Abstract
Background
Type 2 diabetes (T2D) is associated with higher risk of pancreatic cancer (PC), but the underlying mechanisms are not fully understood.
Methods
We conducted a case-subcohort study involving 610 PC cases and 623 subcohort participants with 92 protein biomarkers measured in baseline plasma samples. Genetically-instrumented T2D was derived using 86 single-nucleotide polymorphisms (SNPs), including insulin resistance (IR) SNPs.
Results
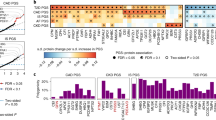
In observational analyses of 623 subcohort participants (mean age, 52 years; 61% women), T2D was positively associated with 13 proteins (SD difference: IL6: 0.52 [0.23–0.81]; IL10: 0.41 [0.12–0.70]), of which 8 were nominally associated with incident PC. The 8 proteins potentially mediated 36.9% (18.7–75.0%) of the association between T2D and PC. In MR, no associations were observed for genetically-determined T2D with proteins, but there were positive associations of genetically-determined IR with IL6 and IL10 (SD difference: 1.23 [0.05–2.41] and 1.28 [0.31–2.24]). In two-sample MR, fasting insulin was associated with both IL6 and PC, but no association was observed between IL6 and PC.
Conclusions
Proteomics were likely to explain the association between T2D and PC, but were not causal mediators. Elevated fasting insulin driven by insulin resistance might explain the associations of T2D, proteomics, and PC.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 24 print issues and online access
$259.00 per year
only $10.79 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
Data availability
CKB investigators are committed to sharing this important resource with the wider scientific community, so that the potential value of the CKB resource can be maximized. Open access to the CKB resource has begun in a phased approach. To facilitate the process a Data Access Committee (see http://www.ckbiobank.org/site/Data+Access) has been established, comprising not only senior CKB scientists but also external experts in related fields. For any external data access requests, an outline proposal defining the purpose of the investigation, the data/samples required and the time-scale for the analysis needs to be completed and submitted for review by the study executive committee. The access request review will assess the scientific merit of the proposal to ensure that research questions are legitimate and that there is no duplication of effort. Only proposals complying with the activities listed in the participant’s original consent and with the study’s ethical approval will be considered. To facilitate future collaboration and streamline data sharing and access, a detailed policy document on data access and a related IT platform has been developed and made available on the study web site (www.ckbiobank.org). The policy reflects the principles of the data access policies promoted by the study funders, as well as certain specific conditions already agreed with the original funder (the Kadoorie Foundation) and Chinese government. Information on access to the CKB resource is actively disseminated through workshops, seminars and conference presentations, in published articles, and through the study website. To date over 250 researchers have registered through our data sharing system and over 100 datasets have been securely delivered to open access users and collaborators using this facility.
References
Kocarnik JM, Compton K, Dean FE, Fu W, Gaw BL, Harvey JD, et al. Cancer incidence, mortality, years of life lost, years lived with disability, and disability-adjusted life years for 29 cancer groups from 2010 to 2019: a systematic analysis for the global burden of disease study 2019. JAMA Oncol. 2022;8:420–44.
The global, regional, and national burden of pancreatic cancer and its attributable risk factors in 195 countries and territories, 1990-2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet Gastroenterol Hepatol. 2019;4:934–47.
Versteijne E, van Dam JL, Suker M, Janssen QP, Groothuis K, Akkermans-Vogelaar JM, et al. Neoadjuvant chemoradiotherapy versus upfront surgery for resectable and borderline resectable pancreatic cancer: long-term results of the Dutch randomized PREOPANC trial. J Clin Oncol. 2022;40:1220–30.
Zhu X, Cao Y, Liu W, Ju X, Zhao X, Jiang L, et al. Stereotactic body radiotherapy plus pembrolizumab and trametinib versus stereotactic body radiotherapy plus gemcitabine for locally recurrent pancreatic cancer after surgical resection: an open-label, randomised, controlled, phase 2 trial. Lancet Oncol. 2022;23:105–15.
Padrón LJ, Maurer DM, O’Hara MH, O’Reilly EM, Wolff RA, Wainberg ZA, et al. Sotigalimab and/or nivolumab with chemotherapy in first-line metastatic pancreatic cancer: clinical and immunologic analyses from the randomized phase 2 PRINCE trial. Nat Med. 2022;28:1167–77.
