Abstract
Background
Cirrhosis is a risk factor for intrahepatic cholangiocarcinoma (iCC). However, its exact prevalence is uncertain and its impact on the management of advanced disease is not established.
Methods
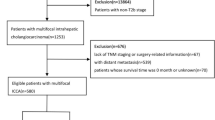
Retrospective analysis of patients treated with systemic chemotherapy for advanced iCC in the 1st-line setting at 2 tertiary cancer referral centres. Cirrhosis was diagnosed based on at least one element prior to any treatment: pathological diagnosis, baseline platelets <150 × 109/L, portal hypertension and/or dysmorphic liver on imaging.
Results
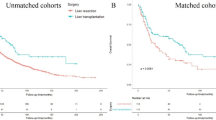
In the cohort of patients (n = 287), 82 (28.6%) had cirrhosis (45 based on pathological diagnosis). Patients with cirrhosis experienced more grade 3/4 haematologic toxicity (44% vs 22%, respectively, P = 0.001), and more grade 3/4 non-haematologic toxicity (34% vs 14%, respectively, P = 0.001) than those without. The overall survival (OS) was significantly shorter in patients with cirrhosis: median 9.1 vs 13.1 months for those without (HR = 1.56 [95% CI: 1.19–2.05]); P = 0.002), confirmed on multivariable analysis (HR = 1.48 [95% CI: 1.04–2.60]; P = 0.028).
Conclusion
Cirrhosis was relatively common in patients with advanced iCC and was associated with increased chemotherapy-induced toxicity and shorter OS. Formal assessment and consideration of cirrhosis in therapeutic management is recommended.

This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 24 print issues and online access
$259.00 per year
only $10.79 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
Data availability
Any request of data should be addressed to the corresponding author.
References
Chang KY, Chang JY, Yen Y. Increasing incidence of intrahepatic cholangiocarcinoma and its relationship to chronic viral hepatitis. J Natl Compr Cancer Netw JNCCN. 2009;7:423–7.
Lamarca A, Benafif S, Ross P, Bridgewater J, Valle JW. Cisplatin and gemcitabine in patients with advanced biliary tract cancer (ABC) and persistent jaundice despite optimal stenting: effective intervention in patients with luminal disease. Eur J Cancer. 2015;51:1694–703.
Izquierdo-Sanchez L, Lamarca A, La Casta A, Buettner S, Utpatel K, Klümpen HJ, et al. Cholangiocarcinoma landscape in Europe: diagnostic, prognostic and therapeutic insights from the ENSCCA Registry. J Hepatol. 2022;76:1109–21.
Alison MR, Lovell MJ. Liver cancer: the role of stem cells. Cell Prolif. 2005;38:407–21.
Roskams T. Liver stem cells and their implication in hepatocellular and cholangiocarcinoma. Oncogene. 2006;25:3818–22.
Clements O, Eliahoo J, Kim JU, Taylor-Robinson SD, Khan SA. Risk factors for intrahepatic and extrahepatic cholangiocarcinoma: a systematic review and meta-analysis. J Hepatol. 2020;72:95–103.
Lee YT, Wang JJ, Luu M, Noureddin M, Nissen NN, Patel TC, et al. Comparison of clinical features and outcomes between intrahepatic cholangiocarcinoma and hepatocellular carcinoma in the United States. Hepatol Balt Md. 2021;74:2622–32.
Jesper D, Heyn SG, Schellhaas B, Pfeifer L, Goertz RS, Zopf S, et al. Effects of liver cirrhosis and patient condition on clinical outcomes in intrahepatic cholangiocarcinoma: a retrospective analysis of 156 cases in a single center. Eur J Gastroenterol Hepatol. 2018;30:552–6.
Hui CK, Yuen MF, Tso WK, Ng IOL, Chan AOO, Lai CL. Cholangiocarcinoma in liver cirrhosis. J Gastroenterol Hepatol. 2003;18:337–41.
Li YY, Chen DJ, Li XR, Tian BN, Liu WD, Liu G, et al. Clinicopathological characteristics of intrahepatic cholangiocarcinoma in patients with cirrhosis. Hepatogastroenterology. 2011;58:1787–90.
