Abstract
Background/Objectives
Non-caloric artificial sweeteners (NAS) are marketed as healthier alternatives to sugar, but the relationship between consumption of NAS and development of diabetes is unclear. This study assessed the associations of diet soda and NAS consumption with (1) early markers of insulin and glucose homeostasis (cross-sectionally) and (2) incident diabetes (over an average of 8 years of follow-up) among American Indians, a population with high rates of obesity.
Subjects/Methods
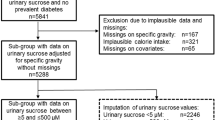
The study population included Strong Heart Family Study participants without cardiovascular disease or diabetes who participated in the 2007–2009 study exam (n = 1359). Diet soda and NAS consumption were assessed using a Block food frequency questionnaire and supplemental NAS questionnaire at the study exam. Fasting plasma glucose and insulin were measured during the study exam after a 12-h overnight fast. Participants were followed for incident diabetes through December 2017 using a single phone interview and medical record review; diabetes was identified by self-report and confirmed by documentation in medical records. Associations of diet soda and NAS consumption with fasting insulin, glucose, and incident diabetes were assessed using generalized estimating equations (fasting insulin and glucose analyses) and parametric survival models with Weibull distributions (incident diabetes analyses).
Results
Just under half of participants reported regularly consuming diet soda (40%) or using NAS to sweeten their beverages (41%). During an average 8 years of follow-up, we identified 98 cases of incident diabetes. After correction for multiple comparisons, there were no statistically significant associations of reported diet soda and NAS consumption with fasting insulin, fasting glucose, or incident diabetes.
Conclusions
Although reported consumption of diet soda and NAS were high, neither were associated with diabetes risk.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Data availability
Due to privacy agreements with the tribal communities involved in this study, access to study data are restricted. Further information can be found at https://strongheartstudy.org/.
References
Morenga LT, Mallard S, Mann J. Dietary sugars and body weight: systematic review and meta-analyses of randomised controlled trials and cohort studies. BMJ. 2013;346:E7492. https://doi.org/10.1136/Bmj.E7492.
Imamura F, O’Connor L, Ye Z, Mursu J, Hayashino Y, Bhupathiraju SN, et al. Consumption of sugar sweetened beverages, artificially sweetened beverages, and fruit juice and incidence of type 2 diabetes: systematic review, meta-analysis, and estimation of population attributable fraction. BMJ. 2015;351:h3576. https://doi.org/10.1136/bmj.h3576.
Malik VS, Popkin BM, Bray GA, Despres JP, Willett WC, Hu FB. Sugar-sweetened beverages and risk of metabolic syndrome and type 2 diabetes: a meta-analysis. Diabetes Care. 2010;33:2477–83. https://doi.org/10.2337/dc10-1079.
Palmer JR, Boggs DA, Krishnan S, Hu FB, Singer M, Rosenberg L. Sugar-sweetened beverages and incidence of type 2 diabetes mellitus in African American women. Arch Intern Med. 2008;168:1487–92. https://doi.org/10.1001/archinte.168.14.1487.
Sylvetsky AC, Welsh JA, Brown RJ, Vos MB. Low-calorie sweetener consumption is increasing in the United States. Am J Clin Nutr. 2012;96:640–6. https://doi.org/10.3945/ajcn.112.034751.
Raben A, Moller BK, Flint A, Vasilaris TH, Christina Moller A, Juul Holst J, et al. Increased postprandial glycaemia, insulinemia, 281and lipidemia after 10 weeks’ sucrose-rich diet compared to an artificially sweetened diet: a randomised controlled trial. Food Nutr Res. 2011;55:5961 [pii]. https://doi.org/10.3402/fnr.v55i0.5961.
Nettleton JA, Lutsey PL, Wang Y, Lima JA, Michos ED, Jacobs DR, Jr. Diet soda intake and risk of incident metabolic syndrome and type 2 diabetes in the Multi-Ethnic Study of Atherosclerosis (MESA). Diabetes Care. 2009;32:688–94. https://doi.org/10.2337/dc08-1799.
Gardener H, Moon YP, Rundek T, Elkind MSV, Sacco RL. Diet soda and sugar-sweetened soda consumption in relation to incident diabetes in the Northern Manhattan Study. Curr Dev Nutr. 2018;2:nzy008. https://doi.org/10.1093/cdn/nzy008.
Huang M, Quddus A, Stinson L, Shikany JM, Howard BV, Kutob RM, et al. Artificially sweetened beverages, sugar-sweetened beverages, plain water, and incident diabetes mellitus in postmenopausal women: the prospective Women’s Health Initiative observational study. Am J Clin Nutr. 2017;106:614–22. https://doi.org/10.3945/ajcn.116.145391.
Fagherazzi G, Vilier A, Saes Sartorelli D, Lajous M, Balkau B, Clavel-Chapelon F. Consumption of artificially and sugar-sweetened beverages and incident type 2 diabetes in the Etude Epidemiologique aupres des femmes de la Mutuelle Generale de l’Education Nationale-European Prospective Investigation into Cancer and Nutrition cohort. Am J Clin Nutr. 2013;97:517–23. https://doi.org/10.3945/ajcn.112.050997.
