Abstract
Background/objectives
Vitamin D deficiency during pregnancy may influence adverse outcomes in offspring. The aim of this systematic review and meta-analysis of observational studies was to assess the association between low prenatal concentrations of 25(OH)D (by using three different cut-off levels), preterm birth (PTB) and anthropometric and neurodevelopmental outcomes in offspring.
Subjects/methods
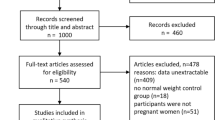
Studies reporting data on the association between maternal vitamin D concentrations and offspring outcomes identified through a systematic review of scientific literature published in PubMed/MEDLINE, Scopus and the Cochrane Library databases up to April 2017.
Results
We included 54 eligible studies. Vitamin D-deficient mothers (<30 nmol/L) had offspring with lower birthweight (MD −87.82 g; 95% CI −119.73, −55.91 g), head circumference (MD −0.19 cm; 95% CI −0.32, −0.06 cm) and a higher risk of small for gestational age (SGA) infants and PTB (OR 1.59; 95% CI 1.24, 2.03) compared to mothers with concentrations ≥30 nmol/L. Vitamin D insufficiency (<50 nmol/L) was associated with a higher risk of SGA and PTB (OR 1.43; 95% CI 1.08, 1.91 and OR 1.28; 95% CI 1.08, 1.52, respectively). Concentrations of 25(OH)D ≥75 nmol/L were not found to be associated with birthweight, SGA or PTB. Offspring of vitamin D-insufficient mothers had lower scores in mental (MD −1.12 points; 95% CI −1.82, −0.42 cm) and language developmental tests (MD −0.35 points; 95% CI −1.00, 0.31 cm).
Conclusion
Maternal vitamin D deficiency is associated with offspring adverse anthropometric outcomes and PTB; insufficiency with a higher risk of SGA, PTB and adverse neurodevelopmental outcomes.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout







Similar content being viewed by others
References
Holick MF. Vitamin D deficiency. N Engl J Med. 2017;357:266–81.
Gordon CM, Depeter KC, Feldman HA, Grace E, Emans SJ. Prevalence of vitamin D deficiency among healthy adolescents. Arch Pediatr Adolesc Med. 2004;158:531–7.
Lips P, Hosking D, Lippuner K, Norquist JM, Wehren L, Maalouf G. The prevalence of vitamin D inadequacy amongst women with osteoporosis: an international epidemiological investigation. J Intern Med. 2006;260:245–54.
Mulligan ML, Felton SK, Riek AE, Bernal-mizrachi C. Implications of vitamin D deficiency in pregnancy and lactation. Am J Obstet Gynecol. 2010;202:429.e1–9.
Aydogmus S, Kelekci S, Aydogmus H, Eriş S, Desdicioğlu R, Yilmaz B, et al. High prevalence of vitamin D deficiency among pregnant women in a Turkish population and impact on perinatal outcomes. J Matern Neonatal Med. 2015;28:1828–32.
Burris HH, Rifas-shiman SL, Camargo CAJ, Litonjua AA, Huh SY, Rich-Edwards JW.et al. Plasma 25-hydroxyvitamin D during pregnancy and small for gestational age in black and white infants. Ann Epidemiol. 2012;22:581–6.
Eckhardt CL, Gernand AD, Roth DE, Bodnar LM. Maternal vitamin D status and infant anthropometry in a US multi-centre cohort study. Ann Hum Biol. 2015;42:215–22.
Gernand AD, Simhan HN, Klebanoff MA, Bodnar LM. Maternal serum 25-hydroxyvitamin D and measures of newborn and placental weight in a U.S. multicenter cohort study. J Clin Endocrinol Metab. 2013;98:398–404.
Leffelaar ER, Vrijkotte TGM, Van Eijsden M. Maternal early pregnancy vitamin D status in relation to fetal and neonatal growth: results of the multi-ethnic Amsterdam Born Children and their Development cohort. Br J Nutr. 2010;104:108–17.
Miliku K, Vinkhuyzen A, Blanken LME, Mcgrath JJ, Eyles DW, Burne TH, et al. Maternal vitamin D concentrations during pregnancy, fetal growth patterns, and risks of adverse birth outcomes. Am J Clin Nutr. 2016;103:1514–22.
Song SJ, Si S, Liu J, Chen X, Zhou L, Jia G, et al. Vitamin D status in Chinese pregnant women and their newborns in Beijing and their relationships to birth size. Public Health Nutr. 2011;16:687–92.
