Abstract
CD4+ T-cell-converted CD4−CD8− double negative (cDNT) have strong suppressive activity in the maintenance of immune tolerance, whereas IL-2 promotes cDNT proliferation and enhances cDNT resistance to apoptosis. However, the intrinsic mechanisms that regulate the survival of cDNT are still unknown. Here we demonstrate that the OX40 molecule was highly expressed on cDNT. The expression of OX40 was necessary to promote proliferation and inhibit apoptosis of cDNT in vivo and in vitro. OX40 promoted the survival of cDNT by regulating the expression of Bcl-2, Bcl-xL, Survivin, and BCL2L11. Canonical NF-κB cell signaling played an important role in the transmission of essential division and survival signals through OX40 in cDNT. IL-2 promoted the survival of cDNT in part via elevating the expression of the OX40 molecule. IL-2 promoted OX40 expression via downregulating the PPARα expression. In conclusion, we elucidated that OX40 is a key molecule that regulates cDNT proliferation and survival. IL-2 promoted OX40 expression by downregulating the PPARα binding to the OX40 promoter, leading to the elevated expression of Bcl-2, Bcl-xL, and Survivin in cDNT, which finally resulted in the promoted proliferation and decreased apoptosis of cDNT.
Similar content being viewed by others
Introduction
Regulatory CD4−CD8− double-negative T cells (DNT), which express αβ T-cell receptor (TCR) but do not express natural killer (NK) cell markers compose only a small population of T lymphocytes (1–5%) in the peripheral blood and lymphoid organs of rodents and humans1,2. DNT cells have strong suppressive activity toward CD4+ T cells and CD8+ T cells3,4,5,6, as well as B cells4,7, dendritic cells (DCs)8, and NK cells9, which are capable of suppressing the immune response and exert significant protection against allograft rejection, graft-versus-host disease, and autoimmune diseases3,6,10,11,12,13.
We have identified the differentiation pathway from CD4+ T cells to DNT, which are important for maintaining immune system homeostasis3,14. The DNT can be derived from activated and proliferated CD4+ T cells, which stimulated by bone marrow-derived DCs in vitro4. The over-activated CD4+ T cells can also be converted into DNT in vivo15. The CD4 T-cell-converted DNT (cDNT) are CD25+, CD44+, CD69+, and Foxp3−. These cDNT potently suppressed vigorous allo- and autoimmune responses, prolonged islet and skin allograft survival, and prevented and cured autoimmune type 1 diabetes with antigen-specificity3,6,16.
Interleukin (IL)-2 is a critical regulator of the activation and proliferation of T lymphocytes, also plays an important role in the generation and expansion of cDNT3. cDNT cells were in an anergic state, whereas exogenous IL-2 could restore cDNT responses, promote cDNT proliferation, and enhance cDNT resistance to Activation Induced Cell Death (AICD)17. However, the intrinsic mechanism that regulates the survival of cDNT and how IL-2 promotes cDNT proliferation and enhance cDNT resistance to AICD remain unknown.
OX40, often recognized as a costimulatory receptor for T cells, is predominantly expressed on activated CD4 T cells. It is essential for regulating the conventional CD4 and CD8 T-cell division, differentiation, and survival. Previous studies reported that the cytokines IL-1, IL-2, IL-4, and tumor necrosis factor stimulation could enhance or prolong OX40 expression15,18. OX40 is also found on Foxp3+ Tregs, but it is dispensable for the genesis and suppressor functions of naturally arising CD4+Foxp3+ Tregs19. However, the expression and function of OX40 in DNT are still unknown. In this study, we have identified OX40 as the key regulator of cDNT survival and the mediator of IL-2 on the promotion of proliferation and resistance to AICD of cDNT.
Results
OX40 molecule was highly expressed on cDNT and was necessary to promote proliferation and inhibit apoptosis of cDNT
As we reported3, after 7 days’ in vitro stimulation with mature DCs, approximately 30% of CD4 T cells lost CD4 expression and became DNT (Fig. 1a, left). By monitoring the apoptosis of activated CD4+ and cDNT, we found that the percentage of Annexin V+ cells was markedly lower in the cDNT than in activated CD4+ T cells (51.7 ± 5.7% vs. 8.1 ± 4.2%, P < 0.05, Fig. 1a, right). Meanwhile, OX40 expression was significantly higher in cDNT than that in activated CD4+ T cells (37.3 ± 5.91% vs. 18.9 ± 4.59%, P < 0.05; Fig. 1a, middle). Furthermore, cDNT and CD4+ T cells were sorted from mixed lymphocyte reaction (MLR) and were assessed for OX40 mRNA expression. As shown in Fig. 1b, the OX40 mRNA expression level of cDNT was also significantly higher than that of CD4+ T cells. No significant differences of CD27, CD28, CD30, CD40, CD95, and ICOS expression between CD4+ T cells and cDNT (supplementary Figure 1), indicating that OX40, the apoptosis-related gene of activated CD4+ and CD8+ T cells, may also play an important role on the survival of cDNT.
