Abstract
Purpose
To examine the safety and economic effect of using fibrin glue to reduce suturing of a donor patch graft and in conjunctival closure during aqueous shunt implantation.
Study design
Retrospective interventional case series of 150 patients from a single institution including historical controls from before the introduction of the change in technique. The surgery was performed by multiple glaucoma surgeons.
Results
One hundred and fifty eyes of 150 patients were identified. The mean age was 54.3 ± 21.1 years. Previous surgery included: cataract extraction (34.7%), trabeculectomy (36%) and retinal surgery (15.3%). All operations were carried out by either a consultant (57%) or fellow (43%). A Baerveldt Glaucoma Implant (Advanced Medical Optics, Santa Ana, California, USA) was used in 149 eyes. Conventional surgery (CS) was performed for 91 eyes and fibrin glue (FG) was used for 59 eyes. Compared with conventional surgery (CS) in which the donor patch graft and conjunctiva were sutured, use of fibrin glue (FG) reduced the overall mean operating time by 11.2 min ± 6.4 min (P = 0.031), though much less for consultants (8.5 min ± 6.2 min) (P = 0.16) than fellows (32.9 min ± 7.2 min) (P < 0.0001). There were four cases of conjunctival dehiscence—three in the FG group and one in the CS group (P = 0.30). Only one patient required re-suturing in the FG group.
Conclusions
The use of fibrin glue is safe and effective during aqueous shunt implantation. We have shown that the mean operating time can be reduced significantly with the use of fibrin glue which has significant implications for resource utilisation.
Similar content being viewed by others
Introduction
Aqueous shunt surgery is now widely performed for medically uncontrolled glaucoma both as a primary procedure and where other filtration procedures such as trabeculectomy and ab interno and ab externo stents have failed. Conventional aqueous shunt implantation may be time consuming, especially for trainees, requiring extensive suturing of the plate and tube portions of the device to sclera, to secure a donor patch graft to cover the tube and to close the conjunctiva and Tenon’s. Depending on the type of suture used, the post-operative course is often marked by suture related sequelae, particularly discomfort. This discomfort can be exacerbated by absorbable sutures, which often cause localised conjunctival inflammation [1]. Non-absorbable sutures can erode through the conjunctiva resulting in discomfort, infection, scleral patch melt and infection [2, 3]. Furthermore, suturing is often the most time-consuming step of the procedure.
Fibrin glue (FG) use during glaucoma surgery has been reported in either single or small case series during trabeculectomy [4, 5], to manage bleb leak following trabeculectomy [6], to prevent leak around the aqueous shunt implant during surgery [7] and to secure the tube, patch graft and conjunctiva during surgery [8]. However, the latter study was a small case series and concluded that further studies are needed to better understand the role of FG in aqueous shunt surgery.
We compare the duration of surgery and safety between “conventional” surgery (CS) and Fibrin glue (FG) assisted aqueous shunt surgery in a large series of patients.
Methods
Consecutive patients who underwent aqueous shunt surgery over a 7-month period, between November 2013 and May 2014, before and after the introduction of the use of FG, were obtained from our operating theatre register. All surgeons made the switch from use of sutures to fibrin glue use following its introduction. Exemption was obtained from our institutional review board to review the data.
A 250 mm2 or 350 mm2 Baerveldt Glaucoma Implant (BGI) (Advanced Medical Optics, Santa Ana, California, USA) was used in all eyes except one in whom an Ahmed Glaucoma Valve was used (New World Medical, Rancho, California, USA).
Surgical technique
Briefly, a limbal conjunctival peritomy was performed. In the majority of patients, this was in the superotemporal quadrant. A 3–0 supramid suture would be inserted into the BGI and the BGI wings were positioned under the recti muscles (between the recti muscles for the Ahmed) and secured to sclera with 9–0 polypropylene (Prolene, Ethicon, Johnson and Johnson, New Jersey, USA). The tube was then placed in the anterior chamber through a 23G or 25G hypodermic needle stab incision and secured to sclera with two 9–0 polypropylene mattress sutures. Either a scleral or human donor pericardial patch graft was secured over the tube with 10–0 nylon (Alcon, Fort Worth, USA) and the conjunctiva was closed with 7–0 Polyglactin (Vicryl, Ethicon, Johnson and Johnson, New Jersey, USA).
