Abstract
Background
To investigate the effect of perioperative intraocular pressure (IOP) lowering medications on controlling postoperative IOP following uncomplicated phacoemulsification.
Methods
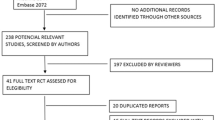
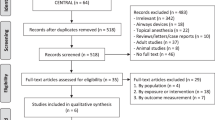
Ovid MEDLINE, EMBASE, and Cochrane CENTRAL databases were searched up until November 2022. Randomised controlled trials (RCTs) that assessed IOP change via applanation tonometry in medicated and control arms following uncomplicated cataract surgery in healthy eyes were included. The primary outcome was the weighted mean difference (WMD) of IOP at 2–8 h, 12–24 h, and 1–7 days postoperatively within each medication class or common fixed-combination formulations. Risk of bias was assessed using the revised risk of bias in randomised trials (RoB-2). Level of evidence was rated using the Grading of Recommendation, Assessment, Development and Evaluation (GRADE)
Results
From 702 screened articles, 30 RCTs involving 2986 eyes were included. There was a statistically significant reduction in IOP favouring treatment arms at 2–8 h (WMD = −3.87 mmHg; 95% CI [−4.75, −3.00]; p < 0.001) and 12–24 h (WMD = −2.69 mmHg; 95% CI [−3.36, −2.02]; p < 0.001), with the effect wearing off beyond 1 day (p = 0.18). Between medication classes, the largest effect at both 2–8 h and 12–24 h was observed with intracameral cholinergics or fixed-combination carbonic anhydrase inhibitor-beta-blocker (FCCB) formulations. Conversely, the smallest effect was observed with prostaglandin analogues, alpha-agonists, and topical carbonic anhydrase inhibitors (CAIs).
Conclusion
Prophylaxis against acute IOP elevations following uncomplicated cataract surgery is effective. FCCB and intracameral cholinergics are the most effective ocular antihypertensive agents, while alpha-agonists, prostaglandin analogues, and topical CAIs were found to be the least effective. These findings may inform future surgical guidelines.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 18 print issues and online access
$259.00 per year
only $14.39 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout








Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
Lundstrom M, Goh PP, Henry Y, Salowi MA, Barry P, Manning S, et al. The changing pattern of cataract surgery indications: a 5-year study of 2 cataract surgery databases. Ophthalmology. 2015;122:31–8.
Lundstrom M, Barry P, Henry Y, Rosen P, Stenevi U. Visual outcome of cataract surgery; study from the European Registry of Quality Outcomes for Cataract and Refractive Surgery. J Cataract Refract Surg. 2013;39:673–9.
Day AC, Donachie PH, Sparrow JM, Johnston RL. Royal College of Ophthalmologists’ National Ophthalmology D. The Royal College of Ophthalmologists’ National Ophthalmology Database study of cataract surgery: report 1, visual outcomes and complications. Eye. 2015;29:552–60.
Ahmed II, Kranemann C, Chipman M, Malam F. Revisiting early postoperative follow-up after phacoemulsification. J Cataract Refract Surg. 2002;28:100–8.
Hildebrand GD, Wickremasinghe SS, Tranos PG, Harris ML, Little BC. Efficacy of anterior chamber decompression in controlling early intraocular pressure spikes after uneventful phacoemulsification. J Cataract Refract Surg. 2003;29:1087–92.
Rainer G, Schmid KE, Findl O, Sacu S, Kiss B, Heinzl H, et al. Natural course of intraocular pressure after cataract surgery with sodium hyaluronate 1% versus hydroxypropylmethylcellulose 2%. Ophthalmology. 2007;114:1089–93.
Rainer G, Menapace R, Schmid KE, Sacu S, Kiss B, Heinze G, et al. Natural course of intraocular pressure after cataract surgery with sodium chondroitin sulfate 4%-sodium hyaluronate 3% (Viscoat). Ophthalmology. 2005;112:1714–8.
Henry JC, Olander K. Comparison of the effect of four viscoelastic agents on early postoperative intraocular pressure. J Cataract Refract Surg. 1996;22:960–6.
Passo MS, Ernest JT, Goldstick TK. Hyaluronate increases intraocular pressure when used in cataract extraction. Br J Ophthalmol. 1985;69:572–5.
Holzer MP, Tetz MR, Auffarth GU, Welt R, Volcker HE. Effect of Healon5 and 4 other viscoelastic substances on intraocular pressure and endothelium after cataract surgery. J Cataract Refract Surg. 2001;27:213–8.
Whitehouse G. Brimonidine and postoperative pressure spikes in cataract surgery. Clin Exp Ophthalmol. 2000;28:364–6.