Pang Y, Holmes MV, Chen Z, Kartsonaki C. A review of lifestyle, metabolic risk factors, and blood-based biomarkers for early diagnosis of pancreatic ductal adenocarcinoma. J Gastroenterol Hepatol. 2019;34:330–45.
Pang Y, Holmes MV, Kartsonaki C, Guo Y, Yang L, Bian Z, et al. Young adulthood and adulthood adiposity in relation to incidence of pancreatic cancer: a prospective study of 0.5 million Chinese adults and a meta-analysis. J Epidemiol Commun Health. 2017;71:1059–67.
Pang Y, Kartsonaki C, Guo Y, Bragg F, Yang L, Bian Z, et al. Diabetes, plasma glucose and incidence of pancreatic cancer: a prospective study of 0.5 million Chinese adults and a meta-analysis of 22 cohort studies. Int J Cancer. 2017;140:1781–8.
Kartsonaki C, Pang Y, Millwood I, Yang L, Guo Y, Walters R, et al. Circulating proteins and risk of pancreatic cancer: a case-subcohort study among Chinese adults. Int J Epidemiol. 2022;51:817–29.
Carreras-Torres R, Johansson M, Gaborieau V, Haycock PC, Wade KH, Relton CL, et al. The role of obesity, type 2 diabetes, and metabolic factors in pancreatic cancer: a Mendelian Randomization study. J Natl Cancer Inst. 2017;109. https://doi.org/10.1093/jnci/djx012.
Bao X, Xu B, Yin S, Pan J, Nilsson PM, Nilsson J, et al. Proteomic profiles of body mass index and waist-to-hip ratio and their role in incidence of diabetes. J Clin Endocrinol Metab. 2022;107:2982–90.
Molvin J, Pareek M, Jujic A, Melander O, Råstam L, Lindblad U, et al. Using a targeted proteomics chip to explore pathophysiological pathways for incident diabetes- the Malmö preventive project. Sci Rep. 2019;9:272 https://doi.org/10.1038/s41598-018-36512-y.
Elhadad MA, Jonasson C, Huth C, Wilson R, Gieger C, Matias P, et al. Deciphering the plasma proteome of type 2 diabetes. Diabetes. 2020;69:2766–78.
Palmquist C, Dehlendorff C, Calatayud D, Hansen CP, Hasselby JP, Johansen JS. Prediction of unresectability and prognosis in patients undergoing surgery on suspicion of pancreatic cancer using Carbohydrate Antigen 19-9, Interleukin 6, and YKL-40. Pancreas. 2020;49:53–61.
Ramsey ML, Talbert E, Ahn D, Bekaii-Saab T, Badi N, Bloomston PM, et al. Circulating interleukin-6 is associated with disease progression, but not cachexia in pancreatic cancer. Pancreatology. 2019;19:80–87.
Long KB, Tooker G, Tooker E, Luque SL, Lee JW, Pan X, et al. IL6 receptor blockade enhances chemotherapy efficacy in pancreatic ductal adenocarcinoma. Mol Cancer Ther. 2017;16:1898–908.
Grote VA, Kaaks R, Nieters A, Tjønneland A, Halkjær J, Overvad K, et al. Inflammation marker and risk of pancreatic cancer: a nested case-control study within the EPIC cohort. Br J Cancer. 2012;106:1866–74.
Bao Y, Giovannucci EL, Kraft P, Qian ZR, Wu C, Ogino S, et al. Inflammatory plasma markers and pancreatic cancer risk: a prospective study of five U.S. cohorts. Cancer Epidemiol Biomark Prev. 2013;22:855–61.
Sjaarda J, Gerstein H, Chong M, Yusuf S, Meyre D, Anand SS, et al. Blood CSF1 and CXCL12 as Causal Mediators of Coronary Artery Disease. J Am Coll Cardiol. 2018;72:300–10.
Sjaarda J, Gerstein HC, Yusuf S, Treleaven D, Walsh M, Mann JFE, et al. Blood HER2 and Uromodulin as Causal Mediators of CKD. J Am Soc Nephrol. 2018;29:1326–35.
Chen Z, Chen J, Collins R, Guo Y, Peto R, Wu F, et al. China Kadoorie Biobank of 0.5 million people: survey methods, baseline characteristics and long-term follow-up. Int J Epidemiol. 2011;40:1652–66.