Tisseel (Baxter AG, Vienna, Austria) is a commercially available FG which has been approved by the US Food and Drug Administration as an adjunct to haemostasis. Tisseel is available as two preparations: a freeze dried kit (which requires reconstitution) and a prefilled syringe (frozen) preparation. The kit contains four bottles:
-
1.
Large blue bottle contains human protein concentrate which has been freeze dried and includes: clottable protein, fibrinogen, plasma fibronectin, factor XIII and plasminogen.
-
2.
Small blue bottle: contains Aprotinin solution (synthetic).
-
3.
Large black bottle: contains freeze dried human thrombin.
-
4.
Small black bottle: contains calcium chloride (activates thrombin).
The frozen preparation comes as two joined syringes (Duplojet syringe) which are thawed prior to use, avoiding the need for reconstitution.
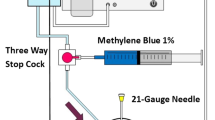
Prior to application the tissue must be dried. The two components of FG can either be applied simultaneously with the syringe (Duplojet) supplied with the product, or sequentially (using separate syringes), which we have found to be preferable as it permits greater control over the amount of glue applied to the tissues. When the latter is deployed, it is advisable to apply the thrombin first (black bottle/syringe marked with black text) followed by a thin layer of fibrinogen. Following application of the glue, a clot forms in approximately 10 s.
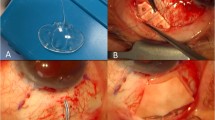
The FG assisted technique was identical to the conventional technique until after the tube had been secured to sclera. The patch graft was secured over the tube using FG (TisseelTM—Baxter AG, Vienna, Austria) applied to the under-surface of the patch and held in place with light pressure until set. Conjunctiva was approximated to the limbus using fibrin glue applied to the under surface. The conjunctiva was held in place, again with light pressure, until the glue had set. The conjunctiva was then examined for any areas of non-approximation either to limbus or conjunctiva itself (radial peritomy) and if required further FG was applied until a satisfactory approximation was obtained. At the surgeon’s discretion, either one or two 10/0 nylon horizontal mattress sutures were applied at the limbus to relieve tension on the FG. No Polyglactin sutures were used. At the end of surgery all patients received subconjunctival injections of Dexamethasone and Cefuroxime. Patients were followed up at 1 day, 1 week, 3 weeks then the further reviews were at the surgeon’s discretion.
Surgical operating times were obtained from the operating department electronic theatre management system (Galaxy international, Abu Dhabi, UAE) and data were collected and tabulated using Microsoft Excel. The cost of FG and consumables was obtained from the procurement department. Data regarding national tariffs and cost of theatre time was obtained from the hospitals finance department.
Statistical analysis was performed using SPSS (version 24 for Windows, SPSS Inc., Chicago, IL). Comparison of mean age and mean duration of the procedure between the conventional surgery (CS) and FG assisted surgery was made using an unpaired t test as our data had a normal distribution according to the Kolmogorov–Smirnov test. Comparison between the two groups for previous surgery, tube type used and tube position was made used the Chi-square test. The incidence of conjunctival dehiscence was compared using the Fisher’s exact test. A P value of 0.05 or less was considered statistically significant.
Results
One hundred and fifty eyes of 150 patients were identified of whom 91 patients underwent aqueous shunt implantation using a “conventional technique” and 59 patients who underwent the same procedure using FG. The mean age was 54.3 years (±21.1). Four-five percent (45%) of patients were female. The principle types of glaucoma were: primary open angle glaucoma (35%), uveitic (22%), secondary (19%), congenital (5%), Aphakic (5%), primary angle closure glaucoma (5%) and other secondary open angle glaucoma’s (9%). Previous surgery included cataract extraction (35%), trabeculectomy (36%) and retinal detachment repair (15%). Consultants performed 57% of all procedures with Glaucoma fellows performing the remaining 43%. With regards to the type of aqueous shunt used: 87% were a 350 mm2 BGI, 12% a 250 mm2 BGI and a single Ahmed Glaucoma valve. The plate was placed superotemporally in 91% of eyes, superonasally in 6% of eyes, inferonasal in 2% of eyes and inferotemporal in a single eye. Mitomycin C was used for 68% of eyes.
