Abstract
Background
Aging is accompanied by the inability to optimally respond to anabolic stimulus of nutrition, with consequent loss of muscle mass and functionality. It has been speculated that not only total protein intake, but also the per meal protein dose may have important implications to protein balance and, hence, muscle mass in middle-aged and older adults, but evidence is lacking in a more vulnerable population such as the frail elderly. The aim was to investigate possible associations between total protein intake and its per meal dose with multiple measures of muscle mass, strength, and functionality in a cohort of pre-frail and frail elderly individuals.
Methods
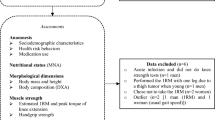
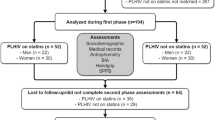
One-hundred-and-fifty-seven pre-frail and frail elderly individuals were assessed for total and per meal protein intake (food diaries), total and appendicular lean mass (DXA), vastus lateralis cross-sectional area [(CSA) B-mode ultrasound], and muscle function [leg-press and bench press 1-RM, timed-stands test, timed-up-and-go test, handgrip, and risk of falls (Biodex Balance System®)].
Results
Protein intake and number of meals with either ≥20 g or ≥30 g of protein were significantly associated (after controlling for confounding factors) with greater total and appendicular lean mass and vastus lateralis CSA.
Conclusions
We found that not only total protein intake but also the number of high-protein containing meals are associated with muscle mass in frail and pre-frail elderly.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Evans WJ. Skeletal muscle loss: cachexia, sarcopenia, and inactivity. Am J Clin Nutr. 2010;91:1123S–7S.
Doherty TJ. Invited review: aging and sarcopenia. J Appl Physiol. 2003;95:1717–27.
Fried LP, Tangen CM, Walston J, Newman AB, Hirsch C, Gottdiener J, et al. Frailty in older adults: evidence for a phenotype. J Gerontol A Biol Sci Med Sci. 2001;56:M146–156.
Cooper C, Dere W, Evans W, Kanis JA, Rizzoli R, Sayer AA, et al. Frailty and sarcopenia: definitions and outcome parameters. Osteoporos Int. 2012;23:1839–48.
Morley JE. Sarcopenia in the elderly. Fam Pract. 2012;29(Suppl 1):i44–8.
Bauer JM, Sieber CC. Sarcopenia and frailty: a clinician’s controversial point of view. Exp Gerontol. 2008;43:674–8.
Baum JI, Kim IY, Wolfe RR. Protein consumption and the elderly: what is the optimal level of intake? Nutrients. 2016;8:pii:E359. https://doi.org/10.3390/nu8060359.
Rahi B, Colombet Z, Gonzalez-Colaco Harmand M, Dartigues JF, Boirie Y, Letenneur L, et al. Higher protein but not energy intake is associated with a lower prevalence of frailty among community-dwelling older adults in the french three-city cohort. J Am Med Dir Assoc. 2016;17:672.e–672.e11.
Granic A, Mendonca N, Sayer AA, Hill TR, Davies K, Adamson A, et al. Low protein intake, muscle strength and physical performance in the very old: the Newcastle 85+ Study. Clin Nutr. 2018;37:2260–70.
Murphy CH, Oikawa SY, Phillips SM. Dietary protein to maintain muscle mass in aging: a case for per-meal protein recommendations. J Frailty Aging. 2016;5:49–58.
Loenneke JP, Loprinzi PD, Murphy CH, Phillips SM. Per meal dose and frequency of protein consumption is associated with lean mass and muscle performance. Clin Nutr. 2016;35:1506–11.
Oikawa SY, Holloway TM, Phillips SM. The impact of step reduction on muscle health in aging: protein and exercise as countermeasures. Front Nutr. 2019;6:75.
Burd NA, Wall BT, van Loon LJ. The curious case of anabolic resistance: old wives’ tales or new fables? J Appl Physiol. 2013;112:1233–5.
Hess M. Portion photos of popular foods, vol. III. American Dietetic Association: Chicago; 1997.
NEPA/UNICAMP NdEePeA. Tabela Brasileira de Composição de Alimentos - TACO. Campinas, Brasil: NEPA/UNICAMP, 2011.
Murakami K, Livingstone MB. Associations between meal and snack frequency and diet quality in US adults: National Health and Nutrition Examination Survey 2003–12. J Acad Nutr Diet. 2016;116:1101–13.
Lixandrao ME, Ugrinowitsch C, Bottaro M, Chacon-Mikahil MP, Cavaglieri CR, Min LL, et al. Vastus lateralis muscle cross-sectional area ultrasonography validity for image fitting in humans. J Strength Cond Res. 2014;28:3293–7.
Phillips WT, Batterham AM, Valenzuela JE, Burkett LN. Reliability of maximal strength testing in older adults. Arch Phys Med Rehabil. 2004;85:329–34.
