Abstract
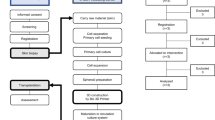
Total phallic construction with radial artery forearm free-flap (RAFFF) is widely regarded as the gold standard approach for phalloplasty. However, donor-site morbidity remains a significant concern, which is typically managed by using a full-thickness skin graft (FTSG) on the forearm. Split thickness skin grafts (STSG) have been proposed as an alternative, along with the use of an acellular dermal matrix substitute. A retrospective comparative analysis was performed to assess the differences in operative, functional and cosmetic outcomes between FTSG (Group A) and the combination of acellular dermal matrix with STSG (Group B). A retrospective cohort study was conducted on all patients who underwent total phallic construction with RAFFF, between 2016 and 2021. Post-operative surgical and functional outcomes were evaluated using validated tools. A total of 34 patients were included in the study, with 18 patients (52.9%) in Group A and 16 patients (47.1%) in Group B. Group B demonstrated a significant advantage in terms of healing time (24 days vs. 30 days, p = 0.003) and complete graft take (93.8% vs. 27.8%, p = 0.001). Group B also had significantly shorter operative times (310 min vs. 447 min, p = 0.001) and a reduced median hospital stay (8 days vs. 10 days, p = 0.001). Satisfaction with cosmesis was significantly higher in Group B (93.8% vs. 66.7%, p = 0.048).
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 8 print issues and online access
$259.00 per year
only $32.38 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout







Similar content being viewed by others
Data availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Wirthmann A, Finke JC, Giovanoli P, Lindenblatt N. Long-term follow-up of donor site morbidity after defect coverage with Integra following radial forearm flap elevation. Eur J Plast Surg. 2014;37:159–66. https://doi.org/10.1007/s00238-013-0918-0.
Falcone M, Blecher G, Anfosso M, Christopher AN, Ralph DJ. Total phallic reconstruction in the genetic male. Eur Urol. 2021;79:684–91. https://doi.org/10.1016/j.eururo.2020.07.025.
Monstrey S, Hoebeke P, Selvaggi G, Ceulemans P, Van Landuyt K, Blondeel P, et al. Penile reconstruction: is the radial forearm flap really the standard technique? Plast Reconstr Surg. 2009;124:510–8.
Doornaert M, Hoebeke P, Ceulemans P, T’Sjoen G, Heylens G, Monstrey S. Penile reconstruction with the radial forearm flap: an update. Handchir Mikrochir Plast Chir. 2011;43:208–14.
Selvaggi G, Dhejne C, Landen M, Elander A. The 2011 WPATH standards of care and penile reconstruction in female-to-male transsexual individuals. Adv Urol. 2012;2012:581712.
Van Caenegem E, Verhaeghe E, Taes Y, Wierckx K, Toye K, Goemaere S, et al. Long-term evaluation of donor-site morbidity after radial forearm flap phalloplasty for transsexual men. J Sex Med. 2013;10:1644–51.
Kovar A, Choi S, Iorio ML. Donor site morbidity in phalloplasty reconstructions: outcomes of the radial forearm free flap. Plast Reconstr Surg Glob Open. 2019;7:e2442.
Ito O, Igawa HH, Suzuki S, Muneuchi G, Kawazoe T, Saso Y, et al. Evaluation of the donor site in patients who underwent reconstruction with a free radial forearm flap. J Reconstr Microsurg. 2005;21:113–7.
Lutz BS, Wei FC, Chang SCN, Yang KH, Chen IH. Donor site morbidity after suprafascial elevation of the radial forearm free flap: a prospective study in 95 consecutive cases. Plast Reconstr Surg. 1999;103:132–7.
Selvaggi G, Monstrey S, Hoebeke P, Ceulemans P, Van Landuyt K, Hamdi M, et al. Donor-site morbidity of the radial forearm free flap after 125 phalloplasties in gender identity disorder. Plast Reconstr Surg. 2006;118:1171–7.
