Abstract
ARHGAP35 has known roles in cell migration, invasion and division, neuronal morphogenesis, and gene/mRNA regulation; prior studies indicate a role in cancer in humans and in the developing eyes, neural tissue, and renal structures in mice. We identified damaging variants in ARHGAP35 in five individuals from four families affected with anophthalmia, microphthalmia, coloboma and/or anterior segment dysgenesis disorders, together with variable non-ocular phenotypes in some families including renal, neurological, or cardiac anomalies. Three variants affected the extreme C-terminus of the protein, with two resulting in a frameshift and C-terminal extension and the other a missense change in the Rho-GAP domain; the fourth (nonsense) variant affected the middle of the gene and is the only allele predicted to undergo nonsense-mediated decay. This study implicates ARHGAP35 in human developmental eye phenotypes. C-terminal clustering of the identified alleles indicates a possible common mechanism for ocular disease but requires further studies.
Similar content being viewed by others
Introduction
Developmental ocular disorders including microphthalmia, anophthalmia, and coloboma (MAC) and anterior segment dysgenesis (ASD) spectrums represent an important cause of vision loss in childhood. Genetic diagnoses are unable to be established in a significant portion of cases: 70–85% of MAC and 40–75% of ASD cases remain unexplained after genetic analysis according to recent studies [1,2,3,4]. While some have idiopathic or environmental causes, others are likely caused by pathogenic variants in genes with a currently unrecognized role in eye development. Establishing a genetic diagnosis is important for clinical management of affected children and provides other family members with the opportunity to clarify their genetic status/risk. Identification of novel genetic causes of ocular disorders enhances our understanding of the mechanisms of ocular development, generating additional opportunities for therapeutic intervention in the future.
ARHGAP35 (Rho GTPase Activating Protein 35), also known as GRLF1 (Glucocorticoid Receptor DNA-binding Factor 1) or p190ARhoGAP-A, is a GTPase-activating protein that regulates GTPases within the Rho and Rac families [5, 6]. It has known direct roles in cell migration/invasion and division as well as neuronal morphogenesis and dendritic spine formation; additional roles include gene/mRNA translation regulation through interaction with TFII-I and eiF3A [5]. Mice homozygous for a loss-of-function Arhgap35 allele display highly penetrant early lethality, structural brain anomalies, cystic glomeruli, and optic cup anomalies including coloboma and microphthalmia while heterozygous mice are unaffected; a subset of homozygous animals also display neural tube closure defects, particularly exencephaly [7, 8]. Little is known about the role of germline variants in humans; only one de novo missense variant, c.1801G > T p.(Val601Phe), has been reported in the literature: limited phenotypic description reported a terminated pregnancy with severe midline birth defects [9]. The rate of de novo variants in ARHGAP35 was also noted to be enriched in a large cohort of individuals with developmental disorders with no details provided [10]. Through exome/genome sequencing and GeneMatcher, we identified a cohort of individuals with developmental ocular disorders and novel damaging variants in ARHGAP35.
Materials and methods
This human study was approved by Institutional Review Boards at Children’s Wisconsin and Einstein Medical Center Philadelphia. Written informed consent including research analysis and photo publication if applicable was obtained for every participant. Exome sequencing was undertaken by Psomagen (Rockville, MD) and analyzed with VarSeq (Golden Helix, Bozeman, MT). In silico analysis of variants of interest included filtering for frequency <0.001 in the general population in gnomAD v2.1.1 [11] and for predicted effect upon the protein. The effect of missense variants on protein function was further analyzed by two combined analysis tools (CADD phred hg19 and REVEL). Samples were first analyzed for variants in known MAC and ASD genes as previously described [12, 13]. Trio analysis in negative cases identified ARHGAP35 as a candidate in two families and screening for variants in this gene specifically identified one more case. Sanger sequencing was used to confirm variants and for segregation analysis. An additional case was identified through clinical genome sequencing and Matchmaker Exchange Databases [14]. Variants in ARHGAP35 were named based on reference sequence NM_004491.4 and human Genome Build hg19 and evaluated according to ACMG/AMP guidelines [15].
Results
Novel damaging variants in ARHGAP35 were identified in five individuals with developmental ocular disorders from four families. Pathogenic variants in other MAC/ASD genes were ruled out in all individuals.
