Abstract
Purpose
Biallelic CAD variants underlie CAD deficiency (or early infantile epileptic encephalopathy-50, [EIEE-50]), an error of pyrimidine de novo biosynthesis amenable to treatment via the uridine salvage pathway. We further define the genotype and phenotype with a focus on treatment.
Methods
Retrospective case series of 20 patients.
Results
Our study confirms CAD deficiency as a progressive EIEE with recurrent status epilepticus, loss of skills, and dyserythropoietic anemia. We further refine the phenotype by reporting a movement disorder as a frequent feature, and add that milder courses with isolated developmental delay/intellectual disability can occur as well as onset with neonatal seizures. With no biomarker available, the diagnosis relies on genetic testing and functional validation in patient-derived fibroblasts. Underlying pathogenic variants are often rated as variants of unknown significance, which could lead to underrecognition of this treatable disorder. Supplementation with uridine, uridine monophosphate, or uridine triacetate in ten patients was safe and led to significant clinical improvement in most patients.
Conclusion
We advise a trial with uridine (monophosphate) in all patients with developmental delay/intellectual disability, epilepsy, and anemia; all patients with status epilepticus; and all patients with neonatal seizures until (genetically) proven otherwise or proven unsuccessful after 6 months. CAD deficiency might represent a condition for genetic newborn screening.
Similar content being viewed by others
INTRODUCTION
Pyrimidine nucleotides play a pivotal role in nucleic acids, protein glycosylation, lipid metabolism, polysaccharide biosynthesis, signal transduction, and proliferation. Uridine 5’-monophosphate (UMP) is the central metabolite in pyrimidine metabolism from which all other pyrimidines are derived.1
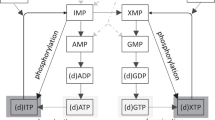
The multifunctional protein CAD, encoded by CAD, contains four highly conserved enzymatic activities (glutamine amidotransferase, carbamoyl-phosphate synthetase 2, aspartate transcarbamylase and dihydroorotase) and catalyzes the first three steps of the de novo UMP biosynthesis. The consecutive steps are catalyzed by dihydroorotate dehydrogenase (DHODH) and UMPS (containing orotate phosphoribosyltransferase and orotidine 5’-phosphate decarboxylase). Alternatively, UMP can be synthesized from uridine via the salvage pathway (Fig. 1a).
(a) Pyrimidine synthesis: de novo versus salvage pathway. De novo synthesis of uridine monophosphate involving three enzymes localized in two cellular compartments. Cytoplasmic CAD (glutamine aminotransferase, carbamoyl phosphate synthase, aspartate transcarbamylase, dihydroorotase) catalyzes the first four steps, dihydroorotate dehydrogenase (DHODH) the subsequent reduction of dihydroorotate in mitochondria, and UMPS (uridine 5’-monophosphate synthase, orotidine 5’-phosphate decarboxylase) the final two steps in the cytoplasm. UMP can also be formed in a single step from uridine by uridine kinase, as part of the pyrimidine recycling pathway. OXPHOS oxidative phosphorylation, PRPP 5-phospho-alpha-D-ribose 1-diphosphate, UMP uridine monophosphate. (b, c) Neuroimaging in CAD deficiency. Coronal T2-weighted magnetic resonance image (MRI): (b) dilated folial fissures indicating cerebellar atrophy (patient UP4, age 4 years). (c) Cerebellar and cerebral atrophy demonstrated by dilated lateral ventricles and extracerebral space (patient UP5, age 5.5 years).
