Abstract
Objectives
To determine 36-month efficacy and safety outcomes of the PRESERFLO Microshunt implant in the treatment of refractory uveitic glaucoma.
Methods
Consecutive patients with uncontrolled uveitic glaucoma despite maximum medical treatment received PRESERFLO Microshunt implant with mitomycin C (MMC) in a tertiary referral glaucoma practice. Efficacy and safety outcomes data were collected at month 6, 12, 24, and 36, postoperatively.
The primary outcome was surgical success, defined as intraocular pressure (IOP) between 5 and 21 mmHg or > 20% reduction from baseline, and absence of criteria for surgical failure. Secondary outcomes were IOP, visual acuity (VA), use of glaucoma medical therapy, surgical complications, rate of reoperation for glaucoma.
Results
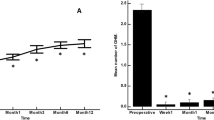
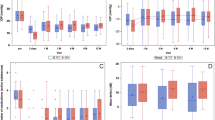
21 eyes of 21 patients were included. The mean rate of success was 0.74 (95%CI 0.48–0.88), 0.68 (0.43–0.84), 0.47 (0.25–0.67), and 0.47 (0.25–0.67, at 6, 12, 24, and 36 months postoperatively, respectively. The mean IOP decreased by 30.7% (95% CI 13.7–47.7), 26.5% (95% CI 3.2–49.8), 33.5% (95% CI 21.8–45.3), and 30.1% (95% CI 7.2–52.9) from baseline at postoperative month 6, 12, 24, and 36, respectively (p < 0.001). The mean ± SD number of glaucoma medications decreased from 4.1 ± 0.9 to 0.9 ± 1.2 at the final follow up (p = 0.0005). No sight-threatening complications were reported by 36 months.
Conclusions
Three-year results of the PRESERFLO Microshunt implant demonstrated favourable efficacy and safety profile in the treatment of refractory uveitic glaucoma.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 18 print issues and online access
$259.00 per year
only $14.39 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author, KB, upon reasonable request.
References
Al-Ani HH, Sims JL, Tomkins-Netzer O, Lightman S, Niederer RL. Vision loss in anterior uveitis. Br J Ophthalmol. 2020;104:1652–7.
Aman R, Engelhard SB, Bajwa A, Patrie J, Reddy AK. Ocular hypertension and hypotony as determinates of outcomes in uveitis. Clin Ophthalmol. 2015;9:2291–8.
Sng CCA, Ang M, Barton K. Uveitis and glaucoma: new insights in the pathogenesis and treatment. Prog Brain Res. 2015;221:243–69.
Liu X, Kelly SR, Montesano G, Bryan SR, Barry RJ, Keane PA, et al. Evaluating the Impact of Uveitis on Visual Field Progression Using Large-Scale Real-World Data. Am J Ophthalmol. 2019;207:144–50.
Din NM, Talat L, Isa H, Tomkins-Netzer O, Barton K, Lightman S. Difference in glaucoma progression between the first and second eye after consecutive bilateral glaucoma surgery in patients with bilateral uveitic glaucoma. Graefe’s Arch Clin Exp Ophthalmol. 2016;254:2439–48.
Ho CL, Wong EYM, Walton DS. Goniosurgery for glaucoma complicating chronic childhood uveitis. Arch Ophthalmol (Chic, Ill 1960) 2004;122:838–44.
Heinz C, Koch JM, Zurek-Imhoff B, Heiligenhaus A. Prevalence of uveitic secondary glaucoma and success of nonsurgical treatment inadults and children in a tertiary referral center. Ocul Immunol Inflamm. 2009;17:243–8.
Wang Q, Wang J, Fortin E, Hamel P. Trabeculotomy in the Treatment of Pediatric Uveitic Glaucoma. J Glaucoma. 2016;25:744–9.
Ceballos EM, Beck AD, Lynn MJ. Trabeculectomy with antiproliferative agents in uveitic glaucoma. J Glaucoma. 2002;11:189–96.
Kaburaki T, Koshino T, Kawashima H, Numaga J, Tomidokoro A, Shirato S, et al. Initial trabeculectomy with mitomycin C in eyes with uveitic glaucoma with inactive uveitis. Eye. 2009;23:1509–17.
Papadaki TG, Zacharopoulos IP, Pasquale LR, Christen WB, Netland PA, Foster CS. Long-term results of Ahmed glaucoma valve implantation for uveitic glaucoma. Am J Ophthalmol. 2007;144:62–69.
Ceballos EM, Parrish RK, Schiffman JC. Outcome of Baerveldt glaucoma drainage implants for the treatment of uveitic glaucoma. Ophthalmology 2002;109:2256–60.
Borisuth NS, Phillips B, Krupin T. The risk profile of glaucoma filtration surgery. Curr Opin Ophthalmol. 1999;10:112–6.