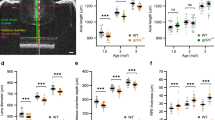
Individual 1A is a 27-year-old female born with right ocular anomalies consisting of severe microphthalmia (axial length 7.6 mm) and sclerocornea; her left eye is normal (Fig. 1A, B). She does have a bifid tragus on both ears. Her father, Individual 1B, is a 68-year-old male born with left ocular anomalies and esotropia; his right eye is normal (Fig. 1C, D). He was diagnosed with left mild microphthalmia with iris and chorioretinal coloboma and a localized spoke shaped opacity in the lens at 6 o’clock at 6 months of age. Additional features included a hemangioma on the right forearm and history of cancer (histocyte rich B cell non-Hodgkin’s lymphoma at 38 years of age and Nodular Lymphocyte Predominant Hodgkin Lymphoma at 61 years of age). Growth and development were normal for both individuals. Exome sequencing identified a heterozygous novel variant in ARHGAP35 c.4251delC p.(Thr1418Argfs*381) shared by both affected individuals. This variant was not present in five unaffected family members: mother, brother, paternal grandmother, and two paternal aunts (paternal grandfather unavailable) (Table 1, Fig. 2, Supplementary Fig. 1A). This variant meets ACMG criteria to be considered Pathogenic (PVS1, PM2_supporting, PP1).
A–C Images from Individual 1A showing right eye severe microphthalmia and sclerocornea, normal left eye, and bifid tragus. D, E Images from Individual 1B showing left eye coloboma and microcornea/microphthalmia and normal right eye. F, G Images from Individual 2 showing bilateral Peters anomaly. H, I Images from Individual 4 showing bilateral anophthalmia.
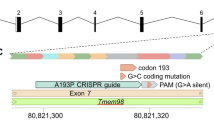
Structure of ARHGAP35 protein (per Uniprot Q9NRY4) with variant positions indicated. Family number for each variant is given in parentheses after the variant. GBD: (GTP)-binding domain, FF: FF domains, pG1&2: pseudoGTPase domains, Rho-GAP: GTPase activating protein domain, dark gray unlabeled box: region required for phospholipid binding and regulation of the substrate preference; light gray unlabeled boxes: disordered regions.
Individual 2 is a 2-year-old male with bilateral type II Peters anomaly consisting of corneal opacity with cataract, iris hypoplasia, and glaucoma treated with keratoprostheses (Fig. 1E, F). Additional features included pulmonary stenosis and thickened aortic leaflet, large left kidney with possible duplex anatomy, nevus flammeus of the glabella, small capillary hemangioma on the occiput, and nuchal cord at birth. He has had normal growth and development to date. Trio exome sequencing of the child and unaffected parents identified a de novo novel variant in ARHGAP35, c.4444delC p.(Gln1482Serfs*317) (Table 1, Fig. 2, Supplementary Fig. 1B). This variant meets ACMG criteria to be considered Pathogenic (PVS1, PS2, PM2_supporting).
Individual 3 is a 3-year-old male who presented with bilateral microphthalmia (axial lengths 13.65 mm and 14.31 mm) and agenesis of the optic nerves. Sclerocornea was observed in the right eye while the left had iris hypoplasia and corectopia. Growth was normal but development showed hypotonia and significant delay (non-ambulatory at 27 months). Additional features include left duplicated ureters and macrocephaly (55 cm at 27 weeks, +4.55 SD). Echocardiogram, skeletal survey, and Brain MRI were normal other than eye and optic nerve anomalies. Pregnancy history is notable for increased nuchal translucency at 12 weeks gestation and identification of renal anomalies and macrocephaly at 22 weeks gestation. Trio genome sequencing of the child and unaffected parents identified de novo novel variants in PTEN, NM_000314.8:c.2 T > G p.(Met1Arg), and ARHGAP35, c.1849C > T p.(Arg617Ter) (Table 1, Fig. 2, Supplementary Fig. 1C). This variant meets ACMG criteria to be considered Pathogenic (PVS1, PS2, PM2_supporting).
Individual 4 is a 42-year-old male with bilateral anophthalmia. Trio exome sequencing identified a novel variant in ARHGAP35, c.4294 T > C p.(Cys1432Arg), inherited from the father, who did not have a MAC phenotype but was reported to wear glasses from a young age with no further details available (Table 1, Fig. 2, Supplementary Fig. 1D). The exome read depth was slightly skewed in the father (37%) but Sanger sequencing showed even peaks (Supplementary Fig. 1D). This missense variant is predicted to be damaging with high CADD (32) and GERP + + (5.6) scores and a moderate REVEL score (0.439). This variant is considered a Variant of Uncertain Significance by ACMG criteria (PM2, PP2, PP3).
Discussion
This study presents the first evidence implicating ARHGAP35 in human developmental ocular phenotypes. Three variants affected the extreme C-terminus of the protein, with two resulting in a frameshift and C-terminal extension and the other a missense change in the Rho-GAP domain. General population data in gnomAD shows significant constraint against both loss of function and missense variants for this gene [11]. The MAC phenotypes observed here are very consistent with those reported in the mouse model. ARHGAP35 was also previously shown to be involved in the regulation of genes within the Hippo signaling pathway [16] including YAP1, which is independently associated with MAC disorders [17,18,19]. Corneal defects, observed in three families in this study, are also seen in Yap1-deficient mice [20].
