of CD274 amplifications, MHC-II expression, and immune gene expression profiles. Of note, an integration of these features into a comprehensive immunogram could potentially overcome the limitations of single biomarkers42,43.
Second, strategies should be investigated to dynamically adapt treatment according to the achievement of pCR. This is indeed among the strongest prognostic factors available in TNBC4, and it is reasonable to test differentiated treatment strategies for patients with and without residual disease after neoadjuvant treatment44. Trials should test the actual need for adjuvant immunotherapy for patients achieving pCR after chemotherapy plus pembrolizumab, as well as the optimal integration of immunotherapy with post-neoadjuvant capecitabine and olaparib for patients with residual disease. Moreover, trials testing the addition of ICIs for patients not achieving pCR to chemotherapy alone (e.g. A-BRAVE trial - NCT02926196; SWOG S1418/BR006 trial - NCT02954874) are ongoing, and may allow to understand if even an adjuvant-only administration of immunotherapy could exert clinical benefits in this challenging population. Besides the achievement of pCR, an emerging tool in this setting which deserves deeper investigation is ctDNA detection, which showed solid prognostic value in BC45 and other cancer histologies22. The cTRACK-TN trial (NCT03145961) is currently investigating the benefit of a tailored escalation of treatment with pembrolizumab for early TNBC patients with detectable ctDNA, and will provide precious data in this field of research.
Third, efforts should be invested in the expansion of neoadjuvant ICIs to other populations of patients potentially deriving benefit from this strategy. As mentioned above, ER-low (1–9%) patients appear biologically very similar to TNBC, with nearly 90% of these tumors harboring a basal-like intrinsic subtype30. Prognosis of these patients is also analogous to that of TNBC, highlighting the need for better treatments for this subgroup30,31. Future immunotherapy trials in TNBC should include this population of patients, to clarify if they derive the same benefit from the addition of ICIs to chemotherapy.
Fourth, novel active agents are emerging for the treatment of TNBC and could provide an opportunity for a de-escalation of traditional chemotherapy. In particular, the anti-TROP2 antibody-drug conjugate sacituzumab govitecan has recently shown to improve survival of TNBC patients in the advanced setting46, and it is currently being investigated in the early setting, including in combination with immunotherapy in the ASPRIA trial, where adjuvant sacituzumab govitecan in combination with atezolizumab is given to TNBC patients with residual disease after neoadjuvant treatment and detectable ctDNA. Results from this and additional studies will tell us if better outcomes can be achieved with the introduction of a targeted delivery of chemotherapy in TNBC.
Conclusion
The improvement in outcomes provided by the addition of pembrolizumab to chemotherapy represents a landmark point for the treatment of early-stage TNBC. As for every major scientific advancement, these results raise a multitude of important questions, and a new set of prospective clinical trials will be required in the next decade to optimally tailor the administration of immunotherapy. This should be accompanied by a strong commitment in biomarker discovery and extensive effort devoted to the mitigation of both immune-related and financial toxicities, in order to achieve the safest possible implementation of immunotherapy for patients with a diagnosis of TNBC.
Reporting summary
Further information on research design is available in the Nature Research Reporting Summary linked to this article.
Data availability
Not applicable.
References
Loibl, S., Poortmans, P., Morrow, M., Denkert, C. & Curigliano, G. Breast cancer. Lancet 397, 1750–1769 (2021).
Schmid, P. et al. Atezolizumab plus nab-paclitaxel as first-line treatment for unresectable, locally advanced or metastatic triple-negative breast cancer (IMpassion130): updated efficacy results from a randomised, double-blind, placebo-controlled, phase 3 trial. Lancet Oncol. 21, 44–59 (2020).
Cardoso, F. et al. 5th ESO-ESMO international consensus guidelines for advanced breast cancer (ABC 5). Ann. Oncol. 31, 1623–1649 (2020).
Cortazar, P. et al. Pathological complete response and long-term clinical benefit in breast cancer: the CTNeoBC pooled analysis. Lancet 384, 164–172 (2014).
Masuda, N. et al. Adjuvant capecitabine for breast cancer after preoperative chemotherapy. N. Engl. J. Med. 376, 2147–2159 (2017).
Tutt, A. N. J. et al. Adjuvant olaparib for patients with BRCA1 - or BRCA2 -mutated breast cancer. N. Engl. J. Med. 384, 2394–2405 (2021).
O’Meara, T. A. & Tolaney, S. M. Tumor mutational burden as a predictor of immunotherapy response in breast cancer. Oncotarget 12, 394–400 (2021).
Schmid, P. et al. Atezolizumab and nab-paclitaxel in advanced triple-negative breast cancer. N. Engl. J. Med. 379, 2108–2121 (2018).