Zhu P, Tong S, Hu W, Hao J, Tao R, Huang K, et al. Cord blood 25-hydroxyvitamin D and fetal growth in the China-Anhui Birth Cohort Study. Sci Rep. 2015;5:14930.
Boyle VT, Thorstensen EB, Mourath D, Jones MB, McCowan LME, Kenny LC, et al. The relationship between 25-hydroxyvitamin D concentration in early pregnancy and pregnancy outcomes in a large, prospective cohort. Br J Nutr. 2016;116:1409–15.
Perez Ferre N, Torrejon MJ, Fuentes M, Fernandez MD, Ramos A, Bordiu E, et al. Association of low serum 25-hydroxyvitamin D levels in pregnancy with glucose homeostasis and obstetric and newborn outcomes. Endocr Pract. 2012;18:676–84.
Schneuer FJ, Roberts CL, Guilbert C, Simpson JM, Algert CS, Khambalia AZ, et al. Effects of maternal serum 25-hydroxyvitamin D concentrations in the first trimester on subsequent pregnancy outcomes in an Australian population. Am J Clin Nutr. 2014;99:287–95.
Vinkhuyzen AAE, Eyles DW, Burne THJ, Blanken LME, Kruithof CJ, Verhulst F, et al. Gestational vitamin D deficiency and autism-related traits: the Generation R Study. Mol Psychiatry. 2016;0:1–7.
Gould JF, Anderson AJ, Yelland LN, Smithers LG, Skeaff CM, Zhou SJ, et al. Association of cord blood vitamin D with early childhood growth and neurodevelopment. J Paediatr Child Health. 2017;53:75–83.
Chawes BL, Bønnelykke K, Jensen PF, Schoos AM, Heickendorff L, Bisgaard H. Cord blood 25(OH)-vitamin D deficiency and childhood asthma, allergy and eczema: the COPSAC2000 birth cohort study. PLoS ONE. 2014;9:e99856.
Feng H, Xun P, Pike K, Wills A, Chawes B, Bisgaard H, et al. In utero exposure to 25-hydroxyvitamin D and risk of childhood asthma, wheeze, and respiratory tract infections: a meta-analysis of birth cohort studies. J Allergy Clin Immunol. 2017;139:1508–17.
Morales E, Romieu I, Guerra S, Ballester F, Rebagliato M, Vioque J, et al. Maternal vitamin D status in pregnancy and risk of lower respiratory tract infections, wheezing, and asthma in offspring. Epidemiology. 2012;23:64–71.
Pacheco-González RM, García-Marcos L, Morales E. Prenatal vitamin D status and respiratory and allergic outcomes in childhood: a meta-analysis of observational studies. Pediatr Allergy Immunol. 2018;29:243–53.
Morales E, Guxens M, Llop S, Rodriguez-Bernal CL, Tardon A, Riano I, et al. Circulating 25-hydroxyvitamin D3 in pregnancy and infant neuropsychological development. Pediatrics. 2012;130:e913–20.
Chi M, Zhu L, Zhang Z-L, Jin F-F, Shao H-R, Zheng J-Y, et al. The relationship between maternal serum vitamin D levels and infant neurodevelopment and anthropometry: a prospective observational study. J Nutr Sci Vitaminol. 2018;64:161–7.
Whitehouse AJ, Holt BJ, Serralha M, Holt PG, Kusel MM, Hart PH. Maternal serum vitamin D levels during pregnancy and offspring neurocognitive development. Pediatrics. 2012;129:485–93.
Hanieh S, Ha TT, Simpson JA, Thuy TT, Khuong NC, Thoang DD, et al. Maternal vitamin D status and infant outcomes in rural vietnam: a prospective cohort study. PLoS ONE. 2014;9:e99005.
Darling AL, Rayman MP, Steer CD, Golding J, Lanham-New SA, Bath SC. Association between maternal Vitamin D status in pregnancy and neurodevelopmental outcomes in childhood: results from the Avon Longitudinal Study of Parents and Children (ALSPAC). Br J Nutr. 2017;117:1682–92.
Tylavsky FA, Kocak M, Murphy LE, Graff JC, Palmer FB, Völgyi E, et al. Gestational vitamin 25(OH)D status as a risk factor for receptive language development: a 24-month, longitudinal, observational study. Nutrients. 2015;7:9918–30.