a CD4+CD25− T cells from C57BL/6 mice were stimulated with mature DBA/2 DCs for 7 days. The converted DNT and activated CD4+ T cells were detected for OX40 expression through flow cytometric analysis. Annexin V staining was used to detect apoptosis of the two cell populations. b The relative mRNA expression of OX40 was determined by real-time PCR in activated CD4+ T cells and cDNT. c Caspase 3/7 activation was determined in B6 cDNT or OX40 KO cDNT after being stimulated with anti-CD3/CD28 antibodies for 24, 48, and 72 h. d The converted C57BL/6 and OX40 KO DNT were incubated with anti-CD3/CD28 antibodies for 24, 48, and 72 h, and apoptosis was assessed via Annexin V staining. A representative flow cytometry image of Annexin V+ cells (% cDNT) from each group is shown (left). Statistical analysis of Annexin V+ cells in OX40 KO cDNT relative to B6 cDNT in each group was determined by flow cytometry (right). e The converted B6 and OX40 KO cDNT were incubated with anti-CD3/CD28 antibodies for 24, 48, and 72 h, and proliferation was assessed via EdU incorporation. Representative flow cytometry image of EdU+ cells (% cDNT) from each group is shown (left). In addition, statistical analysis was determined by flow cytometry (right). f The B6 cDNT and OX40 KO cDNT stimulated with anti-CD3/CD28 antibodies were incubated with Alamar Blue, and the absorbance at 570 nm at different time points was measured. g A total of 5 × 106 converted DNT or OX40 KO DNT were adoptively transferred into B6D2F1 (H-2b/d) recipient mice by tail vein injection. Three days after injection of BrdU (100 µg/day), splenocytes were isolated, and stained with fluorochrome-conjugated antibodies against mouse H2Dd and CD3, and the cDNT (H2Dd−CD3+) apoptosis and proliferation were determined by Annexin V and BrdU staining in vivo. Data are representative of three experiments with similar results. The data are depicted as the mean ± SD, n = 5 in each group. *p < 0.05
To further investigate the functional potential of OX40 on the converted DNT survival, OX40 knockout (KO) DNT converted from OX40 KO CD4+ T cells were stimulated with anti-CD3 and CD28 antibodies in vitro, and the apoptotic and proliferation rate was analyzed with Annexin V and EdU incorporation on 24, 48, and 72 h, respectively. Compared with B6 cDNT, caspase 3/7 activity in OX40 KO cDNT was increased (Fig. 1c), and the apoptotic rates of OX40 KO cDNT were significantly higher (Fig. 1d). In contrast, proliferation was decreased in OX40 KO cDNT determined by EdU incorporation (Fig. 1e). We also measured the proliferation of cDNT using an Alamar Blue cell viability reagent, and as shown in Fig. 1f, C57BL/6 (B6) cDNT had higher fluorescent, which indicated that cDNT had a higher proliferation rate than OX40 KO cDNT.
In addition, we also evaluated the regulation of OX40 on the proliferation and apoptosis of converted DNT in vivo. A total of 5 × 106 converted wild-type (WT) or OX40 KO DNT were adoptively transferred into B6D2F1 (H-2b/d) recipient mice by tail vein injection. After 3 days injection of BrdU (100 µg/day/mouse), splenocytes were isolated and stained with fluorochrome-conjugated antibodies against mouse H2Dd, the proliferation of cDNT (H2Dd-negative cells) was at a lower level when OX40 was deficient; however, the apoptosis of OX40-deficient cDNT was increased (Fig. 1g).
The collective data from in vitro and in vivo studies indicated that the expression of OX40 was necessary to promote proliferation and inhibit apoptosis of cDNT.
OX40 promoted the survival of cDNT by regulating the expression of Bcl-2, Bcl-xL, Survivin, and Bcl-2-like protein 11
OX40 engagement promotes CD4+ T-cell survival through the induction of the anti-apoptotic molecules, Bcl-2, Bcl-xL20, and cell cycle progression-related protein Survivin21. Meanwhile, it also greatly enhances CD8+ T-cell survival by upregulating Bcl-xL22. Ligation of OX40 on neutrophils results in enhanced survival, which correlates with reduced activation of caspase 3 and with augmented levels of anti-apoptotic markers23. To garner further insight into the molecular mechanism by which OX40 modulated cDNT survival, the apoptosis-related proteins Bcl-2, Bcl-xL, Survivin, and Bcl-2-like protein 11 (BCL2L11) were analyzed on converted WT DNT and OX40 KO DNT. cDNT were cultured up to 72 h with anti-CD3 and CD28 antibodies in vitro, the apoptosis of OX40 KO cDNT was increased, together with significant reduction of anti-apoptotic molecules, Bcl-2, Bcl-xL, and Survivin (Fig. 2a) when OX40 was knocked out. In addition, as shown in Fig. 2b, Bcl-2, Bcl-xL, and Survivin mRNA expression were dramatically reduced in OX40 KO cDNT, whereas BCL2L11 mRNA expression was augmented. These data indicated that OX40 could promote cDNT survival through the induction of apoptosis-related protein Bcl-2, Bcl-xL, and Survivin, and the suppression of pro-apoptotic protein BCL2L11.
a Flow cytometric analysis of Bcl-2, Bcl-xl, and Survivin protein expression in B6 cDNT and OX40 KO cDNT after anti-CD3/CD28 stimulation for 48 h. b Relative mRNA expression of anti-apoptosis genes (Bcl-2, Bcl-xl, and Survivin) and pro-apoptosis genes (Bcl2l11) in B6 cDNT and OX40 KO cDNT after incubation with CD3/CD28 for 48 and 72 h. c The relative mRNA levels of NF-κB signaling genes (nfkb1 and rela) in OX40 KO cDNT compared with WT cDNT. d Flow cytometric analysis of RelA, and phosphorylation of IκBα and IKKα/β protein expression in B6 cDNT and OX40 KO cDNT cells after anti-CD3/CD28 stimulation for 48 h. e Nuclear protein extracts were prepared from B6 cDNT cells and OX40 KO cDNT cells after anti-CD3/CD28 stimulation for 48 h. The RelA and p50 protein levels in the cells were analyzed by western blot. The relative density of the RelA and p50 band was normalized to Histone H3. The data are presented as the mean ± SD, n = 5 in each group. *p < 0.05. NS no significance
Canonical nuclear factor (NF)-κB cell signaling plays an important role in the transmission of essential division and survival signals through OX40 in T cells24,25. Therefore, we examined the NF-κB1 and RelA mRNA expression of cDNT after 48 and 72 h cultures in vitro. The mRNA expression of NF-κB1 and RelA of cDNT were significantly reduced when OX40 was deficient (Fig. 2c). We also detected NF-κB signaling pathway through flow cytometry and western blotting at protein level. As shown in Fig. 2d, OX40 deficiency could downregulate phosphorylation events of IKKα/β, IκBα, and RelA (p65) expression of cDNT. Meanwhile, western blotting results also showed OX40 KO cDNT decreased p50 and RelA expression in the nucleus (Fig. 2e), suggesting that canonical NF-κB signaling was also important for transmission of proliferation and survival signals through OX40 in cDNT.