Table 1 compares the demographics, previous surgery, tube type used and tube position between the two groups and there was no statistically significant difference.
FG was used for 59 eyes (39%) of which, 89% had 10/0 nylon limbal sutures. Out of the latter group, 53% of eyes required one suture, 33% requiring two sutures and 14% had 3 or more sutures.
Table 2 compares the mean duration of surgery using CS versus the use of fibrin glue. The use of FG reduced the mean operating time for all surgeons by 11 min (P < 0.05) with the mean operating time for fellows being reduced by 32.9 min (P < 0.0001) and consultants by 8.5 min (P = 0.16).
There was no significant difference in the conjunctival retraction rate between the FG group (three cases) and convention surgery group (one case) (P = 0.30). In all cases of conjunctival retraction, a Baerveldt tube implants was used and placed superotemporally. The conjunctival retraction in the CS group occurred in a patient with previous trabeculectomy with MMC (0.2 mg/ml) at 1 week post aqueous shunt implant however, surgical intervention was not required. In the FB group, out of the three patients that had conjunctival retraction, one had no previous surgery, one had previous cyclodiode laser and the third had previous intracapsular cataract extraction and penetrating keratoplasty and required return to the operating theatre to reglue/suture the conjunctiva.
Discussion
Fibrin Glue is frequently used in anterior segment surgery [9]. It is a blood-derived product that is absorbable and relatively easy to use. FG is a biological tissue adhesive which imitates the final stages of the coagulation cascade. When human tissue is injured, the natural mechanism of wound closure includes bleeding which ceases due to formation of a blood clot. The clot is formed as a product of the final common pathway of blood coagulation. FG mimics this coagulation cascade resulting in its adhesive capability.
FG includes a fibrinogen component and a thrombin component, both prepared by processing plasma. The commercially available products are produced from pools of human plasma and contain high yields of fibrinogen and, consequently, produce firm coagulums.
Once the coagulation cascade is triggered, activated factor X selectively hydrolyses prothrombin to thrombin (Fig. 1). In the presence of thrombin, fibrinogen is converted to fibrin. Thrombin also activates factor XIII (present in the fibrinogen component of the glue), which stabilises the clot, by promoting polymerisation and cross linking of the fibrin chains to form long fibrin strands in the presence of calcium ions. This is the final common pathway for both the extrinsic and intrinsic pathways of coagulation in vivo, which is mimicked by FG to induce tissue adhesion.
There is subsequent proliferation of fibroblasts and formation of granulation tissue within hours of clot polymerisation. Clot organisation is complete 2 weeks after application. The resultant fibrin clot degrades physiologically.
Despite being vapour heat and solvent treated, as the active products are derived from human plasma, the main risk of FG, is infection—namely viral and Creutzfeldt–Jakob disease (CJD). However, there are no reported cases of infection from its use. Hypersensitivity reactions (allergic and anaphylactoid) have also been reported to occur in <1/10,000 cases. The later has been attributed to the Aprotinin synthetic component.
The use of FG during aqueous shunt surgery is limited to two small case series [7, 8]. The first study [7], used FG to tamponade intraoperative peri-tubular drainage following tube insertion, with no cases of post-operative hypotony in all 11 (of 42 eyes) in whom intraoperative peri-tubular drainage was detected. The second study used FG to secure the tube, pericardium patch graft and conjunctiva during routine aqueous shunt surgery in 14 eyes. The authors found that the use of FG compared with CS significantly reduced the operating time and conjunctival inflammation with no cases of tube or patch displacement or conjunctival retraction [8]. The latter study concluded that further studies were needed to better understand the role of FG in aqueous shunt surgery.