Rainer G, Menapace R, Findl O, Petternel V, Kiss B, Georgopoulos M. Effect of topical brimonidine on intraocular pressure after small incision cataract surgery. J Cataract Refract Surg. 2001;27:1227–31.
Katsimpris JM, Siganos D, Konstas AG, Kozobolis V, Georgiadis N. Efficacy of brimonidine 0.2% in controlling acute postoperative intraocular pressure elevation after phacoemulsification. J Cataract Refract Surg. 2003;29:2288–94.
Holm JL, Bach-Holm D, Holm LM, Vestergaard AH. Prophylactic treatment of intraocular pressure elevation after uncomplicated cataract surgery in nonglaucomatous eyes - a systematic review. Acta Ophthalmol. 2019;97:545–57.
Secretariat on Responsible Conduct of R, Canadian Institutes of Health R, Natural S, Engineering Research Council C, Social S, Humanities Research Council of C. Tri-council policy statement : ethical conduct for research involving humans. Ottawa, Ontario: Secretariat on Responsible Conduct of Research; 2022. Available from: http://central.bac-lac.gc.ca/.redirect?app=damspub&id=0ab0f8e2-ddb4-4330-8498-8e235944dfc2. https://publications.gc.ca/collections/collection_2023/irsc-cihr/RR4-2-2023-eng.pdf. https://ethics.gc.ca/eng/policy-politique_tcps2-eptc2_2022.html.
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ. 2021;372:n71.
Sterne JAC, Savović J, Page MJ, Elbers RG, Blencowe NS, Boutron I, et al. RoB 2: a revised tool for assessing risk of bias in randomised trials. BMJ. 2019;366:l4898.
Guyatt GH, Oxman AD, Vist GE, Kunz R, Falck-Ytter Y, Alonso-Coello P, et al. GRADE: an emerging consensus on rating quality of evidence and strength of recommendations. BMJ. 2008;336:924–6.
Wedrich A, Menapace R. Intraocular pressure following small-incision cataract surgery and polyHEMA posterior chamber lens implantation. A comparison between acetylcholine and carbachol. J Cataract Refract Surg. 1992;18:500–5.
Unal M, Yucel I. Effect of bimatoprost on intraocular pressure after cataract surgery. Can J Ophthalmol. 2008;43:712–6.
Ulas F, Balbaba M, Celebi S. Effect of prophylactic intraocular pressure-lowering medication on pain during cataract surgery. J Ocul Pharm Ther. 2013;29:658–62.
Turk A, Ceylan OM, Gokce G, Borazan M, Kola M. Comparison of brimonidine-timolol and dorzolamide-timolol in the management of intraocular pressure increase after phacoemulsi fi cation. Int J Ophthalmol. 2015;8:945–9.
Solomon KD, Stewart WC, Hunt HH, Stewart JA, Cate EA. Intraoperative intracameral carbachol in phacoemulsification and posterior chamber lens implantation. Am J Ophthalmol. 1998;125:36–43.
Scuderi G, Regine F, Perdicchi A, Mannino G, Recupero SM. Comparative efficacy of acetazolamide and apraclonidine in the control of intraocular pressure following phacoemulsification. Ophthalmologica. 2006;220:356–60.
Rainer G, Menapace R, Schmetterer K, Findl O, Georgopoulos M, Vass C. Effect of dorzolamide and latanoprost on intraocular pressure after small incision cataract surgery. J Cataract Refract Surg. 1999;25:1624–9.
Rainer G, Menapace R, Findl O, Sacu S, Schmid K, Petternel V, et al. Effect of a fixed dorzolamide-timolol combination on intraocular pressure after small-incision cataract surgery with Viscoat. J Cataract Refract Surg. 2003;29:1748–52.
Pharmakakis N, Giannopoulos K, Stasinos S, Makri OE, Georgakopoulos CD. Effect of a fixed brimonidine-timolol combination on intraocular pressure after phacoemulsification. J Cataract Refract Surg. 2011;37:279–83.
Ozkurt Y, Oral Y, Karacan O, Comez A, Dogan OK. Comparison of the effects of dorzolamide-timolol fixed combination and brimonidine on intraocular pressure after phacoemulsification surgery. Eye Contact Lens. 2008;34:21–3.
Ornek K, Buyuktortop N, Ornek N, Ogurel R, Erbahceci IE, Onaran Z. Effect of 1% brinzolamide and 0.5% timolol fixed combination on intraocular pressure after cataract surgery with phacoemulsification. Int J Ophthalmol. 2013;6:851–4.
Onal S, Gozum N, Gucukoglu A. Effect of apraclonidine versus dorzolamide on intraocular pressure after phacoemulsification. Ophthalmic Surg Lasers Imaging. 2005;36:457–62.
