Abstract
Purpose
To analyse the topographic characteristics in macular choroidal thickness (mChT) and ocular biometry in myopic maculopathy and to explore the potential cut-off value for prediction of myopic maculopathy (MM).
Methods
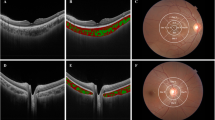
All participants underwent detailed ocular examinations. MM was subdivided into thin choroid, Bruch’s membrane (BM) defects, choroidal neovascularization (CNV), and myopic tractional maculopathy (MTM) according to OCT-based classification system. Peripapillary atrophy area (PPA), tilt ratio, torsion, and mChT were individually measured.
Results
A total of 1947 participants were included. In multivariate logistics models, older age, longer axial length, larger PPA area, and thinner average mChT were more likely to have MM and different type of MM. Female participants were more likely to have MM and BM defects. A lower tilt ratio was more likely to be associated with CNV and MTM. The area under the curve (AUC) of single tilt ratio, PPA area, torsion, and topographic of mChT for MM, thin choroid, BM Defects, CNV, and MTM were 0.6581 to 0.9423, 0.6564 to 0.9335, 0.6120 to 0.9554, 0.5734 to 0.9312, 0.6415 to 0.9382, respectively. After combining PPA area and average mChT for predicting MM, thin choroid, BM defects, CNV, and MTM, the AUC of the combination were 0.9678, 0.9279, 0.9531, 0.9213, 0.9317, respectively.
Conclusion
Progressive and continuous PPA area expanding and thin choroid play a role in the development of myopic maculopathy. The present study showed that a combination of peripapillary atrophy area and the choroidal thickness could be used to predict MM and each type of MM.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 18 print issues and online access
$259.00 per year
only $14.39 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
Correspondence and requests for data materials should be addressed to Jia He.
References
Morgan IG, Ohno-Matsui K, Saw S-M. Myopia. Lancet 2012;379:1739–48.
Dolgin E. The Myopia Boom. Nature. 2015;519:276–8.
Holden BA, Fricke TR, Wilson DA, Jong M, Naidoo KS, Sankaridurg P, et al. Global Prevalence of Myopia and High Myopia and Temporal Trends from 2000 through 2050. Ophthalmology 2016;123:1036–42.
Tang Y, Wang X, Wang J, Huang W, Gao Y, Luo Y, et al. Prevalence and Causes of Visual Impairment in a Chinese Adult Population: The Taizhou Eye Study. Ophthalmology. 2015;122:1480–8.
Fricke TR, Jong M, Naidoo KS, Sankaridurg P, Naduvilath TJ, Ho SM, et al. Global prevalence of visual impairment associated with myopic macular degeneration and temporal trends from 2000 through 2050: systematic review, meta-analysis and modelling. Br J Ophthalmol 2018;102:855–62.
Hsu W-M, Cheng C-Y, Liu J-H, Tsai S-Y, Chou P. Prevalence and causes of visual impairment in an elderly Chinese population in Taiwan: the Shihpai Eye Study. Ophthalmology. 2004;111:62–9.
Verhoeven VJM, Wong KT, Buitendijk GHS, Hofman A, Vingerling JR, Klaver CCW. Visual consequences of refractive errors in the general population. Ophthalmology 2015;122:101–9.
Buch H, Vinding T, Cour ML, Appleyard M, Jensen GB, Nielsen NV. Prevalence and causes of visual impairment and blindness among 9980 Scandinavian adults - The Copenhagen City Eye Study. Ophthalmology. 2004;111:53–61.
Zhao X, Ding X, Lyu C, Li S, Liu B, Li T, et al. Morphological Characteristics and Visual Acuity of Highly Myopic Eyes with Different Severities of Myopic Maculopathy. Retina. 2020;40:461–7.
Ohno-Matsui K, Kawasaki R, Jonas JB, Cheung CMG, Saw S-M, Verhoeven VJM, et al. International photographic classification and grading system for myopic maculopathy. Am J Ophthalmol. 2015;159:877–83-e877.
Fang Y, Du R, Nagaoka N, Yokoi T, Shinohara K, Xu X, et al. OCT-Based Diagnostic Criteria for Different Stages of Myopic Maculopathy. Ophthalmology 2019;126(Jul):1018–32.
Ruiz-Medrano J, Montero JA, Flores-Moreno I, Arias L, García-Layana A, Ruiz-Moreno JM. Myopic maculopathy: Current status and proposal for a new classification and grading system (ATN). Prog Retin Eye Res. 2019;69:80–115.
Fang Y, Yokoi T, Nagaoka N, Shinohara K, Onishi Y, Ishida T, et al. Progression of Myopic Maculopathy during 18-Year Follow-up. Ophthalmology 2018;125:863–77.
Chen Q, He J, Hu G, Xu X, Lv H, Yin Y, et al. Morphological Characteristics and Risk Factors of Myopic Maculopathy in an Older High Myopia Population-Based on the New Classification System (ATN). Am J Ophthalmol. 2019;208(Dec):356–66.
Xie J, Ye L, Chen Q, Shi Y, Hu G, Yin Y, et al. Choroidal thickness and its association with age, axial length, and refractive error in chinese adults. Invest Ophthalmol Vis Sci. 2022;63(Feb):34.
L Ye, Q Chen, G Hu, Y Shi, G Hu, Y Yin, et al. Distribution and association of visual impairment with myopic maculopathy across age groups among highly myopic eyes - based on the new classification system (ATN). Acta Ophthalmol. 2022;100:e957–67.