Cortes, J. et al. Pembrolizumab plus chemotherapy versus placebo plus chemotherapy for previously untreated locally recurrent inoperable or metastatic triple-negative breast cancer (KEYNOTE-355): a randomised, placebo-controlled, double-blind, phase 3 clinical trial. Lancet 396, 1817–1828 (2020).
Hutchinson, K. E. et al. Comprehensive profiling of poor-risk paired primary and recurrent triple-negative breast cancers reveals immune phenotype shifts. Clin. Cancer Res. 26, 657–668 (2020).
Szekely, B. et al. Immunological differences between primary and metastatic breast cancer. Ann. Oncol. 29, 2232–2239 (2018).
Schmid, P. et al. Pembrolizumab for early triple-negative breast cancer. N. Engl. J. Med. 382, 810–821 (2020).
Mittendorf, E. A. et al. Neoadjuvant atezolizumab in combination with sequential nab-paclitaxel and anthracycline-based chemotherapy versus placebo and chemotherapy in patients with early-stage triple-negative breast cancer (IMpassion031): a randomised, double-blind, phase 3 tria. Lancet 396, 1090–1100 (2020).
Nanda, R. et al. Effect of pembrolizumab plus neoadjuvant chemotherapy on pathologic complete response in women with early-stage breast cancer. JAMA Oncol. 6, 676 (2020).
Loibl, S. et al. A randomised phase II study investigating durvalumab in addition to an anthracycline taxane-based neoadjuvant therapy in early triple-negative breast cancer: clinical results and biomarker analysis of GeparNuevo study. Ann. Oncol. 30, 1279–1288 (2019).
Gianni, L. et al. Abstract GS3-04: Pathologic complete response (pCR) to neoadjuvant treatment with or without atezolizumab in triple negative, early high-risk and locally advanced breast cancer. NeoTRIPaPDL1 Michelangelo randomized study. In General Session Abstracts GS3-04-GS3-04 (American Association for Cancer Research, 2020). https://doi.org/10.1158/1538-7445.SABCS19-GS3-04.
Tarantino, P., Gandini, S., Trapani, D., Criscitiello, C. & Curigliano, G. Immunotherapy addition to neoadjuvant chemotherapy for early triple negative breast cancer: A systematic review and meta-analysis of randomized clinical trials. Crit. Rev. Oncol. Hematol. 159, 103223 (2021).
Loibl, S. et al. Durvalumab improves long-term outcome in TNBC: results from the phase II randomized GeparNUEVO study investigating neodjuvant durvalumab in addition to an anthracycline/taxane based neoadjuvant chemotherapy in early triple-negative breast cancer (TNBC). J. Clin. Oncol. 39, 506–506 (2021).
Schmid, P. et al. VP7-2021: KEYNOTE-522: Phase III study of neoadjuvant pembrolizumab + chemotherapy vs. placebo + chemotherapy, followed by adjuvant pembrolizumab vs. placebo for early-stage TNBC. Ann. Oncol. 32, 1198–1200 (2021).
Oncologic Drugs Advisory Committee (ODAC) Meeting—February 9, 2021. https://www.fda.gov/media/145654/download.
https://www.fda.gov/drugs/resources-information-approved-drugs/fda-grants-accelerated-approval-pembrolizumab-locally-recurrent-unresectable-or-me. FDA grants accelerated approval to pembrolizumab for locally recurrent unresectable or metastatic TNBC. Accessed 13 Aug 2021.
De Mattos-Arruda, L. & Siravegna, G. How to use liquid biopsies to treat patients with cancer. ESMO Open 6, 100060 (2021).
Buono, G. et al. Circulating tumor DNA analysis in breast cancer: Is it ready for prime-time? Cancer Treat. Rev. 73, 73–83 (2019).
Magbanua, M. J. M. et al. Circulating tumor DNA in neoadjuvant-treated breast cancer reflects response and survival. Ann. Oncol. 32, 229–239 (2021).
Loi, S. et al. Tumor-infiltrating lymphocytes and prognosis: a pooled individual patient analysis of early-stage triple-negative breast cancers. J. Clin. Oncol. 37, 559–569 (2019).
Park, J. H. et al. Prognostic value of tumor-infiltrating lymphocytes in patients with early-stage triple-negative breast cancers (TNBC) who did not receive adjuvant chemotherapy. Ann. Oncol. 30, 1941–1949 (2019).
Bachelot, T. et al. Durvalumab compared to maintenance chemotherapy in metastatic breast cancer: the randomized phase II SAFIR02-BREAST IMMUNO trial. Nat. Med. (2021). https://doi.org/10.1038/s41591-020-01189-2.
