Abstract
Objectives
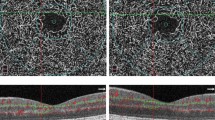
To study the changes in vessel densities (VD) stratified by vessel diameter in the retinal superficial and deep vascular complexes (SVC/DVC) using optical coherence tomography angiography (OCTA) images obtained from people with diabetes and age-matched healthy controls.
Methods
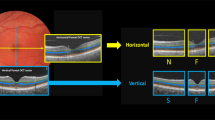
We quantified the VD based on vessel diameter categorized as <10, 10–20 and >20 μm in the SVC/DVC obtained on 3 × 3 mm2 OCTA scans using a deep learning-based segmentation and vascular graph extraction tool in people with diabetes and age-matched healthy controls.
Results
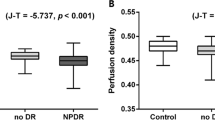
OCTA images obtained from 854 eyes of 854 subjects were divided into 5 groups: healthy controls (n = 555); people with diabetes with no diabetic retinopathy (DR, n = 90), mild and moderate non-proliferative DR (NPDR) (n = 96), severe NPDR (n = 42) and proliferative DR (PDR) (n = 71). Both SVC and DVC showed significant decrease in VD with increasing DR severity (p < 0.001). The largest difference was observed in the <10 μm vessels of the SVC between healthy controls and no DR (13.9% lower in no DR, p < 0.001). Progressive decrease in <10 μm vessels of the SVC and DVC was seen with increasing DR severity (p < 0.001). However, 10–20 μm vessels only showed decline in the DVC, but not the SVC (p < 0.001) and there was no change observed in the >20 μm vessels in either plexus.
Conclusions
Our findings suggest that OCTA is able to demonstrate a distinct vulnerability of the smallest retinal vessels in both plexuses that worsens with increasing severity of DR.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 18 print issues and online access
$259.00 per year
only $14.39 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
Sabanayagam C, Banu R, Chee ML, Lee R, Wang YX, Tan G, et al. Incidence and progression of diabetic retinopathy: a systematic review. Lancet Diabetes Endocrinol 2019;7:140–9.
De Carlo TE, Chin AT, Bonini Filho MA, Adhi M, Branchini L, Salz DA, et al. Detection of microvascular changes in eyes of patients with diabetes but not clinical diabetic retinopathy using optical coherence tomography angiography. Retina. 2015;35:2364–70.
Cao D, Yang D, Huang Z, Zeng Y, Wang J, Hu Y, et al. Optical coherence tomography angiography discerns preclinical diabetic retinopathy in eyes of patients with type 2 diabetes without clinical diabetic retinopathy. Acta Diabetol. 2018;55:469–77.
Fayed AE, Abdelbaki AM, El Zawahry OM, Fawzi AA. Optical coherence tomography angiography reveals progressive worsening of retinal vascular geometry in diabetic retinopathy and improved geometry after panretinal photocoagulation. PLoS One. 2020;14:e0226629.
Stitt AW, Lois N, Medina RJ, Adamson P, Curtis TM. Advances in our understanding of diabetic retinopathy. Clin Sci. 2013;125:1–17.
Ansari P, Tabasumma N, Snigdha NN, Siam NH, Panduru RV, Azam S, et al. Diabetic retinopathy: an overview on mechanisms, pathophysiology and pharmacotherapy. Diabetology. 2022;3:159–75.
Soares M, Neves C, Marques IP, Pires I, Schwartz C, Costa MÂ, et al. Comparison of diabetic retinopathy classification using fluorescein angiography and optical coherence tomography angiography. Br J Ophthalmol. 2017;101:62–8.
Group ETDRSR. Classification of diabetic retinopathy from fluorescein angiograms: ETDRS report number 11. Ophthalmology. 1991;98:807–22.