IL-2 promoted the survival of cDNT in part via elevating the expression of OX40 molecule
IL-2 is critical for the activation and proliferation of T cells, plays an important role in the generation and expansion of cDNT. In this study, we found that IL-2 could remarkably promote the expression of OX40 in cDNT (Fig. 3a, b), however, CD27, CD28, CD30, CD40, CD95, and ICOS were not influenced by IL-2 (supplementary Figure 2). Therefore, we tested whether the regulation of IL-2 on cDNT proliferation and apoptosis was OX40-dependent. Accordingly, converted WT DNT and OX40 KO DNT were stimulated with anti-CD3 and CD28 antibodies in vitro with or without rIL-2. With exogenous IL-2, the apoptosis rates of cDNT from WT B6 mice and OX40 KO mice were both decreased (Fig. 3c, d); however, the reduction of apoptosis in converted WT B6 cDNT was markedly greater than that in OX40 KO cDNT (Fig. 3e). IL-2 could inhibit the activity of caspase 3/7 in cDNT; however, the reduction of caspase 3/7 activity of cDNT with rIL-2 stimulation in vitro was impaired when OX40 was deficient (Fig. 3f, g). Similarly, the proliferation of cDNT was significantly augmented in the presence of rIL-2 stimulation (Fig. 3h, i). Nevertheless, the proliferation enhancements of cDNT with rIL-2 stimulation in vitro were reduced when OX40 was knocked out (Fig. 3j). The Alamar Blue cell proliferation assay further supported that OX40 was involved in the regulation of IL-2 on the survival of cDNT (Fig. 3k).
a Statistical analysis of OX40 expression on cDNT with or without IL-2 for 24, 48, and 72 h based on flow cytometric analysis. b Relative changes in OX40 expression induced by IL-2 in cDNT were plotted as fold changes of B6 cDNT without IL-2 stimulation. c B6 cDNT and OX40 KO cDNT were stimulated with or without IL-2 for 24, 48, and 72 h, and apoptosis of the cells was detected through Annexin V staining. Representative flow cytometric image of Annexin V+ cDNT from each group. d Statistical analysis of Annexin V+ cells in each group at a different time point. e Relative changes of Annexin V+ cells with or without IL-2 in B6 cDNT were compared with that in OX40 KO cDNT at 24, 48, and 72 h. f Caspase 3/7 activation was determined in B6 cDNT and OX40 KO cDNT after stimulation with or without IL-2. g The relative changes of Caspase 3/7 activation with or without IL-2 in B6 cDNT were compared with the ratio in OX40 KO cDNT at 24, 48, and 72 h. h The percentages of EdU+ cells relative to the total numbers of B6 cDNT or OX40 KO cDNT with or without IL-2 was determined by flow cytometry in the indicated groups. i Statistical analysis of EdU+ cells in each group at different time points. j Relative changes of EdU+ cells with or without IL-2 in B6 cDNT were compared with that in OX40 KO cDNT at 24, 48, and 72 h. k The B6 cDNT and OX40 KO cDNT were stimulated with IL-2 or without IL-2, and Alamar Blue was incubated during the stimulation. The proliferations of the cells were detected at the absorbance of 570 nm at different time points. #P < 0.05, IL-2 + B6 cDNT versus B6 cDNT; *P < 0.05, IL-2 + B6 cDNT versus IL-2 + OX40 KO cDNT. l A total of 5 × 106 B6 cDNT or OX40 KO cDNT were adoptively transferred into B6D2F1 recipient mice by tail vein injection in the presence or absence of IL-2/Fc protein. After 3 days, cDNT were analyzed by flow cytometry for proliferation and apoptosis with BrdU and Annexin V detection. Data are representative of three experiments with similar results. The data are presented as the mean ± SD, n = 5 in each group. *p < 0.05, **p < 0.01, NS no significance
Additionally, B6D2F1 mice underwent adoptive transfer with 5 × 106 B6 cDNT or OX40 KO cDNT in the presence or absence of IL-2/Fc. Three days after injection of BrdU, cDNT were analyzed by flow cytometry for proliferation and apoptosis with BrdU and Annexin V detection. As shown in Fig. 3l, the effect of OX40 on IL-2-regulating cDNT survival in vivo was comparable to those in vitro.
