Abstract
Objective
Dietary modification of insulin resistance may be a strategy for reducing chronic disease. For this study, we tested the hypothesis that higher fasting insulin, a marker for insulin resistance, would be related to diet patterns with a high proportion of carbohydrates, those with a high glycemic index, and those characterized by added sugar and processed starches.
Study design
Data were analyzed on 13,528 nondiabetic participants of the REasons for Geographic and Ethnic Differences in Stroke (REGARDS), an observational study of adults aged ≥45 years residing in 1855 counties across the continental USA. Information on habitual diet was collected using the Block 98 Food Frequency Questionnaire. Percent energy from carbohydrate, glycemic index, and glycemic load were determined for each participant, as well as adherence to five established diet patterns. Logistic regression was used to examine associations of baseline diet characteristics with odds for high fasting insulin [quartiles 3 and 4 (median = 98.9 pmol/L) vs. quartile 1], after adjusting for covariates.
Result
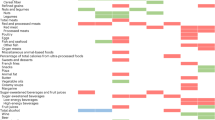
Greater percent carbohydrate, glycemic index, and glycemic load, and adherence to sweets/fat and southern diet patterns, was associated with greater odds for high insulin (P for trend <0.05 to <0.0001), whereas adherence to the plant-based and alcohol/salad patterns was associated with lower odds for high insulin (P for linear trend <0.0001).
Conclusion
In conclusion, diet pattern is associated with fasting insulin. Future studies are needed to determine if diet interventions designed to lower insulin, perhaps based on the patterns identified in this study, can improve risk for chronic disease.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Xun P, Wu Y, He Q, He K. Fasting insulin concentrations and incidence of hypertension, stroke, and coronary heart disease: a meta-analysis of prospective cohort studies. Am J Clin Nutr. 2013;98:1543–54. https://doi.org/10.3945/ajcn.113.065565.
Haffner SM, Stern MP, Mitchell BD, Hazuda HP, Patterson JK. Incidence of type II diabetes in Mexican Americans predicted by fasting insulin and glucose levels, obesity, and body-fat distribution. Diabetes. 1990;39:283–8.
Tulloch-Reid MK, Hanson RL, Saremi A, Looker HC, Williams DE, Krakoff J, et al. Hematocrit and the incidence of type 2 diabetes in the pima indians. Diabetes Care. 2004;27:2245–6.
Xun P, Liu K, Cao W, Sidney S, Williams OD, He K. Fasting insulin level is positively associated with incidence of hypertension among American young adults: a 20-year follow-up study. Diabetes Care. 2012;35:1532–7.
He J, Klag MJ, Caballero B, Appel LJ, Charleston J, Whelton PK. Plasma insulin levels and incidence of hypertension in African Americans and whites. Arch Intern Med. 1999;159:498–503.
Levin G, Kestenbaum B, Ida Chen YD, Jacobs DR Jr, Psaty BM, Rotter JI, et al. Glucose, insulin, and incident hypertension in the multi-ethnic study of atherosclerosis. Am J Epidemiol. 2010;172:1144–54. https://doi.org/10.1093/aje/kwq266.
Mitchell BD, Haffner SM, Hazuda HP, Valdez R, Stern MP. The relation between serum insulin levels and 8-year changes in lipid, lipoprotein, and blood pressure levels. Am J Epidemiol. 1992;136:12–22.
Folsom AR, Rasmussen ML, Chambless LE, Howard G, Cooper LS, Schmidt MI, et al. Prospective associations of fasting insulin, body fat distribution, and diabetes with risk of ischemic stroke. The Atherosclerosis Risk in Communities (ARIC) Study Investigators. Diabetes Care. 1999;22:1077–83.
Lawlor DA, Fraser A, Ebrahim S, Smith GD. Independent associations of fasting insulin, glucose, and glycated haemoglobin with stroke and coronary heart disease in older women. PLoS Med. 2007;4:e263. https://doi.org/10.1371/journal.pmed.0040263.
Kurl S, Zaccardi F, Onaemo VN, Jae SY, Kauhanen J, Ronkainen K, et al. Association between HOMA-IR, fasting insulin and fasting glucose with coronary heart disease mortality in nondiabetic men: a 20-year observational study. Acta Diabetol. 2015;52:183–6. https://doi.org/10.1007/s00592-014-0615-x.
Chandler-Laney PC, Morrison SA, Goree LL, Ellis AC, Casazza K, Desmond R, et al. Return of hunger following a relatively high carbohydrate breakfast is associated with earlier recorded glucose peak and nadir. Appetite. 2014;80:236–41. https://doi.org/10.1016/j.appet.2014.04.031.
Reynolds RC, Stockmann KS, Atkinson FS, Denyer GS, Brand-Miller JC. Effect of the glycemic index of carbohydrates on day-long (10 h) profiles of plasma glucose, insulin, cholecystokinin and ghrelin. Eur J Clin Nutr. 2009;63:872–8.