Lai JS, Chua JK, Loo A, Ho SY, Lam DS. Effect of intracameral acetylcholine on latanoprost in preventing ocular hypertension after phacoemulsification and intraocular lens implantation. J Cataract Refract Surg. 2001;27:700–5.
Lai JS, Chua JK, Leung AT, Lam DS. Latanoprost versus timolol gel to prevent ocular hypertension after phacoemulsification and intraocular lens implantation. J Cataract Refract Surg. 2000;26:386–91.
Kocak-Altintas AG, Anayol MA, Cakmak HB, Simsek S. Effects of topical dorzolamide on IOP after phacoemulsification with different types of ophthalmic viscosurgical devices. Eur J Ophthalmol. 2007;17:38–44.
Kir E, Cakmak H, Dayanir V. Medical control of intraocular pressure with brinzolamide 1% after phacoemulsification. Can J Ophthalmol. 2008;43:559–62.
Kasetti SR, Desai SP, Sivakumar S, Sunderraj P. Preventing intraocular pressure increase after phacoemulsification and the role of perioperative apraclonidine. J Cataract Refract Surg. 2002;28:2177–80.
Georgakopoulos CD, Makri OE, Plotas P, Pharmakakis N. Brinzolamide-timolol fixed combination for the prevention of intraocular pressure elevation after phacoemulsification. Clin Exp Ophthalmol. 2013;41:662–7.
Georgakopoulos CD, Kagkelaris K, Pagoulatos D, Plotas P, Makri OE. Brinzolamide-brimonidine fixed combination for the prevention of intraocular pressure elevation after phacoemulsification. Eur J Ophthalmol. 2020;30:293–8.
Ermis SS, Ozturk F, Inan UU. Comparing the effects of travoprost and brinzolamide on intraocular pressure after phacoemulsification. Eye. 2005;19:303–7.
Erdogan H, Ozec AV, Caner C, Toker MI, Arici MK, Topalkara A. Effect of latanoprost/timolol and dorzolamide/tiomolol on intraocular pressure after phacoemulsification surgery. Int J Ophthalmol. 2011;4:190–4.
Dayanir V, Ozcura F, Kir E, Topaloglu A, Ozkan SB, Aktunc T. Medical control of intraocular pressure after phacoemulsification. J Cataract Refract Surg. 2005;31:484–8.
Cetinkaya A, Akman A, Akova YA. Effect of topical brinzolamide 1% and brimonidine 0.2% on intraocular pressure after phacoemulsification. J Cataract Refract Surg. 2004;30:1736–41.
Cekic O, Batman C. Effect of intracameral carbachol on intraocular pressure following clear corneal phacoemulsification. Eye. 1999;13:209–11.
Borazan M, Karalezli A, Akman A, Akova YA. Effect of antiglaucoma agents on postoperative intraocular pressure after cataract surgery with Viscoat. J Cataract Refract Surg. 2007;33:1941–5.
Bomer TG, Lagreze WD, Funk J. Intraocular pressure rise after phacoemulsification with posterior chamber lens implantation: effect of prophylactic medication, wound closure, and surgeon’s experience. Br J Ophthalmol. 1995;79:809–13.
Arici MK, Erdogan H, Toker I, Vural A, Topalkara A. The effect of latanoprost, bimatoprost, and travoprost on intraocular pressure after cataract surgery. J Ocul Pharm Ther. 2006;22:34–40.
Erdogan H, Toker MI, Arici MK, Topalkara A. Effect of latanoprost 0.005% and brimonidine 0.2% on intraocular pressure after phacoemulsification and intraocular lens implantation surgery. Jpn J Ophthalmol. 2004;48:600–1.
Hutzelmann J, Owens S, Shedden A, Adamsons I, Vargas E. Comparison of the safety and efficacy of the fixed combination of dorzolamide/timolol and the concomitant administration of dorzolamide and timolol: a clinical equivalence study. International Clinical Equivalence Study Group. Br J Ophthalmol. 1998;82:1249–53.
Goni FJ, Brimonidine/Timolol Fixed Combination Study G. 12-week study comparing the fixed combination of brimonidine and timolol with concomitant use of the individual components in patients with glaucoma and ocular hypertension. Eur J Ophthalmol. 2005;15:581–90.
Berson FG, Patterson MM, Epstein DL. Obstruction of aqueous outflow by sodium hyaluronate in enucleated human eyes. Am J Ophthalmol. 1983;95:668–72.
Rosenberg LF, Krupin T, Ruderman J, McDaniel DL, Siegfried C, Karalekas DP, et al. Apraclonidine and anterior segment laser surgery. Comparison of 0.5% versus 1.0% apraclonidine for prevention of postoperative intraocular pressure rise. Ophthalmology. 1995;102:1312–8.
