Abstract
Background
Whether obesity and being overweight, defined by body mass index (BMI), increase hepatocellular carcinoma (HCC) has been less apparent in Asian populations.
Methods
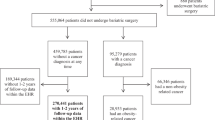
Overall, 14,265,822 Korean adults who underwent routine health examinations during 2003–2006 were followed up for HCC. Multivariable-adjusted hazard ratios (HRs) associated with BMI were calculated.
Results
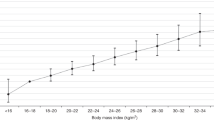
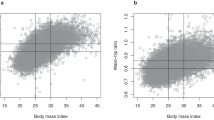
During 13.7 years (mean) of follow-up, 47,308 individuals developed HCC. HRs of HCC associated with BMIs of 25.0–26.4, 26.5–27.9, 28.0–29.4, 29.5–30.9 and ≥31 kg/m² compared to those for 23.5–24.9 kg/m² were 1.05, 1.20, 1.39, 1.59 and 2.13, respectively. For BMI < 25 kg/m², linear associations were not apparent. For BMI ≥ 25 kg/m2, the HR per 5 kg/m2 increase in BMI was 1.60 (total), 1.60 (men), and 1.59 (women). The corresponding HRs were 1.56, 1.61 and 1.60 for individuals aged <45, 45–64 and ≥65 years, respectively. Further adjustment for alanine transaminase (ALT) levels substantially reduced the HRs for high BMI, especially in men and younger adults.
Conclusions
Overweight and obesity clearly increase HCC risk in Koreans. ALT levels are a mediator of the impact of obesity, but it may not accurately predict high BMI-induced liver damage that can potentially progress to HCC, especially in women and older adults.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 24 print issues and online access
$259.00 per year
only $10.79 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
Data availability
The data underlying the results presented in the study are available from the National Health Insurance Service (https://nhiss.nhis.or.kr/bd/ab/bdaba000eng.do).
Code availability
All data analyses were performed using SAS, version 9.4 (SAS Institute, Inc., Cary, NC). The code used to perform the analysis is available on request to the authors.
References
Petrick JL, Braunlin M, Laversanne M, Valery PC, Bray F, McGlynn KA. International trends in liver cancer incidence, overall and by histologic subtype, 1978-2007. Int J Cancer. 2016;139:1534–45.
Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A, et al. Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2021;71:209–49.
Parr CL, Batty GD, Lam TH, Barzi F, Fang X, Ho SC, et al. Body-mass index and cancer mortality in the Asia-Pacific Cohort Studies Collaboration: pooled analyses of 424 519 participants. Lancet Oncol. 2010;11:741–52.
Yi SW, Choi JS, Yi JJ, Lee YH, Han KJ. Risk factors for hepatocellular carcinoma by age, sex, and liver disorder status: a prospective cohort study in Korea. Cancer. 2018;124:2748–57.
Gupta A, Das A, Majumder K, Arora N, Mayo HG, Singh PP, et al. Obesity is independently associated with increased risk of hepatocellular cancer-related mortality: a systematic review and meta-analysis. Am J Clin Oncol. 2018;41:874.
Calle EE, Rodriguez C, Walker-Thurmond K, Thun MJ. Overweight, obesity, and mortality from cancer in a prospectively studied cohort of US adults. N. Engl J Med. 2003;348:1625–38.
Liu X, Ju W, Huo C, Zhang S, Wang X, Huang K. Overweight and obesity as independent factors for increased risk of hepatocellular cancer-related mortality: a meta-analysis. J Am Coll Nutr. 2021;40:287–93.
Setiawan VW, Lim U, Lipworth L, Lu SC, Shepherd J, Ernst T, et al. Sex and ethnic differences in the association of obesity with risk of hepatocellular carcinoma. Clin Gastroenterol Hepatol. 2016;14:309–16.
