Abstract
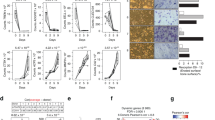
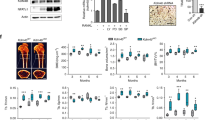
Monocyte/macrophage lineage cells are highly plastic and can differentiate into various cells under different environmental stimuli. Bone-resorbing osteoclasts are derived from the monocyte/macrophage lineage in response to receptor activator of NF-κB ligand (RANKL). However, the epigenetic signature contributing to the fate commitment of monocyte/macrophage lineage differentiation into human osteoclasts is largely unknown. In this study, we identified RANKL-responsive human osteoclast-specific superenhancers (SEs) and SE-associated enhancer RNAs (SE-eRNAs) by integrating data obtained from ChIP-seq, ATAC-seq, nuclear RNA-seq and PRO-seq analyses. RANKL induced the formation of 200 SEs, which are large clusters of enhancers, while suppressing 148 SEs in macrophages. RANKL-responsive SEs were strongly correlated with genes in the osteoclastogenic program and were selectively increased in human osteoclasts but marginally presented in osteoblasts, CD4+ T cells, and CD34+ cells. In addition to the major transcription factors identified in osteoclasts, we found that BATF binding motifs were highly enriched in RANKL-responsive SEs. The depletion of BATF1/3 inhibited RANKL-induced osteoclast differentiation. Furthermore, we found increased chromatin accessibility in SE regions, where RNA polymerase II was significantly recruited to induce the extragenic transcription of SE-eRNAs, in human osteoclasts. Knocking down SE-eRNAs in the vicinity of the NFATc1 gene diminished the expression of NFATc1, a major regulator of osteoclasts, and osteoclast differentiation. Inhibiting BET proteins suppressed the formation of some RANKL-responsive SEs and NFATc1-associated SEs, and the expression of SE-eRNA:NFATc1. Moreover, SE-eRNA:NFATc1 was highly expressed in the synovial macrophages of rheumatoid arthritis patients exhibiting high-osteoclastogenic potential. Our genome-wide analysis revealed RANKL-inducible SEs and SE-eRNAs as osteoclast-specific signatures, which may contribute to the development of osteoclast-specific therapeutic interventions.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout







Similar content being viewed by others
References
Tsukasaki M, Takayanagi H. Osteoimmunology: evolving concepts in bone-immune interactions in health and disease. Nat Rev Immunol. 2019;19:626–42. https://doi.org/10.1038/s41577-019-0178-8.
Park-Min KH. Mechanisms involved in normal and pathological osteoclastogenesis. Cell Mol life Sci: CMLS. 2018;75:2519–28. https://doi.org/10.1007/s00018-018-2817-9.
Novack DV, Teitelbaum SL. The osteoclast: friend or foe? Annu Rev Pathol. 2008;3:457–84. https://doi.org/10.1146/annurev.pathmechdis.3.121806.151431.
Goldring SR. Pathogenesis of bone and cartilage destruction in rheumatoid arthritis. Rheumatol (Oxf). 2003;42(Suppl 2):ii11–16. https://doi.org/10.1093/rheumatology/keg327.
Sato K, Takayanagi H. Osteoclasts, rheumatoid arthritis, and osteoimmunology. Curr Opin Rheumatol. 2006;18:419–26. https://doi.org/10.1097/01.bor.0000231912.24740.a5.
Schett G, Gravallese E. Bone erosion in rheumatoid arthritis: mechanisms, diagnosis and treatment. Nat Rev Rheumatol. 2012;8:656–64. https://doi.org/10.1038/nrrheum.2012.153.
Yasui T, Hirose J, Tsutsumi S, Nakamura K, Aburatani H, Tanaka S. Epigenetic regulation of osteoclast differentiation: possible involvement of Jmjd3 in the histone demethylation of Nfatc1. J Bone Min Res. 2011;26:2665–71.
Asagiri M, Sato K, Usami T, Ochi S, Nishina H, Yoshida H, et al. Autoamplification of NFATc1 expression determines its essential role in bone homeostasis. J Exp Med. 2005;202:1261–9.
Yasui T, Hirose J, Aburatani H, Tanaka S. Epigenetic regulation of osteoclast differentiation. Ann N. Y Acad Sci. 2011;1240:7–13.