Three inborn errors of metabolism (IEMs) due to deficiency of the three consecutive enzymes of this pathway are known: UMPS deficiency (orotic aciduria, MIM 258900), DHODH deficiency (Miller syndrome, MIM 263750), and the recently described CAD deficiency (early infantile epileptic encephalopathy 50, EIEE-50, MIM 114010).2,3,4,5 CAD deficiency is characterized by global developmental delay (GDD), loss of skills, therapy refractory epilepsy, brain atrophy, and dyserythropoietic anemia. Oral supplementation with uridine or UMP was shown to reverse anemia, control seizures, and improve development in three CAD-deficient patients.2,6
The pathophysiologic cellular mechanisms by which pyrimidine metabolism defects cause central nervous system (CNS) pathology are still largely unknown. In epileptic encephalopathy, epileptic activity contributes significantly to cognitive and behavioral impairment regardless of etiology, type of epilepsy, and age; successful treatment of epileptic activity may improve cognitive impairment in an epileptic encephalopathy.7 Dyserythropoiesis might be due to shortage of pyrimidine-dependent nucleotide–lipid cofactors required for erythrocyte membrane synthesis.8
The diagnosis of CAD deficiency is hampered by the lack of biomarkers and relies entirely on genetic testing, with its pitfalls of variant interpretation as made poignantly clear by del Caño-Ochoa et al.9
Using CRISPR/Cas9, del Caño-Ochoa et al. generated a human CAD-knockout cell line that requires uridine supplements for survival. Transient transfection of the knockout cells with recombinant CAD restores growth in absence of uridine. This system determines missense variants that inactivate CAD and do not rescue the growth phenotype.9
The lack of additional and follow-up data on efficacy and safety hampers the treatment of seriously ill patients and prevents reimbursement for therapy. Therefore, we performed a twofold study including an international cohort study and a literature review to describe the clinical presentations of 20 CAD-deficient patients, the details of uridine supplementation therapy, and patient outcomes.
MATERIALS AND METHODS
This is a case series of individuals who have undergone individual treatment with an over-the-counter food supplement and one individual treated off-label with uridine triacetate.
Patient cohort
All health-care providers who had previously contacted the authors (J.K., S.B.W.) concerning CAD-deficient individuals and uridine treatment were invited to contribute their cases to this case series. Patients were included if they had confirmed biallelic CAD variants and were not previously published. Data were collected retrospectively by clinicians in each center using a standardized questionnaire. All available magnetic resonance images (MRIs) were reviewed by the same investigator (E.B.). Additionally, to identify all reported CAD patients a search for relevant publications was performed in PubMed with filters for English language publications and human species (search completed 17 March 2020).
Functional investigations in patient-derived fibroblasts
Nucleotide sugars in primary fibroblasts were analyzed by ion-pair reversed-phase ultraperformance liquid chromatography as described previously after growth on standard and uridine-enriched culture media.2
Ethics statement
The study was performed in compliance with the Declaration of Helsinki and conforming to the laws and regulations of the respective countries and institutes. All individuals gave written—by proxy—informed consent for genetic investigations and functional investigations in fibroblasts as well as for publication of data; this part of the study was approved by the local ethics committees, either Technical University München (TUM), Munich, Germany (5360/12 S) or Land Salzburg, Salzburg, Austria (415-E/2552/10-2019) as appropriate.
RESULTS
Patient cohort
Via international collaboration 17 patients were included. Four patients (F1:II.2, F1:II.3, F2:II.2, and F3:II.4) were previously published, the other 13 (UPX) were unpublished (of note, UP8 is also included in the functional testing presented in del Cano-Ochoa et al.)2,9 The patients were treated at hospitals in Austria, France, Germany, Greece, Iran, Switzerland, and the United States. The data of three additional patients were extracted from the literature (UPD4003, F9, FiN), making a total of 20 patients from 13 families with CAD deficiency.6,10,11
Genetic patient characteristics
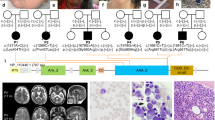
Sixteen individuals were diagnosed via proband-only, proband–parent trio exome sequencing, or multigene panel; three siblings (F1:II.3, UP3.2, UP6.2) were identified via Sanger sequencing following local protocols.12,13 Using exome or Sanger sequencing all parents were proven to carry one variant each. A total of 19 different variants in CAD (NM_004341) were found of which 7 were previously published. These were 6 loss-of-function (LoF) variants and 13 missense variants. Table 1 and Fig. 2 give an overview of all variants, the conservation, the predicted protein change, the American College of Medical Genetics and Genomics (ACMG) classification (manually adjusted at http://wintervar.wglab.org) and the frequencies in the Genome Aggregation Database (gnomAD). In the Supplementary data we provide the detailed prediction of pathogenicity for all missense variants with several prediction programs (https://varsome.com) and the additional genetic investigations in UP5.
(a) Distribution of novel and known variants in the CAD gene. The open reading frame and known domains of the CAD protein (NP_0043332.2) are shown as well as the evolutionary conservation of amino acid residues affected by missense changes. (b, c) The effect of supplementing the growth medium with uridine. Cells were cultured with and without 5 µM uridine. Patient cell lines (F2:II.2, UP1.1, UP5) were compared with controls (n = 2).
