Abstract
Purpose
To report the clinical course of corneal ulceration/perforation in patients with Sjogren’s syndrome.
Methods
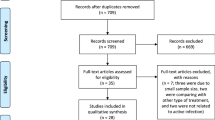
Retrospective descriptive study of patients diagnosed with Sjogren’s syndrome (primary and secondary) and corneal ulceration over past 8 years at tertiary eye care network. Assessed parameters were demographics, clinical details, microbiological profile, types of intervention and their outcomes.
Results
Forty-six eyes of 44 patients (11 males; mean age, 50 years) had corneal ulceration (28 eyes) or perforation (18 eyes) at the time of presentation. Of 46 eyes, 38 had sterile ulceration/perforation and rest 8 showed microorganism on microscopy or culture. The location was peripheral in 63% of eyes and it was the first presenting sign of Sjogren’s syndrome in 26% of patients. All 43 eyes (3 lost to follow-up after intervention) had successful management of corneal ulceration/perforation. Twenty-eight eyes with ulceration required medical management alone in 15 eyes, soft contact lens and isobutylcyanoacrylate in 12 eyes, and amniotic membrane grafting in one eye. Four eyes with ulceration worsened and required penetrating keratoplasty (n = 2), and amniotic membrane grafting (n = 2). Corneal perforations were successfully managed with isobutylcyanoacrylate patch and BCL (n = 15), corneal patch graft (n = 2) and multilayered amniotic membrane grafting (n = 1). The average time taken for ulcers to heal was 49 days over a mean follow-up duration of 10 months.
Conclusion
Corneal ulceration or perforation in Sjogren’s syndrome is often sterile and can be a presenting sign of undiagnosed SS. These patients usually respond to intensive medical therapy and bandage contact lens and isobutylcyanoacrylate patch application.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 18 print issues and online access
$259.00 per year
only $14.39 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
Data availability
Raw data is available with authors and can be shared upon reasonable request.
References
Singh S, Das AV, Basu S. Ocular involvement in Sjögren syndrome: Risk factors for severe visual impairment and vision-threatening corneal complications. Am J Ophthalmol. 2020;225:11–7.
Akpek EK, Mathews P, Hahn S, Hessen M, Kim J, Grader-Beck T, et al. Ocular and systemic morbidity in a longitudinal cohort of Sjögren’s syndrome. Ophthalmology 2015;122:56–61.
Krachmer JH, Laibson PR. Corneal thinning and perforation in Sjögren’s syndrome. Am J Ophthalmol. 1974;78:917–20.
Cohen KL. Sterile corneal perforation after cataract surgery in Sjögren’s syndrome. Br J Ophthalmol. 1982;66:179–82.
Gudas PP Jr, Altman B, Nicholson DH, Green WR. Corneal perforations in Sjögren syndrome. Arch Ophthalmol. 1973;90:470–2.
Vivino FB, Minerva P, Huang CH, Orlin SE. Corneal melt as the initial presentation of primary Sjögren’s syndrome. J Rheumatol. 2001;28:379–82.
Murtagh P, Comer R, Fahy G. Corneal perforation in undiagnosed Sjögren’s syndrome following topical NSAID and steroid drops post routine cataract extraction. BMJ Case Rep. 2018;2018:bcr2018225428.
Ou JI, Manche EE. Corneal perforation after conductive keratoplasty in a patient with previously undiagnosed Sjögren syndrome. Arch Ophthalmol. 2007;125:1131–2.
Petroutsos G, Drosos A, Psilas K. Repeated melting of corneal grafts in a patient with rheumatoid arthritis and Sjögren’s syndrome. Eur J Ophthalmol. 1992;2:36–8.
Bernauer W, Ficker LA, Watson PG, Dart JK. The management of corneal perforations associated with rheumatoid arthritis. An analysis of 32 eyes. Ophthalmology. 1995;102:1325–37.
Shiboski SC, Shiboski CH, Criswell L, Baer A, Challacombe S, Lanfranchi H, et al. American College of Rheumatology classification criteria for Sjogren’s syndrome: a data-driven, expert consensus approach in the Sjogren’s International Collaborative Clinical Alliance cohort. Arthritis Care Res. 2012;64:475–87.
Sharma S, Kunimoto DY, Gopinathan U, Athmanathan S, Garg P, Rao GN. Evaluation of corneal scraping smear examination methods in the diagnosis of bacterial and fungal keratitis: a survey of eight years of laboratory experience. Cornea 2002;21:643–7.
Karampatakis V, Konidaris V, Michailidou M, Gerofotis A, Daniilidis M. Peripheral corneal ulceration associated with rheumatoid arthritis. Am J Case Rep. 2013;14:318–21.
Tuominen IS, Konttinen YT, Vesaluoma MH, Moilanen JA, Helintö M, Tervo TM. Corneal innervation and morphology in primary Sjögren’s syndrome. Invest Ophthalmol Vis Sci. 2003;44:2545–9.
Pfister RR, Murphy GE. Corneal ulceration and perforation associated with Sjögren’s syndrome. Arch Ophthalmol. 1980;98:89–94.
Tzamalis A, Matsou A, Anastasopoulos E, Ziakas N. Treatment of spontaneous corneal perforation secondary to undiagnosed Sjögren’s syndrome using regenerating agent and autologous serum eye drops. Eur J Ophthalmol. 2021;31:NP17–21.
Zierhut M, Thiel HJ, Weidle EG, Waetjen R, Pleyer U. Topical treatment of severe corneal ulcers with cyclosporin A. Graefes Arch Clin Exp Ophthalmol. 1989;227:30–5.
Acknowledgements
We thank Dr Zarin Modiwala, MBBS for her support in data collection and Dr Savitri Sharma, MBBS, MD, Dr Joveeta Joseph, MBBS, DNB, Mr. Venkateshwara Rao, Mr. Balakrishna, Mrs. Renuka, Mr. Gorappa, Laboratory technicians, Jhaveri Microbiology Centre, L V Prasad Eye Institute, Hyderabad for microbiological data.
Funding
Hyderabad Eye Research Foundation (HERF), India.
Author information
Authors and Affiliations
Contributions
SS and SB were responsible for designing the study protocol, writing the protocol and IRB, conducting the literature review and writing the manuscript along with interpreting results, and creating tables. SC and AVD were responsible for extracting the data from electronic records and analysing data and interpreting results.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Singh, S., Chaudhary, S., Das, A.V. et al. Presentation, aetiology and outcomes of corneal ulceration in Sjogren’s Syndrome. Eye 37, 3217–3220 (2023). https://doi.org/10.1038/s41433-023-02494-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41433-023-02494-z