Bennett AG, Rudnicka AR, Edgar DF. Improvements on Littmann’s method of determining the size of retinal features by fundus photography. Graefes Arch Clin Exp Ophthalmol. 1994;232:361–7.
Hu G, Chen Q, Xu X, Lv H, Du Y, Wang L, et al. Morphological Characteristics of the Optic Nerve Head and Choroidal Thickness in High Myopia. Invest Ophthalmol Vis Sci. 2020;61(Apr):46.
Wong Y-L, Sabanayagam C, Ding Y, Wong CW, Yeo AC, Cheung Y-B, et al. Prevalence, Risk Factors, and Impact of Myopic Macular Degeneration on Visual Impairment and Functioning Among Adults in Singapore. Invest Ophthalmol Vis Sci. 2018;59:4603–13.
Hopf S, Korb C, Nickels S, Schulz A, Münzel T, Wild PS, et al. Prevalence of myopic maculopathy in the German population: results from the Gutenberg health study. Br J Ophthalmol. 2020;104(Sep):1254–9.
Dai Y, Jonas JB, Huang H, Wang M, Sun X. Microstructure of parapapillary atrophy: beta zone and gamma zone. Invest Ophthalmol Vis Sci. 2013;54:2013–8.
Vianna JR, Malik R, Danthurebandara VM, Sharpe GP, Belliveau AC, Shuba LM, et al. Beta and Gamma Peripapillary Atrophy in Myopic Eyes With and Without Glaucoma. Investigative Opthalmology Vis Sci. 2016;57:3103.
Kim M, Choung H-K, Lee KM, Oh S, Kim SH. Longitudinal Changes of Optic Nerve Head and Peripapillary Structure during Childhood Myopia Progression on OCT: Boramae Myopia Cohort Study Report 1. Ophthalmology 2018;125:1215–23.
Almeida I, Ushida M, Lins I, Dias DT, Prata TS. Peripapillary Atrophy in Myopic Eyes: Comparison of Gamma to Beta Zone Ratio Between Those With and Without Glaucoma. Invest Ophthalmol Vis Sci. 2016;57(Nov):6031.
Jonas JB, Wang YX, Zhang Q, Fan YY, Xu L, Wei WB, et al. Parapapillary Gamma Zone and Axial Elongation-Associated Optic Disc Rotation: The Beijing Eye Study. Invest Ophthalmol Vis Sci. 2016;57:396–402.
Ohno-Matsui K, Jonas JB, Spaide RF. Macular Bruch’s Membrane Holes in Highly Myopic Patchy Chorioretinal Atrophy. Am J Ophthalmol. 2016;166:22–8.
Tay E, Seah SK, Chan S-P, Lim ATH, Chew S-J, Foster PJ, et al. Optic disk ovality as an index of tilt and its relationship to myopia and perimetry. Am J Ophthalmol. 2005;139:247–52.
How ACS, Tan GSW, Chan Y-H, Wong TTL, Seah SK, Foster PJ, et al. Population prevalence of tilted and torted optic discs among an adult Chinese population in Singapore: the Tanjong Pagar Study. Arch Ophthalmol. 2009;127:894–9.1.
Kim T-W, Kim M, Weinreb RN, Woo SJ, Park KH, Hwang J-M. Optic disc change with incipient myopia of childhood. Ophthalmology 2012;119:21–6-e1-3.
Samarawickrama C, Mitchell P, Tong L, Gazzard G, Lim L, Wong T-Y, et al. Myopia-related optic disc and retinal changes in adolescent children from singapore. Ophthalmology 2011;118:2050–7.
Neelam K, Cheung CG, Ohno-Matsui K, Lai TYY, Wong TY. Choroidal neovascularization in pathological myopia. Prog retinal eye Res. 2012;31:495–525.
Wong TY, Ferreira A, Hughes R, Carter G, Mitchell P. Epidemiology and disease burden of pathologic myopia and myopic choroidal neovascularization: an evidence-based systematic review. Am J Ophthalmol. 2014;157:9–25-e12.
Acknowledgements
This study was funded by Shanghai Public Health System Three-Year Plan Personnel Construction Subjects (Project No.GWV-10.2-YQ40, GWV-10.1-XK7) Shanghai Shenkang Hospital Clinical Research Program (Project No. SHDC12019X18). The sponsors or funding organizations had no role in the design or conduct of this research. The authors had no proprietary or commercial interest in any materials discussed in this manuscript. All authors attest that they meet the current ICMJE criteria for authorship.
Author information
Authors and Affiliations
Contributions
JH, LY, CC, QC, DS, JX, YF, JZ, XX, and JH were involved in the study design and conduct. JH, GH, YS, QC, YY, LY, HZ, and JH were involved in data collection, management, and analysis. JH and LY interpreted the data. JH, LY, QC, and YF were involved in manuscript preparation, review, or approval.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics statement
The study was designed following the ethical standards of the Declaration of Helsinki and approved by the ethical committee of Shanghai General Hospital, Shanghai Jiao Tong University, Shanghai, China.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
He, J., Ye, L., Chu, C. et al. Using a combination of peripapillary atrophy area and choroidal thickness for the prediction of different types of myopic maculopathy. Eye 37, 2801–2809 (2023). https://doi.org/10.1038/s41433-023-02423-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41433-023-02423-0