Carey HA, Hildreth BE, Samuvel DJ, Thies KA, Rosol TJ, Toribio RE, et al. Eomes partners with PU.1 and MITF to Regulate Transcription Factors Critical for osteoclast differentiation. iScience. 2019;11:238–45. https://doi.org/10.1016/j.isci.2018.12.018.
Park-Min KH. Epigenetic regulation of bone cells. Connect Tissue Res. 2017;58:76–89. https://doi.org/10.1080/03008207.2016.1177037.
Li J, Sarosi I, Yan XQ, Morony S, Capparelli C, Tan HL, et al. RANK is the intrinsic hematopoietic cell surface receptor that controls osteoclastogenesis and regulation of bone mass and calcium metabolism. Proc Natl Acad Sci USA. 2000;97:1566–71.
Kong YY, Yoshida H, Sarosi I, Tan HL, Timms E, Capparelli C, et al. OPGL is a key regulator of osteoclastogenesis, lymphocyte development and lymph-node organogenesis. Nature. 1999;397:315–23. https://doi.org/10.1038/16852.
Dougall WC, Glaccum M, Charrier K, Rohrbach K, Brasel K, De Smedt T, et al. RANK is essential for osteoclast and lymph node development. Genes Dev. 1999;13:2412–24. https://doi.org/10.1101/gad.13.18.2412.
Takayanagi H, Kim S, Koga T, Nishina H, Isshiki M, Yoshida H, et al. Induction and activation of the transcription factor NFATc1 (NFAT2) integrate RANKL signaling in terminal differentiation of osteoclasts. Developmental cell. 2002;3:889–901.
Winslow MM, Pan M, Starbuck M, Gallo EM, Deng L, Karsenty G, et al. Calcineurin/NFAT signaling in osteoblasts regulates bone mass. Developmental cell. 2006;10:771–82. https://doi.org/10.1016/j.devcel.2006.04.006.
Aliprantis AO, Ueki Y, Sulyanto R, Park A, Sigrist KS, Sharma SM, et al. NFATc1 in mice represses osteoprotegerin during osteoclastogenesis and dissociates systemic osteopenia from inflammation in cherubism. J Clin Invest. 2008;118:3775–89. https://doi.org/10.1172/JCI35711.
Arrowsmith CH, Bountra C, Fish PV, Lee K, Schapira M. Epigenetic protein families: a new frontier for drug discovery. Nat Rev Drug Disco. 2012;11:384–400. https://doi.org/10.1038/nrd3674.
Berdasco M, Esteller M. Clinical epigenetics: seizing opportunities for translation. Nat Rev Genet. 2019;20:109–27. https://doi.org/10.1038/s41576-018-0074-2.
Nishikawa K, Iwamoto Y, Kobayashi Y, Katsuoka F, Kawaguchi S, Tsujita T, et al. DNA methyltransferase 3a regulates osteoclast differentiation by coupling to an S-adenosylmethionine-producing metabolic pathway. Nat Med. 2015;21:281–7. https://doi.org/10.1038/nm.3774.
Park-Min KH, Lim E, Lee MJ, Park SH, Giannopoulou E, Yarilina A, et al. Inhibition of osteoclastogenesis and inflammatory bone resorption by targeting BET proteins and epigenetic regulation. Nat Commun. 2014;5:5418. https://doi.org/10.1038/ncomms6418.
Meng S, Zhang L, Tang Y, Tu Q, Zheng L, Yu L, et al. BET Inhibitor JQ1 Blocks Inflammation and Bone Destruction. J Dent Res. 2014;93:657–62. https://doi.org/10.1177/0022034514534261.
Williamson I, Hill RE, Bickmore WA. Enhancers: from developmental genetics to the genetics of common human disease. Dev Cell. 2011;21:17–19. https://doi.org/10.1016/j.devcel.2011.06.008.
Whyte WA, Orlando DA, Hnisz D, Abraham BJ, Lin CY, Kagey MH, et al. Master transcription factors and mediator establish super-enhancers at key cell identity genes. Cell. 2013;153:307–19. https://doi.org/10.1016/j.cell.2013.03.035.