The previously reported variant c.98T>G, p.Met33Arg was found in four families originating from Serbia, Croatia, and Bulgaria arguing for the possibility that this disease allele might be more frequently observed in these populations. Its functional relevance was shown in del Caño-Ochoa et al.9 Four of the variants that we have detected in our cohort and one of the published variants were classified as variants of unknown significance (VUS), and one as benign. The VUS c.2995G>A, p.Val999Met was shown to have functional relevance in del Caño-Ochoa et al.9 We also consider the other VUS as pathogenic based on the prediction data, the absence in homozygous state from gnomAD, the matching clinical phenotype (F9), as well as the effect of treatment (UP7, UP10). In UP5 we found a deep intronic variant c.4397-209T>G, Pro1465_Gly1466ins40 that leads to a new cryptic exon termed exon 27a that inserts 120 bp (40 amino acids) after exon 27. This additional exon 27a was also observed in two controls but only in minor amount. Insertion of exon 27a does not change the reading frame and results in a stable messenger RNA (mRNA) transcript (see Supplementary data for details).
Functional investigations in patient-derived fibroblasts
In vitro studies show a decreased concentration of pyrimidine nucleotides in CAD-deficient fibroblasts (F2:II.2, UP1.1, UP5). Uridine supplementation of the culture medium corrects the decreased levels of pyrimidine nucleotides in these cells (Fig. 2b, c). This implies that the pyrimidine salvage pathway is able to completely replenish the pyrimidine nucleotide pools and should restore the biochemical processes dependent on pyrimidine metabolites. Noteworthy is that CAD cells show a decrease in adenosine triphosphate (ATP) content of 15–20% upon supplementation with uridine. The decrease in ATP could be caused by depletion of ATP due to phosphorylation of uridine to UMP.
Clinical patient characteristics
Key clinical data are summarized in Table 2, and the detailed case reports can be found in the Supplementary data. The individuals (9 females, 11 males, 18 Caucasian, 2 Asian) presented at a median age of 15 months (range 3 days to 7 years) with GDD (12/20; 60%); seizures (10/20; 50%); anemia (2/20; 10%); and regression, ataxia, muscular hypotonia, autistic features, and failure to thrive (each 1/20; 5%). The median age at last follow-up was 6 years (range 9 months to 43 years), and three individuals were deceased at a median age of 5 years (range 4 to 9 years). During the course of disease, GDD and/or intellectual disability (ID) were seen in all patients and seizures were seen in all but two patients (18/20; 90%). Anemia was seen in all patients with exception of UP8, which might be attributable to his young age of 9 months.
Eight of the previously unpublished individuals (UP2, UP3.1, UP4, UP5, UP7-10) showed essentially the same course as four of the previously published individuals (F1:II.3, F2:II.2, F3:II.4, FiN) with delayed development, progressive epileptic encephalopathy with difficult to control seizures and/or recurrent (super-refractory) status epilepticus, and loss of skills (12/20 [60%]). Of note, two individuals (UP1.1, UP1.2) showed isolated DD/ID without seizures during the follow-up of 8 and 2 years, respectively. For two individuals (UP6.1, UP6.2), the diagnosis was made at the age of 41 and 43 years, respectively; both females were followed for ID/DD, ataxia, seizures, and variable anemia. They lost the ability to walk and became wheelchair dependent due to ataxia by the age of 38 and 21 years, respectively. They never experienced a status epilepticus but their seizures were at times difficult to control.
In our initial report we did not mention the hyperkinetic movements of individuals F1:I.:3 and F3:II.4 as we attributed them to the terminal phase of disease.2 Within the entire cohort we found ataxia in 6/20 (30%) of patients and tremor in 3/20 (19%); in three additional children an unsteady broad based gait was seen.
Individual UP10 was prenatally found to have a complex brain malformation with hydrocephalus. As these kinds of congenital anomalies are very uncommon in IEMs, we consider this a separate disorder in a child with a highly consanguineous background and assume that CAD deficiency related findings presented at the age of 2 months, when the first epileptic seizure occurred.