Lee AJ, McCluskey P. Fixed combination of topical brimonidine 0.2% and timolol 0.5% for glaucoma and uncontrolled intraocular pressure. Clin Ophthalmol. 2008;2:545–55.
Costagliola C, dell’Omo R, Romano MR, Rinaldi M, Zeppa L, Parmeggiani F. Pharmacotherapy of intraocular pressure: part I. Parasympathomimetic, sympathomimetic and sympatholytics. Expert Opin Pharmacother. 2009;10:2663–77.
Civan MM, Macknight AD. The ins and outs of aqueous humour secretion. Exp Eye Res. 2004;78:625–31.
Sugrue MF. Pharmacological and ocular hypotensive properties of topical carbonic anhydrase inhibitors. Prog Retin Eye Res. 2000;19:87–112.
Nieminen T, Lehtimaki T, Maenpaa J, Ropo A, Uusitalo H, Kahonen M. Ophthalmic timolol: plasma concentration and systemic cardiopulmonary effects. Scand J Clin Lab Invest. 2007;67:237–45.
Orzalesi N, Rossetti L, Bottoli A, Fogagnolo P. Comparison of the effects of latanoprost, travoprost, and bimatoprost on circadian intraocular pressure in patients with glaucoma or ocular hypertension. Ophthalmology. 2006;113:239–46.
Schwenn O, Xia N, Krummenauer F, Dick HB. [Prevention of early postoperative increase in intraocular pressure after phacoemulsification. Comparison of different antiglaucoma drugs]. Ophthalmologe 2001;98:934–43.
Olson RJ, Braga-Mele R, Chen SH, Miller KM, Pineda R 2nd, Tweeten JP, et al. Cataract in the Adult Eye Preferred Practice Pattern(R). Ophthalmology. 2017;124:P1–P119.
Canadian Ophthalmological Society Cataract Surgery Clinical Practice Guideline Expert C. Canadian Ophthalmological Society evidence-based clinical practice guidelines for cataract surgery in the adult eye. Can J Ophthalmol. 2008;43:S7–57.
Acknowledgements
Financial disclosures: MMP, AS, CH: none. RK: Allergan/Abbvie. IIKA: Alcon, Johnson & Johnson Vision, Bausch Health, Santen, Carl Zeiss AG, Aequus, Akorn, Aquea Health, Inc, ArcScan, Beaver Visitec, Beyeonics, Centricity Vision, Inc, CorNeat Vision, Costum Surgical, ELT Sight, ElutiMed, Equinox, Genentech, Gore, Iantrek, InjectSense, Iridex, iStar, LayerBio, Leica Microsystems, Long Bridge Medical, Inc, MicroOptx, New World Medical, Ocular Instruments, Ocular Therapeutix, Oculo, Omega Ophthalmics, PolyActiva, Radiance Therapeutics, Ripple Therapeutics, Sanoculis, Shifamed, LLC, Sight Sciences, Smartlens, Inc, Stroma, Thea Pharma, ViaLase, Vizzario. HS: Alcon/Novartis, Allergan/Abbvie, Bausch Health, Glaukos, Labtician Thea, Aerie Pharmaceuticals, Johnson & Johnson, Ivantis, Zeiss.
Author information
Authors and Affiliations
Contributions
Designing/revising the protocol: RK, MMP, AS, CH, IIKA, HS. - Conducting the search and screening the studies: RK, MMP, AS, HS - Extracting and analysing the data: RK, MMP, AS, HS - Interpreting the results: RK, MMP, AS, CH, IIK, HS - Writing the report and creating figures/tables: RK, MMP, AS, HS - Critically revising the paper: RK, MMP, AS, CH, IIKA, HS.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval
The study protocol was reviewed by the McGill University’s Faculty of Medicine Institutional Review Board and was exempt from ethics review based on article 2.2(b) of the Tri-Council Policy Statement: Ethical Conduct for Research Involving Humans. The study adhered to the tenets of the Declaration of Helsinki.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
41433_2024_2940_MOESM4_ESM.pdf
Supplementary Table 4: Grading of Recommendations, Assessment, Development, and Evaluation (GRADE) Summary of Findings Table
41433_2024_2940_MOESM6_ESM.pdf
Supplementary Figure 1: Modified Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) Flow Diagram.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kanjee, R., Popovic, M.M., Salimi, A. et al. Prophylaxis against intraocular pressure spikes following uncomplicated phacoemulsification: a systematic-review and meta-analysis. Eye (2024). https://doi.org/10.1038/s41433-024-02940-6
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41433-024-02940-6