Loven J, Hoke HA, Lin CY, Lau A, Orlando DA, Vakoc CR, et al. Selective inhibition of tumor oncogenes by disruption of super-enhancers. Cell. 2013;153:320–34. https://doi.org/10.1016/j.cell.2013.03.036.
Hnisz D, Abraham BJ, Lee TI, Lau A, Saint-Andre V, Sigova AA, et al. Super-enhancers in the control of cell identity and disease. Cell. 2013;155:934–47. https://doi.org/10.1016/j.cell.2013.09.053.
Stower H. Gene expression: Super enhancers. Nat Rev Genet. 2013;14:367. https://doi.org/10.1038/nrg3496.
Shin HY. Targeting Super-Enhancers for Disease Treatment and Diagnosis. Mol Cells. 2018;41:506–14. https://doi.org/10.14348/molcells.2018.2297.
Arnold PR, Wells AD, Li XC. Diversity and Emerging Roles of Enhancer RNA in Regulation of Gene Expression and Cell Fate. Front Cell Dev Biol. 2019;7:377. https://doi.org/10.3389/fcell.2019.00377.
Zentner GE, Henikoff S. Regulation of nucleosome dynamics by histone modifications. Nat Struct Mol Biol. 2013;20:259–66. https://doi.org/10.1038/nsmb.2470.
Adam RC, Yang H, Rockowitz S, Larsen SB, Nikolova M, Oristian DS, et al. Pioneer factors govern super-enhancer dynamics in stem cell plasticity and lineage choice. Nature. 2015;521:366–70. https://doi.org/10.1038/nature14289.
Carey HA, Hildreth BE, Geisler JA, Nickel MC, Cabrera J, Ghosh S, et al. Enhancer variants reveal a conserved transcription factor network governed by PU.1 during osteoclast differentiation. Bone Res. 2018;6:8. https://doi.org/10.1038/s41413-018-0011-1.
Ko JY, Oh S, Yoo KH. Functional Enhancers As Master Regulators of Tissue-Specific Gene Regulation and Cancer Development. Mol Cells. 2017;40:169–77. https://doi.org/10.14348/molcells.2017.0033.
Pefanis E, Wang J, Rothschild G, Lim J, Kazadi D, Sun J, et al. RNA exosome-regulated long non-coding RNA transcription controls super-enhancer activity. Cell. 2015;161:774–89. https://doi.org/10.1016/j.cell.2015.04.034.
Chang HC, Huang HC, Juan HF, Hsu CL. Investigating the role of super-enhancer RNAs underlying embryonic stem cell differentiation. BMC Genomics. 2019;20:896. https://doi.org/10.1186/s12864-019-6293-x.
Liang J, Zhou H, Gerdt C, Tan M, Colson T, Kaye KM, et al. Epstein-Barr virus super-enhancer eRNAs are essential for MYC oncogene expression and lymphoblast proliferation. Proc Natl Acad Sci USA. 2016;113:14121–6. https://doi.org/10.1073/pnas.1616697113.
Alvarez-Dominguez JR, Knoll M, Gromatzky AA, Lodish HF. The Super-Enhancer-Derived alncRNA-EC7/Bloodlinc Potentiates Red Blood Cell Development in trans. Cell Rep. 2017;19:2503–14. https://doi.org/10.1016/j.celrep.2017.05.082.
Kim TK, Hemberg M, Gray JM, Costa AM, Bear DM, Wu J, et al. Widespread transcription at neuronal activity-regulated enhancers. Nature. 2010;465:182–7. https://doi.org/10.1038/nature09033.
Kim, YW, Lee, S, Yun, J & Kim, A Chromatin looping and eRNA transcription precede the transcriptional activation of gene in the beta-globin locus. Biosci Rep. 2015;35. https://doi.org/10.1042/BSR20140126.
Benner C, Isoda T, Murre C. New roles for DNA cytosine modification, eRNA, anchors, and superanchors in developing B cell progenitors. Proc Natl Acad Sci USA. 2015;112:12776–81. https://doi.org/10.1073/pnas.1512995112.
Kaikkonen MU, Spann NJ, Heinz S, Romanoski CE, Allison KA, Stender JD, et al. Remodeling of the enhancer landscape during macrophage activation is coupled to enhancer transcription. Mol Cell. 2013;51:310–25. https://doi.org/10.1016/j.molcel.2013.07.010.