Del Prato S, Leonetti F, Simonson DC, Sheehan P, Matsuda M, DeFronzo R. Effect of sustained physiologic hyperinsulinaemia and hyperglycaemia on insulin secretion and insulin sensitivity in man. Diabetologia. 1994;37:1025–35.
Salmeron J, Aschirio A, Rimm EB, Colditz GA, Spiegelman D, Jenkins DJ, et al. Dietary fiber, glycemic load, and risk of NIDDM in men. Diabetes Care. 1997;20:545–50.
Salmeron J, Manson JE, Stampfer MJ, Colditz GA, Wing AL, Willett WC. Dietary fiber, glycemic load, and risk of non-insulin-dependent diabetes mellitus in women. J Am Med Assoc. 1997;277:472–7.
Schwingshackl L, Hoffmann G. Long-term effects of low glycemic index/load vs. high glycemic index/load diets on parameters of obesity and obesity-associated risks: a systematic review and meta-analysis. Nutr Metab Cardiovasc Dis. 2013;23:699–706. https://doi.org/10.1016/j.numecd.2013.04.008.
Mayer EJ, Newman B, Quesenberry CP Jr, Selby JV. Usual dietary fat intake and insulin concentrations in healthy women twins. Diabetes Care. 1993;16:1459–69.
Parker DR, Weiss ST, Troisi R, Cassano PA, Vokonas PS, Landsberg L. Relationship of dietary saturated fatty acids and body habitus to serum insulin concentrations: the Normative Aging Study. Am J Clin Nutr. 1993;58:129–36.
Maron DJ, Fair JM, Haskell WL. Saturated fat intake and insulin resistance in men with coronary artery disease. The Stanford Coronary Risk Intervention Project Investigators and Staff. Circulation. 1991;84:2020–7.
Marshall JA, Bessesen DH, Hamman RF. High saturated fat and low starch and fibre are associated with hyperinsulinaemia in a non-diabetic population: the San Luis Valley Diabetes Study. Diabetologia. 1997;40:430–8. https://doi.org/10.1007/s001250050697.
Manolio TA, Savage PJ, Burke GL, Hilner JE, Liu K, Orchard TJ, et al. Correlates of fasting insulin levels in young adults: the CARDIA study. J Clin Epidemiol. 1991;44:571–8.
Jacobs DR Jr, Tapsell LC. Food, not nutrients, is the fundamental unit in nutrition. Nutr Rev. 2007;65:439–50.
Howard VJ, Cushman M, Pulley L, Gomez CR, Go RC, Prineas RJ, et al. The reasons for geographic and racial differences in stroke study: objectives and design. Neuroepidemiology. 2005;25:135–43. https://doi.org/10.1159/000086678.
Shikany JM, Safford MM, Newby PK, Durant RW, Brown TM, Judd SE. Southern dietary pattern is associated with hazard of acute coronary heart disease in the Reasons for Geographic and Racial Differences in Stroke (REGARDS) Study. Circulation. 2015;132:804–14. https://doi.org/10.1161/circulationaha.114.014421.
Kiage JN, Merrill PD, Robinson CJ, Cao Y, Malik TA, Hundley BC, et al. Intake of trans fat and all-cause mortality in the Reasons for Geographical and Racial Differences in Stroke (REGARDS) cohort. Am J Clin Nutr. 2013;97:1121–8. https://doi.org/10.3945/ajcn.112.049064.
Judd SE, Gutierrez OM, Newby PK, Howard G, Howard VJ, Locher JL, et al. Dietary patterns are associated with incident stroke and contribute to excess risk of stroke in black Americans. Stroke. 2013;44:3305–11. https://doi.org/10.1161/strokeaha.113.002636.
Judd SE, Letter AJ, Shikany JM, Roth DL, Newby PK. Dietary patterns derived using exploratory and confirmatory factor analysis are stable and generalizable across race, region, and gender subgroups in the REGARDS Study. Front Nutr. 2014;1:29. https://doi.org/10.3389/fnut.2014.00029.
Gunter MJ, Xie X, Xue X, Kabat GC, Rohan TE, Wassertheil-Smoller S, et al. Breast cancer risk in metabolically healthy but overweight postmenopausal women. Cancer Res. 2015;75:270–4. https://doi.org/10.1158/0008-5472.can-14-2317.
Shrira I, Christenfeld N, Howard G. Exposure to the US Stroke Buckle as a risk factor for cerebrovascular mortality. Neuroepidemiology. 2008;30:229–33. https://doi.org/10.1159/000128102.
Grey N, Kipnis DM. Effect of diet composition on the hyperinsulinemia of obesity. N Engl J Med. 1971;285:827–31. https://doi.org/10.1056/nejm197110072851504.