The non-ocular features within our cohort were more variable. The presence of duplicated renal structures in two individuals is intriguing, though it does not perfectly replicate the hypodysplasia phenotype observed in mice. With regards to the history of cancer in Individual 1B, while a tumor suppressor role has been identified for ARHGAP35, particularly in carcinomas [5], an association with lymphoma has not been reported to date so it is unclear whether this phenotype is coincidental or related to the genetic variant. Interestingly, only one variant was associated with an additional neurological phenotype in this cohort (Individual 3, p.(Arg617Ter)). That variant occurred earlier in the gene, within the first exon, and is expected to lead to complete loss of function due to nonsense-mediated decay. Mice with neurological phenotypes similarly had complete loss-of-function alleles [7, 8]. The other three variants identified in individuals with normal neurological function occurred in or after the RhoGAP domain in the final exon of the gene; thus, the variant proteins would be expected to escape nonsense-mediated decay and may retain enough function for normal neurological development. However, the patient with a neurological phenotype also has a PTEN variant in the initiation codon. While similar PTEN variants have been reported in individuals with macrocephaly and variable autism/intellectual disability [21], the hypotonia/gross motor phenotype is more severe than is typical for PTEN variants, so it is likely that the ARHGAP35 variant is also contributing to the neurological phenotype.
Two of the four variants were de novo, supporting a likely causative role. One of the others was inherited from an affected parent- while it could not be conclusively proven to be de novo, it was not present in five unaffected family members. Interestingly, in this family both affected individuals had a unilateral ocular phenotype, similar to the recently reported PRR12 gene with dominant unilateral MAC or ASD phenotypes [22]. In the final case, the variant was inherited from a parent without MAC but with reduced vision that required corrective lenses. Because available clinical data was limited, it is impossible to conclude whether this represents a case of incomplete penetrance, variable expressivity, or somatic mosaicism (though no strong evidence of mosaicism was detected); it is also possible that this is a benign allele that does not contribute to the ocular phenotype. Incomplete penetrance and variable expressivity are noted for other MAC genes including YAP1 (regulated by ARHGAP35).
In combination with the mouse model, this study strongly supports a role for ARHGAP35 in vertebrate ocular development, consistent with its known regulation of Hippo-YAP signaling. C-terminal clustering of the identified alleles indicates a possible common mechanism for ocular disease. Other variable developmental features were present in several patients indicating a possible role for ARHGAP35 in other systems, consistent with the mouse model. Given its known role as a tumor suppressor, further investigation is needed to determine whether individuals with ocular phenotypes are at increased risk for cancer.
Data availability
ARHGAP35 variants were submitted to ClinVar (Accession numbers SCV002605061 - SCV002605064). There are no additional data available.
References
Ma A, Yousoof S, Grigg JR, Flaherty M, Minoche AE, Cowley MJ, et al. Revealing hidden genetic diagnoses in the ocular anterior segment disorders. Genet Med. 2020;22:1623–32.
Chassaing N, Causse A, Vigouroux A, Delahaye A, Alessandri JL, Boespflug-Tanguy O, et al. Molecular findings and clinical data in a cohort of 150 patients with anophthalmia/microphthalmia. Clin Genet. 2014;86:326–34.
Patel A, Hayward JD, Tailor V, Nyanhete R, Ahlfors H, Gabriel C, et al. The Oculome Panel Test: Next-Generation Sequencing to Diagnose a Diverse Range of Genetic Developmental Eye Disorders. Ophthalmology. 2019;126:888–907.
Jackson D, Malka S, Harding P, Palma J, Dunbar H, Moosajee M. Molecular diagnostic challenges for non-retinal developmental eye disorders in the United Kingdom. Am J Med Genet C Semin Med Genet. 2020;184:578–89.
Heraud C, Pinault M, Lagree V, Moreau V. p190RhoGAPs, the ARHGAP35- and ARHGAP5-Encoded Proteins, in Health and Disease. Cells 2019;8:351.
Levay M, Bartos B, Ligeti E. p190RhoGAP has cellular RacGAP activity regulated by a polybasic region. Cell Signal. 2013;25:1388–94.
Brouns MR, Matheson SF, Hu KQ, Delalle I, Caviness VS, Silver J, et al. The adhesion signaling molecule p190 RhoGAP is required for morphogenetic processes in neural development. Development. 2000;127:4891–903.
Stewart K, Gaitan Y, Shafer ME, Aoudjit L, Hu D, Sharma R, et al. A Point Mutation in p190A RhoGAP Affects Ciliogenesis and Leads to Glomerulocystic Kidney Defects. PLoS Genet. 2016;12:e1005785.