Genotype–phenotype correlations
Within the cohort no genotype–phenotype correlations could be established, neither when correlating age of onset or age of the death with LoF or non-LoF variants (data not shown). Significant phenotypic variability, even within one family, was seen for the c.98T>G, p.Met33Arg variant. This might be attributable to environmental factors, especially the uridine content of the diet.
Neuroimaging characteristics
MRIs for re-evaluation were available from ten individuals (F1:II.2, F2:II.2, UP3.1, UP3.2, UP4, UP5, UP7–UP10); follow-up MRIs were available for all but UP8. Neuroimaging of one infant (UP8) investigated at 9 months was normal. The individuals UP3.1 and UP4 had cerebellar atrophy aged 3.3 and 4 years (Fig. 1b); five subjects had marked cerebellar and less pronounced cerebral atrophy at 3.2 years (UP9), 3.5 years (F1:II.2), 5 years (UP4), and 5.5 years (F2:II.2, UP5, Fig. 1c), respectively. Remarkably, the MRI was normal in individual UP7 at the age of 3.7 and in UP3.2 at the age of 10.6 years. The MRIs of the published patients were not available for reanalysis, but were reported as unremarkable (1.4 years, UPD4003) and as showing progressive cerebellar and cerebral atrophy (3.6 and 5.5 years, FiN), respectively.6,10 It seems that increasing age correlates with more brain atrophy. The cerebellum seems to be affected first. Caution, however, is advised in drawing general conclusions in view of the limited number of available MRIs.
Treatment with UMP, uridine, and uridine triacetate
UMP is the central metabolite in pyrimidine metabolism (Fig. 1a). CAD deficiency impairs the de novo biosynthesis of UMP, but UMP can alternatively be synthesized from uridine via the salvage pathway.1 Uridine triacetate (UT, Xuriden) is a triacetylated prodrug of uridine and FDA-approved for UMPS deficiency (orotic aciduria, MIM 258900), the enzyme downstream of CAD in the pyrimidine biosynthesis.
Consumption of 2 g UMP by human adults raised plasma uridine levels by threefold (from 6.0 to 21.9 μM) for 5–6 hours.14 Circulating uridine crosses the blood–brain barrier via an adenosine transporter (CNT2) that is unsaturated at physiologic plasma uridine concentrations (as reviewed in Cansev et al.).14
The individuals F1:II.2 and F2:II.2 were prescribed uridine (Audor, Leppersdorf, Germany). Due to the shortage of uridine on the world market, currently all other patients except F1:II.2 and UP4 are treated with UMP as over-the-counter food supplement from various sources (e.g., Focus supplements, Jarrow). Given the molecular masses of uridine (244.20) and UMP (324.18), one should give 132.8 mg of UMP to provide 100 mg of uridine.
Uridine costs €0.2/kg/day at an assumed starting dose of 100 mg/kg/day; for UMP the approximate costs are €0.5/kg/day. UT costs $22.5/kg/d at a starting dose of 60 mg/kg/day. UP4 receives 120 mg/kg/day, which is currently 3.6 g/day and treatment costs of 1500 $/day as two capsules of 2 g have to be opened and 0.4 g has to be discarded every day.
Treatment outcome
In general, the response of the patients receiving UMP was comparable with the previously reported effect of uridine in F1:II.3 and F2:II.2. No difference was seen in the beneficial treatment response when F2:II.2 and UP10 were switched from uridine to UMP after 2 years or 3 months, respectively. The response to UT in UP4 was satisfying for correction of hematological issues, while there was only a transient improvement in seizure control and virtually no effect on development. All data are summarized in Table 3.
Data on treatment with uridine or UMP were available for 9 individuals. These are 6 previously unpublished individuals (UP3.1, UP3.2, UP5, UP7, UP9, UP10) plus an update for two previously published individuals (F1:II.3, F2:II.2) and data on one individual in the literature (FiN).