Milcheski DA, Chang AA, Lobato RC, Nakamoto HA, Tuma P Jr, Ferreira MC. Coverage of deep cutaneous wounds using dermal template in combination with negative-pressure therapy and subsequent skin graft. Plast Reconstr Surg Glob Open. 2014;2:e170.
Menn ZK, Lee E, Klebuc MJ. Acellular dermal matrix and negative pressure wound therapy: a tissue-engineered alternative to free tissue transfer in the compromised host. J Reconstr Microsurg. 2012;28:139–44.
Lee JW, Jang YC, Oh SJ. Use of the artificial dermis for free radial forearm flap donor site. Ann Plast Surg. 2005;55:500–2. https://doi.org/10.1097/01.sap.0000183789.00146.c6.
Yu P, Qi Z. Prospective randomized comparison of scar appearances between cograft of acellular dermal matrix with autologous split-thickness skin and autologous split-thickness skin graft alone for full-thickness skin defects of the extremities. Plast Reconstr Surg. 2016;137:906. https://doi.org/10.1097/PRS.0000000000001518.
Lee YJ, Park MC, Park DH, Hahn HM, Kim SM, Lee IJ. Effectiveness of acellular dermal matrix on autologous split-thickness skin graft in treatment of deep tissue defect: esthetic subjective and objective evaluation. Aesthetic Plast Surg. 2017;41:1049–57. https://doi.org/10.1007/s00266-017-0891-2.
Cheshire PA, Herson MR, Cleland H, Akbarzadeh S. Artificial dermal templates: a comparative study of NovoSorbTM biodegrad- able temporising matrix (BTM) and Integra® dermal regenera- tion template (DRT). Burns. 2016;42:1088–96.
Zuidam JM, Coert JH, Hofer SOP. Closure of the donor site of the free radial forearm flap: a comparison of full-thickness graft and split-thickness skin graft. Ann Plast Surg. 2005;55:612–6.
Moiemen NS, Vlachou E, Staiano JJ, Thawy Y, Frame JD. Reconstructive surgery with Integra dermal regeneration template: histologic study, clinical evaluation, and current practice. Plast Reconstr Surg. 2006;117:160S–74S. https://doi.org/10.1097/01.prs.0000222609.40461.68.
De Angelis B, Orlandi F, Fernandes Lopes Morais D’Autilio M, Scioli MG, Orlandi A, Cervelli V, et al. Long-term follow-up comparison of two different bi-layer dermal substitutes in tissue regeneration: clinical outcomes and histological findings. Int Wound J. 2018;15:695–706. https://doi.org/10.1111/iwj.12912.
Müller-Richter UD, Driemel O, Mörtl M, Schwarz S, Zorger N, Wagener H, et al. The value of Allen’s test in harvesting a radial forearm flap: correlation of ex-vivo angiography and histopathological findings. Int J Oral Maxillofac Surg. 2008;37:672–4. https://doi.org/10.1016/j.ijom.2008.01.012.
Chang TS, Hwang WY. Forearm flap in one-stage reconstruction of the penis. Plast Reconstr Surg. 1984;74:251–8. https://doi.org/10.1097/00006534-198408000-00014.
Mitropoulos D, Artibani W, Biyani CS, Bjerggaard Jensen J, Rouprêt M, Truss M. Validation of the Clavien–Dindo grading system in urology by the European Association of Urology guidelines ad hoc panel. Eur Urol Focus. 2018;4:608–13. https://doi.org/10.1016/j.euf.2017.02.014.
Sullivan T, Smith J, Kermode J, McIver E, Courtemanche DJ. Rating the burn scar. J Burn Care Rehabil. 1990;11:256–60. https://doi.org/10.1097/00004630-199005000-00014.
Draaijers LJ, Tempelman FR, Botman YA, Tuinebreijer WE, Middelkoop E, Kreis RW, et al. The patient and observer scar assessment scale: a reliable and feasible tool for scar evaluation. Plast Reconstr Surg. 2004;113:1960–5. https://doi.org/10.1097/01.prs.0000122207.28773.56.
Gajdosik RL, Bohannon RW. Clinical measurement of range of motion: review of goniometry emphasizing reliability and validity. Phys Ther. 1987;67:1867–72. https://doi.org/10.1093/ptj/67.12.1867.