Meng FL, Du Z, Federation A, Hu J, Wang Q, Kieffer-Kwon KR, et al. Convergent transcription at intragenic super-enhancers targets AID-initiated genomic instability. Cell. 2014;159:1538–48. https://doi.org/10.1016/j.cell.2014.11.014.
Lai F, Orom UA, Cesaroni M, Beringer M, Taatjes DJ, Blobel GA, et al. Activating RNAs associate with Mediator to enhance chromatin architecture and transcription. Nature. 2013;494:497–501. https://doi.org/10.1038/nature11884.
Arner E, Daub CO, Vitting-Seerup K, Andersson R, Lilje B, Drabløs F, et al. Transcribed enhancers lead waves of coordinated transcription in transitioning mammalian cells. Science. 2015;347:1010–4. https://doi.org/10.1126/science.1259418.
Imamura K, et al. Diminished nuclear RNA decay upon Salmonella infection upregulates antibacterial noncoding RNAs. EMBO J. 2018;37. https://doi.org/10.15252/embj.201797723.
Dorighi KM, Swigut T, Henriques T, Bhanu NV, Scruggs BS, Nady N, et al. Mll3 and Mll4 Facilitate Enhancer RNA Synthesis and Transcription from Promoters Independently of H3K4 Monomethylation. Mol Cell. 2017;66:568–76 e564. https://doi.org/10.1016/j.molcel.2017.04.018.
Cheng JH, Pan DZ, Tsai ZT, Tsai HK. Genome-wide analysis of enhancer RNA in gene regulation across 12 mouse tissues. Sci Rep. 2015;5:12648. https://doi.org/10.1038/srep12648.
Ren C, Liu F, Ouyang Z, An G, Zhao C, Shuai J, et al. Functional annotation of structural ncRNAs within enhancer RNAs in the human genome: implications for human disease. Sci Rep. 2017;7:15518. https://doi.org/10.1038/s41598-017-15822-7.
Li W, Notani D, Ma Q, Tanasa B, Nunez E, Chen AY, et al. Functional roles of enhancer RNAs for oestrogen-dependent transcriptional activation. Nature. 2013;498:516–20. https://doi.org/10.1038/nature12210.
Andersson R, Gebhard C, Miguel-Escalada I, Hoof I, Bornholdt J, Boyd M, et al. An atlas of active enhancers across human cell types and tissues. Nature. 2014;507:455–61. https://doi.org/10.1038/nature12787.
Gordon RA, Grigoriev G, Lee A, Kalliolias GD, Ivashkiv LB. The interferon signature and STAT1 expression in rheumatoid arthritis synovial fluid macrophages are induced by tumor necrosis factor alpha and counter-regulated by the synovial fluid microenvironment. Arthritis rheumatism. 2012;64:3119–28. https://doi.org/10.1002/art.34544.
Arnett FC, Edworthy SM, Bloch DA, McShane DJ, Fries JF, Cooper NS, et al. The American Rheumatism Association 1987 revised criteria for the classification of rheumatoid arthritis. Arthritis rheumatism. 1988;31:315–24.
Park-Min KH, Serbina NV, Yang W, Ma X, Krystal G, Neel BG, et al. FcgammaRIII-dependent inhibition of interferon-gamma responses mediates suppressive effects of intravenous immune globulin. Immunity. 2007;26:67–78. https://doi.org/10.1016/j.immuni.2006.11.010.
Bae S, Lee MJ, Mun SH, Giannopoulou EG, Yong-Gonzalez V, Cross JR, et al. MYC-dependent oxidative metabolism regulates osteoclastogenesis via nuclear receptor ERRalpha. J Clin Invest. 2017;127:2555–68. https://doi.org/10.1172/JCI89935.
Miyauchi Y, Ninomiya K, Miyamoto H, Sakamoto A, Iwasaki R, Hoshi H, et al. The Blimp1-Bcl6 axis is critical to regulate osteoclast differentiation and bone homeostasis. J Exp Med. 2010;207:751–62. https://doi.org/10.1084/jem.20091957.
Zhu L, et al. Osteoclast-mediated bone resorption is controlled by a compensatory network of secreted and membrane-tethered metalloproteinases. Sci Transl Med. 2020;12. https://doi.org/10.1126/scitranslmed.aaw6143.
