Abstract
Background/Objectives
Weight loss diets affect food choices and control of eating. We evaluated the effects of intermittent energy restriction (IER) vs. continuous energy restriction (CER) on nutritional composition and eating behavior.
Subject/Methods
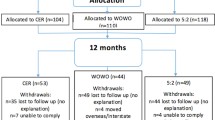
Individuals with BMI 30–45 kg/m2, abdominal obesity and ≥1 additional metabolic syndrome component were randomized to IER vs. CER with similar energy restriction. Of 112 participants, 98 completed weighed dietary records and the Three Factor Eating Questionnaire at baseline and three months. In statistical analysis, changes were adjusted for baseline values.
Results
Weight loss, energy intake, and macronutrient composition were similar in the IER and CER groups. The CER group reported a greater increase in fruit and berries (45 g/day [95% CI 21, 71] vs. 2 g/day [−28, 33]; p = 0.047) and vegetables (135 g/day [91, 179] vs. 65 g/day [35, 96]; p = 0.010) than the IER group. Fiber intake increased in the CER compared to the IER group (1.0 g/MJ/day [0.8, 1.2] vs. 0.2 [0.0, 0.4]; p < 0.001). Sugar intake was reduced in the CER compared to the IER group (−2.2E% [−3.2, −2.2] vs. −0.1E% [−1.2, 1.0]; p = 0.007). Intakes of folate, potassium, and magnesium decreased more in the IER than the CER group, while vitamin C increased more in the CER group (all p-values <0.014). Both diets improved eating behavior scores, but cognitive restraint increased more in the CER than the IER group (34 [30, 39] vs. 17 [12, 22]; p = 0.013).
Conclusions
Men and women with obesity had more favorable changes in nutritional composition and eating behavior with CER than IER.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
World Health Organization. Obesity and overweight. Fact Sheet No. 311. 2014. URL http://www.who.int/mediacentre/factsheets/fs311/en/ [accessed April 2015].
Guh DP, Zhang W, Bansback N, Amarsi Z, Birmingham CL, Anis AH The incidence of co‐morbidities related to obesity and overweight: a systematic review and meta‐analysis. BMC Public Health. 2009;9-88; https://doi.org/10.1186/1471-2458-9-88.
Jensen MD, Ryan DH, Apovian CM, Ard JD, Comuzzie AG, Donato KA, et al. 2013 AHA/ACC/TOS guideline for the management of overweight and obesity in adults: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines and The Obesity Society. American College of Cardiology/American Heart Association Task Force on Practice Guidelines; Obesity Society. J Am Coll Cardiol. 2014;63:2985–3023. https://doi.org/10.1016/j.jacc.2013.11.004.(25 Pt B)Epub 2013 Nov 12.
Yumuk V1, Tsigos C, Fried M, Schindler K, Busetto L, Micic D, Toplak H. European Guidelines for Obesity Management in Adults. Obesity Management Task Force of the European Association for the Study of Obesity. Obes Facts. 2015;8:402–24. https://doi.org/10.1159/000442721. Epub 2015 Dec 5.
Tapsell LC, Neale EP, Satija A, Hu FB. Foods, nutrients, and dietary patterns: interconnections and implications for dietary guidelines. Adv Nutr. 2016;7:445–54. https://doi.org/10.3945/an.115.011718.
Schwingshackl L, Hoffmann G. Diet quality as assessed by the Healthy Eating Index, the Alternate Healthy Eating Index, the Dietary Approaches to Stop Hypertension score, and health outcomes: A systematic review and meta-analysis of cohort studies. J Acad Nutr Diet. 2015;115:780–800.e785. https://doi.org/10.1016/j.jand.2014.12.009.
Schwingshackl L, Bogensberger B, Hoffmann G.Diet Quality as Assessed by the Healthy Eating Index, Alternate Healthy Eating Index, Dietary Approaches to Stop Hypertension Score, and Health Outcomes: An Updated Systematic Review and Meta-Analysis of Cohort Studies. J Acad Nutr Diet. 2018;118:74–100.e11. https://doi.org/10.1016/j.jand.2017.08.024.