We also noticed that rIL-2 upregulated anti-apoptotic molecules, Bcl-2 (Fig. 4a), Bcl-xl (Fig. 4b), and Survivin (Fig. 4c) expression and downregulated pro-apoptotic gene Bcl2l11 expression (Fig. 4d) of cDNT. However, the regulation of IL-2 on these apoptotic-related genes was impaired in OX40-deficient cDNT (Fig. 4a–d). These data suggested that IL-2 promoted the survival of cDNT at least in part via the elevation of OX40 molecule expression.
a Relative mRNA expression of anti-apoptosis genes Bcl-2 (a), Bcl-xl (b), and Survivin (c), and pro-apoptosis genes Bcl2l11 (d) in B6 cDNT and OX40 KO cDNT stimulated with IL-2 or without IL-2 at different time points. Relative changes of the genes in the presence or absence of IL-2 in B6 cDNT compared with that in OX40 KO cDNT. The data are presented as the mean ± SD, n = 5 in each group. *p < 0.05, **p < 0.01, NS no significance
IL-2 promoted OX40 expression by downregulating the PPARα expression
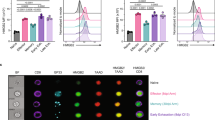
To investigate the intrinsic mechanism of IL-2 regulation on OX40 molecular expression in cDNT, the upstream factors regulating OX40 were investigated. In the OX40 promoter region (−1032/+28 region), potential transcription factor (TF)-binding sites are presented in Fig. 5a and were based on bioinformatic prediction. To further identify the TFs that bind to the OX40 core promoter region and regulate the activation of the OX40 gene, a competitive promoter-binding TF profiling array for the OX40 core promoter in cDNT was performed. Among the potential TF-binding sites, PPAR has relative higher changes of chemiluminescence activity between the absence (control) of OX40 core promoter vs. presence (control + promoter) of the promoter within the OX40 promoter (Fig. 5b, c). Furthermore, PPARα and PPARγ mRNA expression was markedly decreased in the cDNT under IL-2 stimulation (Fig. 5d).
a Nucleotide sequence of the OX40 promoter region. Potential regulatory elements identified according to the Transcription Factor Binding Sites database TRANSFAC are shown underlined and identified by the appropriate symbols. b Promoter-binding transcription factor (TF) profiling array assay of mice OX40 core promoter was performed. This is a competitive binding assay performed to identify promoter-bound TFs through comparisons of the results in the presence (with promoter) or absence (without promoter) of the mouse OX40 core promoter. If the OX40 promoter contains a TF-binding sequence, it will display a lower chemiluminescence activity. c Relative change of chemiluminescence activity in the absence (control) of the OX40 core promoter with presence (control + promoter) of the promoter. d Relative mRNA levels of the transcription factors in the presence or absence of IL-2. The data are presented as the mean ± SD, n = 3 in each group. *p < 0.05, **p < 0.01, NS no significance. e ChIP analysis of cDNT stimulated with IL-2 (50 ng/ml) for 48 h. Conventional PCR was performed to measure the relative levels of the antibody-bound DNA fragments. Soluble chromatin from the cDNT was immunoprecipitated with the PPARα, PPARγ antibody, or incubated with normal rabbit serum (IgG) for control purposes. The amplification for soluble chromatin before immunoprecipitation are shown as input. f Real-time PCR was used to determine the levels of PPARα and PPARγ bound directly to OX40 promoter sequence (−945/−736 bp and −1017/−950 bp upstream from transcription start site). The data are presented as the mean ± SD, n = 5 in each group. *p < 0.05, NS no significance
Then we performed ChIP assays with the OX40 promoter to test whether PPARα or PPARγ was associated with the OX40 gene upregulation of cDNT in the presence of IL-2. As shown in Fig. 5e, after immunoprecipitation with PPARα antibodies, a positive band of approximately −945/−736 bp was yielded in the bound DNA of cDNT without IL-2 stimulation, however, lower amplification of bound DNA from cDNT with IL-2 stimulation was shown. Precipitation with PPARα or without antibody did not show significant changes of positive DNA band (approximately −435/−139 bp). Precipitation with PPARγ antibody or without antibody did not show significant changes of positive DNA band between cDNT treated with or without IL-2, which strongly suggested that PPARα is able to bind to the OX40 promoter and is involved in regulation of OX40 expression by IL-2. Real-time PCR further proved that PPARα direct binding to OX40 promoter sequence (−945/−736 bp) was reduced in cDNT treated with IL-2 compared to cDNT without IL-2 stimulation.
To ascertain the possible involvement of PPARα activity in regulation of IL-2 on OX40 molecule, the cultures were performed in the presence or absence of the PPARα agonist and rIL-2. As an aforementioned result, OX40 expression and proliferation of cDNT were significantly augmented in the presence of rIL-2 stimulation; however, the upregulation of OX40 expression induced by IL-2 was abrogated by a PPARα agonist dose dependently (Fig. 6a, b). In addition, the effect of rIL-2 on the upregulation of anti-apoptotic molecules, Bcl-2, Bcl-xl, and Survivin, or the downregulation of the pro-apoptotic gene Bcl2l11 were all impaired in the presence of a PPARα agonist (Fig. 6c). Unquestionably, PPARα agonist neutralized the anti-apoptotic effect of IL-2 on cDNT, the percent of apoptotic rate was increased in the presence of a PPARα agonist (Fig. 6d). In contrast, the proliferation rates of cDNT with rIL-2 stimulation in vitro were reduced in the presence of a PPARα agonist, and the changes were dose-dependent (Fig. 6e).
a Inhibition of OX40 mRNA levels after incubation with or without IL-2 for 48 h by a PPARα agonist (80 µM). b The percentage of OX40+ cDNT was detected after stimulation with a PPARα agonist in the presence or absence of IL-2. Statistical analysis of OX40+ cells proportion stimulation with IL-2 relative to the proportion without IL-2 in each group, as determined by flow cytometry. c Relative mRNA levels of anti-apoptosis genes (Bcl-2, Bcl-xl, and Survivin) and pro-apoptosis genes (Bcl2l11) of cDNT after incubation with a PPARα agonist with or without IL-2. Statistical analysis of the genes expression stimulation with IL-2 relative to the genes without IL-2 in each group was determined. d Apoptosis of cDNT (Annexin V+) was detected after stimulation with a PPARα agonist with or without IL-2 by flow cytometry. e The proliferation of cDNT (EdU+) was detected after stimulation with a PPARα agonist with or without IL-2 by flow cytometry. The data are presented as the mean ± SD, n = 5 in each group. *p < 0.05, **p < 0.01, NS no significance
Taken together, these results suggested that IL-2 promoted OX40 expression by downregulating the PPARα expression, leading to the elevated expression of Bcl-2, Bcl-xL, and Survivin in cDNT, which finally resulted in promoted proliferation and decreased apoptosis.