Zhao B, Takami M, Yamada A, Wang X, Koga T, Hu X, et al. Interferon regulatory factor-8 regulates bone metabolism by suppressing osteoclastogenesis. Nat Med. 2009;15:1066–71. https://doi.org/10.1038/nm.2007.
Kim I, Kim JH, Kim K, Seong S, Kim N. The IRF2BP2-KLF2 axis regulates osteoclast and osteoblast differentiation. BMB Rep. 2019;52:469–74.
Sun L, Lian JX, Meng S. MiR-125a-5p promotes osteoclastogenesis by targeting TNFRSF1B. Cell Mol Biol Lett. 2019;24:23. https://doi.org/10.1186/s11658-019-0146-0.
Wagner EF, Eferl R. Fos/AP-1 proteins in bone and the immune system. Immunol Rev. 2005;208:126–40. https://doi.org/10.1111/j.0105-2896.2005.00332.x.
Dorsey MJ, Tae HJ, Sollenberger KG, Mascarenhas NT, Johansen LM, Taparowsky EJ. B-ATF: a novel human bZIP protein that associates with members of the AP-1 transcription factor family. Oncogene. 1995;11:2255–65.
Echlin DR, Tae HJ, Mitin N, Taparowsky EJ. B-ATF functions as a negative regulator of AP-1 mediated transcription and blocks cellular transformation by Ras and Fos. Oncogene. 2000;19:1752–63. https://doi.org/10.1038/sj.onc.1203491.
Tussiwand R, Lee WL, Murphy TL, Mashayekhi M, KC W, Albring JC, et al. Compensatory dendritic cell development mediated by BATF-IRF interactions. Nature. 2012;490:502–7. https://doi.org/10.1038/nature11531.
Xiao S, Huang Q, Ren H, Yang M. The mechanism and function of super enhancer RNA. Genesis. 2021;59:e23422. https://doi.org/10.1002/dvg.23422.
De Santa F, Barozzi I, Mietton F, Ghisletti S, Polletti S, Tusi BK, et al. A large fraction of extragenic RNA pol II transcription sites overlap enhancers. PLoS Biol. 2010;8:e1000384. https://doi.org/10.1371/journal.pbio.1000384.
Dhaliwal NK, Mitchell JA. Nuclear RNA Isolation and Sequencing. Methods Mol Biol. 2016;1402:63–71. https://doi.org/10.1007/978-1-4939-3378-5_7.
Kwak H, Fuda NJ, Core LJ, Lis JT. Precise maps of RNA polymerase reveal how promoters direct initiation and pausing. Science. 2013;339:950–3. https://doi.org/10.1126/science.1229386.
Wang Z, Chu T, Choate LA, Danko CG. Identification of regulatory elements from nascent transcription using dREG. Genome Res. 2019;29:293–303. https://doi.org/10.1101/gr.238279.118.
Yarilina A, Xu K, Chen J, Ivashkiv LB. TNF activates calcium-nuclear factor of activated T cells (NFAT)c1 signaling pathways in human macrophages. Proc Natl Acad Sci USA. 2011;108:1573–8. https://doi.org/10.1073/pnas.1010030108.
Abdallah BM, Al-Shammary A, Skagen P, Abu Dawud R, Adjaye J, Aldahmash A, et al. CD34 defines an osteoprogenitor cell population in mouse bone marrow stromal cells. Stem Cell Res. 2015;15:449–58. https://doi.org/10.1016/j.scr.2015.09.005.
Tjonnfjord GE, Veiby OP, Steen R, Egeland T. T lymphocyte differentiation in vitro from adult human prethymic CD34+ bone marrow cells. J Exp Med. 1993;177:1531–9. https://doi.org/10.1084/jem.177.6.1531.
Matayoshi A, Brown C, DiPersio JF, Haug J, Abu-Amer Y, Liapis H, et al. Human blood-mobilized hematopoietic precursors differentiate into osteoclasts in the absence of stromal cells. Proc Natl Acad Sci USA. 1996;93:10785–90. https://doi.org/10.1073/pnas.93.20.10785.
Peng Y, Kang H, Luo J, Zhang Y. A Comparative Analysis of Super-Enhancers and Broad H3K4me3 Domains in Pig, Human, and Mouse Tissues. Front Genet. 2021;12:701049. https://doi.org/10.3389/fgene.2021.701049.