Oliver SC, Schwartz SD. Peripheral vessel leakage (PVL): a new angiographic finding in diabetic retinopathy identified with ultra wide-field fluorescein angiography. Pap Presente Semin Ophthalmol. 2010;25:27–33.
Fayed AE, Nesper PL, Fawzi AA. Imaging of retinal vascular disease. In: Retinal Vascular Disease. 107–125 Springer Singapore; 2020.
MacKinnon JR, McKillop G, O’Brien C, Swa K, Butt Z, Nelson P. Colour Doppler imaging of the ocular circulation in diabetic retinopathy. Acta Ophthalmol Scand. 2000;78:386–9.
Paula KY, Mehnert A, Athwal A, Sarunic MV, Yu D-Y. Use of the retinal vascular histology to validate an optical coherence tomography angiography technique. Transl Vis Sci Technol. 2021;10:29–9.
Fawzi AA, Fayed AE, Linsenmeier RA, Gao J, Yu F. Improved macular capillary flow on optical coherence tomography angiography after panretinal photocoagulation for proliferative diabetic retinopathy. Am J Ophthalmol. 2019;206:217–27.
Fayed AE, Gerges TK. Optical coherence tomography angiography reveals paradoxically decreasing choroidal thickness & increasing blood flow in remitting Vogt Koyanagi Harada syndrome. RETINA. 2022;42:1788–95.
Scarinci F, Nesper PL, Fawzi AA. Deep retinal capillary nonperfusion is associated with photoreceptor disruption in diabetic macular ischemia. Am J Ophthalmol. 2016;168:129–38.
Estawro RG, Fayed AE, Gerges TK, Baddar DN. Choriocapillaris Island: an optical coherence tomography angiography finding observed in central serous chorioretinopathy. Int J Retin Vitreous. 2021;7:1–8.
Ashraf M, Nesper PL, Jampol LM, Yu F, Fawzi AA. Statistical model of optical coherence tomography angiography parameters that correlate with severity of diabetic retinopathy. Invest Ophthalmol Vis Sci. 2018;59:4292–8.
Carnevali A, Sacconi R, Corbelli E, Tomasso L, Querques L, Zerbini G, et al. Optical coherence tomography angiography analysis of retinal vascular plexuses and choriocapillaris in patients with type 1 diabetes without diabetic retinopathy. Acta Diabetol. 2017;54:695–702.
Spaide RF, Fujimoto JG, Waheed NK. Image artifacts in optical coherence angiography. Retina (Phila, Pa). 2015;35:2163.
Menten MJ, Paetzold JC, Dima A, Menze BH, Knier B, Rueckert D. Physiology-based simulation of the retinal vasculature enables annotation-free segmentation of OCT angiographs. Paper presented at: Medical Image Computing and Computer Assisted Intervention–MICCAI 2022: 25th International Conference, Singapore, September 18–22, 2022, Proceedings, Part VIII2022.
Kreitner L, Paetzold JC, Rauch N, Chen C, Hagag AM, Fayed AE, et al. Synthetic optical coherence tomography angiographs for detailed retinal vessel segmentation without human annotations. IEEE Trans Med Imaging. 2024. https://doi.org/10.1109/TMI.2024.3354408. Online ahead of print.
Wang X, Wei Q, Wu X, Cao S, Chen C, Zhang J, et al. The vessel density of the superficial retinal capillary plexus as a new biomarker in cerebral small vessel disease: an optical coherence tomography angiography study. Neurol Sci. 2021;42:3615–24.
Hirano T, Toriyama Y, Takamura Y, Sugimoto M, Nagaoka T, Sugiura Y, et al. Outcomes of a 2-year treat-and-extend regimen with aflibercept for diabetic macular edema. Sci Rep. 2021;11:4488.
Pak KY, Shin JP, Kim HW, Sagong M, Kim YC, Lee SJ, et al. One-year results of treatment of diabetic macular edema with aflibercept using the treat-and-extend dosing regimen: the VIBIM study. Ophthalmologica. 2020;243:255–62.