Gonzalez-Ericsson, P. I. et al. Tumor-specific major histocompatibility-II expression predicts benefit to anti–PD-1/L1 therapy in patients with HER2-negative primary breast cancer (Online Ahead of Print). Clin. Cancer Res. (2021). https://doi.org/10.1158/1078-0432.CCR-21-0607.
Dhatchinamoorty, K., Colbert, J. D. & Rock, k. L. Cancer immune evasion through loss of MHC class I antigen presentation. Front. Immunol. 12, 636568, https://doi.org/10.3389/fimmu.2021.636568 (2021).
Villegas, S. L. et al. Therapy response and prognosis of patients with early breast cancer with low positivity for hormone receptors – An analysis of 2765 patients from neoadjuvant clinical trials. Eur. J. Cancer 148, 159–170 (2021).
Schrodi, S. et al. Outcome of breast cancer patients with low hormone receptor positivity: analysis of a 15-year population-based cohort (Online ahead of print). Ann. Oncol. (2021). https://doi.org/10.1016/j.annonc.2021.08.1988.
Page, D. et al. Abstract P2-09-03: Updated efficacy of first or second-line pembrolizumab (pembro) plus capecitabine (cape) in metastatic triple negative breast cancer (mTNBC) and correlations with baseline lymphocyte and naïve CD4+ T-cell count. In Poster Session Abstracts P2-09-03-P2-09–03 (American Association for Cancer Research, 2019). https://doi.org/10.1158/1538-7445.SABCS18-P2-09-03.
Maio, M. et al. Abstract CT178: Olaparib plus pembrolizumab in patients with previously treated advanced solid tumors with homologous recombination repair mutation (HRRm) and/or homologous recombination deficiency (HRD): Initial results of the phase 2 KEYLYNK-007 study. Cancer Res. 81, CT178–CT178 (2021).
Loibl, S. et al. Addition of the PARP inhibitor veliparib plus carboplatin or carboplatin alone to standard neoadjuvant chemotherapy in triple-negative breast cancer (BrighTNess): a randomised, phase 3 trial. Lancet Oncol. 19, 497–509 (2018).
Loibl, S. et al. Event-free survival (EFS), overall survival (OS), and safety of adding veliparib (V) plus carboplatin (Cb) or carboplatin alone to neoadjuvant chemotherapy in triple-negative breast cancer (TNBC) after ≥4 years of follow-up: BrighTNess, a randomized phase. Ann. Oncol. 32, S407–S446 (2021).
Early Breast Cancer Trialists’ Collaborative Group. Increasing the dose intensity of chemotherapy by more frequent administration or sequential scheduling: a patient-level meta-analysis of 37 298 women with early breast cancer in 26 randomised trials. Lancet 393, 1440–1452 (2019).
Criscitiello, C., Corti, C., Pravettoni, G. & Curigliano, G. Managing side effects of immune checkpoint inhibitors in breast cancer. Crit. Rev. Oncol. Hematol. 162, 103354 (2021).
Haanen, J. B. A. G. et al. Management of toxicities from immunotherapy: ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-up. Ann. Oncol. 28, iv119–iv142 (2017).
Duma, N. & Lambertini, M. It is time to talk about fertility and immunotherapy. Oncologist 25, 277–278 (2020).
Osarogiagbon, R. U., Sineshaw, H. M., Unger, J. M., Acuña-Villaorduña, A. & Goel, S. Immune-based cancer treatment: addressing disparities in access and outcomes. Am. Soc. Clin. Oncol. Educ. B. 66–78 (2021). https://doi.org/10.1200/EDBK_323523.
Trapani, D. et al. The global landscape of treatment standards for breast cancer. JNCI J. Natl. Cancer Inst. 113, 1143–1155 (2021).
Tarantino, P. & Curigliano, G. Defining the immunogram of breast cancer: a focus on clinical trials. Expert Opin. Biol. Ther. 19, 383–385 (2019).
Blank, C. U., Haanen, J. B., Ribas, A. & Schumacher, T. N. The “cancer immunogram” visualizing the state of cancer–immune system interactions may spur personalized therapy. Science 352, 658–660 (2016).
Korde, L. A. et al. Neoadjuvant chemotherapy, endocrine therapy, and targeted therapy for breast cancer: ASCO guideline. J. Clin. Oncol. 39, 1485–1505 (2021).
Cullinane, C. et al. Association of circulating tumor DNA with disease-free survival in breast cancer. JAMA Netw. Open 3, e2026921 (2020).
Bardia, A. et al. Sacituzumab govitecan in metastatic triple-negative breast cancer. N. Engl. J. Med. 384, 1529–1541 (2021).
