Abstract
Background
Recently, a novel HOXB13 variant (X285K) was observed in men of African descent with prostate cancer (PCa) in Martinique. Little is known about this or other variants in HOXB13 which may play a role in PCa susceptibility in African-American (AA) men.
Methods
We sequenced HOXB13 in an AA population of 1048 men undergoing surgical treatment for PCa at Johns Hopkins Hospital.
Results
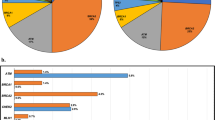
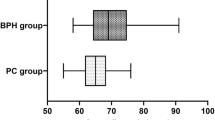
Seven non-synonymous germline variants were observed in the patient population. While six of these variants were seen only once, X285K was found in eight patients. In a case–case analysis, we find that carriers of this latter variant are at increased risk of clinically significant PCa (1.2% carrier rate in Gleason Score ≥7 PCa vs. 0% in Gleason Score <7 PCa, odds ratio, OR = inf; 95% Confidence Interval, 95%CI:1.05-inf, P = 0.028), as well as PCa with early age at diagnosis (2.4% carrier rate in patients <50 year vs. 0.5% carrier rate in patients ≥50 year, OR = 5.25, 95% CI:1.00–28.52, P = 0.03).
Conclusions
While this variant is rare in the AA population (~0.2% MAF), its ancestry-specific occurrence and apparent preferential association with risk for the more aggressive disease at an early age emphasizes its translational potential as an important, novel PCa susceptibility marker in the high-risk AA population.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 24 print issues and online access
$259.00 per year
only $10.79 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
Data availability
The data of the study are available upon reasonable request from the corresponding author.
References
American Cancer Society. Cancer Facts & Figures for African Americans 2019-2021. 2019. https://www.cancer.org/content/dam/cancer-org/research/cancer-facts-and-statistics/cancer-facts-and-figures-for-african-americans/cancer-facts-and-figures-for-african-americans-2019-2021.pdf (accessed 16 Mar 2021).
Paller CJ, Wang L, Brawley OW. Racial inequality in prostate cancer outcomes-socioeconomics, not biology. JAMA Oncol. 2019;5:983–4.
Abeshouse A, Ahn J, Akbani R, Ally A, Amin S, Andry CD, et al. The molecular taxonomy of primary prostate cancer. Cell. 2015;163:1011–25.
Ewing CM, Ray AM, Lange EM, Zuhlke KA, Robbins CM, Tembe WD, et al. Germline mutations in HOXB13 and prostate-cancer risk. N. Engl J Med. 2012;366:141–9.
Nyberg T, Govindasami K, Leslie G, Dadaev T, Bancroft E, Ni Raghallaigh H, et al. Homeobox B13 G84E mutations and prostate cancer risk. Eur Urol. 2019;75:834–45.
Xu J, Lange EM, Lu L, Zheng SL, Wang Z, Thibodeau SN, et al. HOXB13 is a susceptibility gene for prostate cancer: results from the International Consortium for Prostate Cancer Genetics (ICPCG). Hum Genet. 2013;132:5–14.
Karlsson R, Aly M, Clements M, Zheng L, Adolfsson J, Xu J, et al. A population-based assessment of germline HOXB13 G84E mutation and prostate cancer risk. Eur Urol. 2014;65:169–76.
Laitinen VH, Wahlfors T, Saaristo L, Rantapero T, Pelttari LM, Kilpivaara O, et al. HOXB13 G84E mutations in Finland: population-based analysis of prostate, breast, and colorectal cancer risk. Cancer Epidemiol Biomark Prev. 2013;22:452–60.
Akbari MR, Trachtenberg J, Lee J, Tam S, Bristow R, Loblaw A, et al. Association between germline HOXB13 G84E mutations and risk of prostate cancer. J Natl Cancer Inst. 2012;104:1260–2.
Marlin R, Créoff M, Merle S, Jean-Marie-Flore M, Rose M, Malsa S, et al. Mutation HOXB13 c.853delT in Martinican prostate cancer patients. Prostate. 2020;80:463–70.
Landrum MJ, Lee JM, Riley GR, Jang W, Rubinstein WS, Church DM, et al. ClinVar: public archive of relationships among sequence variation and human phenotype. Nucleic Acids Res. 2014;42. https://doi.org/10.1093/nar/gkt1113.
