Abstract
Objective
To evaluate the accuracy of the ABCD Progression Display and the ABCD grading system in a population of adult patients with keratoconus.
Methods
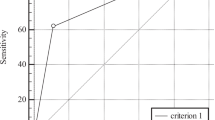
A retrospective cohort analysis of all adult patients with keratoconus followed at the Shamir Medical Center between 2012 and 2017. A recommendation by the cornea specialist to undergo corneal crosslinking (CXL) was used as a surrogate of ectasia progression. The ABCD grading was not available to the treating physician and was computed post-hoc. Sensitivity and specificity of the ABCD Progression Display was calculated, and multivariate regression was used to estimate the risk to undergo CXL when the ABCD Progression Display indicated progression. The ABCD grading was compared between patients who required CXL to those who did not. A single eye of each patient was included. Sensitivity and specificity of the ABCD Progression Display were 82% and 73%, respectively. A multivariable model adjusted for possible confounders, found that ABCD Progression was associated with a 7-fold risk of undergoing CXL compared to a patient in whom progression was not recorded in the ABCD Progression Display (OR = 7.55; 95% CI = 3.82–14.93, p < 0.001).
Results
293 eyes of 293 patients were analysed. Mean age at presentation was 26.92 ± 6.12 years. In 68 eyes, progression of keratoconus was recorded and CXL was performed (CXL-group).
Conclusion
The ABCD Progression Display demonstrated adequate sensitivity and specificity and high predictive capabilities of keratoconus progression. It can be effectively utilized as an initial screening test in adults with keratoconus.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 18 print issues and online access
$259.00 per year
only $14.39 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
Data availability
The datasets generated and/or analyzed during the current study are available from the corresponding author on reasonable request.
Change history
03 February 2023
A Correction to this paper has been published: https://doi.org/10.1038/s41433-022-02296-9
References
Krachmer JH, Feder RS, Belin MW. Keratoconus and related noninflammatory corneal thinning disorders. Surv Ophthalmol. 1984;28:293–322.
Rabinowitz YS. Keratoconus. Surv Ophthalmol. 1998;42:297–319.
Meiri Z, Keren S, Rosenblatt A, Sarig T, Shenhav L, Varssano D. Efficacy of corneal collagen cross-linking for the treatment of Keratoconus: A systematic review and meta-analysis. Cornea 2016;35:417–28.
Sklar JC, Wendel C, Zhang A, Chan CC, Yeung SN, Iovieno A. Did collagen cross-linking reduce the requirement for corneal transplantation in Keratoconus? The Canadian experience. Cornea 2019;38:1390–4.
Wittig-Silva C, Chan E, Islam FMA, Wu T, Whiting M, Snibson GR. A randomized, controlled trial of corneal collagen cross-linking in progressive keratoconus: three-year results. Ophthalmology 2014;121:812–21.
Chatzis N, Hafezi F. Progression of keratoconus and efficacy of pediatric [corrected] corneal collagen cross-linking in children and adolescents. J Refractive Surg (Thorofare, N. J: 1995). 2012;28:753–8.
Kanellopoulos AJ, Asimellis G. Revisiting keratoconus diagnosis and progression classification based on evaluation of corneal asymmetry indices, derived from Scheimpflug imaging in keratoconic and suspect cases. Clin Ophthalmol (Auckl, N. Z). 2013;7:1539–48.
Belin MW, Duncan JK. Keratoconus: The ABCD Grading System. Klinische Monatsblatter Fur Augenheilkd. 2016;233:701–7.
Belin MW, Villavicencio OF, Ambrósio RR. Tomographic parameters for the detection of keratoconus: suggestions for screening and treatment parameters. Eye Contact Lens. 2014;40:326–30.
Balparda K, Herrera-Chalarca T, Silva-Quintero LA, Torres-Soto SA, Segura-Muñoz L, Vanegas-Ramirez CM. Both subjective emotional distress and visual handicap correlate with Belin ABCD classification in the worse eye as measured with the “Keratoconus End-Points Assessment Questionnaire” (KEPAQ). Clin Ophthalmol (Auckl, N. Z). 2020;14:1839–45.
Sedaghat M-R, Momeni-Moghaddam H, Belin MW, Zarei-Ghanavati S, Akbarzadeh R, Sabzi F, et al. Changes in the ABCD keratoconus grade after intracorneal ring segment implantation. Cornea 2018;37:1431–7.
Belin MW, Alizadeh R, Torres-Netto EA, Hafezi F, Ambrósio R, Pajic B. Determining progression in ectatic corneal disease. Asia-Pac J Ophthalmol (Phila, Pa). 2020;9:541–8.
Dubinsky-Pertzov B, Reinhardt O, Gazit I, Or L, Hecht I, Pras E, et al. The ABCD keratoconus grading system-a useful tool to estimate keratoconus progression in the pediatric population. Cornea 2021;40:1322–9.
Krumeich JH, Daniel J, Knülle A. Live-epikeratophakia for keratoconus. J Cataract Refractive Surg. 1998;24:4.