Ciesla N, Dinglas V, Fan E, Kho M, Kuramoto J, Needham D. Manual muscle testing: a method of measuring extremity muscle strength applied to critically ill patients. J Vis Exp. 2011;2632. https://doi.org/10.3791/2632.
Gottlieb LJ, Levine LA. A new design for the radial forearm free-flap phallic construction. Plast Reconstr Surg. 1993;92:276–83.
Song C, Wong M, Wong CH, Ong YS. Modifications of the radial forearm flap phalloplasty for female-to-male gender reassignment. J Reconstr Microsurg. 2011;27:115–20. https://doi.org/10.1055/s-0030-1268210.
Wirthmann AE, Majenka P, Kaufmann MC, Wellenbrock SV, Kasper L, Hüttinger S, et al. Phalloplasty in female-to-male transsexuals by Gottlieb and Levine’s free radial forearm flap technique—a long-term single-center experience over more than two decades. J Reconstr Microsurg. 2018;34:235–41.
Garaffa G, Christopher NA, Ralph DJ. Total phallic reconstruction in female-to-male transsexuals. Eur Urol. 2010;57:715–22. https://doi.org/10.1016/j.eururo.2009.05.018.
Murray RC, Gordin EA, Saigal K, Leventhal D, Krein H, Heffelfinger RN. Reconstruction of the radial forearm free flap donor site using integra artificial dermis. Microsurgery. 2011;31:104–8. https://doi.org/10.1002/micr.20833.
Molteni G, Gazzini L, Bisi N, Nocini R, Ferri A, Bellanti L. et al. Donor site aesthetic and functional outcomes of radial forearm free flap: a comparison between full-thickness and split-thickness skin grafts. Eur J Plast Surg. 2022;45:583–90. https://doi.org/10.1007/s00238-021-01922-1.
Davis WJ 3rd, Wu C, Sieber D, Vandevender DK. A comparison of full and split thickness skin grafts in radial forearm donor sites. J Hand Microsurg. 2011;3:18–24. https://doi.org/10.1007/s12593-011-0036-9.
Haslik W, Kamolz LP, Manna F, Hladik M, Rath T, Frey M. Management of full-thickness skin defects in the hand and wrist region: first long-term experiences with the dermal matrix Matriderm. J Plast Reconstr Aesthet Surg. 2010;63:360–4. https://doi.org/10.1016/j.bjps.2008.09.026.
Demiri E, Papaconstantinou A, Dionyssiou D, Dionyssopoulos A, Kaidoglou K, Efstratiou I. Reconstruction of skin avulsion injuries of the upper extremity with integra® dermal regeneration template and skin grafts in a single-stage procedure. Arch Orthop Trauma Surg. 2013;133:1521–6. https://doi.org/10.1007/s00402-013-1834-2.
Shores JT, Hiersche M, Gabriel A, Gupta S. Tendon coverage using an artificial skin substitute. J Plast Reconstr Aesthet Surg. 2012;65:1544–50. https://doi.org/10.1016/j.bjps.2012.05.021.
Wester JL, Pittman AL, Lindau RH, Wax MK. AlloDerm with split-thickness skin graft for coverage of the forearm free flap donor site. Otolaryngol Head Neck Surg. 2014;150:47–52. https://doi.org/10.1177/0194599813513713.
Author information
Authors and Affiliations
Contributions
Conceived and/or designed the work that led to the submission, acquired data, and/or played an important role in interpreting the results: MF, MP, DC, FP, NP, and MS; LC and MT. Drafted or revised the manuscript: MP, MF, FP, IL, AS, and GB. Approved the final version: MF, MP, DC, PG, and GB. Agreed to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved: MF, MP, and DC.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval
The study was approved by the local institutional review board with protocol number: 201/2021.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Falcone, M., Preto, M., Ciclamini, D. et al. Bioengineered dermal matrix (Integra®) reduces donor site morbidity in total phallic construction with radial artery forearm free-flap. Int J Impot Res (2023). https://doi.org/10.1038/s41443-023-00775-5
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41443-023-00775-5