Lundberg M, Thorsen SB, Assarsson E, Villablanca A, Tran B, Gee N, et al. Multiplexed homogeneous proximity ligation assays for high-throughput protein biomarker research in serological material. Mol Cell Proteom. 2011;10:M110.004978.
Assarsson E, Lundberg M, Holmquist G, Björkesten J, Thorsen SB, Ekman D, et al. Homogenous 96-plex PEA immunoassay exhibiting high sensitivity, specificity, and excellent scalability. PLoS One. 2014;9:e95192 https://doi.org/10.1371/journal.pone.0095192.
Olink. Olink validation document for the Immuno-Oncology panel (article number 95310). https://www.olink.com/resources-support/document-download-center/. 2018. Accessed December 2018.
Gan W, Bragg F, Walters RG, Millwood IY, Lin K, Chen Y, et al. Genetic predisposition to type 2 diabetes and risk of subclinical atherosclerosis and cardiovascular diseases among 160,000 Chinese adults. Diabetes. 2019;68:2155–64.
Morris AP, Voight BF, Teslovich TM, Ferreira T, Segrè AV, Steinthorsdottir V, et al. Large-scale association analysis provides insights into the genetic architecture and pathophysiology of type 2 diabetes. Nat Genet. 2012;44:981–90.
Dimas AS, Lagou V, Barker A, Knowles JW, Mägi R, Hivert MF, et al. Impact of type 2 diabetes susceptibility variants on quantitative glycemic traits reveals mechanistic heterogeneity. Diabetes. 2014;63:2158–71.
Prokopenko I, Poon W, Mägi R, Prasad BR, Salehi SA, Almgren P, et al. A central role for GRB10 in regulation of islet function in man. PLoS Genet. 2014;10:e1004235.
Manning AK, Hivert MF, Scott RA, Grimsby JL, Bouatia-Naji N, Chen H, et al. A genome-wide approach accounting for body mass index identifies genetic variants influencing fasting glycemic traits and insulin resistance. Na Genet. 2012;44:659–69.
Tingley D, Yamamoto T, Hirose K, Keele L, Imai K. mediation: R package for causal mediation analysis. J Stat Softw. 2014;59:1–38.
Acknowledgements
The chief acknowledgment is to the participants, the project staff, and the China National Centre for Disease Control and Prevention (CDC) and its regional offices for access to death and disease registries. The Chinese National Health Insurance scheme provides electronic linkage to all hospital admission data.
Funding
This work was supported by National Natural Science Foundation of China (82304223, 82192901, 82192904, 82192900). The CKB baseline survey and the first re-survey were supported by a grant from the Kadoorie Charitable Foundation in Hong Kong. The long-term follow-up is supported by grants from the UK Wellcome Trust (212946/Z/18/Z, 202922/Z/16/Z, 104085/Z/14/Z, 088158/Z/09/Z), grants (2016YFC0900500) from the National Key R&D Program of China, National Natural Science Foundation of China (81390540, 91846303, 81941018), and Chinese Ministry of Science and Technology (2011BAI09B01). Dr Pang acknowledges support from the Peking University Medicine Fund of Fostering Young Scholars’ Scientific & Technological Innovation (BMU2022RCZX022), the Fundamental Research Funds for the Central Universities, and the Peking University Start-up Grant (BMU2022PY014). The proteomics analysis was funded by NDPH Pump Priming Award, Pancreatic Cancer UK (A102016RIFProfZChen), and Cancer Research UK Oxford Centre (C552/A17720). The funders had no role in the study design, data collection, data analysis and interpretation, writing of the report, or the decision to submit the article for publication.
Author information
Authors and Affiliations
Contributions
YP, LL, ZC, and CK had full access to the data. YP and CK conducted data analysis and are responsible for accuracy of the results and the decision to submit for publication. All authors were involved in study design, conduct, long-term follow-up, review and coding of disease events, interpretation of the results, or writing the report. All authors approved the final version of the manuscript. YP is the guarantor of this work and, as such, had full access to all the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Pang, Y., Lv, J., Wu, T. et al. Associations of diabetes, circulating protein biomarkers, and risk of pancreatic cancer. Br J Cancer 130, 504–510 (2024). https://doi.org/10.1038/s41416-023-02533-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41416-023-02533-2