Galinsky KJ, Bhatia G, Loh PR, Georgiev S, Mukherjee S, Patterson NJ, et al. Fast principal-component analysis reveals convergent evolution of ADH1B in Europe and East Asia. Am J Hum Genet. 2016;98:456–72.
Economides KD, Capecchi MR. Hoxb13 is required for normal differentiation and secretory function of the ventral prostate. Development. 2003;130:2061–9.
Pomerantz MM, Li F, Takeda DY, Lenci R, Chonkar A, Chabot M, et al. The androgen receptor cistrome is extensively reprogrammed in human prostate tumorigenesis. Nat Genet. 2015;47:1346–51.
Chen Z, Wu D, Thomas-Ahner JM, Lu C, Zhao P, Zhang Q, et al. Diverse AR-V7 cistromes in castration-resistant prostate cancer are governed by HoxB13. Proc Natl Acad Sci USA. 2018;115:6810–5.
Norris JD, Chang CY, Wittmann BM, Kunder RS, Cui H, Fan D, et al. The homeodomain protein HOXB13 regulates the cellular response to androgens. Mol Cell. 2009;36:405–16.
Witte JS, Mefford J, Plummer SJ, Liu J, Cheng I, Klein EA, et al. HOXB13 mutation and prostate cancer: Studies of siblings and aggressive disease. Cancer Epidemiol Biomark Prev. 2013;22:675–80.
Dhamija S, Yang CM, Seiler J, Myacheva K, Caudron-Herger M, Wieland A, et al. A pan-cancer analysis reveals nonstop extension mutations causing SMAD4 tumour suppressor degradation. Nat Cell Biol. 2020;22:999–1010.
Momozawa Y, Iwasaki Y, Hirata M, Liu X, Kamatani Y, Takahashi A, et al. Germline pathogenic variants in 7636 Japanese patients with prostate cancer and 12 366 controls. J Natl Cancer Inst. 2020;112:369–76.
Lin X, Qu L, Chen Z, Xu C, Ye D, Shao Q, et al. A novel germline mutation in HOXB13 is associated with prostate cancer risk in Chinese men. Prostate. 2013;73:169–75.
Williams TM, Williams ME, Innis JW. Range of HOX/TALE superclass associations and protein domain requirements for HOXA13:MEIS interaction. Dev Biol. 2005;277:457–71.
Bhanvadia RR, Van Opstall C, Brechka H, Barashi NS, Gillard M, McAuley EM, et al. MEIS1 and MEIS2 expression and prostate cancer progression: a role for HOXB13 binding partners in metastatic disease. Clin Cancer Res. 2018;24:3668–80.
Johng D, Torga G, Ewing CM, Jin K, Norris JD, McDonnell DP, et al. HOXB13 interaction with MEIS1 modifies proliferation and gene expression in prostate cancer. Prostate. 2019;79:414–24.
Acknowledgements
The generous support from the Patrick C Walsh Hereditary Prostate Cancer program is gratefully acknowledged.
Funding
The generous support from the Patrick C Walsh Hereditary Prostate Cancer program is gratefully acknowledged. This study was supported by grants from the Department of Defense (W81XWH-16-1-0764, W81XWH-16-1-0765 and W81XWH-16-1-0766).
Author information
Authors and Affiliations
Contributions
WI conceived and designed the study. RN, MG, CS, DR, KC, PW, SC and LZ contributed materials and collected the data. RN and JW analysed the data. RN, WI and JX wrote the manuscript.
Corresponding author
Ethics declarations
Competing interests
KAC and WBI are coinventors on a patent (no. 9593380; Inst.) related to the discovery of HOXB13 as a prostate cancer susceptibility gene.
Ethics approval and consent to participate
The study was approved by the Institutional Review Boards at Johns Hopkins University. The study was performed in accordance with the Declaration of Helsinki.
Consent to publish
All the authors have reviewed and approved the current version of the manuscript.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Na, R., Wei, J., Sample, C.J. et al. The HOXB13 variant X285K is associated with clinical significance and early age at diagnosis in African American prostate cancer patients. Br J Cancer 126, 791–796 (2022). https://doi.org/10.1038/s41416-021-01622-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41416-021-01622-4
This article is cited by
-
Germline Mutations and Ancestry in Prostate Cancer
Current Oncology Reports (2024)
-
Prostate cancer genetic risk and associated aggressive disease in men of African ancestry
Nature Communications (2023)
-
Genetic and biological drivers of prostate cancer disparities in Black men
Nature Reviews Urology (2023)