Armes JE, Williams M, Price G, Wallis T, Gallagher R, Matsika A, et al. Application of Whole Genome Sequencing Technology in the Investigation of Genetic Causes of Fetal, Perinatal, and Early Infant Death. Pediatr Dev Pathol. 2018;21:54–67.
Kaplanis J, Samocha KE, Wiel L, Zhang Z, Arvai KJ, Eberhardt RY, et al. Evidence for 28 genetic disorders discovered by combining healthcare and research data. Nature. 2020;586:757–62.
Karczewski KJ, Francioli LC, Tiao G, Cummings BB, Alfoldi J, Wang Q, et al. The mutational constraint spectrum quantified from variation in 141,456 humans. Nature. 2020;581:434–43.
Deml B, Reis LM, Lemyre E, Clark RD, Kariminejad A, Semina EV. Novel mutations in PAX6, OTX2 and NDP in anophthalmia, microphthalmia and coloboma. Eur J Hum Genet. 2016;24:535–41.
Weh E, Reis LM, Happ HC, Levin AV, Wheeler PG, David KL, et al. Whole exome sequence analysis of Peters anomaly. Hum Genet. 2014;133:1497–511.
Philippakis AA, Azzariti DR, Beltran S, Brookes AJ, Brownstein CA, Brudno M, et al. The Matchmaker Exchange: a platform for rare disease gene discovery. Hum Mutat. 2015;36:915–21.
Richards S, Aziz N, Bale S, Bick D, Das S, Gastier-Foster J, et al. Standards and guidelines for the interpretation of sequence variants: a joint consensus recommendation of the American College of Medical Genetics and Genomics and the Association for Molecular Pathology. Genet Med. 2015;17:405–24.
Frank SR, Kollmann CP, Luong P, Galli GG, Zou L, Bernards A, et al. p190 RhoGAP promotes contact inhibition in epithelial cells by repressing YAP activity. J Cell Biol. 2018;217:3183–201.
Williamson KA, Rainger J, Floyd JA, Ansari M, Meynert A, Aldridge KV, et al. Heterozygous loss-of-function mutations in YAP1 cause both isolated and syndromic optic fissure closure defects. Am J Hum Genet. 2014;94:295–302.
Oatts JT, Hull S, Michaelides M, Arno G, Webster AR, Moore AT. Novel heterozygous mutation in YAP1 in a family with isolated ocular colobomas. Ophthalmic Genet. 2017;38:281–3.
DeYoung C, Guan B, Ullah E, Blain D, Hufnagel RB, Brooks BP. De novo frameshift mutation in YAP1 associated with bilateral uveal coloboma and microphthalmia. Ophthalmic Genet. 2022;43:513–7.
Kim S, Thomasy SM, Raghunathan VK, Teixeira LBC, Moshiri A, FitzGerald P, et al. Ocular phenotypic consequences of a single copy deletion of the Yap1 gene (Yap1 (+/-)) in mice. Mol Vis. 2019;25:129–42.
Stenson PD, Mort M, Ball EV, Chapman M, Evans K, Azevedo L, et al. The Human Gene Mutation Database (HGMD((R))): optimizing its use in a clinical diagnostic or research setting. Hum Genet. 2020;139:1197–207.
Reis LM, Costakos D, Wheeler PG, Bardakjian T, Schneider A, Fung SSM et al. Dominant variants in PRR12 result in unilateral or bilateral complex microphthalmia. Clin Genet. 2021;99:437–42.
Acknowledgements
We would like to express gratitude to the individuals and families who participated in this study.
Author information
Authors and Affiliations
Contributions
LMR enrolled participants, collected clinical data, and analyzed exome data. NC provided clinical assessment and analysis of genome data. TB was involved in enrollment and clinical data collection. ST completed Sanger sequencing analysis. AS provided clinical assessment. EVS designed and supervised the study. LMR and EVS wrote the original draft of the paper; NC, TB, ST, and AS edited the paper.
Corresponding author
Ethics declarations
Funding
Funding for this study was provided by NIH grants EY015518 and EY025718 (EVS).
Competing interests
The authors declare no competing interests.
Ethics approval
This human study was approved by the Institutional Review Boards of Children’s Wisconsin (#124172) and Einstein Medical Center Philadelphia (#HN2191). Written informed consent was obtained from participants and/or legal guardians for all research study activities and photo publication (if applicable).
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Reis, L.M., Chassaing, N., Bardakjian, T. et al. ARHGAP35 is a novel factor disrupted in human developmental eye phenotypes. Eur J Hum Genet 31, 363–367 (2023). https://doi.org/10.1038/s41431-022-01246-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41431-022-01246-z
This article is cited by
-
2023 in the European Journal of Human Genetics
European Journal of Human Genetics (2024)
-
Genes=disease (?)
European Journal of Human Genetics (2023)