Discussion
OX40 is induced primarily during T-cell activation and plays an important role in the survival and proliferation of T cells26,27. OX40 is mainly expressed on activated T cells and is preferentially expressed on CD4+ T cells, although activated CD8+ T cells also express OX40, albeit at lower levels24. OX40 is also highly expressed on both natural and induced Foxp3+ Tregs; however, in contrast to its costimulatory role to T effector cells, OX40 is a rather potent negative regulator of Foxp3+ Tregs25,28. OX40 costimulation did not influenced the survival of the Foxp3+ Tregs significantly, but markedly inhibited Foxp3 gene expression25.
In this study, we have demonstrated for the first time that OX40 is highly expressed on cDNT; moreover, similar to its costimulatory role to activated T effector cells, unlike Foxp3+ Tregs, OX40 is also a potent regulator on cDNT proliferation and survival. OX40-deficient cDNT had a higher apoptotic rate and lower proliferation rate than WT cDNT. OX40 participated into cDNT survival regulation by inducting the expression of apoptotic-related proteins Bcl-2, Bcl-xL, and Survivin, thus suppressing the expression of pro-apoptotic gene BCL2L11.
OX40 signaling can target the canonical NF-κB (NF-κB1) pathway in peripheral antigen-responding CD4 T cells24,25. In this study, we also identified significantly lower phosphorylation events of IKKα/β, IκBα, RelA (p65) expression, and p50, RelA nuclear import in OX40-deficient cDNT accompanied by the changes of Bcl-2 and Bcl-xL indicating that OX40 might promote the survival of cDNT by regulating the expression of Bcl-2 and Bcl-xL via NF-κB cell signaling. OX40 signals also controls Survivin expression of cDNT. Survivin, a member of the inhibitor of apoptosis family, was found to bind the active forms of the executioner proteases caspase 3 and 7, but not the upstream initiator caspase 8, and this inhibited apoptosis induced by overexpression of procaspase 3 and 7. Moreover, cotransfection of Survivin prevented spontaneous processing of caspase 7 and caspase 3 to their active forms29. In CD4+ T cells, blocking Survivin suppressed S-phase transition and division of T cells and led to apoptosis21. Converted DNT highly that expressed Survivin may also have contributed to cDNT proliferation and anti-apoptosis.
Research over the past decade has definitively shown the importance of OX40–OX40L interactions in development of immune-mediated disease24, based on that the OX40–OX40L checkpoint inhibition may have potential clinical application in the treatment in autoimmune diseases. However, because anti-OX40/OX40L has complicated effects on different cell types, the use of OX40–OX40L checkpoint inhibition should be cautious, especially in the combination with cDNT-based cell therapy.
IL-2 plays an unequivocal role in priming activated T cells to undergo apoptotic cell death, which serves as a critical feedback regulator of clonal expansion30; however, accumulating evidence suggests that IL-2 is essential for the activation and suppressive function of Foxp3+ Tregs31,32,33 and is sufficient to induce proliferation of Foxp3+ Tregs. Converted DNT were hypo-responsive when stimulated by mature DCs, and IL-2 promoted the expression of OX40 in cDNT. Meanwhile, IL-2 completely restored their responsiveness, and enhanced cDNT proliferation. In addition, IL-2 increased the resistance of cDNT to apoptosis. However, the regulation of IL-2 on cDNT proliferation and apoptosis was impaired when OX40 in cDNT was knocked out. Furthermore, the mRNA expression of Bcl-2, Bcl-xL, and Survivin was reduced in OX40-deficient cDNT, even in the presence of IL-2, whereas mRNA expression of BCL2L11 was augmented. These data suggested that IL-2 promoted the survival of cDNT in part via elevation of the expression of the OX40 molecule.
The regulation of IL-2 on OX40 upregulation of cDNT is unknown. In this study, we provide evidence that this regulation is PPARα-dependent. Promoter-binding TF profiling arrays revealed that a possible presence of binding site for PPARα and PPARγ within the OX40 promoter. The ChIP assay further supported that PPARα but not PPARγ is able to bind to the OX40 promoter and involves in the negative regulation of OX40 expression in cDNT. Furthermore, OX40 expression of cDNT were significantly augmented in the presence of rIL-2 stimulation. In contrast, the OX40 expression of cDNT with rIL-2 stimulation in vitro was reduced when a PPARα agonist was presented.
The PPARs are members of the nuclear-hormone-receptor superfamily; they transduce a wide variety of signals, including environmental, nutritional, and inflammatory events. Genetic ablation of PPARα or PPARγ on CD4 T cells results in higher production of interferon γ and IL-2 through PPAR-mediated transrepression activities34. In this study, we found that the administration of IL-2 effectively promoted OX40 expression in cDNT through a PPARα-dependent process and consequently enhanced Bcl-2, Bcl-xL, and Survivin expression, and finally enhanced survival of cDNT. However, how IL-2 affects PPARα activities needs to be further studied.
