Abstract
Background/Objectives
Posterior Capsule Opacification (PCO) is the most common long-term post-operative adverse occurrence after cataract surgery often requiring treatment with YAG laser posterior capsulotomy. This study aimed to identify potential risk factors, known at the time of cataract surgery, that influence the development of PCO.
Subject/Methods
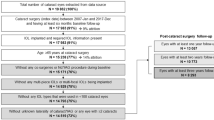
A retrospective study of publicly funded cataract surgery from The Royal College of Ophthalmologists’ National Ophthalmology Database. Eligible for analysis were 500,872 cataract operations performed in 41 participating centres.
Results
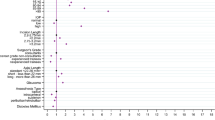
The 500,872 operations were performed on 243,167 (48.5%) left eyes and 257,705 (51.5%) right eyes from 373,579 patients by 2196 surgeons. Post-cataract PCO was recorded for 61,778 (12.3%) eyes and the six month, one, three, five and nine year observed rates of PCO were 2.3%, 4.4%, 19.7%, 34.0% and 46.9% respectively. Different PCO profiles were observed between IOL materials and the identified risk factors that increased the risk of developing PCO included hydrophilic IOL material, axial length >26 mm, the presence of high myopia and implantation of lower IOL powers and previous vitrectomy surgery, along with younger age and female gender.
Conclusions
Many factors influence the development of PCO relating to the patient, the eye, the lens and the surgery. Some factors are modifiable such as IOL material, therefore the opportunity exists to attempt to reduce PCO rates, benefitting patients and the UK NHS.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 18 print issues and online access
$259.00 per year
only $14.39 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Maedel S, Evans JR, Harrer-Seely A, Findl O. Intraocular lens optic edge design for the prevention of posterior capsule opacification after cataract surgery. Cochrane Database Syst Rev. 2021;8:CD012516.
Findl O, Buehl W, Bauer P, Sycha T. Interventions for preventing posterior capsule opacification. Cochrane Database Syst Rev. 2010;2:CD003738.
Cullin F, Busch T, Lundstrom M. Economic considerations related to choice of intraocular lens (IOL) and posterior capsule opacification frequency - a comparison of three different IOLs. Acta Ophthalmol. 2014;92:179–83.
Ursell PG, Dhariwal M, Majirska K, Ender F, Kalson-Ray S, Venerus A, et al. Three-year incidence of Nd:YAG capsulotomy and posterior capsule opacification and its relationship to monofocal acrylic IOL biomaterial: a UK Real World Evidence study. Eye. 2018;32:1579–89.
Buchan JC, Donachie PHJ, Cassels-Brown A, Liu C, Pyott A, Yip JLY, et al. The Royal College of Ophthalmologists’ National Ophthalmology Database study of cataract surgery: report 7, immediate sequential bilateral cataract surgery in the UK: Current practice and patient selection. Eye. 2020;34:1866–74.
Johansson B. Clinical consequences of acrylic intraocular lens material and design: Nd:YAG-laser capsulotomy rates in 3 × 300 eyes 5 years after phacoemulsification. Br J Ophthalmol. 2010;94:450–5.
Buchan JC, Amoaku W, Barnes B, Cassels-Brown A, Chang BY, Harcourt J, et al. How to defuse a demographic time bomb: the way forward? Eye. 2017;31:1519–22.
Zhao Y, Yang K, Li J, Huang Y, Zhu S. Comparison of hydrophobic and hydrophilic intraocular lens in preventing posterior capsule opacification after cataract surgery: An updated meta-analysis. Medicine. 2017;96:e8301.
Tokko HA, Hussain F, Al-Awadi A, Mei F, Zeiter JH, Kim C, et al. Factors associated with the development of posterior capsule opacification requiring yttrium aluminum garnet capsulotomy. Optom Vis Sci. 2019;96:492–9.
Prajna NV, Ellwein LB, Selvaraj S, Manjula K, Kupfer C. The madurai intraocular lens study IV: posterior capsule opacification. Am J Ophthalmol. 2000;130:304–9.
Zhang K, Dong Y, Zhao M, Nie L, Ding X, Zhu C. The effect of capsule tension ring on posterior capsule opacification: a meta-analysis. PLoS One. 2021;16:e0246316.
Yoshizaki M, Ramke J, Zhang JH, Aghaji A, Furtado JM, Burn H, et al. How can we improve the quality of cataract services for all? A global scoping review. Clin Exp Ophthalmol. 2021;49:672–85.