Reedy J, Krebs-Smith SM, Miller PE, Liese AD, Kahle LL, Park Y, Subar AF. Higher diet quality is associated with decreased risk of all-cause, cardiovascular disease, and cancer mortality among older adults. J Nutr. 2014;144:881–9. https://doi.org/10.3945/jn.113.189407. Epub 2014 Feb 26.
Jacobs DR,Jr, Steffen LM. Nutrients, foods, and dietary patterns as exposures in research: a framework for food synergy. Am J Clin Nutr. 2003;78(3 Suppl):508S–513S. https://doi.org/10.1093/ajcn/78.3.508S.
Greenberg I, Stampfer MJ, Schwarzfuchs D, Shai. Adherence and success in long-term weight loss diets: the dietary intervention randomized controlled trial (DIRECT). J Am Coll Nutr. 2009;28:159–68.
Greenway FL. Physiological adaptations to weight loss and factors favouring weight regain. Int J Obes. 2015;39:1188–96. https://doi.org/10.1038/ijo.2015.59. Epub 2015 Apr 21.
Keränen AM, Savolainen MJ, Reponen AH, Kujari ML, Lindeman SM, Bloigu RS, et al. The effect of eating behavior on weight loss and maintenance during a lifestyle intervention. Prev Med. 2009;49:32–8. https://doi.org/10.1016/j.ypmed.2009.04.011. Epub 2009 May 4.
Sarlio-Lähteenkorva S, Rissanen A. Weight loss maintenance: determinants of long-term success. Eat Weight Disord. 1998;3:131–5.
Nurkkala M, Kaikkonen K, Vanhala ML, Karhunen L, Keränen AM, Korpelainen R. Lifestyle intervention has a beneficial effect on eating behavior and long-term weight loss in obese adults. Eat Behav. 2015;18:179–85. https://doi.org/10.1016/j.eatbeh.2015.05.009. Epub 2015 Jun 10.
Sundfør TM, Svendsen M, Tonstad S. Effect of intermittent versus continuous energy restriction on weight loss, maintenance and cardiometabolic risk: A randomized 1-year trial. Nutr Metab Cardiovasc Dis. 2018;28:698–706. https://doi.org/10.1016/j.numecd.2018.03.009. Epub 2018 Mar 29.
Thomas DM, Martin CK, Redman LM, Heymsfield SB, Lettieri S, Levine JA, Bouchard C, Schoeller DA. Effect of dietary adherence on the body weight plateau: a mathematical model incorporating intermittent compliance with energy intake prescription. Am J Clin Nutr. 2014;100:787–95. https://doi.org/10.3945/ajcn.113.079822. Epub2014 Jul 30.
James BL, Roe LS, Loken E, Rolls BJ. Early predictors of weight loss in a 1‐year behavioural weight‐loss programme. Obes Sci Pract. 2018;4:20–28. https://doi.org/10.1002/osp4.149. Published online 2018 Jan 12.
Thompson FE, Byers T. Dietary assessment resource manual. J Nutr. 1994;124(11 Suppl):2245S–2317S.
Kostholdsplanleggeren. https://www.kostholdsplanleggeren.no/ [accessed March 2018].
The Food Composition Table 2017. Food Safety Authority, Directorate of health and the University of Oslo. www.matvaretabellen.no". [accessed March 2018].
Nordic Council of Ministers (2014), Nordic Nutrition Recommendations 2012: Integrating nutrition and physical activity, Nord, Nordic Council of Ministers, Copenhagen K, https://doi.org/10.6027/Nord2014-002.
Cappelleri JC, Bushmakin AG, Gerber RA, Leidy NK, Sexton CC, Lowe MR, Karlsson J. Psychometric analysis of the Three-Factor Eating Questionnaire-R21: results from a large diverse sample of obese and non-obese participants. Int J Obes (Lond). 2009;33:611–20. https://doi.org/10.1038/ijo.2009.74.
Karlsson J, Persson LO, Sjostrom L, Sullivan M. Psychometric properties and factor structure of the Three-Factor Eating Questionnaire (TFEQ) in obese men and women. Results from the Swedish Obese Subjects (SOS) study. Int J Obes Relat Metab Disord. 2000;24:1715–25. https://doi.org/10.1038/sj.ijo.0801442.
Elliott AC, Woodward WA. Statistical analysis quick reference guidebook with SPSS examples. 1st ed. London: Sage Publications; 2007.