In conclusion, we elucidated that OX40 is a key molecule that controls CD4 T-cell-converted DNT proliferation and apoptosis by upregulation of Survivin, Bcl-2, and Bcl-xL, and downregulation of pro-apoptotic gene BCL2L11. IL-2 promotes cDNT proliferation and resistance to apoptosis in part by upregulation of OX40. This regulation of IL-2 on OX40 expression in cDNT is controlled by PPARα. These Snew findings may have important implications in cDNT-based cell therapy for the future.
Materials and Methods
Mice
Male C57BL/6 (H-2b) mice, C57BL/6 OX40 KO (H-2b) mice, DBA/2 (H-2d) mice, and B6D2F1 (H-2b/d) mice were obtained from the Jackson Laboratory (Bar Harbor, ME, USA). The mice were maintained in a pathogen-free, temperature-controlled environment under a 12-h light/dark cycle at the Beijing Friendship Hospital, and all animal protocols were approved by the Institutional Animal Care and Ethics Committee.
Antibodies and reagents
Recombinant mouse IL-2 (rmIL-2) and granulocyte-macrophage colony-stimulating factor were purchased from PeproTech (Rocky Hill, NJ, USA). Mouse IL-2/Fc fusion protein (a long-lasting form of IL-2) was obtained from Jiangsu Futai Biotechnology (Jiangsu, China). Fluorochrome-conjugated antibodies against mouse CD3, CD4, CD8, NK1.1, TCRγδ, CD86, OX40, Bcl-2, H2Dd, isotype controls, and BrdU staining kits were obtained from eBioscience (San Diego, CA, USA). Anti-mouse PE-Bcl-xL and Survivin were obtained from CST (Boston, MA, USA). Anti-mouse p105/p50, p65, and IKB alpha (phosphor S36) were obtained from Abcam (Cambridge, MA, USA), while anti-mouse phosphor-IKKα/β (Ser176/180) and Histone H3 were obtained from CST. Purified anti-CD3, CD28 antibodies, and Annexin V-PE antibodies were purchased from BD Pharmingen (San Diego, CA, USA). Paraformaldehyde, saponin, Triton X-100, and PPARα agonist (WY-14643) were obtained from Sigma (St. Louis, MO, USA). A mouse T-cell enrichment column was purchased from R&D Systems (Minneapolis, MN). Anti-PE microbeads, and magnetic bead separation columns were obtained from Miltenyi Biotec (Auburn, CA). The ChIP assay kit was from Millipore (Bedford, MA, USA).
Conversion of DNT in vitro
The generation of CD4 T cells converted to DNT was described previously3. Briefly, CD4+CD25− T cells were isolated from spleens and lymph nodes of C57BL/6 mice or C57BL/6 OX40 KO mice. The purified CD4+CD25− T cells were then cultured with DBA/2 mature DCs and rmIL-2 (50 ng/ml) for 7 days. Converted DNT were sorted from culture through a fluorescence-activated cell sorter (FACS Aria II; BD Biosciences, San Diego, CA, USA).
Re-stimulation of cDNT in vitro
Converted DNT and OX40 KO DNT (2 × 105/well) were re-stimulated with 5 μg/ml anti-CD3 and 2 μg/ml anti-CD28 with or without rmIL-2 (50 ng/ml) in a 96-well flat-bottom culture plates for 3 days. EdU (RiboBio, Guangzhou, China) was added to the plates 12 h before harvest (final concentrations were 50 μM). Cell proliferation was measured via EdU incorporation according to the manufacturer’s instructions (EdU staining kit, RiboBio Corporation, Guangzhou, China).
Re-stimulation of cDNT in vivo
In all, 5 × 106 converted DNT or OX40 KO DNT were adoptively transferred into B6D2F1 recipient mice by tail vein injection. IL-2/Fc (1 µg/day) and BrdU (100 µg/day) were administered by intraperitoneal injection. Splenocytes were isolated on day 3, cDNT proliferation was measured via BrdU incorporation according to the manufacturer’s instructions (eBioscience).
Alamar Blue assay
Converted DNT and OX40 KO DNT (2 × 105/well) were re-stimulated with 5 μg/ml anti-CD3 and 2 μg/ml anti-CD28 with or without rmIL-2 (50 ng/ml) in 96-well flat-bottom culture plates for 5 days. A 1/10th volume of Alamar Blue® reagent was added directly to cells in culture medium, and they were incubated at 37 °C in a cell culture incubator, protected from direct light. The absorbance of Alamar Blue® at 570 nm was measured using 600 nm as a reference wavelength (normalized to the 600 nm value) at different time points.
Caspase 3/7 activation
Caspase 3/7 activities were measured using the Caspase-Glo 3/7 Assay (Promega, USA). Briefly, the converted DNT and OX40 KO DNT (2 × 105/well) were re-stimulated with 5 μg/ml anti-CD3 and 2 μg/ml anti-CD28 with or without rmIL-2 (50 ng/ml) in 96-well flat-bottom culture plates for 24, 48, and 72 h. The caspase 3/7 reagent was then added to each well at a different time point, and the plate was incubated on a rotary shaker for 30 min at room temperature. Luminescence was recorded for each well. The caspase 3/7 activity is presented as the mean of the results from the three experiments.
