Abstract
Background
Glaucoma is the commonest cause of irreversible blindness worldwide. As it is typically asymptomatic until advanced, the risk of blindness from late presentation is higher than other eye diseases. This study aims to investigate the risk factors for late presentation of primary glaucoma patients.
Methods
We undertook a hospital-based case-control study of a random sample of glaucoma patients from a hospital in Hong Kong. Structured questionnaires and existing information from the electronic patient record were used, and the odds of presenting late were analysed by logistic regression.
Results
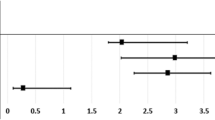
Of 210 recruited participants, 83 (39.5%) presented with advanced glaucoma unilaterally or bilaterally. The mean age of participants was 61.1 ± 11.9 years, with 110 males (52.4%). Univariate analysis revealed that male sex and primary angle-closure glaucoma (PACG) have 3.06 (CI95:1.71–5.48; P < 0.001) and 2.47 (CI95:1.11–5.49; P = 0.03) times higher odds of late presentation, respectively. Multivariate analysis revealed late presenters were 3.54 (CI95:1.35–9.35; P = 0.01) times more likely to have PACG than primary open-angle glaucoma (POAG). Patients with elevated baseline intraocular pressure (IOP) also had 1.06 times higher odds of presenting with advanced glaucoma (CI95:1.02–1.11; P = 0.002). Linear regression revealed that PACG patients present with 7.12 mmHg higher IOP than POAG patients (CI95:4.23–10.0; P < 0.001).
Conclusion
In conclusion, a high proportion of glaucoma patients present late in Hong Kong, with gender and type of glaucoma being significant determinants. Our study shows that PACG presents with higher IOP and, along with male gender, are more likely to have advanced disease than POAG.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 18 print issues and online access
$259.00 per year
only $14.39 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
Data availability
Deidentified individual participant data that underlies the results reported in this article are available for sharing. Data will be available upon request immediately following publication and ending 5 years following article publication, with investigators whose proposed use of the data has been approved by an independent review committee identified for this purpose. Proposals should be directed to laianakinlai2@gmail.com.
References
Foster PJ, Buhrmann R, Quigley HA, Johnson GJ. The definition and classification of glaucoma in prevalence surveys. Br J Ophthalmol. 2002;86:238–42.
Quigley HA, Broman AT. The number of people with glaucoma worldwide in 2010 and 2020. Br J Ophthalmol. 2006;90:262–7.
Vajaranant TS, Nayak S, Wilensky JT, Joslin CE. Gender and glaucoma: what we know and what we need to know. Curr Opin Ophthalmol. 2010;21:91–9.
Wu J, Mak HK, Chan YK, Lin C, Kong C, Leung CKS, et al. An in vitro pressure model towards studying the response of primary retinal ganglion cells to elevated hydrostatic pressures. Sci Rep. 2019;9:9057.
Quaranta L, Riva I, Gerardi C, Oddone F, Floriani I, Konstas AG. Quality of Life in Glaucoma: A Review of the Literature. Adv Ther. 2016;33:959–81.
Jonas JB, Aung T, Bourne RR, Bron AM, Ritch R, Panda-Jonas S. Glaucoma. Lancet. 2017;390:2183–93.
He M, Foster PJ, Ge J, Huang W, Zheng Y, Friedman DS, et al. Prevalence and Clinical Characteristics of Glaucoma in Adult Chinese: A Population-Based Study in Liwan District, Guangzhou. Investig Opthalmol Vis Sci. 2006;47;2782–88.
You QS, Choy BKN, Chan JCH, Ng ALK, Shih KC, Cheung JJC, et al. Prevalence and Causes of Visual Impairment and Blindness among Adult Chinese in Hong Kong—The Hong Kong Eye Study. Ophthalmic Epidemiol. 2020;27:354–63.
Chan EW, Li X, Tham YC, Liao J, Wong TY, Aung T, et al. Glaucoma in Asia: regional prevalence variations and future projections. Br J Ophthalmol. 2016;100:78–85.
Wilson R, Walker AM, Dueker DK, Crick RP. Risk Factors for Rate of Progression of Glaucomatous Visual Field Loss. Arch Ophthalmol. 1982;100:737–41.
Jay JL, Murdoch JR. The rate of visual field loss in untreated primary open angle glaucoma. Br J Ophthalmol. 1993;77:176–8.
Buys YM, Jin YP. Canadian Glaucoma Risk Factor Study G. Socioeconomic status as a risk factor for late presentation of glaucoma in Canada. Can J Ophthalmol. 2013;48:83–7.
Peters D, Bengtsson B, Heijl A. Lifetime risk of blindness in open-angle glaucoma. Am J Ophthalmol. 2013;156:724–30.
Wong PW, Lau JK, Choy BN, Shih KC, Ng AL, Chan JC, et al. Epidemiological factors associated with health knowledge of three common eye diseases: A community-based pilot survey in Hong Kong. SAGE Open. Medicine. 2020;8:1–13.
Kong X, Yang Y, Gao J, Guan J, Liu Y, Wang R, et al. Overview of the health care system in Hong Kong and its referential significance to mainland China. J Chin Med Assoc. 2015;78:569–73.
Tham YC, Li X, Wong TY, Quigley HA, Aung T, Cheng CY. Global prevalence of glaucoma and projections of glaucoma burden through 2040: a systematic review and meta-analysis. Ophthalmology. 2014;121:2081–90.