Juanola-Falgarona M, Salas-Salvado J, Ibarrola-Jurado N, Rabassa-Soler A, Diaz-Lopez A, Guasch-Ferre M, et al. Effect of the glycemic index of the diet on weight loss, modulation of satiety, inflammation, and other metabolic risk factors: a randomized controlled trial. Am J Clin Nutr. 2014;100:27–35. https://doi.org/10.3945/ajcn.113.081216.
AlEssa HB, Bhupathiraju SN, Malik VS, Wedick NM, Campos H, Rosner B, et al. Carbohydrate quality and quantity and risk of type 2 diabetes in US women. Am J Clin Nutr. 2015;102:1543–53. https://doi.org/10.3945/ajcn.115.116558.
de Munter JS, Hu FB, Spiegelman D, Franz M, van Dam RM. Whole grain, bran, and germ intake and risk of type 2 diabetes: a prospective cohort study and systematic review. PLoS Med. 2007;4:e261. https://doi.org/10.1371/journal.pmed.0040261.
Schulze MB, Schulz M, Heidemann C, Schienkiewitz A, Hoffmann K, Boeing H. Fiber and magnesium intake and incidence of type 2 diabetes: a prospective study and meta-analysis. Arch Intern Med. 2007;167:956–65. https://doi.org/10.1001/archinte.167.9.956.
Gower BA, Bergman R, Stefanovski D, Darnell B, Ovalle F, Fisher G, et al. Baseline insulin sensitivity affects response to high-amylose maize resistant starch in women: a randomized, controlled trial. Nutr Metab. 2016;13:2. https://doi.org/10.1186/s12986-016-0062-5.
Robertson MD. Dietary-resistant starch and glucose metabolism. Curr Opin Clin Nutr Metab Care. 2012;15:362–7. https://doi.org/10.1097/MCO.0b013e3283536931.
Hill JO, Peters JC, Reed GW, Schlundt DG, Sharp T, Greene HL. Nutrient balance in humans: effects of diet composition. Am J Clin Nutr. 1991;54:10–7.
Boden G, Sargrad K, Homko C, Mozzoli M, Stein TP. Effect of a low-carbohydrate diet on appetite, blood glucose levels, and insulin resistance in obese patients with type 2 diabetes. Ann Intern Med. 2005;142:403–11.
Gower BA, Chandler-Laney PC, Ovalle F, Goree LL, Azziz R, Desmond RA, et al. Favourable metabolic effects of a eucaloric lower-carbohydrate diet in women with PCOS. Clin Endocrinol. 2013;79:550–7. https://doi.org/10.1111/cen.12175.
Sun Y, Liu B, Snetselaar LG, Robinson JG, Wallace RB, Peterson LL, et al. Association of fried food consumption with all cause, cardiovascular, and cancer mortality: prospective cohort study. BMJ. 2019;364:k5420. https://doi.org/10.1136/bmj.k5420.
Okuyama H, Langsjoen PH, Ohara N, Hashimoto Y, Hamazaki T, Yoshida S, et al. Medicines and vegetable oils as hidden causes of cardiovascular disease and diabetes. Pharmacology. 2016;98:134–70. https://doi.org/10.1159/000446704.
Kanner J. Dietary advanced lipid oxidation endproducts are risk factors to human health. Mol Nutr Food Res. 2007;51:1094–101. https://doi.org/10.1002/mnfr.200600303.
Pedersen BK. Anti-inflammatory effects of exercise: role in diabetes and cardiovascular disease. Eur J Clin Investig. 2017;47:600–11. https://doi.org/10.1111/eci.12781.
Vlassara H, Uribarri J. Advanced glycation end products (AGE) and diabetes: cause, effect, or both? Curr Diab Rep. 2014;14:453.https://doi.org/10.1007/s11892-013-0453-1.
Tabung FK, Wang W, Fung TT, Hu FB, Smith-Warner SA, Chavarro JE, et al. Development and validation of empirical indices to assess the insulinaemic potential of diet and lifestyle. Br J Nutr. 2016:1–12. https://doi.org/10.1017/S0007114516003755.
Acknowledgements
The REGARDS research project is supported by a cooperative agreement U01 NS041588 from the National Institute of Neurological Disorders and Stroke, National Institutes of Health, Department of Health and Human Service. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institute of Neurological Disorders and Stroke or the National Institutes of Health. Representatives of the funding agency have been involved in the review of the paper but not directly involved in the collection, management, analysis or interpretation of the data. Additional support was provided by General Mills for coding of the Block Food Frequency Questionnaire. The authors thank the other investigators, the staff, and the participants of the REGARDS study for their valuable contributions. A full list of participating REGARDS investigators and institutions can be found at http://www.regardsstudy.org.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Gower, B.A., Pearson, K., Bush, N. et al. Diet pattern may affect fasting insulin in a large sample of black and white adults. Eur J Clin Nutr 75, 628–635 (2021). https://doi.org/10.1038/s41430-020-00762-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41430-020-00762-9