Chakhtoura M, Ghandour SEl, Shawwa K, Akl EA, Arabi A, Mahfoud Z, et al. Vitamin D replacement in children, adolescents and pregnant women in the Middle East and North Africa: a systematic review and meta-analysis of randomized controlled trials. Metabolism. 2017;70:160–76.
Qin L, Lu F, Yang S, Xu H, Luo B. Does maternal vitamin D deficiency increase the risk of preterm birth: a meta-analysis of observational studies. Nutrients. 2016;8:E301.
Abe S, Balogun O, Ota E, Takahashi K, Mori R. Supplementation with multiple micronutrients for breastfeeding women for improving outcomes for the mother and baby (Review). Cochrane Databases Syst Rev. 2016;CD010647.
Perez López F, Pasupuleti V, Mezones Holguin E, Benites Zapata V, Thota P, Deshpande A, et al. Effect of vitamin D supplementation during pregnancy on maternal and neonatal outcomes: a systematic review and meta-analysis of randomized controlled trials. Fertil Steril. 2015;103:1278–88.
Aghajafari F, Nagulesapillai T, Ronksley P, Tough S, O´Beirne M, Rabi D. Association between maternal serum 25-hydroxyvitamin D level and pregnancy and neonatal outcomes: systematic review and meta-analysis of. BMJ. 2013;1169:1–14.
Wei S, Qi H, Luo Z, Fraser WD. Maternal vitamin D status and adverse pregnancy outcomes: a systematic review and meta-analysis. Matern Neonatal Med. 2013;26:889–99.
Thorne-lyman A, Fawzi WW. Vitamin D during pregnancy and maternal, neonatal and infant health outcomes: a systematic review and meta-analysis. Pediatr Perinat Epidemiol. 2012;26:75–90.
Papapetrou P. The interrelationship of serum 1,25-dihydroxyvitamin D, 25-hydroxyvitamin D and 24,25-dihydroxyvitamin D in pregnancy at term: a meta-analysis. Hormones. 2010;9:136–44.
Roth DE, Leung M, Mesfin E, Qamar H, Watterworth J, Papp E. Vitamin D supplementation during pregnancy: state of the evidence from a systematic review of randomised trials. BMJ. 2017;359:j5237.
Santamaria C, Bi WG, Leduc L, Tabatabaei N, Jantchou P, Luo Z-C, et al. Prenatal vitamin D status and offspring’s growth, adiposity and metabolic health: a systematic review and meta-analysis. Br J Nutr. 2018;25:1–10.
Stroup D, Berlin J, Morton S, Olkin I, Williamson D, Rennie D, et al. Meta-analisis of observational studies in epidemiology. JAMA. 2000;19:2008–12.
Moher D, Liberati A, Tetzlaff J, Altman DG, Group P. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. BMJ. 2009;339:332–6.
Institute of Medicine. Dietary reference intakes for calcium and Vitamin D. Washington, DC: National Academy Press; 2010.
Holick MF, Binkley NC, Bischoff-Ferrari HA, Gordon CM, Hanley DA, Heaney RP, et al. Evaluation, treatment, and prevention of vitamin D deficiency: an endocrine society clinical practice guideline. J Clin Endocrinol Metab. 2011;96:1911–30.
Vitamin D Council. https://www.vitamindcouncil.org/for-health-professionals-position-statement-on-supplementation-blood-levels-and-sun-exposure/ (accessed 22 May 2018).
Von Elm E, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, Vandenbroucke JP. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. J Clin Epidemiol. 2008;61:344–9.
Higgins JPT, Thompson SG, Deeks JJ, Altman DG. Measuring inconsistency in meta-analyses. BMJ. 2003;327:557–60.
StataCorp. Stata Statistical Software: Release 12. College Station, TX: StataCorp LP; 2011.
Sedgwick P. Meta-analyses: how to read a funnel plot. BMJ. 2013;1342:1–2.
Review Manager (RevMan) [Computer program]. Version 5.3. Copenhagen: The Nordic Cochrane Centre; 2014.
Wang H, Xiao Y, Zhang L, et al. Maternal early pregnancy vitamin D status in relation to low birth weight and small-for-gestational-age offspring. J Steroid Biochem Mol Biol. 2018;175:146–50.
Ates S, Sevket O, Ozcan P, Ozkal F, Kaya MO, Dane B. Vitamin D status in the first-trimester: effects of Vitamin D deficiency on pregnancy outcomes. Afr Health Sci. 2016;16:36–43.