The greatest benefit of FG use during aqueous shunt surgery is a reduction in the operative time. In our institution, ~300 aqueous shunt procedures are performed per year of which ~130 are performed by fellows and 170 by consultants. In this study, we have observed, on average, the use of FG during aqueous shunt surgery, reduces the surgical procedure time by 11 min, although the degree of reduction in operating time appears to be inversely related to the seniority of the surgeon, with 33 min being saved for fellows and 9 min saved for consultants. This amounts to a potential total time saved of 5732 min (95.5 h) over the course of 12 months (Table 3). At the time of the study, the approximate cost of 60 min of theatre time was £1300 and therefore, from a financial perspective, this amounts to £124,150. Alternatively, the time saved could be utilised to perform other glaucoma procedures (such as cyclodiode laser or bleb needling) or cataract surgery. As cataract surgery is the commonest performed ophthalmic procedure, we have used this procedure to create a hypothetical illustration of the potential income generated from the time saved. However, the illustration could also be applied to income gained from performing additional glaucoma procedures such as cyclodiode laser or bleb needling. Assuming that a routine phacoemulsification and lens implant takes 30 min of operating theatre time, the time saved from the use of FG could potentially free operating theatre space for an additional 191 extra phacoemulsification cases in 1 year at our institution. Based on the national cataract tariff less the cost of consumables required for cataract surgery, each cataract case could earn our institution £415 pounds, amounting to a net income of £79,265. Although FG is relatively expensive costing £117 (cost to the National Health Service at the time of the study), this cost is outweighed by the ability to use the time saved to perform extra surgical cases to generate extra income. Table 4 shows a theoretical computation showing that after deducting the cost of FG, the net potential income gained from being able to use the time saved for cataract surgery is significant.
Although post-operative conjunctival inflammation assessment and patient discomfort did not form part of the study, it is of the author’s view, that the use of FG induced less post-operative conjunctival inflammation and discomfort (presumed due to the very limited use of sutures). This is supported by the findings by Kahook and Noekar [8] who found that conjunctival inflammation was statistically significantly lower in the FG group compared with the CS group. Furthermore, the use of FG obviates the need to trim/remove conjunctiva sutures post-operation—which are often the cause of patient discomfort and anxiety.
Despite the benefits of FG, it has some caveats to its use, such as: the potential risks of infection (namely viral and CJD) and hypersensitivity, the need to ensure timely approximation of tissues during use, risk of conjunctival retraction and the cost.
The main limitations of our study, is its retrospective nature, with cases non-randomised to either group. Further randomised studies are required to assess conjunctival inflammation and patient reported outcomes (namely discomfort).
Summary
What was known before
-
FG used successfully for treating peri-tubular leak FG could be used for securing the patch graft and conjunctival closure in aqueous shunt surgery (in a small case series) but larger studies were required.
What this study adds
-
Large study showing that FG use can significantly reduce the duration of aqueous shunt surgery The time saved, allows teams to increase theatre capacity at a time when theatre time/space is often limited.
References
Wong VWY, Rao SK, Lam DSC. Polyglactin sutures versus nylon sutures for suturing of conjunctival autograft in pterygium surgery: a randomized, controlled trial. Acta Ophthalmol Scand. 2007;85:658–61.
Shahinian S, Brown SL. Postoperative complications with protruding monofilament nylon sutures. Am J Ophthalmol. 1977;83:546–8.
Verinder S, Nirankari MD, Karesh JW, Richards RD. Complications of exposed monofilament sutures. Am J OphthalmoI. 1983;95:515–9.
O’Sullivan F, Dalton R, Rostron CK. Fibrin glue: an alternative method of wound closure in glaucoma surgery. J Glaucoma. 1996;5:367–70.
Seligsohn A, Moster M, Steinmann W, Fontanarosa J. Use of Tisseel fibrin sealant to manage bleb leaks and hypotony: case series. J Glaucoma. 2004;13:227.
Asrani SG, Wilensky JT. Management of bleb leaks after glaucoma filtering surgery. Use of autologous fibrin tissue glue as an alternative. Ophthalmology. 1996;103:294–8.
Valimaki J. Fibrin glue for preventing immediate postoperative hypotony following glaucoma drainage implant surgery. Acta Ophthalmol Scand. 2006;84:372–4.
Kahook MY, Noeker RJ. Fibrin-glue assisted glaucoma drainage surgery. Br J Ophthalmol. 2006;90:1486–9.
Panda A, Kumar S, Kumar A, Bansal S, Bhartiya S. Fibrin glue in ophthalmology. Indian J Ophthalmol. 2009;57:371–9.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Tailor, R., Tsaousis, K.T., Lim, LA. et al. The use of fibrin glue during aqueous shunt surgery. Eye 35, 639–643 (2021). https://doi.org/10.1038/s41433-020-0935-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41433-020-0935-8