Abstract
Background
Studies on association between low-dose aspirin use and ovarian cancer risk were mostly based on self-reported medication use and few had large enough sample size to investigate the potential modification effect by ovarian cancer risk factors.
Methods
In these two nationwide nested case-control studies among the Danish and Swedish female population, 11,874 women with ovarian cancer (30–84 years old) (Denmark: 7328 diagnosed in 2000–2019, Sweden: 4546 diagnosed in 2010–2018) were randomly age- matched with 473,960 female controls (293,120 from Denmark, and 181,840 from Sweden). We used conditional logistic regression to estimate odds ratios (OR) and 95% confidence intervals (CI) and combined the estimates based the fixed-effect assumption. Effect modification by inflammation-related risk factors and by indication (cardiovascular disease, CVD) were also investigated.
Results
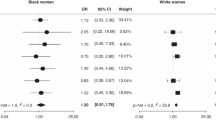
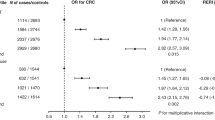
Ever use of low-dose aspirin was not strongly associated with the overall risk of ovarian cancer (OR = 0.97; 95%CI: 0.92–1.03). However, the association differed according to parity (nulliparous: OR = 0.80, 95%CI: 0.70–0.92; parous: OR = 1.00, 95%CI: 0.94–1.07; p-interaction = 0.0024), and according to history of CVD (no CVD: OR = 0.91, 95%CI: 0.82–1.00; ever CVD: OR = 1.05, 95%CI: 0.97–1.13; p-interaction =0.0204).
Conclusions
Low-dose aspirin use was associated with a decreased ovarian cancer risk especially in nulliparous women and in women without CVD diagnosis.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 24 print issues and online access
$259.00 per year
only $10.79 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
Data availability
The Danish data is based on pseudonymized registry data located on a secure platform at Statistics Denmark, which can be accessed given the relevant data permissions. The Swedish data is located on an encrypted server at Karolinska Institutet and is available from the study authors given all relevant data permissions.
References
Cabasag CJ, Fagan PJ, Ferlay J, Vignat J, Laversanne M, Liu L, et al. Ovarian cancer today and tomorrow: A global assessment by world region and Human Development Index using GLOBOCAN 2020. Int J Cancer. 2022;151:1535-41.
Savant SS, Sriramkumar S, O’Hagan HM. The role of inflammation and inflammatory mediators in the development, progression, metastasis, and chemoresistance of epithelial ovarian cancer. Cancers. 2018;10:251.
Trabert B, Tworoger SS, O’Brien KM, Townsend MK, Fortner RT, Iversen ES, et al. The risk of ovarian cancer increases with an increase in the lifetime number of ovulatory cycles: an analysis from the ovarian cancer cohort consortium (OC3). Cancer Res. 2020;80:1210–8.
Reid BM, Permuth JB, Sellers TA. Epidemiology of ovarian cancer: a review. Cancer Biol Med. 2017;14:9–32.
Rasmussen CB, Kjaer SK, Albieri V, Bandera EV, Doherty JA, Høgdall E, et al. Pelvic inflammatory disease and the risk of ovarian cancer and borderline ovarian tumors: a pooled analysis of 13 case-control studies. Am J Epidemiol. 2017;185:8–20.
Hermens M, van Altena AM, Nieboer TE, Schoot BC, van Vliet HAAM, Siebers AG, et al. Incidence of endometrioid and clear-cell ovarian cancer in histological proven endometriosis: the ENOCA population-based cohort study. Am J Obstet Gynecol. 2020;223:107.e1–e11.
Huang T, Tworoger SS, Willett WC, Stampfer MJ, Rosner BA. Associations of early life and adulthood adiposity with risk of epithelial ovarian cancer. Ann Oncol. 2019;30:303–9.
Peres LC, Mallen AR, Townsend MK, Poole EM, Trabert B, Allen NE, et al. High levels of C-reactive protein are associated with an increased risk of ovarian cancer: results from the ovarian cancer cohort consortiumc-reactive protein and ovarian cancer risk. Cancer Res. 2019;79:5442–51.
Bosetti C, Santucci C, Gallus S, Martinetti M, La Vecchia C. Aspirin and the risk of colorectal and other digestive tract cancers: an updated meta-analysis through 2019. Ann Oncol. 2020;31:558–68.
Trabert B, Ness RB, Lo-Ciganic WH, Murphy MA, Goode EL, Poole EM, et al. Aspirin, nonaspirin nonsteroidal anti-inflammatory drug, and acetaminophen use and risk of invasive epithelial ovarian cancer: a pooled analysis in the ovarian cancer association consortium. J Natl Cancer Inst. 2014;106:djt431.
Trabert B, Poole EM, White E, Visvanathan K, Adami HO, Anderson GL, et al. Analgesic use and ovarian cancer risk: an analysis in the ovarian cancer cohort consortium. J Natl Cancer Inst. 2019;111:137–45.
Santucci C, Gallus S, Martinetti M, La Vecchia C, Bosetti C. Aspirin and the risk of nondigestive tract cancers: an updated meta‐analysis to 2019. Int J Cancer. 2021;148:1372–82.
Hurwitz LM, Pinsky PF, Huang WY, Freedman ND, Trabert B. Aspirin use and ovarian cancer risk using extended follow-up of the PLCO Cancer Screening Trial. Gynecol Oncol. 2020;159:522–6.
Barnard ME, Poole EM, Curhan GC, Eliassen AH, Rosner BA, Terry KL, et al. Association of analgesic use with risk of ovarian cancer in the nurses’ health studies. JAMA Oncol. 2018;4:1675–82.