Ansari-Lari MA, Oeltjen JC, Schwartz S, Zhang Z, Muzny DM, Lu J, et al. Comparative sequence analysis of a gene-rich cluster at human chromosome 12p13 and its syntenic region in mouse chromosome 6. Genome Res. 1998;8:29–40.
Hardison RC, Oeltjen J, Miller W. Long human-mouse sequence alignments reveal novel regulatory elements: a reason to sequence the mouse genome. Genome Res. 1997;7:959–66. https://doi.org/10.1101/gr.7.10.959.
Ungerback J, Hosokawa H, Wang X, Strid T, Williams BA, Sigvardsson M, et al. Pioneering, chromatin remodeling, and epigenetic constraint in early T-cell gene regulation by SPI1 (PU.1). Genome Res. 2018;28:1508–19. https://doi.org/10.1101/gr.231423.117.
Natoli G, Ghisletti S, Barozzi I. The genomic landscapes of inflammation. Genes Dev. 2011;25:101–6. https://doi.org/10.1101/gad.2018811.
Heinz S, Benner C, Spann N, Bertolino E, Lin YC, Laslo P, et al. Simple combinations of lineage-determining transcription factors prime cis-regulatory elements required for macrophage and B cell identities. Mol Cell. 2010;38:576–89. https://doi.org/10.1016/j.molcel.2010.05.004.
Izawa N, Kurotaki D, Nomura S, Fujita T, Omata Y, Yasui T, et al. Cooperation of PU.1 With IRF8 and NFATc1 Defines Chromatin Landscapes During RANKL-Induced Osteoclastogenesis. J Bone Min Res. 2019;34:1143–54. https://doi.org/10.1002/jbmr.3689.
Liang HC, Costanza M, Prutsch N, Zimmerman MW, Gurnhofer E, Montes-Mojarro IA, et al. Super-enhancer-based identification of a BATF3/IL-2R-module reveals vulnerabilities in anaplastic large cell lymphoma. Nat Commun. 2021;12:5577. https://doi.org/10.1038/s41467-021-25379-9.
Zhang QG, Qian J, Zhu YC. Targeting bromodomain-containing protein 4 (BRD4) benefits rheumatoid arthritis. Immunol Lett. 2015;166:103–8. https://doi.org/10.1016/j.imlet.2015.05.016.
Cabili MN, Trapnell C, Goff L, Koziol M, Tazon-Vega B, Regev A, et al. Integrative annotation of human large intergenic noncoding RNAs reveals global properties and specific subclasses. Genes Dev. 2011;25:1915–27. https://doi.org/10.1101/gad.17446611.
Derrien T, Johnson R, Bussotti G, Tanzer A, Djebali S, Tilgner H, et al. The GENCODE v7 catalog of human long noncoding RNAs: analysis of their gene structure, evolution, and expression. Genome Res. 2012;22:1775–89. https://doi.org/10.1101/gr.132159.111.
Liu W, Li Z, Cai Z, Xie Z, Li J, Li M, et al. LncRNA-mRNA expression profiles and functional networks in osteoclast differentiation. J Cell Mol Med. 2020;24:9786–9797. https://doi.org/10.1111/jcmm.15560.
Silva AM, Moura SR, Teixeira JH, Barbosa MA, Santos SG, Almeida MI. Long noncoding RNAs: a missing link in osteoporosis. Bone Res. 2019;7:10. https://doi.org/10.1038/s41413-019-0048-9.
Sakaguchi Y, Nishikawa K, Seno S, Matsuda H, Takayanagi H, Ishii M. Roles of Enhancer RNAs in RANKL-induced Osteoclast Differentiation Identified by Genome-wide Cap-analysis of Gene Expression using CRISPR/Cas9. Sci Rep. 2018;8:7504. https://doi.org/10.1038/s41598-018-25748-3.
Kim JH, Kim N. Regulation of NFATc1 in Osteoclast Differentiation. J Bone Metab. 2014;21:233–41. https://doi.org/10.11005/jbm.2014.21.4.233.
Wu Y, Zeng J, Roscoe BP, Liu P, Yao Q, Lazzarotto CR, et al. Highly efficient therapeutic gene editing of human hematopoietic stem cells. Nat Med. 2019;25:776–83. https://doi.org/10.1038/s41591-019-0401-y.