Thomas DM, Gonzalez MC, Pereira AZ, Redman LM, Heymsfield SB. Time to correctly predict the amount of weight loss with dieting. J Acad Nutr Diet. 2014;114:857–61. https://doi.org/10.1016/j.jand.2014.02.003. Epub 2014 Mar 31.
Diet, nutrition and the prevention of chronic diseases: Report of the joint WHO/FAO expert consultation, WHO Technical Report Series, No. 916 (TRS 916). Publication date: 2003.
Prevention of cardiovascular disease: Guideline for assessment and management of cardiovascular risk. WHO. Publication date: 2007.
Guideline: Sugars Intake for Adults and Children. Geneva: WHO; 2015. P. https://www.ncbi.nlm.nih.gov/books/NBK285537/.
Mozaffarian D, Hao T, Rimm EB, Willett WC, Hu FB. Changes in diet and lifestyle and long-term weight gain in women and men. N Engl J Med. 2011;364:2392–404. https://doi.org/10.1056/NEJMoa1014296.
Fogelholm M, Anderssen S, Gunnarsdottir I, Lahti-Koski M Dietary macronutrients and food consumption as determinants of long-term weight change in adult populations: a systematic literature review. Food Nutr Res 2012;56. https://doi.org/10.3402/fnr.v56i0.19103. Epub2012 Aug 13.
Gardner CD, Kim S, Bersamin A, Dopler-Nelson M, Otten J, Oelrich B, Cherin R. Micronutrient quality of weight-loss diets that focus on macronutrients: results from the ATOZ study. Am J Clin Nutr. 2010;92:304–12. https://doi.org/10.3945/ajcn.2010.29468. Epub 2010 Jun 23.
Rachel K Johnson. Dietary Intake—How Do We Measure What People Are Really Eating? First published: 17 September 2012. https://doi.org/10.1038/oby.2002.192.
Westerterp-Plantenga MS, Kempen KP, Saris WH. Determinants of weight maintenance in women after diet-induced weight reduction. Int J Obes Relat Metab Disord. 1998;22:1–6.
Vogels N, Westerterp-Plantenga MS. Successful long-term weight maintenance: a 2-year follow-up. Obes (Silver Spring). 2007;15:1258–66.
Lara JJ, Scott JA, Lean ME. Intentional mis-reporting of food consumption and its relationship with body mass index and psychological scores in women. J Hum Nutr Diet. 2004;17:209–18. https://doi.org/10.1111/j.1365-277X.2004.00520.
Acknowledgements
We thank Merete Helgeland MS in Nutrition for assistance with dietary counseling, Hanna Frydenberg MS in Nutrition for help with analyzing the dietary records, Sasa Dusanov MD, Eli Heggen MD PhD and Tor Ole Klemsdal MD PhD for medical examinations, and Ragnhild Kleve and Lise Bergengen for assistance with study procedures.
Author information
Authors and Affiliations
Contributions
T.M.S., S.T., and M.S. designed the study; T.M.S. conducted the dietary counselling and project supervision; T.M.S. analyzed the data; and T.M.S., S.T., and M.S. wrote the paper. S.T. had primary responsibility for the final content. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Sundfør, T.M., Tonstad, S. & Svendsen, M. Effects of intermittent versus continuous energy restriction for weight loss on diet quality and eating behavior. A randomized trial. Eur J Clin Nutr 73, 1006–1014 (2019). https://doi.org/10.1038/s41430-018-0370-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41430-018-0370-0
This article is cited by
-
Self-initiated lifestyle changes during a fasting-mimicking diet programme in patients with type 2 diabetes: a mixed-methods study
BMC Primary Care (2024)
-
Network meta-analysis of three different forms of intermittent energy restrictions for overweight or obese adults
International Journal of Obesity (2024)
-
Time-restricted eating (16/8) and energy-restricted diet: effects on diet quality, body composition and biochemical parameters in healthy overweight females
BMC Nutrition (2023)
-
Integration of Time-Based Recommendations with Current Pediatric Health Behavior Guidelines: Implications for Obesity Prevention and Treatment in Youth
Current Obesity Reports (2022)
-
Importance of circadian timing for aging and longevity
Nature Communications (2021)