Quantitative real-time PCR
Total RNA was extracted from cells using an RNeasy mini-kit (Qiagen, Valencia, CA, USA) and reverse transcribed into cDNA with the SuperScript III RT-kit (Invitrogen, Carlsbad, CA, USA). Real-time quantitative polymerase chain reaction was performed with the Power SYBR Green master mix (Applied Biosystems, Foster City, CA, USA) and gene amplification was performed on the ABI 7500 Sequence Detection System (Applied Biosystems). Gene-specific primers used for specific genes and GAPDH are shown in Supplementary Table 1. The relative gene expression was quantitatively analyzed by the comparative Ct method (2−ΔΔCT). Data were normalized to the levels of GAPDH mRNA.
Western blot
Nuclear protein extracts from B6 cDNT and OX40 KO cDNT were prepared with NE-PER® Nuclear and Cytoplasmic Extraction reagents (Thermo Fisher Scientific, Inc., Pittsburgh, PA, USA). After determination of concentration, the samples containing 20 μg protein were separated by 12% sodium dodecyl sulfate-polyacrylamide gel electrophoresis and transferred to a polyvinylidene difluoride membrane (Millipore). Primary antibodies against p50/p105 (diluted 1:2000), p65 (RelA, diluted 1:2000), and Histone H3 (diluted 1:5000) were used. The membranes were incubated with secondary antibodies conjugated to horseradish peroxidase (HRP), and the proteins were detected by enhanced chemiluminescence (Thermo). The relative density of the protein bands was quantitatively determined using ImageJ software (National Institutes of Health, Bethesda, MD, USA).
Promoter-binding TF profiling array assay
To examine the potential TFs that bind to the OX40 core promoter region (−1032/+28 region) in cDNT, TF activation profiling plate array kits were used (Signosis, CA, USA). The assay was performed according to the kit’s instructions. First, 15 μl TF-binding buffer, 3 μl TF probe, 10 μg cDNT nuclear extract, and 5 μl OX40 promoter PCR fragment were mixed in a tube, and incubated at 20–23 °C for 30 min to form TF/DNA complex. Separation of TF/DNA complex from free probes. Then eluted the bound probe from the complex, and incubated the probe with hybridization plate overnight at 42 °C. After washing with hybridization wash buffer, streptavidin-HRP conjugate were added to each well, which contained the bound probe, and incubated for 45 min gently shaking at room temperature. Finally, incubated with substrate solution for 1 min and detected the probe relative light units on a microplate luminometer (Wallac 1450, Wallac, MA, USA).
Chromatin immunoprecipitation assay
The chromatin immunoprecipitation (ChIP) assay was performed according to the kit’s instructions (Millipore). After treatment with mouse IL-2 (50 ng/ml) for 48 h, the cDNT were fixed, sonicated, and collected for ChIP assay. DNA fragments were immunoprecipitated with antibodies specific to PPARα, PPARγ, or control rabbit IgG at 4 °C overnight. Subsequently, the DNA fragments were de-crosslinked, purified from the complexes, and ethanol-precipitated. The immunoprecipitated chromatin was amplified by primers (Supplementary Table 1) corresponding to specific regions of the OX40 genomic locus. Meanwhile, the immunoprecipitated DNA fragments were detected by quantitative real-time. To calculate the fold enrichment of the precipitated PPAR element, each sample was normalized to the corresponding input. All ChIP assays were performed in triplicate.
Flow cytometric analysis
All samples were acquired on a FACS Aria II flow cytometer (BD Biosciences), and the data were analyzed using FlowJo software (TreeStar, Ashland, OR, USA).
Statistical analysis
Statistical analysis was performed using the Prism 5.0 software (GraphPad Software, San Diego, CA, USA). The values are expressed as the mean ± SD. Analyses for significant differences were performed using Student’s t test and one-way analysis of variance. p Values < 0.05 were considered significant.
References
Juvet, S. C. & Zhang, L. Double negative regulatory T cells in transplantation and autoimmunity: recent progress and future directions. J. Mol. Cell Biol. 4, 48–58 (2012).
Hillhouse, E. E. & Lesage, S. A comprehensive review of the phenotype and function of antigen-specific immunoregulatory double negative T cells. J. Autoimmun. 40, 58–65 (2013).
Zhang, D. et al. New differentiation pathway for double-negative regulatory T cells that regulates the magnitude of immune responses. Blood 109, 4071–4079 (2007).
Zhang, Z. X. et al. Double-negative T cells, activated by xenoantigen, lyse autologous B and T cells using a perforin/granzyme-dependent, Fas-Fas ligand-independent pathway. J. Immunol. 177, 6920–6929 (2006).
Chen, W., Diao, J., Stepkowski, S. M. & Zhang, L. Both infiltrating regulatory T cells and insufficient antigen presentation are involved in long-term cardiac xenograft survival. J. Immunol. 179, 1542–1548 (2007).
Zhang, D. et al. Adoptive cell therapy using antigen-specific CD4−CD8− T regulatory cells to prevent autoimmune diabetes and promote islet allograft survival in NOD mice. Diabetologia 54, 2082–2092 (2011).
Li, W. et al. Ex vivo converted double negative T cells suppress activated B cells. Int. Immunopharmacol. 20, 164–169 (2014).
Gao, J. F. et al. Regulation of antigen-expressing dendritic cells by double negative regulatory T cells. Eur. J. Immunol. 41, 2699–2708 (2011).
He, K. M. et al. Donor double-negative Treg promote allogeneic mixed chimerism and tolerance. Eur. J. Immunol. 37, 3455–3466 (2007).
Zhang, Z. X., Yang, L., Young, K. J., DuTemple, B. & Zhang, L. Identification of a previously unknown antigen-specific regulatory T cell and its mechanism of suppression. Nat. Med. 6, 782–789 (2000).
Young, K. J., DuTemple, B., Phillips, M. J. & Zhang, L. Inhibition of graft-versus-host disease by double-negative regulatory T cells. J. Immunol. 171, 134–141 (2003).