Gilbert LA, Larson MH, Morsut L, Liu Z, Brar GA, Torres SE, et al. CRISPR-mediated modular RNA-guided regulation of transcription in eukaryotes. Cell. 2013;154:442–51. https://doi.org/10.1016/j.cell.2013.06.044.
Smolen JS, Aletaha D, Barton A, Burmester GR, Emery P, Firestein GS, et al. Rheumatoid arthritis. Nat Rev Dis Prim. 2018;4:18001. https://doi.org/10.1038/nrdp.2018.1.
van der Heijde DM. Joint erosions and patients with early rheumatoid arthritis. Br J Rheumatol. 1995;34(Suppl 2):74–78.
Machold KP, Stamm TA, Nell VP, Pflugbeil S, Aletaha D, Steiner G, et al. Very recent onset rheumatoid arthritis: clinical and serological patient characteristics associated with radiographic progression over the first years of disease. Rheumatology. 2007;46:342–9. https://doi.org/10.1093/rheumatology/kel237.
Ejbjerg B, Narvestad E, Rostrup E, Szkudlarek M, Jacobsen S, Thomsen HS, et al. Magnetic resonance imaging of wrist and finger joints in healthy subjects occasionally shows changes resembling erosions and synovitis as seen in rheumatoid arthritis. Arthritis rheumatism. 2004;50:1097–106. https://doi.org/10.1002/art.20135.
Alippe Y, Mbalaviele G. Omnipresence of inflammasome activities in inflammatory bone diseases. Semin Immunopathol. 2019;41:607–18. https://doi.org/10.1007/s00281-019-00753-4.
Gravallese EM, Harada Y, Wang JT, Gorn AH, Thornhill TS, Goldring SR. Identification of cell types responsible for bone resorption in rheumatoid arthritis and juvenile rheumatoid arthritis. Am J Pathol. 1998;152:943–51.
Pettit AR, Ji H, von Stechow D, Muller R, Goldring SR, Choi Y, et al. TRANCE/RANKL knockout mice are protected from bone erosion in a serum transfer model of arthritis. Am J Pathol. 2001;159:1689–99. https://doi.org/10.1016/S0002-9440(10)63016-7.
Redlich K, Hayer S, Ricci R, David JP, Tohidast-Akrad M, Kollias G, et al. Osteoclasts are essential for TNF-alpha-mediated joint destruction. J Clin Investig. 2002;110:1419–27. https://doi.org/10.1172/JCI15582.
Acknowledgements
We thank Dr. Lionel Ivashkiv for providing human patient samples. This work was supported by National Research Foundation of Korea (NRF) grants funded by the Korean government (MSIP; No. 2020R1A2C1006101 and No. 2020M3A9B603885111 to SP) and by the Tow Foundation (to K-HP-M). Figure 1a was generated by BioRender.
Author information
Authors and Affiliations
Contributions
SB and KK designed and performed experiments and bioinformatics analysis, analyzed the data, and wrote the manuscript. KK performed the bioinformatics analysis and contributed his expertise. HK, ML, BO and KK performed experiments and analyzed data. HK, SM and JHC contributed their expertise. EYL, SHP and K-HP-M designed and supervised the study, and wrote the manuscript. K-HP-M conceptualized the study. All authors reviewed and provided input on the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Bae, S., Kim, K., Kang, K. et al. RANKL-responsive epigenetic mechanism reprograms macrophages into bone-resorbing osteoclasts. Cell Mol Immunol 20, 94–109 (2023). https://doi.org/10.1038/s41423-022-00959-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41423-022-00959-x
Keywords
This article is cited by
-
Histone demethylase KDM7A regulates bone homeostasis through balancing osteoblast and osteoclast differentiation
Cell Death & Disease (2024)
-
Integrative Analyses of Bulk and Single-Cell RNA Seq Identified the Shared Genes in Acute Respiratory Distress Syndrome and Rheumatoid Arthritis
Molecular Biotechnology (2024)
-
CircZNF367 promotes osteoclast differentiation and osteoporosis by interacting with FUS to maintain CRY2 mRNA stability
Journal of Orthopaedic Surgery and Research (2023)