Chen Y, Wang X, Wang J, Yan Z, Luo J. Excess body weight and the risk of primary liver cancer: an updated meta-analysis of prospective studies. Eur J Cancer. 2012;48:2137–45.
Oh SW, Yoon YS, Shin S-A. Effects of excess weight on cancer incidences depending on cancer sites and histologic findings among men: Korea National Health Insurance Corporation Study. J Clin Oncol. 2005;23:4742–54.
Batty GD, Barzi F, Huxley R, Chang CY, Jee SH, Jamrozik K, et al. Obesity and liver cancer mortality in Asia: the Asia Pacific cohort studies collaboration. Cancer Epidemiol. 2009;33:469–72.
Nam GE, Kim YH, Han K, Jung JH, Rhee EJ, Lee WY, et al. Obesity fact sheet in Korea, 2020: prevalence of obesity by obesity class from 2009 to 2018. J Obes Metab Syndr. 2021;30:141–8.
Hales CM, Carroll MD, Fryar CD, Ogden CL. Prevalence of obesity and severe obesity among adults: United States, 2017-2018. NCHS Data Brief. 2020;(360):1–8.
Wong MCS, Huang JLW, George J, Huang J, Leung C, Eslam M, et al. The changing epidemiology of liver diseases in the Asia-Pacific region. Nat Rev Gastroenterol Hepatol. 2019;16:57–73.
Chiang CH, Lee LT, Hung SH, Lin WY, Hung HF, Yang WS, et al. Opposite association between diabetes, dyslipidemia, and hepatocellular carcinoma mortality in the middle-aged and elderly. Hepatology. 2014;59:2207–15.
Loomba R, Yang H-I, Su J, Brenner D, Barrett-Connor E, Iloeje U, et al. Synergism between obesity and alcohol in increasing the risk of hepatocellular carcinoma: a prospective cohort study. Am J Epidemiol. 2013;177:333–42.
Nderitu P, Bosco C, Garmo H, Holmberg L, Malmstrom H, Hammar N, et al. The association between individual metabolic syndrome components, primary liver cancer and cirrhosis: a study in the Swedish AMORIS cohort. Int J Cancer. 2017;141:1148–60.
Yi SW, Ohrr H, Shin SA, Yi JJ. Sex-age-specific association of body mass index with all-cause mortality among 12.8 million Korean adults: a prospective cohort study. Int J Epidemiol. 2015;44:1696–705.
Oh CM, Won YJ, Jung KW, Kong HJ, Cho H, Lee JK, et al. Cancer statistics in Korea: incidence, mortality, survival, and prevalence in 2013. Cancer Res Treat. 2016;48:436–50.
Seo HJ, Oh IH, Yoon SJ. A comparison of the cancer incidence rates between the national cancer registry and insurance claims data in Korea. Asian Pac J Cancer Prev. 2012;13:6163–8.
Lee EY, Lee YH, Yi SW, Shin SA, Yi JJ. BMI and all-cause mortality in normoglycemia, impaired fasting glucose, newly diagnosed diabetes, and prevalent diabetes: a cohort study. Diabetes Care. 2017;40:1026–33.
Yi SW, Kim SH, Han KJ, Yi JJ, Ohrr H. Higher cholesterol levels, not statin use, are associated with a lower risk of hepatocellular carcinoma. Br J Cancer. 2020;122:630–3.
Borena W, Strohmaier S, Lukanova A, Bjørge T, Lindkvist B, Hallmans G, et al. Metabolic risk factors and primary liver cancer in a prospective study of 578,700 adults. Int J Cancer. 2012;131:193–200.
Hassan MM, Abdel-Wahab R, Kaseb A, Shalaby A, Phan AT, El-Serag HB, et al. Obesity early in adulthood increases risk but does not affect outcomes of hepatocellular carcinoma. Gastroenterology. 2015;149:119–29.
Jee SH, Yun JE, Park EJ, Cho ER, Park IS, Sull JW, et al. Body mass index and cancer risk in Korean men and women. Int J Cancer. 2008;123:1892–6.