Dalgärd C, Petersen MS, Steuerwald U, Weihe P, Grandjean P. Umbilical cord serum 25-hydroxyvitamin D concentrations and relation to birthweight, head circumference and infant length at age 14 days. Paediatr Perinat Epidemiol. 2016;30:238–45.
Eggemoen A, Jenum A, Mdala I, Knutsen K, Largelov P, Sletner L. Vitamin D levels during pregnancy and associations with birth weight and body composition of the newborn: a longitudinal multiethnic population-based study. Br J Nutr. 2017;117:985–93.
Farrant HJW, Krishnaveni G, Hill J, Boucher B, Fisher D, Noonan K, et al. Vitamin D insufficiency is common in Indian mothers but is not associated with gestational diabetes or variation in newborn size. Eur J Clin Nutr. 2009;63:646–52.
Gale CR, Robinson SM, Harvey NC, Javaid MK, Jiang B, Martyn CN, et al. Maternal vitamin D status during pregnancy and child outcomes. Eur J Clin Nutr. 2008;62:68–77.
Morley R, Carlin JB, Pasco JA, Wark JD. Maternal 25-hydroxyvitamin D and parathyroid hormone concentrations and offspring birth size. J Clin Endocrinol Metab. 2006;91:906–12.
Ong YL, Quah PL, Tint MT, Aris IM, Wei L. The association of maternal vitamin D status with infant birth outcomes, postnatal growth and adiposity in the first two years of life in a multi-ethnic Asian population: the GUSTO cohort study. Br J Nutr. 2016;116:621–31.
Rodriguez A, García-Esteban R, Basterretxea M, Lertxundi A, Rodríguez-Bernal C, Iñiguez C, et al. Associations of maternal circulating 25-hydroxyvitamin D3 concentration with pregnancy and birth outcomes. BJOG. 2015;122:1695–704.
Weinert S, Reichelt AJ, Schmitt LR, Boff R, Oppermann R, Camargo JL, et al. Vitamin D deficiency increases the risk of adverse neonatal outcomes in gestational diabetes. PLoS ONE. 2016;11:1–11.
Shor DB-A, Barzel J, Tauber E, Amital H. The effects of maternal vitamin D on neonatal growth parameters. Eur J Pediatr. 2015;174:1169–74.
Viljakainen HT, Saarnio E, Hytinantti T, Miettinen M, Surcel H, Mäkitie O, et al. Maternal vitamin D status determines bone variables in the newborn. J Clin Endocrinol Metab. 2010;95:1749–57.
Chen Y, Zhu B, Wu X, Li S, Tao F. Association between maternal vitamin D deficiency and small for gestational age: evidence from a meta-analysis of prospective cohort studies. BMJ Open. 2017;27:1–10.
Chen Y-H, Fu L, Hao J-H, Yu Z, Zhu P, Wang H, et al. Maternal vitamin D deficiency during pregnancy elevates the risks of small for gestational age and low birth weight infants in Chinese population. J Clin Endocrinol Metab. 2015;100:1912–9.
Bodnar L, Catov J, Zmuda J, Cooper M, Parrott M, Roberts J, et al. Maternal serum 25-hydroxyvitamin D concentrations are associated with small-for-gestational age births in white women. Am J Clin Nutr. 2010;140:999–1006.
Swamy G, Garret M, Miranda M, Ashley-Koch A. Maternal vitamin D receptor genetic variation contributes to infant birthweight among black mothers. Am J Med Genet A. 2011;155:1264–71.
Kim JH, Jun G, Donghee K, Jae L, Ko H, Lim I, et al. Higher maternal vitamin D concentrations are associated with longer leukocyte telomeres in newborns. Matern Child Nutr. 2017;14. https://doi.org/10.1111/mcn.12475.
De Regil L, Palacios C, Lombardo L, Peña-rosas J. Vitamin D supplementation for women during pregnancy (Review). Cochrane Databases Syst Rev. 2016;CD008873.
Bollopragada S, Youssef R, Jordan F, Greer I, Norman J, Nelson S. Term labor is associated with a core inflammatory response in human fetal membranes, myometrium and cervix. Am J Obstet Gynecol. 2009;200:104.e1–11.
Muller K, Diamant M, Bendtzen K. Inhibition of production and functionof interleukin-6 by 1,25 hydroxyvitamin D3. Immunol Lett. 1991;28:115–20.
Muller K, Odum N, Bendtzen K. 1,25 hydroxyvitamin D3 selectively reduce interleukin 2 levels and proliferation of human T cell lines in vitro. Immunol Lett. 1993;35:177–82.