Bhupathiraju SN, Pan A, Malik VS, Manson JE, Willett WC, van Dam RM, et al. Caffeinated and caffeine-free beverages and risk of type 2 diabetes. Am J Clin Nutr. 2013;97:155–66. https://doi.org/10.3945/ajcn.112.048603.
Sakurai M, Nakamura K, Miura K, Takamura T, Yoshita K, Nagasawa SY, et al. Sugar-sweetened beverage and diet soda consumption and the 7-year risk for type 2 diabetes mellitus in middle-aged Japanese men. Eur J Nutr. 2014;53:251–8. https://doi.org/10.1007/s00394-013-0523-9.
O’Connor L, Imamura F, Lentjes MA, Khaw KT, Wareham NJ, Forouhi NG. Prospective associations and population impact of sweet beverage intake and type 2 diabetes, and effects of substitutions with alternative beverages. Diabetologia. 2015;58:1474–83. https://doi.org/10.1007/s00125-015-3572-1.
Azad MB, Abou-Setta AM, Chauhan BF, Rabbani R, Lys J, Copstein L, et al. Non-nutritive sweeteners and cardiometabolic health: a systematic review and meta-analysis of randomized controlled trials and prospective cohort studies. CMAJ. 2017;189:E929–E939. https://doi.org/10.1503/cmaj.161390.
Toews I, Lohner S, Kullenberg de Gaudry D, Sommer H, Meerpohl JJ. Association between intake of non-sugar sweeteners and health outcomes: systematic review and meta-analyses of randomised and non-randomised controlled trials and observational studies. BMJ. 2019;364:k4718. https://doi.org/10.1136/bmj.k4718.
North KE, Howard BV, Welty TK, Best LG, Lee ET, Yeh JL, et al. Genetic and environmental contributions to cardiovascular disease risk in American Indians: the strong heart family study. Am J Epidemiol. 2003;157:303–14.
Block G, Thompson FE, Hartman AM, Larkin FA, Guire KE. Comparison of two dietary questionnaires validated against multiple dietary records collected during a 1-year period. J Am Diet Assoc. 1992;92:686–93.
Lee ET, Welty TK, Fabsitz R, Cowan LD, Le NA, Oopik AJ, et al. The Strong Heart Study. A study of cardiovascular disease in American Indians: design and methods. Am J Epidemiol. 1990;132:1141–55.
Marsh AP, Vance RM, Frederick TL, Hesselmann SA, Rejeski WJ. Objective assessment of activity in older adults at risk for mobility disability. Med Sci Sports Exerc. 2007;39:1020–6. https://doi.org/10.1249/mss.0b013e3180423ac3.
Suez J, Korem T, Zeevi D, Zilberman-Schapira G, Thaiss CA, Maza O, et al. Artificial sweeteners induce glucose intolerance by altering the gut microbiota. Nature. 2014;514:181–6. https://doi.org/10.1038/nature13793.
Pepino MY. Metabolic effects of non-nutritive sweeteners. Physiol Behav. 2015;152:450–5. https://doi.org/10.1016/j.physbeh.2015.06.024.
Greenwood DC, Threapleton DE, Evans CE, Cleghorn CL, Nykjaer C, Woodhead C, et al. Association between sugar-sweetened and artificially sweetened soft drinks and type 2 diabetes: systematic review and dose-response meta-analysis of prospective studies. Br J Nutr. 2014;112:725–34. https://doi.org/10.1017/s0007114514001329.
Koepsell TD, Weiss NS. Epidemiologic methods: studying the occurrence of illness. Oxford, New York: Oxford University Press; 2003.
Sievenpiper JL, Khan TA, Ha V, Viguiliouk E, Auyeung R. The importance of study design in the assessment of nonnutritive sweeteners and cardiometabolic health. CMAJ. 2017;189:E1424–E1425. https://doi.org/10.1503/cmaj.733381.
Malik VS. Non-sugar sweeteners and health. BMJ. 2019;364:k5005. https://doi.org/10.1136/bmj.k5005.
Acknowledgements
We thank the study participants and the Strong Heart Study staff.
Funding
The Strong Heart Family Study is supported by the National Institutes of Health cooperative agreement grants U01-HL41642, U01-HL41652, U01-HL41654, U01-HL65520, and U01-HL65521 and research grants R01-HL109315, R01-HL109301, R01-HL109284, R01-HL109282, and R01-HL109319. AMF is also supported by 5KL2TR000421.
Author information
Authors and Affiliations
Contributions
PNJ drafted the manuscript, analyzed the data, had full access to the data in the study, and had final responsibility for the decision to submit for publication. LB, MO, RBD, SAC, JWM, TA, ETL, FLY, and JY contributed to the interpretation of results and critically reviewed the manuscript. JGU and BVH contributed to the conception and design of the study, the acquisition of data, and critically reviewed the manuscript. AMF contributed to the conception and design of the study, the data analysis, and critically reviewed the manuscript. All authors approved the final version and agreed to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Jensen, P.N., Howard, B.V., Best, L.G. et al. Associations of diet soda and non-caloric artificial sweetener use with markers of glucose and insulin homeostasis and incident diabetes: the Strong Heart Family Study. Eur J Clin Nutr 74, 322–327 (2020). https://doi.org/10.1038/s41430-019-0461-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41430-019-0461-6