Li YY, Li H, Lv P, Liu G, Li XR, Tian BN, et al. Prognostic value of cirrhosis for intrahepatic cholangiocarcinoma after surgical treatment. J Gastrointest Surg J Soc Surg Aliment Trac. 2011;15:608–13.
Jeong S, Gao L, Tong Y, Xia L, Xu N, Sha M, et al. Prognostic impact of cirrhosis in patients with intrahepatic cholangiocarcinoma following hepatic resection. Can J Gastroenterol Hepatol. 2017;2017:6543423.
Johnson PJ, Berhane S, Kagebayashi C, Satomura S, Teng M, Reeves HL, et al. Assessment of liver function in patients with hepatocellular carcinoma: a new evidence-based approach—the ALBI grade. J Clin Oncol. 2015;33:550–8.
Childs A, Zakeri N, Ma YT, O’Rourke J, Ross P, Hashem E, et al. Biopsy for advanced hepatocellular carcinoma: results of a multicentre UK audit. Br J Cancer. 2021;125:1350–5.
Neuzillet C, Emery C, Teissier C, Bouée S, Lièvre A. Patient healthcare trajectories of intrahepatic cholangiocarcinoma in France: a nationwide retrospective analysis. Lancet Reg Health - Eur. 2022;15:100324.
Funding
This study did not receive any funding.
Author information
Authors and Affiliations
Contributions
MMN: research grant support: Servier, Ipsen and NuCana. Travel and accommodation: Bayer and Ipsen, Speaker honoraria: Advanced Accelerator Applications (UK and Ireland) Ltd., Pfizer, Ipsen, NuCana and Mylan. Advisory boards: Celgene, Ipsen, Sirtex, Baxalta, Incyte and AstraZeneca. AL: Dr Angela Lamarca has received travel and educational support from Ipsen, Pfizer, Bayer, AAA, SirtEx, Novartis, Mylan and Delcath; speaker honoraria from Merck, Pfizer, Ipsen, Incyte, AAA, QED, Servier, AstraZeneca and EISAI; advisory and consultancy honoraria from EISAI, Nutricia Ipsen, QED, Roche, Servier, Boston Scientific, Albireo Pharma, AstraZeneca, Boehringer Ingelheim, GENFIT and TransThera Biosciences; she is member of the Knowledge Network and NETConnect Initiatives funded by Ipsen. JE: Honoraria: MSD, Eisai, BMS, AstraZeneca, Bayer, Roche, Ipsen, Basilea, Merck Serono, Incyte, Servier, Beigene; Travel expense: Amgen; Research funding (institutional): BMS, Beigene. RAH: Travel and accommodation support from Ipsen, BMS, Bayer, Roche; speaker honoraria from IPSEN, Mylan, Beigene; advisory and consultancy honoraria from EISAI, Roche, Boston Scientific, Novartis, and Beigene. AL (A Lièvre): honoraria from AAA, Amgen, Astellas, Bayer, BMS, Incyte, Ipsen, Leo-pharma, Mylan, Novartis, Pierre Fabre, Roche, Sandoz, Sanofi, Servier and Viatris; travel/congress registration support from Boehringer, Ipsen, Mylan, MSD, Pierre Fabre, Roche and Servier; research funding (institutional) from Bayer, Lilly, Novartis. JWV: honoraria from Agios, AstraZeneca, Baxter, Genoscience Pharma, Hutchmed, Imaging Equipment Ltd (AAA), Incyte, Ipsen, Mundipharma EDO, Mylan, QED, Servier, Sirtex and Zymeworks; grants, personal fees and non-financial support from NuCana, all outside the submitted work.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
d’Abrigeon, C., McNamara, M.G., Le Sourd, S. et al. Influence of cirrhosis on outcomes of patients with advanced intrahepatic cholangiocarcinoma receiving chemotherapy. Br J Cancer 129, 1766–1772 (2023). https://doi.org/10.1038/s41416-023-02460-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41416-023-02460-2