The median age at start of treatment was five years. Prescribed doses ranged between 67 and 150 mg/kg/day uridine, divided in three daily doses. Individual treatment duration ranged from 5 to 48 months (median 15.5 months); the cumulative treatment duration is 14.3 patient-years. No side effects were reported in any of the treated individuals, especially no clinical signs suggesting hyperglycemia (as reported in mice with long-term 400 mg/kg/day uridine feeding).15
Anemia and anisopoikilocytosis resolved in eight individuals within three months, only in UP7 is there still some anemia/anisopoikilocytosis after 6 months of treatment, and no follow-up blood smear was available for UP9. Improved seizure control was achieved in seven patients; in the other two, seizure control with antiepileptic drugs (AED) was already achieved before the start of treatment. Importantly, in four patients with recurrent, up to weekly, status epilepticus requiring extensive and frequent hospital admission before treatment, not a single status epilepticus was seen during treatment. In six of the individuals, AEDs could be tapered off after uridine supplementation was started. The developmental improvement varied; in individuals FiN, UP3.1, UP5, and UP7 an impressive improvement was seen. These individuals regained the ability to walk independently and especially also made improvements in communication by learning to speak in sentences of more than three words. In UP3.2, the brother of UP3.1 with a milder course of DD/ID and controlled seizures, only very little improvement of attention span and alertness was seen. The same holds for individual UP9. For F1:II.3 and F2:II.2, we can report the follow-up of 48 months of treatment. F1:II.3 (7 years) still is seizure free on uridine supplementation only. While she is progressing in all areas, her performance is below peers. She is able to walk, run, and communicate with sentences, but attends a school for children with special needs. However, her brother F1:II.2 died aged four years in a refractory status epilepticus in a minimal conscious state. While F2:II.2 initially showed an impressive improvement in seizure frequency (>100 seizures per month to seizure free), she still suffers seizures occasionally and needs three different AEDs from the earlier five, while two were stopped. She regained the ability to do some steps with a walker, has improved balance, and regained the ability to swallow and is completely fed orally. However, she seems to lack interest and motivation in learning more skills and “stays in her own world.”
Obviously, it is impossible to draw conclusions from one patient. Nevertheless, it seems that uridine triacetate did not outperform the uridine or UMP treatment strategies.
DISCUSSION
Here we have shown that biallelic CAD variants typically lead to GDD/ID, a progressive epileptic encephalopathy with difficult to control seizures and/or recurrent (super-refractory) status epilepticus and loss of skills. Additionally to this relatively homogeneous phenotype in 60% of the patients, we did observe notable phenotypic heterogeneity within the cohort. The initial report suggested a lethal course without uridine supplementation. When overlooking a bigger cohort, we can now report that indeed 15% of patients did not survive beyond the age of 4.5–9 years, but we can also report individuals showing a milder course of disease, including two untreated females with a notably longer survival of up to 43 years. Incomplete penetrance of neurological features is commonly seen in other IEMs with epilepsy and ID/DD.16
Our study further broadens the phenotypic spectrum of CAD deficiency by reporting two individuals with isolated ID without seizures up to the age of eight years. Additionally, we can add ataxia and tremor to the clinical features of CAD deficiency. This is in line with the neuroimaging features (Fig. 1b) showing that increasing age correlates with more atrophic changes, affecting the cerebellum first.
We have previously speculated about a possible correlation between breastfeeding (poor uridine source) versus bottle feeding (fortified with UMP) and the onset of seizures (6 months versus 20–24 months), as well as the influence of tube feeding formulas (fortified with UMP) on anemia.2,17 The same would hold for frequent consumption of pyrimidine-rich food like yeast-based products or organ meat. Here we report one patient who already presented neonatal onset of seizures. For him no data concerning early nutrition are available. Two siblings died in infancy with the same course of disease without a confirmed genetic diagnosis. For the majority of the other patients no data on (early) nutrition were available, which makes it impossible to further comment on this topic. Our data set does not allow concluding a better outcome in patients receiving uridine supplementation at an earlier age or with a milder course of disease. However, it seems logical that in an IEM leading to the lack of the pivotal metabolite UMP the earliest possible treatment, even before the onset of clinical signs and symptoms, could lead to a better outcome. Moreover, vice versa, delayed treatment will not be able to reverse all previous damage. CAD deficiency might represent a potential condition for genetic newborn screening.18,19
Dyserythropoietic anemia is a distinctive feature of CAD deficiency. One should be aware that this anemia is per definition normocytic, but the abnormal size distribution and morphology lead to an abnormal red cell distribution width (RCDW), a parameter included in every automated blood count. While anemia is mostly not present at the onset of seizures, it develops during the course of the disease in all patients. The anemia can be mild and nutritional uridine may correct the anemia but the anisopoikilocytosis only resolved after oral uridine supplementation. Anisopoikilocytosis with or without anemia in a patient with epilepsy may be an important indication to suspect CAD deficiency.