Acknowledgements
It is with gratitude that we remember our friend and colleague Robert Johnston, who sadly died in September 2016. Without his inspirational vision, determination and career long commitment to quality improvement in ophthalmology this work would not have been possible. We acknowledge the support of the hospitals that participated in this National Ophthalmology Database Audit study and thank our medical and non-medical colleagues for the considerable time and effort devoted to data collection.
The 41 centres with data in this analysis are listed in alphabetical order below separated into the regions they are located in.
English NHS trusts: Barking, Havering and Redbridge University Hospitals NHS Trust; Barts Health NHS Trust; Bradford Teaching Hospitals NHS Foundation Trust; Calderdale and Huddersfield NHS Foundation Trust; Chesterfield Royal Hospital NHS Foundation Trust; County Durham and Darlington NHS Foundation Trust; East Sussex Healthcare NHS Trust; Epsom and St Helier University Hospitals NHS Trust; Frimley Health NHS Foundation Trust; Gloucestershire Hospitals NHS Foundation Trust; Hampshire Hospitals NHS Foundation Trust; Imperial College Healthcare NHS Trust; King’s College Hospital NHS Foundation Trust; Leeds Teaching Hospitals NHS Trust; Liverpool University Hospitals NHS Foundation Trust; Mid Cheshire Hospitals NHS Foundation Trust; Moorfields Eye Hospital NHS Foundation Trust*; North West Anglia NHS Foundation Trust; Nottingham University Hospitals NHS Trust; Oxford University Hospitals NHS Foundation Trust; Portsmouth Hospitals NHS Trust; Royal Berkshire NHS Foundation Trust; Royal Cornwall Hospitals NHS Trust; Royal Devon University Healthcare NHS Foundation Trust**; Royal United Hospitals Bath NHS Foundation Trust; Salisbury NHS Foundation Trust; Sandwell and West Birmingham Hospitals NHS Trust; Sheffield Teaching Hospitals NHS Foundation Trust; South Warwickshire NHS Foundation Trust; The Hillingdon Hospitals NHS Foundation Trust; The Mid Yorkshire Hospitals NHS Trust; The Newcastle upon Tyne Hospitals NHS Foundation Trust; The Shrewsbury and Telford Hospital NHS Trust; University Hospital Southampton NHS Foundation Trust; University Hospitals Birmingham NHS Foundation Trust; University Hospitals Bristol and Weston NHS Foundation Trust; University Hospitals Coventry and Warwickshire NHS Trust; University Hospitals Plymouth NHS Trust; Wrightington, Wigan and Leigh NHS Foundation Trust; Yeovil District Hospital NHS Foundation Trust.
Guernsey: Medical specialists group Guernsey;
*Includes data from Bedford Hospital within Bedfordshire Hospitals NHS Foundation Trust and Croydon Health Services NHS Trust as the ophthalmology services in these places are part of Moorfields Eye Hospital NHS Foundation Trust.
**This NHS Trust was formed from a merger of two former NHS Trusts since the data was collected. In this analysis only data from the former Northern Devon Healthcare NHS Trust is included.
Funding
This analysis was funded by an unconditional grant from Alcon (Geneva, Switzerland) in support of the Royal College of Ophthalmologists National Ophthalmology Database cataract audit. The funders did not have any editorial oversight, right of veto or academic input into the analysis or write up of this work. The National Cataract Audit is currently funded through participation fees from centres as well as unrestricted financial contributions from Bausch + Lomb and Alcon.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Donachie, P.H.J., Barnes, B.L., Olaitan, M. et al. The Royal College of Ophthalmologists’ National Ophthalmology Database study of cataract surgery: Report 9, Risk factors for posterior capsule opacification. Eye 37, 1633–1639 (2023). https://doi.org/10.1038/s41433-022-02204-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41433-022-02204-1
This article is cited by
-
Long-term real-life outcomes of the Clareon® hydrophobic intraocular lens: the Clarte study in 191 eyes
BMC Ophthalmology (2024)
-
The Royal College of Ophthalmologists’ National Ophthalmology Database study of cataract surgery: report 16, influence of remuneration model on choice of intraocular lens in the UK
Eye (2023)
-
Hydrophobic versus hydrophilic acrylic intraocular lenses within public sector based on the type of funding contacts: the debate continues
Eye (2023)