Krishna R, Godfrey DG, Budenz DL, Escalona-Camaano E, Gedde SJ, Greenfield DS, et al. Intermediate-term outcomes of 350-mm(2) Baerveldt glaucoma implants. Ophthalmology 2001;108:621–6.
Landers J, Martin K, Sarkies N, Bourne R, Watson P. A twenty-year follow-up study of trabeculectomy: risk factors and outcomes. Ophthalmology 2012;119:694–702.
Chaku M, Bajwa A, Lee JK, Netland PA. Treatment of Uveitis and Outcomes of Glaucoma Drainage Implant Surgery: A Meta-Analysis. Ocul Immunol Inflamm. 2020;28:833–8.
Kerr NM, Wang J, Barton K. Minimally invasive glaucoma surgery as primary stand-alone surgery for glaucoma. Clin Exp Ophthalmol. 2017;45:393–400.
Sng CC, Wang J, Hau S, Htoon HM, Barton K. XEN-45 collagen implant for the treatment of uveitic glaucoma. Clin Exp Ophthalmol. 2018;46:339–45.
Kerr NM, Wang J, Sandhu A, Harasymowycz PJ, Barton K. Ab Interno Gel Implant-associated Bleb-related Infection. Am J Ophthalmol. 2018;189:96–101.
Gedde SJ, Chen PP, Heuer DK, Singh K, Wright MM, Feuer WJ, et al. The primary tube versus trabeculectomy study: Methodology of a multicenter randomized clinical trial comparing tube shunt surgery and trabeculectomy with Mitomycin C. Ophthalmology 2018;125:774–81.
Gedde SJ, Schiffman JC, Feuer WJ, Parrish RK 2nd, Heuer DK, Brandt JD. The tube versus trabeculectomy study: design and baseline characteristics of study patients. Am J Ophthalmol. 2005;140:275–87.
Batlle JF, Fantes F, Riss I, Pinchuk L, Alburquerque R, Kato YP, et al. Three-year follow-up of a novel aqueous humor microshunt. J Glaucoma. 2016;25:e58–65.
Schlenker MB, Durr GM, Michaelov E, Ahmed IIK. Intermediate outcomes of a novel standalone Ab Externo SIBS microshunt with Mitomycin C. Am J Ophthalmol. 2020;215:141–53.
Bhayani R, Martinez de la Casa JM, Figus M, Klabe K, Rabiolo A, Mercieca K. Short-term safety and efficacy of Preserflo™ Microshunt in glaucoma patients: A multicentre retrospective cohort study. Eye (Lond). 2022;12:1–6.
Broadway DC, Bates AK, Lightman SL, Grierson I, Hitchings RA. The importance of cellular changes in the conjunctiva of patients with uveitic glaucoma undergoing trabeculectomy. Eye (Lond). 1993;7:495–501.
Ni M, Chan CC, Nussenblatt RB, Li SZ, Mao W. Iris inflammatory cells, fibronectin, fibrinogen, and immunoglobulin in various ocular diseases. Arch Ophthalmol (Chic, Ill 1960) 1988;106:392–5.
Chow A, Burkemper B, Varma R, Rodger DC, Rao N, Richter GM. Comparison of surgical outcomes of trabeculectomy, Ahmed shunt, and Baerveldt shunt in uveitic glaucoma. J Ophthalmic Inflamm Infect. 2018;8:9.
Vinod K, Gedde SJ, Feuer WJ, Panarelli JF, Chang TC, Chen PP, et al. Practice preferences for glaucoma surgery: A survey of the American glaucoma society. J Glaucoma. 2017;26:687–93.
Do AT, Parikh H, Panarelli JF. Subconjunctival microinvasive glaucoma surgeries: An update on the Xen gel stent and the PreserFlo MicroShunt. Curr Opin Ophthalmol. 2020;31:132–8.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Author information
Authors and Affiliations
Contributions
GT: Conceptualization, Methodology, Formal analysis, Investigation, Data curation, Writing – Original draft, Writing – Review & Editing; JW: Conceptualization, Investigation; Soledad SA-M: Methodology, Investigation, Data curation; HJ: Formal analysis, Writing – Review & Editing; KB: Conceptualization, Writing – Review & Editing; Supervision.
Corresponding author
Ethics declarations
Competing interests
Keith Barton lectured and consulted for Santen, receiving compensation. The rest of co-authors declare no competing financial interests related to the topic of this paper.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Triolo, G., Wang, J., Aguilar-Munoa, S. et al. Preserflo microshunt implant for the treatment of refractory uveitic glaucoma: 36-month outcomes. Eye 37, 2535–2541 (2023). https://doi.org/10.1038/s41433-022-02368-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41433-022-02368-w
This article is cited by
-
XEN®-45 implantation for refractory uveitic glaucoma
Graefe's Archive for Clinical and Experimental Ophthalmology (2024)