Shetty R, Rao H, Khamar P, Sainani K, Vunnava K, Jayadev C, et al. Keratoconus screening indices and their diagnostic ability to distinguish normal from ectatic corneas. Am J Ophthalmol. 2017;181:140–8.
Poli M, Lefevre A, Auxenfans C, Burillon C. Corneal collagen cross-linking for the treatment of progressive corneal ectasia: 6-year prospective outcome in a French population. Am J Ophthalmol. 2015;160:654–62.e1.
Gomes JAP, Tan D, Rapuano CJ, Belin MW, Ambrósio R, Guell JL, et al. Glob Consens Keratoconus Ectatic Dis: Cornea. 2015;34:359–69.
Godefrooij DA, Soeters N, Imhof SM, Wisse RPL. Corneal Cross-Linking for Pediatric Keratoconus: Long-Term Results. Cornea 2016;35:954–8.
Anon. Gomes et al. - 2015 - Global Consensus on Keratoconus and Ectatic Diseas.pdf.
Mas Tur V, MacGregor C, Jayaswal R, O’Brart D, Maycock N. A review of keratoconus: Diagnosis, pathophysiology, and genetics. Surv Ophthalmol. 2017;62:770–83.
Wollensak G, Spoerl E, Seiler T. Riboflavin/ultraviolet-a-induced collagen crosslinking for the treatment of keratoconus. Am J Ophthalmol. 2003;135:620–7.
Spoerl E, Mrochen M, Sliney D, Trokel S, Seiler T. Safety of UVA-riboflavin cross-linking of the cornea. Cornea 2007;26:385–9.
Raiskup-Wolf F, Hoyer A, Spoerl E, Pillunat LE. Collagen crosslinking with riboflavin and ultraviolet-A light in keratoconus: long-term results. J Cataract Refractive Surg. 2008;34:796–801.
Kamiya K, Ishii R, Shimizu K, Igarashi A. Evaluation of corneal elevation, pachymetry and keratometry in keratoconic eyes with respect to the stage of Amsler-Krumeich classification. Br J Ophthalmol. 2014;98:459–63.
Khachikian SS, Belin MW, Ciolino JB. Intrasubject corneal thickness asymmetry. J Refractive Surg. 2008;24:606–9.
Uçakhan ÖÖ, Özkan M, Kanpolat A. Corneal thickness measurements in normal and keratoconic eyes: Pentacam comprehensive eye scanner versus noncontact specular microscopy and ultrasound pachymetry. J Cataract Refractive Surg. 2006;32:970–7.
Kawana K, Miyata K, Tokunaga T, Kiuchi T, Hiraoka T, Oshika T. Central corneal thickness measurements using orbscan II scanning slit topography, noncontact specular microscopy, and ultrasonic pachymetry in eyes with keratoconus. Cornea 2005;24:967–71.
Ozalp O, Atalay E. Belin ABCD progression display identifies keratoconus progression earlier than conventional metrics: Belin ABCD display detects keratoconus progression earlier. Am J Ophthalmol. 2021;S0002-9394:00524–9.
Ambrósio R, Belin MW. Imaging of the cornea: Topography vs tomography. J Refractive Surg (Thorofare, N. J: 1995). 2010;26:847–9.
Kanellopoulos AJ, Asimellis G. OCT corneal epithelial topographic asymmetry as a sensitive diagnostic tool for early and advancing keratoconus. Clin Ophthalmol (Auckl, N. Z). 2014;8:2277–87.
Khachikian SS, Belin MW. Posterior elevation in keratoconus. Ophthalmology. 2009;116:816. 816.e1; author reply 816-817.
Acknowledgements
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
BDP was responsible for designing the protocol, interpreting results and led the writing of the manuscript. OS were responsible for extracting the data and contributed to the writing of the final manuscript. IG was responsible for extracting the data. LO and AS were responsible for analysing data and interpreting results. IH contributed to result interpretation and the writing of the final manuscript. EP contributed to the protocol design, interpretation of results and writing the final manuscript. AEL devised and supervised the project and the main conceptual ideas, contributed to the final manuscript. All authors discussed the results and contributed to the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval
The study was conducted in accordance with the tenets of the Declaration of Helsinki, and approval was obtained from the institutional review board.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this article was revised: The Abstract was given incomplete: The last sentences under Methods was missing. The missing sentence is: Sensitivity and specificity of the ABCD Progression Display were 82% and 73%, respectively. A multivariable model adjusted for possible confounders, found that ABCD Progression was associated with a 7-fold risk of undergoing CXL compared to a patient in whom progression was not recorded in the ABCD Progression Display (OR = 7.55; 95% CI = 3.82–14.93, p < 0.001).
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Dubinsky-Pertzov, B., Segal, O., Hecht, I. et al. Predictive accuracy of the ABCD progression display among patients with keratoconus: A historic cohort analysis. Eye 37, 1834–1839 (2023). https://doi.org/10.1038/s41433-022-02242-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41433-022-02242-9