Brown L, Weir J. ASEP procedures recommendation I: accurate assessment of muscular strength and power. J Exerc Physiol. 2001;4:1–21.
Newcomer KL, Krug HE, Mahowald ML. Validity and reliability of the timed-stands test for patients with rheumatoid arthritis and other chronic diseases. J Rheumatol. 1993;20:21–27.
Podsiadlo D, Richardson S. The timed “Up & Go”: a test of basic functional mobility for frail elderly persons. J Am Geriatr Soc. 1991;39:142–8.
Arnold BL, Schmitz RJ. Examination of balance measures produced by the biodex stability system. J Athl Train. 1998;33:323–7.
Bartali B, Frongillo EA, Bandinelli S, Lauretani F, Semba RD, Fried LP, et al. Low nutrient intake is an essential component of frailty in older persons. J Gerontol A Biol Sci Med Sci. 2006;61:589–93.
Mustafa J, Ellison RC, Singer MR, Bradlee ML, Kalesan B, Holick MF, et al. Dietary protein and preservation of physical functioning among middle-aged and older adults in the framingham offspring Study. Am J Epidemiol. 2018;187:1411–9.
Gray-Donald K, St-Arnaud-McKenzie D, Gaudreau P, Morais JA, Shatenstein B, Payette H. Protein intake protects against weight loss in healthy community-dwelling older adults. J Nutr. 2014;144:321–6.
Houston DK, Nicklas BJ, Ding J, Harris TB, Tylavsky FA, Newman AB, et al. Dietary protein intake is associated with lean mass change in older, community-dwelling adults: the Health, Aging, and Body Composition (Health ABC) Study. Am J Clin Nutr. 2008;87:150–5.
Morley JE, Vellas B, van Kan GA, Anker SD, Bauer JM, Bernabei R, et al. Frailty consensus: a call to action. J Am Med Dir Assoc. 2013;14:392–7.
Moore DR, Churchward-Venne TA, Witard O, Breen L, Burd NA, Tipton KD, et al. Protein ingestion to stimulate myofibrillar protein synthesis requires greater relative protein intakes in healthy older versus younger men. J Gerontol A Biol Sci Med Sci. 2015;70:57–62.
Areta JL, Burke LM, Ross ML, Camera DM, West DW, Broad EM, et al. Timing and distribution of protein ingestion during prolonged recovery from resistance exercise alters myofibrillar protein synthesis. J Physiol. 2013;591:2319–31.
Farsijani S, Morais JA, Payette H, Gaudreau P, Shatenstein B, Gray-Donald K, et al. Relation between mealtime distribution of protein intake and lean mass loss in free-living older adults of the NuAge study. Am J Clin Nutr. 2016;104:694–703.
Farsijani S, Payette H, Morais JA, Shatenstein B, Gaudreau P, Chevalier S. Even mealtime distribution of protein intake is associated with greater muscle strength, but not with 3-y physical function decline, in free-living older adults: the Quebec longitudinal study on Nutrition as a Determinant of Successful Aging (NuAge study). Am J Clin Nutr. 2017;106:113–24.
Pouyet V, Cuvelier G, Benattar L, Giboreau A. A photographic method to measure food item intake. Validation in geriatric institutions. Appetite. 2015;84:11–9.
van Staveren WA, de Groot LC, Blauw YH, van der Wielen RP. Assessing diets of elderly people: problems and approaches. Am J Clin Nutr. 1994;59:221S–3S.
Acknowledgements
The authors are grateful to all who participated and contributed to the present research.
Funding
This work was supported by Fundação do Amparo à Pesquisa do Estado de São Paulo (FAPESP), Conselho Nacional de Pesquisa e Desenvolvimento (CNPq), and Coordenação de Aperfeiçoamento de Pessoal de Nível Superior (CAPES)—Finance Code 001.
Author information
Authors and Affiliations
Contributions
APH, BG, and HR designed the research, analyzed the data, and wrote the paper. APH, SFD, MDC, LSG, ALF, JCJ, DAS, ML, RTSP, LR, and RMRP conducted the research. ML performed statistical analysis. All authors have seen and approved the final version of the manuscript for publication.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Hayashi, A.P., de Capitani, M.D., Dias, S.F. et al. Number of high-protein containing meals correlates with muscle mass in pre-frail and frail elderly. Eur J Clin Nutr 74, 1047–1053 (2020). https://doi.org/10.1038/s41430-020-0618-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41430-020-0618-3
This article is cited by
-
Distribution of daily protein intake and appendicular skeletal muscle mass in healthy free-living Chinese older adults
European Journal of Nutrition (2024)
-
Protein Consumption: Inadequacy in Amount, Food Sources, and Mealtime Distribution in Community-Dwelling Older Adults
Ageing International (2023)
-
Adequate protein intake in at least one meal is associated with higher appendicular muscle mass index in women: a cross-sectional study
Nutrire (2021)