Peres LC, Camacho F, Abbott SE, Alberg AJ, Bandera EV, Barnholtz-Sloan J, et al. Analgesic medication use and risk of epithelial ovarian cancer in African American women. Br J Cancer. 2016;114:819–25.
Hannibal CG, Rossing MA, Wicklund KG, Cushing-Haugen KL. Analgesic drug use and risk of epithelial ovarian cancer. Am J Epidemiol. 2008;167:1430–7.
Hurwitz LM, Townsend MK, Jordan SJ, Patel AV, Teras LR, Lacey JV, et al. Modification of the association between frequent aspirin use and ovarian cancer risk: a meta-analysis using individual-level data from two ovarian cancer consortia. J Clin Oncol. 2022;40:4207–17.
Gjerstorff ML. The Danish cancer registry. Scand J Public Health. 2011;39:42–5.
Ji J, Sundquist K, Sundquist J, Hemminki K. Comparability of cancer identification among death registry, cancer registry and hospital discharge registry. Int J cancer. 2012;131:2085–93.
Gaster N, Hallas J, Pottegård A, Friis S, Schmidt M. The validity of danish prescription data to measure use of aspirin and other non-steroidal anti-inflammatory drugs and quantification of bias due to non-prescription drug use. Clin Epidemiol. 2021;13:569–79.
Jonsson F, Yin L, Lundholm C, Smedby KE, Czene K, Pawitan Y. Low-dose aspirin use and cancer characteristics: a population-based cohort study. Br J Cancer. 2013;109:1921–5.
Vandenbroucke JP, Pearce N. Case-control studies: basic concepts. Int J Epidemiol. 2012;41:1480–9.
Gupta RA, Tejada LV, Tong BJ, Das SK, Morrow JD, Dey SK, et al. Cyclooxygenase-1 is overexpressed and promotes angiogenic growth factor production in ovarian cancer1. Cancer Res. 2003;63:906–11.
Huang Y, Lichtenberger LM, Taylor M, Bottsford-Miller JN, Haemmerle M, Wagner MJ, et al. Antitumor and antiangiogenic effects of aspirin-PC in ovarian cancer. Mol Cancer Ther. 2016;15:2894–904.
Beeghly-Fadiel A, Wilson AJ, Keene S, El Ramahi M, Xu S, Marnett LJ, et al. Differential cyclooxygenase expression levels and survival associations in type I and type II ovarian tumors. J Ovarian Res. 2018;11:17.
Xie Y, Pan M, Gao Y, Zhang L, Ge W, Tang P. Dose-dependent roles of aspirin and other non-steroidal anti-inflammatory drugs in abnormal bone remodeling and skeletal regeneration. Cell Biosci. 2019;9:1–11.
Joharatnam-Hogan N, Cafferty FH, Macnair A, Ring A, Langley RE. The role of aspirin in the prevention of ovarian, endometrial and cervical cancers. Women’s Health (Lond, Engl). 2020;16:1745506520961710.
Wernli KJ, Newcomb PA, Hampton J, Trentham-Dietz A, Egan KM. Inverse association of NSAID use and ovarian cancer in relation to oral contraceptive use and parity. Br J Cancer. 2008;98:1781–3.
Joseph P, Leong D, McKee M, Anand SS, Schwalm J-D, Teo K, et al. Reducing the global burden of cardiovascular disease, part 1: the epidemiology and risk factors. Circul Res. 2017;121:677–94.
Skriver C, Maltesen T, Dehlendorff C, Skovlund CW, Schmidt M, Sørensen HT, et al. Long-term aspirin use and cancer risk: a 20-year cohort study. J Natl Cancer Inst. 2023:djad231, https://doi.org/10.1093/jnci/djad231.
Acknowledgements
We express our gratitude to Senior Researcher Søren Friis for providing his expert opinion on the correlation between low-dose aspirin and ovarian cancer.
Funding
This work was funded by the Mermaid project (Mermaid III).
Author information
Authors and Affiliations
Contributions
G.Z.: Conceptualization, Methodology, Investigation, Data management, Formal analysis, Writing—original draft. M.T.F.: Conceptualization, Methodology, Writing—review & editing, Project administration. J.W.: Investigation, Writing—review & editing, Project administration. L.B.: Conceptualization, Methodology, Writing—review & editing. R.H.L.: Data management, Investigation, Writing—review & editing. K.S.: Investigation, Writing—review & editing, Project administration. S.K.K.: Conceptualization, Methodology, Investigation, Writing—review & editing, Project administration, Supervision, Funding.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval
The study is based on data from Danish and Swedish health registries with no direct involvement of study participants and thus no ethical approval was needed. For the data from Denmark, the relevant approvals for use of the included register data, which are placed in a project database at Statistics Denmark (project number 704327), were obtained. The Danish Cancer Society is responsible for the data stored at the Danish Cancer Society Research Center’s project database at Statistics Denmark. In agreement with the General Data Protection Regulation, the project is registered in the Danish Cancer Society’s internal list of projects that are dealing with personalized data (Journal numbers 2018-DCRC-0050 and 2019-DCRC-0054). The study was performed in accordance with the Declaration of Helsinki. For the data from Sweden, ethical approval for the study was obtained from the Ethical Review Authority of Sweden. Karolinska Institutet is responsible for the data stored for use in the project.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zheng, G., Faber, M.T., Wang, J. et al. Low-dose aspirin use and risk of ovarian cancer: a combined analysis from two nationwide studies in Denmark and Sweden. Br J Cancer 130, 1279–1285 (2024). https://doi.org/10.1038/s41416-024-02609-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41416-024-02609-7