Lee Y-H, Kim C-S. Hong S-p. Rate of Visual Field Progression in Primary Open-angle Glaucoma and Primary Angle-closure Glaucoma. Korean J Ophthalmol. 2004;18:106–15.
Yip JL, Nolan WP, Davaatseren U, Baasankhuu J, Lee PS, Khaw PT, et al. Primary angle closure glaucoma in East Asia: educational attainment as a protective factor. Ophthalmic Epidemiol. 2011;18:217–25.
Baskaran M, Foo RC, Cheng CY, Narayanaswamy AK, Zheng YF, Wu R, et al. The Prevalence and Types of Glaucoma in an Urban Chinese Population: The Singapore Chinese Eye Study. JAMA Ophthalmol. 2015;133:874–80.
Adekoya BJ, Shah SP, Onakoya AO, Ayanniyi AA. Glaucoma in southwest Nigeria: clinical presentation, family history and perceptions. Int Ophthalmol. 2014;34:1027–36.
Gogate P, Deshpande R, Chelerkar V, Deshpande S, Deshpande M. Is glaucoma blindness a disease of deprivation and ignorance? A case-control study for late presentation of glaucoma in India. Indian J Ophthalmol. 2011;59:29–35.
Fraser S, Bunce C, Wormald R, Brunner E. Deprivation and late presentation of glaucoma: case-control study. Br Med J. 2001;322:639–43.
Society THKO. Ophthalmologist Directory 2021.
Shiose Y, Kitazawa Y, Tsukahara S, Akamatsu T, Mizokami K, Futa R, et al. Epidemiology of glaucoma in Japan–a nationwide glaucoma survey. Jpn J Ophthalmol. 1991;35:133–55.
Seo SJ, Lee YH, Lee SY, Bae HW, Hong S, Seong GJ, et al. Estimated Prevalence of Glaucoma in South Korea Using the National Claims Database. J Ophthalmol. 2016;2016:1690256.
Garg A, Vickerstaff V, Nathwani N, Garway-Heath D, Konstantakopoulou E, Ambler G, et al. Primary Selective Laser Trabeculoplasty for Open-Angle Glaucoma and Ocular Hypertension: Clinical Outcomes, Predictors of Success, and Safety from the Laser in Glaucoma and Ocular Hypertension Trial. Ophthalmology. 2019;126:1238–48.
Gazzard G, Konstantakopoulou E, Garway-Heath D, Garg A, Vickerstaff V, Hunter R, et al. Selective laser trabeculoplasty versus eye drops for first-line treatment of ocular hypertension and glaucoma (LiGHT): a multicentre randomised controlled trial. Lancet. 2019;393:1505–16.
Noble S, McLennan D, Noble M, Plunkett E, Gutacker N, Silk M, et al. The English Indices of Deprivation 2019.
Statistics UIf. International Standard Classification of Education: ISCED 2011. 2012.
Office IL. International Standard Classification of Occupations: Structure, group definitions and correspondence tables.
Fraser S, Bunce C, Wormald R. Retrospective analysis of risk factors for late presentation of chronic glaucoma. Br J Ophthalmol. 1999;83:24–8.
Kyari F, Abdull MM, Wormald R, Evans JR, Nolan W, Murthy GV, et al. Risk factors for open-angle glaucoma in Nigeria: results from the Nigeria National Blindness and Visual Impairment Survey. BMC Ophthalmol. 2016;16:78.
Odayappan A, Kavitha S, Ramulu ST, Upadhyaya S, Venkatesh R. Assessment of Reasons for Presentation in New Primary Glaucoma Patients and Identification of Risk Factors for Late Presentation. Ophthalmic Glaucoma. 2020;S2589-4196:30318–5.
Sukumar S, Spencer F, Fenerty C, Harper R, Henson D. The influence of socioeconomic and clinical factors upon the presenting visual field status of patients with glaucoma. Eye. 2009;23:1038–44.
Boland MV, Ervin AM, Friedman DS, Jampel HD, Hawkins BS, Vollenweider D, et al. Comparative effectiveness of treatments for open-angle glaucoma: a systematic review for the U.S. Preventive Services Task Force. Ann Intern Med. 2013;158:271–9.
Ting DSW, Cheung CY, Lim G, Tan GSW, Quang ND, Gan A, et al. Development and Validation of a Deep Learning System for Diabetic Retinopathy and Related Eye Diseases Using Retinal Images From Multiethnic Populations With Diabetes. JAMA. 2017;318:2211–23.
Hark LA, Myers JS, Ines A, Jiang A, Rahmatnejad K, Zhan T, et al. Philadelphia Telemedicine Glaucoma Detection and Follow-up Study: confirmation between eye screening and comprehensive eye examination diagnoses. Br J Ophthalmol. 2019;103:1820–6.
Acknowledgements
This project would not be possible without the help from the staff at ICEH, LSHTM and the Grantham Hospital.
Author information
Authors and Affiliations
Contributions
ACKL was responsible for the development of the methodology, data analysis method, and the drafting of the article under the supervision of JCC, JCB, and WN, JCC, JCB and WN advised on the development of the methodology, interpretation of the findings and drafting of the manuscript. All authors have read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval
This study was approved by the London School of Hygiene and Tropical Medicine Ethics Committee and the Institutional Review Board of the University of Hong Kong/Hospital Authority Hong Kong West Cluster.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Lai, A.C.K., Buchan, J.C., Chan, J.CH. et al. Determinants of late presentation of glaucoma in Hong Kong. Eye 37, 1717–1724 (2023). https://doi.org/10.1038/s41433-022-02235-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41433-022-02235-8