Acknowledgements
Supported by an American-Italian Cancer Foundation Post-Doctoral Research Fellowship.
Author information
Authors and Affiliations
Contributions
Conceptualization and design: P.T., C.C., P.S., J.C., E.A.M., H.R., S.M.T., G.B., F.A. and G.C. Manuscript writing—original draft: P.T. and C.C. Manuscript writing—review and editing: P.T., C.C., P.S., J.C., E.A.M., H.R., S.M.T., G.B., F.A. and G.C. Final approval of manuscript: P.T., C.C., P.S., J.C., E.A.M., H.R., S.M.T., G.B., F.A. and G.C.
Corresponding author
Ethics declarations
Competing interests
P.T. served as advisor/consultant for AstraZeneca. P.S. reports research support (grants) to his institution from Genentech, F. Hoffmann-La Roche, OncoGenex and Novartis; reports honoraria from AstraZeneca, F. Hoffmann-La Roche, Medscape and G1 Therapeutics; reports a consulting or advisory role with AstraZeneca, Novartis, F. Hoffmann-La Roche, Merck, Boehringer Ingelheim, Bayer, Eisai, Celgene, Pfizer and Puma; and reports that his spouse has a consulting role for Genentech and F. Hoffmann-La Roche. J.C. has declared consulting role for Roche, Celgene, Cellestia, AstraZeneca, Biothera Pharmaceutical, Seattle Genetics, Daiichi Sankyo, Erytech, Athenex, Polyphor, Lilly, MSD, GlaxoSmithKline (GSK), Leuko, Bioasis, and Clovis Oncology; honoraria from Roche, Novartis, Celgene, Eisai, Pfizer, Samsung Bioepis, Lilly, MSD, and Daiichi Sankyo; research funding to the institution from Roche, Ariad Pharmaceuticals, AstraZeneca, Baxalta GMBH–Servier Affaires, Bayer healthcare, Eisai, F Hoffman-La Roche, Guardant Health, MSD, Pfizer, Piqur Therapeutics, Puma C, and Queen Mary University of London and intellectual property for MedSIR. E.A.M. served as advisor/consultant for: Bristol Myers Squib, Exact Sciences (formerly Genomic Health), Genentech/Roche, Lily and Merck. H.S.R. reports the following: Research support for clinical trials through the University of California: Pfizer, Merck, Novartis, Lilly, Roche, Odonate, Daiichi, Seattle Genetics, Macrogenics, Sermonix, Boehringer Ingelheim, Polyphor, Astra Zeneca, OBI and Immunomedics. Honoraria: Puma, Mylan, Samsung. S.M.T. has served as an advisor/consultant to Novartis, Eli Lilly, Pfizer, Merck, AstraZeneca, Eisai, Puma, Genentech, Immunomedics, Nektar, Tesaro, Daiichi Sankyo, Athenex, Bristol Meyers Squibb, and Nanostring. G.B. received honoraria for speaker, consultancy or advisory rule from Roche, Pfizer, AstraZeneca, Lilly, Novartis, Neopharm Israel, Amgen, MSD, Chugai, Sanofi, Daiichi Sankyo, EISAI, Gilead, Seagen, Exact Science, Gilead, Seagen. F.A. received research funding and served as speaker/advisor (compensated to the hospital) for Roche, AstraZeneca, Daiichi Sankyo, Pfizer, Novartis and Lilly. G.C. received honoraria for speaker, consultancy or advisory rule from AstraZeneca, Roche, Pfizer, Novartis, Seattle Genetics, Lilly, Ellipses Pharma, Foundation Medicine, Daiichi Sankyo and Samsung. The remaining authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Tarantino, P., Corti, C., Schmid, P. et al. Immunotherapy for early triple negative breast cancer: research agenda for the next decade. npj Breast Cancer 8, 23 (2022). https://doi.org/10.1038/s41523-022-00386-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41523-022-00386-1
This article is cited by
-
The safety and efficacy of systemic delivery of a new liver-de-targeted TGFβ signaling inhibiting adenovirus in an immunocompetent triple negative mouse mammary tumor model
Cancer Gene Therapy (2024)
-
Immunotherapy in the Treatment of Cancer: Today and Tomorrow
Current Molecular Biology Reports (2024)
-
Advances in immunotherapy for triple-negative breast cancer
Molecular Cancer (2023)
-
Increased expression of the immunoproteasome subunits PSMB8 and PSMB9 by cancer cells correlate with better outcomes for triple-negative breast cancers
Scientific Reports (2023)
-
Deep learning model improves tumor-infiltrating lymphocyte evaluation and therapeutic response prediction in breast cancer
npj Breast Cancer (2023)