Azzieh F, Alyahya K, Raghupathy R. Association between levels of vitamin D and inflammatory markers in healthy women. J Inflamm Res. 2016;9:51–7.
Tolppanen A-M, Sayers A, Fraser WD, Lawlor DA. Association of serum 25-hydroxyvitamin D3 and D2 with academic performance in childhood: findings from a prospective birth cohort. J Epidemiol Community Health. 2012;66:1137–42.
Staples J, Ponsonby A-L, Lim L. Low maternal exposure to ultraviolet radiation in pregnancy, month of birth, and risk of multiple sclerosis in offspring: longitudinal analysis. BMJ. 2010;340:c1640.
Arija V, Fargas F, March G, Abajo S, Basora J, Canals J, et al. Adapting iron dose supplementation in pregnancy for greater effectiveness on mother and child health: protocol of the ECLIPSES randomized clinical trial. BMC Pregnancy Childbirth. 2014;14:33.
Sigurdsson T, Duvarci S. Hippocampal-prefrontal interactions in cognition, behavior and psychiatric disease. Front Syst Neurosci. 2016;9:1–18.
Nie J, Li G, Wang L, Gilmore JH, Lin W, Shen D. A computational growth model for measuring dynamic cortical development in the first year of life. Cereb Cortex. 2012;22:2272–84.
Raizada R, Kishiyama M. Effects of socioeconomic status on brain development, and how cognitive neuroscience may contribute to leveling the playing field. Front Hum Neurosci. 2010;4:1–11.
Belfort MB, Rifas-Shiman SL, Kleinman KP, Guthrie LB, Bellinger DC, Taveras EM, et al. Infant feeding and childhood cognition at ages 3 and 7 years: effects of breastfeeding duration and exclusivity. JAMA Pediatr. 2013;167:836–44.
Kingston D, Tough S. Prenatal and postnatal maternal mental health and school-age child development: a systematic review. Matern Child Health J. 2014;18:1728–41.
Zhu P, Tong S, Hao J, Tao R, Huang K, Hu W, et al. Cord blood vitamin D and neurocognitive development are nonlinearly related in toddlers. J Nutr. 2015;145:1232–8.
Almeras L, Eyles D, Benech P, Laffite D, Villard C, Patatian A, et al. Developmental vitamin D deficiency alters brain protein expression in the adult rat: implications for neuropsychiatric disorders. Proteomics. 2007;7:769–80.
Bodnar L, Platt R, Simhan H. Early-pregnancy vitamin D deficiency and risk of preterm birth subtypes. Obstet Gynecol. 2015;125:439–47.
Choi R, Kim S, Yoo H, Cho YY, Kim SW, Chung JH, et al. High prevalence of vitamin D deficiency in pregnant Korean women: the first trimester and the winter season as risk factors for vitamin D deficiency. Nutrients. 2015;7:3427–48.
Flood Nichols SK, Tinnemore D, Huang RR, Napolitano PG, Ippolito DL. Vitamin D deficiency in early pregnancy. PLoS ONE. 2015;10:1–15.
Gernad A, Simhan HN, Caritis S, Bodnar L. Maternal vitamin D status and small for gestational age offspring in women at high risk for preeclampsia. Obstet Gynecol. 2014;123:40–48.
Morgan C, Dodds L, Langille D, Weiler H, Armson B, Forest J, et al. Cord blood vitamin D status and neonatal outcomes in a birth cohort in Quebec, Canada. Arch Gynecol Obs. 2016;293:731–8.
Shand AW, Nassar N, Von Dadelszen P, Innis SM, Green TJ. Maternal vitamin D status in pregnancy and adverse pregnancy outcomes in a group at high risk for pre-eclampsia. BJOG. 2010;117:1593–8.
Thorp J, Camargo C, McGee P, Harper M, Klebanoff M, Sorokin Y, et al. Vitamin D status and recurrent preterm birth: a nested case-control study in high risk women. BJOG. 2012;119:1617–23.
Wagner CL, Baggerly C, McDonnell S, Baggerly KA, French CB, Baggerly L, et al. Post-hoc analysis of vitamin D status and reduced risk of preterm birth in two vitamin D pregnancy cohorts compared with South Carolina March of Dimes 2009-11 rates. J Steroid Biochem Mol Biol. 2016;155:245–51.
Yang L, Pan S, Zhou Y, Wang X, Qin A, Huang Y, et al. The correlation between serum vitamin D deficiency and preterm birth. Med Sci Monit. 2016;22:4401–5.