No biomarker is available for screening or follow-up of CAD deficiency and the final diagnosis relies on genetic testing. Of note, five of the variants in this cohort were classified as VUS. This may partly explain why only two additional patients have been reported since the original reports in 2015 and 2016.2,6,10,11,14 The assay presented by del Caño-Ochoa et al. using a CAD-knockout cell line generated by CRISP/Cas9 should largely circumvent this problem as they demonstrate the superiority of their cell-based assay over pathogenicity prediction software.9 With regard to the functional assays, there is a difference in approach. Our in vitro experiments were designed to assess the effect of uridine on the intracellular pyrimidine nucleotide concentrations. Both assays aim to predict clinical response. Our work complements that of del Caño-Ochoa et al., who demonstrate loss of CAD functionality by means of a complementation assay that allows to assess the detrimental effect of single CAD variants. However, they do not show intracellular metabolites or rescue of CAD-transfected variants by uridine supplementation. Together, the newly presented work of both research groups now provides us both with the possibility to assess the effect of genetic CAD variants and predict the clinical response to treatment with uridine or UMP. Nonetheless, CAD deficiency is yet another excellent example that a meaningful diagnosis relies on the collaboration between the (phenotyping) physician and the (variant-interpreting) genetic laboratory specialists. Further, we would like to suggest that “response to pathomechanism based treatment” should be added as an additional factor for pathogenicity to the ACMG criteria.
Treatment with the uridine supplementation in CAD deficiency is unlicensed but was shown to be successful and without side effects in ten patients. As uridine is currently unavailable on the world market, it is important to underline that treatment with UMP was as effective. Obviously, it is impossible to draw conclusions from one patient. Nevertheless, it seems that UT, which is about 45-fold more expensive, did not outperform the uridine or UMP treatment strategies.
Anemia resolved in all but one patient who showed near normalization. Clear improvement of seizure control, especially the ending of the frequently recurring status epilepticus requiring long hospital admissions, was seen in 80% of patients. In the remaining patients, seizure control was already achieved before the start of uridine. Uridine supplementation further enabled sparing of AEDs in at least half of the patients. The effect on the motor, language, and intellectual skills is more difficult to summarize and interpret. While regaining of motor or language skills was impressive in at least six patients in our study, less effect was seen in other patients. One could speculate that this might indicate a genotype–phenotype relationship or that it is dependent on the age at start of treatment, but we cannot conclude this from our data set.
In conclusion, CAD deficiency is a treatable IEM that typically presents as a progressive early infantile epileptic encephalopathy with recurrent status epilepticus, loss of skills, movement disorder, and dyserythropoietic anemia. Milder courses of DD/ID without epilepsy can occur as well as onset with neonatal seizures. No biomarker is available for screening and diagnosis relies on genetic testing. Underlying disease causing variants might be rated as VUS when following the ACMG criteria, which could lead to underrecognition of this treatable disorder. Supplementation with uridine is safe and leads to significant clinical improvement in most of the patients. We therefore advice a 6-month trial of uridine or UMP supplementation in all patients with ID/DD, epilepsy, and anemia; all patients with status epilepticus; and all patients with neonatal seizures until genetically proven otherwise or proven unsuccessful during 6 months. Furthermore, CAD deficiency might represent a potential condition for genetic newborn screening.18,19
References
Loffler M, Carrey EA, Zameitat E. New perspectives on the roles of pyrimidines in the central nervous system. Nucleosides Nucleotides Nucl Acids. 2018;37:290–306.
Koch J, Mayr JA, Alhaddad B, et al. CAD mutations and uridine-responsive epileptic encephalopathy. Brain. 2017;140:279–286.
Ng SB, Buckingham KJ, Lee C, et al. Exome sequencing identifies the cause of a mendelian disorder. Nat Genet. 2010;42:30–35.
Huguley CM Jr, Bain JA, Rivers SL, Scoggins RB. Refractory megaloblastic anemia associated with excretion of orotic acid. Blood. 1959;14:615–634.
Wortmann SB, Chen MA, Colombo R, et al. Mild orotic aciduria in UMPS heterozygotes: a metabolic finding without clinical consequences. J Inherit Metab Dis. 2017;40:423–431.