Liu Y, Warren Andersen S, Wen W, Gao YT, Lan Q, Rothman N, et al. Prospective cohort study of general and central obesity, weight change trajectory and risk of major cancers among Chinese women. Int J Cancer. 2016;139:1461–70.
Chen CL, Yang HI, Yang WS, Liu CJ, Chen PJ, You SL, et al. Metabolic factors and risk of hepatocellular carcinoma by chronic hepatitis B/C infection: a follow-up study in Taiwan. Gastroenterology. 2008;135:111–21.
Duan D, Xu J, Feng X, Astell-Burt T, Xu G, Lu N, et al. Does body mass index and adult height influence cancer incidence among Chinese living with incident type 2 diabetes? Cancer Epidemiol. 2018;53:187–94.
Chen C-T, Chen J-Y, Wang J-H, Chang K-C, Tseng P-L, Kee K-M, et al. Diabetes mellitus, metabolic syndrome and obesity are not significant risk factors for hepatocellular carcinoma in an HBV- and HCV-endemic area of Southern Taiwan. Kaohsiung J Med Sci. 2013;29:451–9.
Bhaskaran K, Douglas I, Forbes H, dos-Santos-Silva I, Leon DA, Smeeth L. Body-mass index and risk of 22 specific cancers: a population-based cohort study of 5· 24 million UK adults. Lancet. 2014;384:755–65.
Li Y, Yatsuya H, Yamagishi K, Wakai K, Tamakoshi A, Iso H, et al. Body mass index and weight change during adulthood are associated with increased mortality from liver cancer: the JACC Study. J Epidemiol. 2013;23:219–26.
Campbell PT, Newton CC, Freedman ND, Koshiol J, Alavanja MC, Freeman LEB, et al. Body mass index, waist circumference, diabetes, and risk of liver cancer for US adults. Cancer Res. 2016;76:6076–83.
Ma X, Liu S, Zhang J, Dong M, Wang Y, Wang M, et al. Proportion of NAFLD patients with normal ALT value in overall NAFLD patients: a systematic review and meta-analysis. BMC Gastroenterol. 2020;20:10.
Goh GB, Pagadala MR, Dasarathy J, Unalp-Arida A, Pai RK, Yerian L, et al. Age impacts ability of aspartate-alanine aminotransferase ratio to predict advanced fibrosis in nonalcoholic fatty liver disease. Dig Dis Sci. 2015;60:1825–31.
Funding
This research was supported by Medical Research Promotion Program through the Gangneung Asan Hospital funded by the Asan Foundation (2021IB005).
Author information
Authors and Affiliations
Contributions
BGJ and SWY conceived the study concept and design. SWY acquired the data and performed statistical analyses. BGJ, MK and SWY wrote the first draft. HSS and JJY searched literature. BGJ, MK, SWY, HSS and JJY analysed and interpreted the data. All authors contributed to the critical revision of the manuscript. All authors have read and approved the final submitted version of the manuscript. SWY is the guarantor of this study, and, as such, had full access to all the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
This study was performed in accordance with the Declaration of Helsinki. This study was approved by the Institutional Review Board of Catholic Kwandong University. Informed consent was waived because the anonymized data were used that was provided by NHIS according to strong confidentiality protocol.
Consent to publish
Not applicable.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Jun, B.G., Kim, M., Shin, H.S. et al. Impact of overweight and obesity on the risk of hepatocellular carcinoma: a prospective cohort study in 14.3 million Koreans. Br J Cancer 127, 109–115 (2022). https://doi.org/10.1038/s41416-022-01771-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41416-022-01771-0
This article is cited by
-
Metabolomic Analysis of Human Cirrhosis and Hepatocellular Carcinoma: A Pilot Study
Digestive Diseases and Sciences (2024)
-
Palmitoylation-driven PHF2 ubiquitination remodels lipid metabolism through the SREBP1c axis in hepatocellular carcinoma
Nature Communications (2023)