Curry BA, Sanfilippo PG, Chan S, Hewitt AW, Verma N. Clinical outcomes of a treat and extend regimen with intravitreal aflibercept injections in patients with diabetic macular edema: experience in clinical practice. Ophthalmol Ther. 2020;9:87–101.
Wilkinson C, Ferris FL, Klein RE, Lee PP, Agardh CD, Davis M, et al. Proposed international clinical diabetic retinopathy and diabetic macular edema disease severity scales. Ophthalmology. 2003;110:1677–82.
Jia Y, Tan O, Tokayer J, Potsaid B, Wang Y, Liu JJ, et al. Split-spectrum amplitude-decorrelation angiography with optical coherence tomography. Opt Express. 2012;20:4710–25.
Campbell J, Zhang M, Hwang T, Bailey S, Wilson D, Jia Y, et al. Detailed vascular anatomy of the human retina by projection-resolved optical coherence tomography angiography. Sci Rep. 2017;7:42201.
Giarratano Y, Bianchi E, Gray C, Morris A, MacGillivray T, Dhillon B, et al. Automated segmentation of optical coherence tomography angiography images: benchmark data and clinically relevant metrics. Transl Vis Sci Technol. 2020;9:5–5.
Isensee F, Jaeger PF, Kohl SA, Petersen J, Maier-Hein KH. nnU-Net: a self-configuring method for deep learning-based biomedical image segmentation. Nat Methods. 2021;18:203–11.
Kreitner L, Paetzold JC, Rauch N, Chen C, Hagag AM, Fayed AE, et al. Detailed retinal vessel segmentation without human annotations using simulated optical coherence tomography angiographs. arXiv preprint arXiv:230610941. 2023.
Meyer-Spradow J, Ropinski T, Mensmann J, Hinrichs K. Voreen: a rapid-prototyping environment for ray-casting-based volume visualizations. IEEE Comput Graph Appl. 2009;29:6–13.
Paetzold JC, McGinnis J, Shit S, Ezhov I, Büschl P, Prabhakar C, et al. Whole brain vessel graphs: a dataset and benchmark for graph learning and neuroscience. Paper presented at: Thirty-fifth Conference on Neural Information Processing Systems Datasets and Benchmarks Track (Round 2)2021.
Gardiner TA, Archer DB, Curtis TM, Stitt AW. Arteriolar involvement in the microvascular lesions of diabetic retinopathy: implications for pathogenesis. Microcirculation. 2007;14:25–38.
Stitt A, Anderson H, Gardiner T, Archer D. Diabetic retinopathy: quantitative variation in capillary basement membrane thickening in arterial or venous environments. Br J Ophthalmol. 1994;78:133–7.
Hogan MJ, Feeney L. The ultrastructure of the retinal vessels: II. The small vessels. J Ultrastruct Res. 1963;9:29–46.
Mohammed S, Li T, Chen XD, Warner E, Shankar A, Abalem MF, et al. Density-based classification in diabetic retinopathy through thickness of retinal layers from optical coherence tomography. Sci Rep. 2020;10:15937.
Sohn EH, van Dijk HW, Jiao C, Kok PH, Jeong W, Demirkaya N, et al. Retinal neurodegeneration may precede microvascular changes characteristic of diabetic retinopathy in diabetes mellitus. Proc Natl Acad Sci. 2016;113:E2655–E2664.
Harris A, Arend O, Danis RP, Evans D, Wolf S, Martin BJ. Hyperoxia improves contrast sensitivity in early diabetic retinopathy. Br J Ophthalmol. 1996;80:209–13.
Harris A, Arend O, Bohnke K, Kroepfl E, Danis R, Martin B. Retinal blood flow during dynamic exercise. Graefes Arch Clin Exp Ophthalmol. 1996;234:440–4.