Fernández Alonso AM, Dionis Sánchez EC, Chedraui P, González Salmerón MD, Pérez López FR. First-trimester maternal serum 25-hydroxyvitamin D 3 status and pregnancy outcome. Int J Gynecol Obstet. 2012;116:6–9.
Bowyer L, Catling-Paull C, Diamond T, Homer C, Davis G, Craig ME. Vitamin D, PTH and calcium levels in pregnant women and their neonates. Clin Endocrinol. 2009;70:372–7.
McDonnell SL, Baggerly KA, Baggerly CA, Aliano JL, French CB, Baggerly LL, et al. Maternal 25(OH)D concentrations≥40 ng/mL associated with 60% lower preterm birth risk among general obstetrical patients at an urban medical center. PLoS ONE. 2017;12:1–12.
Reichetzeder C, Chen H, Föller M, Slowinski T, Li J, Chen YP, et al. Maternal vitamin D deficiency and fetal programming - lessons learned from humans and mice. Kidney Blood Press Res. 2014;39:315–29.
Baker A, Haeri S, Camargo C, Stuebe A, Boggess K. A nested case-control study of first-trimester maternal vitamin D status and risk for spontaneous preterm birth. Am J Perinatol. 2011;28:667–71.
Bärebring L, Bullarbo M, Glantz A, Hulthén L, Ellis J, Jagner Å, et al. Trajectory of vitamin D status during pregnancy in relation to neonatal birth size and fetal survival: a prospective cohort study. BMC Pregnancy Childbirth. 2018;18:51.
Ertl R, Yu KH, Samaha R.. Maternal serum vitamin D at 11 - 13 weeks in pregnancies delivering small for gestational age neonates. Fetal Diagn Ther. 2011;31:103–8.
Seto TL, Tabangin ME, Langdon G, Mangeot C, Dawodu A, Steinhoff M, et al. Racial disparities in cord blood vitamin D levels and its association with small-for-gestational-age infants. J Perinatol. 2016;36:623–8.
Tabatabaei N, Auger N, Herba CM, Wei S, Allard C, Fink GD, et al. Maternal vitamin D insufficiency early in pregnancy is associated with increased risk of preterm birth in ethnic minority women. J Nutr. 2017;147:1–7.
Wetta L, Biggio J, Cliver S, Abramovici A, Barnes S, Tita A. Is midtrimester vitamin D status associated with spontaneous preterm birth and preeclampsia? Am J Perinatol. 2014;31:541–6.
Zhou J, Su L, Liu M, Liu Y, Cao X, Wang Z, et al. Associations between 25-hydroxyvitamin D levels and pregnancy outcomes: a prospective observational study in southern China. Eur J Clin Nutr. 2014;68:925–30.
Zhu T, Liu T-J, Ge X, Kong J, Zhang L-J, Zhao Q. High prevalence of maternal vitamin D deficiency in preterm births in northeast China, Shenyang. Int J Clin Exp Pathol. 2015;28:1828–32.
Keim SA, Bodnar LM, Klebanoff MA. Maternal and cord blood 25(OH)-vitamin D concentrations in relation to child development and behaviour. Paediatr Perinat Epidemiol. 2014;28:434–44.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Supplementary information
Rights and permissions
About this article
Cite this article
Tous, M., Villalobos, M., Iglesias, L. et al. Vitamin D status during pregnancy and offspring outcomes: a systematic review and meta-analysis of observational studies. Eur J Clin Nutr 74, 36–53 (2020). https://doi.org/10.1038/s41430-018-0373-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41430-018-0373-x
This article is cited by
-
Association between vitamin D level in mother’s serum and the level of vitamin D in the serum of pre-term infants
BMC Pediatrics (2023)
-
Maternal plasma vitamin D levels across pregnancy are not associated with neonatal birthweight: findings from an Australian cohort study of low-risk pregnant women
BMC Pregnancy and Childbirth (2023)
-
Maternal and neonatal blood vitamin D status and neurodevelopment at 24 months of age: a prospective birth cohort study
World Journal of Pediatrics (2023)
-
Predictors of 25-hydroxyvitamin D concentrations during pregnancy: A longitudinal analysis in the Brazilian Amazon
European Journal of Clinical Nutrition (2022)
-
Risk factors of lower birth weight, small-for-gestational-age infants, and preterm birth in pregnancies following bariatric surgery: a scoping review
Archives of Gynecology and Obstetrics (2022)