Zhou L, Xu H, Wang T, Wu Y. A patient with CAD deficiency responsive to uridine and literature review. Front Neurol. 2020;11:64.
van Karnebeek CDM, Sayson B, Lee JJY, et al. Metabolic evaluation of epilepsy: a diagnostic algorithm with focus on treatable conditions. Front Neurol. 2018;9:1016.
Bailey CJ. Orotic aciduria and uridine monophosphate synthase: a reappraisal. J Inherit Metab Dis. 2009;32(Suppl 1):S227–233.
del Caño-Ochoa F, Ng BG, Abedalthagafi M, et al. Cell-based analysis of CAD variants identifies individuals likely to benefit from uridine therapy. Genet Med. 28 May 2020; https://doi.org/10.1038/s41436-020-0833-2 [Epub ahead of print].
Ng BG, Wolfe LA, Ichikawa M, et al. Biallelic mutations in CAD, impair de novo pyrimidine biosynthesis and decrease glycosylation precursors. Hum Mol Genet. 2015;24:3050–3057.
Russo R, Andolfo I, Manna F, et al. Multi-gene panel testing improves diagnosis and management of patients with hereditary anemias. Am J Hematol. 2018;93:672–682.
Wagner M, Berutti R, Lorenz-Depiereux B, et al. Mitochondrial DNA mutation analysis from exome sequencing—a more holistic approach in diagnostics of suspected mitochondrial disease. J Inherit Metab Dis. 2019;42:909–917.
Wagner M, Levy J, Jung-Klawitter S. et al. Loss of TNR causes a nonprogressive neurodevelopmental disorder with spasticity and transient opisthotonus. Genet Med. 2020;22:1061–1068.
Cansev M. Uridine and cytidine in the brain: their transport and utilization. Brain Res Rev. 2006;52:389–397.
Urasaki Y, Pizzorno G, Le TT. Chronic uridine administration induces fatty liver and pre-diabetic conditions in mice. PLoS One. 2016;11:e0146994.
Wortmann SB, Zietkiewicz S, Kousi M, et al. CLPB mutations cause 3-methylglutaconic aciduria, progressive brain atrophy, intellectual disability, congenital neutropenia, cataracts, movement disorder. Am J Hum Genet. 2015;96:245–257.
Janas LM, Picciano MF. The nucleotide profile of human milk. Pediatr Res. 1982;16:659–662.
Andermann A, Blancquaert I, Beauchamp S, Dery V. Revisiting Wilson and Jungner in the genomic age: a review of screening criteria over the past 40 years. Bull World Health Organ. 2008;86:317–319.
Ceyhan-Birsoy O, Murry JB, Machini K, et al. Interpretation of genomic sequencing results in healthy and ill newborns: results from the BabySeq Project. Am J Hum Genet. 2019;104:76–93.
Acknowledgements
We thank Ms. Schittek (Sana Pharmacy, Düsseldorf, Germany) for ongoing efforts to provide UMP to the patients in Germany and Austria. This work was funded by the Jubiläumsfonds of the OeNB (number 18023) and a research grant restricted to CAD deficiency provided by Milupa metabolics to S.B.W.
Author information
Authors and Affiliations
Contributions
DR, JAM, JB and SBW are responsible for study design, evaluation of data, and writing of the manuscript. All authors read the manuscript and contributed intellectual content.
Corresponding author
Ethics declarations
Disclosure
The authors declare no conflicts of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Rymen, D., Lindhout, M., Spanou, M. et al. Expanding the clinical and genetic spectrum of CAD deficiency: an epileptic encephalopathy treatable with uridine supplementation. Genet Med 22, 1589–1597 (2020). https://doi.org/10.1038/s41436-020-0933-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41436-020-0933-z
Keywords
This article is cited by
-
Novel CAD gene mutations in a boy with developmental and epileptic encephalopathy 50 with dramatic response to uridine therapy: a case report and a review of the literature
BMC Pediatrics (2024)
-
Comprehensive multi-omics integration identifies differentially active enhancers during human brain development with clinical relevance
Genome Medicine (2021)
-
Treatable inherited metabolic disorders causing intellectual disability: 2021 review and digital app
Orphanet Journal of Rare Diseases (2021)
-
Molekulare Medizin: Pathobiochemie als Schlüssel zur personalisierten Therapie vererbter Krankheiten
Monatsschrift Kinderheilkunde (2021)