McIver, Z. et al. Double-negative regulatory T cells induce allotolerance when expanded after allogeneic haematopoietic stem cell transplantation. Br. J. Haematol. 141, 170–178 (2008).
Ford, M. S. et al. Peptide-activated double-negative T cells can prevent autoimmune type-1 diabetes development. Eur. J. Immunol. 37, 2234–2241 (2007).
Zhao, X. et al. A novel differentiation pathway from CD4+T cells to CD4- T cells for maintaining immune system homeostasis. Cell Death Dis. 7, e2193 (2016).
Toennies, H. M., Green, J. M. & Arch, R. H. Expression of CD30 and Ox40 on T lymphocyte subsets is controlled by distinct regulatory mechanisms. J. Leukoc. Biol. 75, 350–357 (2004).
Liu, T. et al. Combination of double negative T cells and anti-thymocyte serum reverses type 1 diabetes in NOD mice. J. Transl. Med. 14, 57 (2016).
Cong, M. et al. Interleukin-2 enhances the regulatory functions of CD4(+)T cell-derived CD4(-)CD8(-) double negative T cells. J. Interferon Cytokine Res. 36, 499–505 (2016).
Redmond, W. L., Triplett, T., Floyd, K. & Weinberg, A. D. Dual anti-OX40/IL-2 therapy augments tumor immunotherapy via IL-2R-mediated regulation of OX40 expression. PLoS ONE 7, e34467 (2012).
Vu, M. D. et al. OX40 costimulation turns off Foxp3(+) tregs. Blood 110, 2501–2510 (2007).
Rogers, P. R., Song, J., Gramaglia, I., Killeen, N. & Croft, M. OX40 promotes Bcl-xL and Bcl-2 expression and is essential for long-term survival of CD4 T cells. Immunity 15, 445–455 (2001).
Song, J., So, T., Cheng, M., Tang, X. & Croft, M. Sustained survivin expression from OX40 costimulatory signals drives T cell clonal expansion. Immunity 22, 621–631 (2005).
Bansal-Pakala, P., Halteman, B. S., Cheng, M. H. & Croft, M. Costimulation of CD8 T cell responses by OX40. J. Immunol. 172, 4821–4825 (2004).
Baumann, R. et al. Functional expression of CD134 by neutrophils. Eur. J. Immunol. 34, 2268–2275 (2004).
Croft, M. Control of immunity by the TNFR-related molecule OX40 (CD134). Annu. Rev. Immunol. 28, 57–78 (2010).
Song, J., So, T. & Croft, M. Activation of NF-kappaB1 by OX40 contributes to antigen-driven T cell expansion and survival. J. Immunol. 180, 7240–7248 (2008).
Calderhead, D. M. et al. Cloning of mouse Ox40: a T cell activation marker that may mediate T-B cell interactions. J. Immunol. 151, 5261–5271 (1993).
Sugamura, K., Ishii, N. & Weinberg, A. D. Therapeutic targeting of the effector T-cell co-stimulatory molecule OX40. Nat. Rev. Immunol. 4, 420–431 (2004).
Valzasina, B. et al. Triggering of OX40 (CD134) on CD4(+)CD25+T cells blocks their inhibitory activity: a novel regulatory role for OX40 and its comparison with GITR. Blood 105, 2845–2851 (2005).
Tamm, I. et al. IAP-family protein survivin inhibits caspase activity and apoptosis induced by Fas (CD95), Bax, caspases, and anticancer drugs. Cancer Res. 58, 5315–5320 (1998).
Lenardo, K. M. Interleukin-2 programs mouse ab T lymphocytes for apoptosis. Nature 353, 858–861 (1991).
de la Rosa, M., Rutz, S., Dorninger, H. & Scheffold, A. Interleukin-2 is essential for CD4 + CD25 + regulatory T cell function. Eur. J. Immunol. 34, 2480–2488 (2004).
Kang, H. G. et al. Effects of cyclosporine on transplant tolerance: the role of IL-2. Am. J. Transplant. 7, 1907–1916 (2007).
Mahmud, S. A., Manlove, L. S. & Farrar, M. A. Interleukin-2 and STAT5 in regulatory T cell development and function. JAKSTAT 2, e23154 (2013).
Daynes, R. A. & Jones, D. C. Emerging roles of PPARs in inflammation and immunity. Nat. Rev. Immunol. 2, 748–759 (2002).
Acknowledgements
This work was supported by grants from the National Natural Science Foundation of China (No. 81570510, 81500598, and 81501379), the Natural Science Foundation of Beijing Municipality (No. 7172060), and Open project from Beijing Key Laboratory of Translational Medicine in Liver Cirrhosis.
Author information
Authors and Affiliations
Contributions
All listed authors participated meaningfully in the study and that they have seen and approved the submission of this manuscript. G.S., X.S., and W.L. participated in performing the research, analyzing the data, and initiating the original draft of the article. K.L., D.T., Y.D., and X.S. participated in performing the research and collecting the data. D.Z. and H.X. established the hypotheses, supervised the studies, analyzed the data, and co-wrote the manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Edited by M. Herold
Electronic supplementary material
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Sun, G., Sun, X., Li, W. et al. Critical role of OX40 in the expansion and survival of CD4 T-cell-derived double-negative T cells. Cell Death Dis 9, 616 (2018). https://doi.org/10.1038/s41419-018-0659-x
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41419-018-0659-x
This article is cited by
-
OX40/OX40 ligand and its role in precision immune oncology
Cancer and Metastasis Reviews (2024)
-
IL-33 promotes double negative T cell survival via the NF-κB pathway
Cell Death & Disease (2023)