Balaratnasingam C, An D, Hein M, Yu P, Yu D-Y. Studies of the retinal microcirculation using human donor eyes and high-resolution clinical imaging: Insights gained to guide future research in diabetic retinopathy. Prog Retin Eye Res. 2022;94:101134.
An D, Yu P, Freund KB, Yu D-Y, Balaratnasingam C. Three-dimensional characterization of the normal human parafoveal microvasculature using structural criteria and high-resolution confocal microscopy. Invest Ophthalmol Vis Sci. 2020;61:3–3.
Falcão M, Falcão-Reis F, Rocha-Sousa A. Diabetic retinopathy: understanding pathologic angiogenesis and exploring its treatment options. Open Circ Vasc J. 2010;3:30–42.
Niki T, Muraoka K, Shimizu K. Distribution of capillary nonperfusion in early-stage diabetic retinopathy. Ophthalmology. 1984;91:1431–9.
Lavia C, Couturier A, Erginay A, Dupas B, Tadayoni R, Gaudric A. Reduced vessel density in the superficial and deep plexuses in diabetic retinopathy is associated with structural changes in corresponding retinal layers. PLoS One. 2019;14:e0219164.
AttaAllah HR, Mohamed AAM, Ali MA. Macular vessels density in diabetic retinopathy: quantitative assessment using optical coherence tomography angiography. Int Ophthalmol. 2019;39:1845–59.
An D, Pulford R, Morgan WH, Yu D-Y, Balaratnasingam C. Associations between capillary diameter, capillary density, and microaneurysms in diabetic retinopathy: a high-resolution confocal microscopy study. Transl Vis Sci Technol 2021;10:6–6.
Nesper PL, Roberts PK, Onishi AC, Chai H, Liu L, Jampol LM, et al. Quantifying microvascular abnormalities with increasing severity of diabetic retinopathy using optical coherence tomography angiography. Invest Ophthalmol Vis Sci. 2017;58:BIO307–15.
Hirano T, Kitahara J, Toriyama Y, Kasamatsu H, Murata T, Sadda S. Quantifying vascular density and morphology using different swept-source optical coherence tomography angiographic scan patterns in diabetic retinopathy. Br J Ophthalmol. 2019;103:216–21.
Sim DA, Keane PA, Rajendram R, Karampelas M, Selvam S, Powner MB, et al. Patterns of peripheral retinal and central macula ischemia in diabetic retinopathy as evaluated by ultra-widefield fluorescein angiography. Am J Ophthalmol. 2014;158:144–153.e141.
Silva PS, Liu D, Glassman AR, Aiello LP, Grover S, Kingsley RM, et al. Assessment of fluorescein angiography nonperfusion in eyes with diabetic retinopathy using ultrawide field retinal imaging. Retina. 2022;42:1302–10.
Author information
Authors and Affiliations
Contributions
AEF, MM AMH and SS conceptualized the project. AEF, SB and RRF collected the imaging and patient information. MM, LK, JCP and DR performed the data analysis. AMH performed the statistical analysis. AEF wrote the manuscript. All authors contributed to reviewing the manuscript.
Corresponding author
Ethics declarations
Competing interests
AF: None, MM: None, LK: None, JCP: None, DR: None, SB: None, AH: Boehringer Ingelheim Ltd (E), SS: Bayer (F), Novartis (F), Abbvie (F), Roche (F), Boehringer Ingelheim (F), Optos (F), EyeBiotech (F), Biogen (F)Apellis (F), Janssen Pharmaceuticals (F), Ocular Therapeutix (F), OcuTerra (F). SS is a member of the Eye Editorial Board.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Fayed, A.E., Menten, M.J., Kreitner, L. et al. Retinal vasculature of different diameters and plexuses exhibit distinct vulnerability in varying severity of diabetic retinopathy. Eye (2024). https://doi.org/10.1038/s41433-024-03021-4
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41433-024-03021-4