Abstract
Background
Antihypertensives may inhibit pancreatic carcinogenesis. We examined the association between use of these drugs and pancreatic cancer in patients with chronic pancreatitis.
Methods
We conducted a nationwide population-based cohort study of all chronic pancreatitis patients diagnosed in Denmark during 1996–2012. Using a Cox proportional hazards model with time-varying exposure lagged by 1 year, we examined the risk of pancreatic cancer according to antihypertensive drug use.
Results
We included 8,311 patients with chronic pancreatitis and observed 153 pancreatic cancers during follow-up. At baseline, 2197 patients (26.4%) were exposed to at least one class of antihypertensive drugs. We did not observe any measurable associations between the use of antihypertensive drugs and pancreatic cancer.
Conclusions
Our findings suggest little evidence of an association between the use of antihypertensive drugs and pancreatic cancer risk in patients with chronic pancreatitis. Confirmation is warranted in future studies.
Similar content being viewed by others
Introduction
Chronic pancreatitis is an inflammatory disease characterised by progressive and irreversible destruction of the exocrine and endocrine pancreas and may eventually progress to pancreatic cancer.1 Pancreatic carcinogenesis in chronic pancreatitis patients may be inhibited by antihypertensive drugs. Experimental evidence suggest that several classes of antihypertensive drugs have anticancer properties (e.g., inhibition of pancreatic stellate cells, a key player in pancreatic carcinogenesis, by drugs acting on the renin–angiotensin system and induction of pancreatic cancer cell apoptosis by beta-blockers).2,3 Thus, antihypertensive drugs may have multiple effects on pancreatic carcinogenesis, which could decrease the risk of pancreatic cancer in patients with chronic pancreatitis and improve survival in patients with pancreatic cancer. However, findings from epidemiological studies are ambiguous.4,5,6 One study found that the use of drugs acting on the renin–angiotensin system had limited effect on pancreatic cancer risk in healthy individuals,4 but it was associated with an improved prognosis in pancreatic cancer patients.5 Other investigators suggested that beta-blockers could improve pancreatic cancer prognosis.6 Given their widespread use and generally favourable risk profiles, any potential anticancer properties of antihypertensive drugs is intriguing, as these could be used as both preventive and therapeutic agents. It is particularly important to investigate if these drugs could affect pancreatic cancer risk among patients with chronic pancreatitis, as these patients have an inherently higher risk of pancreatic cancer compared with the general population.1 We therefore conducted a nationwide population-based cohort study to examine the potential association between the use of antihypertensive drugs and pancreatic cancer risk in patients with chronic pancreatitis.
Methods
We have previously described the study design and analytic framework in detail.7 In brief, we used the Danish National Patient Registry to identify a cohort of all patients with a first-time diagnosis of chronic pancreatitis in Denmark during 1996–2012. Individual-level data linkage to the Danish Cancer Registry, Danish National Prescription Registry and the Danish Civil Registration System was used to obtain information on pancreatic cancers, comorbidities, prescription drug use and vital status. We followed patients from 1 year after their chronic pancreatitis diagnosis until pancreatic cancer, death, emigration or 31 December 2015, whichever occurred first.
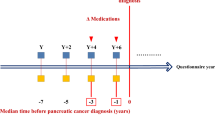
We assessed the use of antihypertensive drugs (angiotensin-converting enzyme (ACE) inhibitors, aldosterone receptor antagonists, angiotensin-II receptor antagonists, beta-blockers, calcium channel blockers and diuretics), requiring at least two filled prescriptions of the same drug class to be considered exposed. We considered drug exposure to be time varying with a 1-year lag period, allowing patients to switch between exposed and unexposed status. We considered the exposure to be continuous if two prescriptions plus their days’ supply overlapped, allowing a 30-day grace period for delays in prescription filling.
For each drug class, we calculated the crude incidence rate ratio as the ratio between the incidence rate among drug users compared with non-users. Using Cox regression, we estimated the hazard ratio (HR) of pancreatic cancer comparing drug users with non-users. In the multivariable model, we adjusted for age (restricted cubic spline with three knots), sex, socioeconomic status, year of chronic pancreatitis diagnosis, Gagne Comorbidity Index score8 and use of other antihypertensive drugs. In a supplementary analysis, we additionally adjusted for alcohol-related and smoking-related diseases to assess potential confounding from exposure to these substances.
All estimates are presented with associated 95% confidence intervals (CIs).
Results
We identified 8,311 patients with incident chronic pancreatitis in Denmark during the study period. Median age was 54 years (IQR: 45–64 years), and 5,498 (66.2%) were men (for full descriptive characteristics, please see Online Supplementary Information). In total, 153 pancreatic cancers were diagnosed during 60,365 person-years of follow-up (median 5.0 years, IQR: 2.3–8.9 years). The overall distribution of the risk estimates for the drug classes appeared to be centred around the null with few exceptions (Table 1). Our findings indicated that users of aldosterone receptor antagonists may have lower risk of pancreatic cancer, whereas the risk may be elevated in users of calcium channel blockers. However, these estimates were imprecise (Table 1). Findings from our supplementary analysis showed that adjustments for alcohol-related and smoking-related diseases did not have any measurable impact on our estimates.
Discussion
We did not observe any clinically relevant association between use of antihypertensive drugs and pancreatic cancer risk in patients with chronic pancreatitis. Chronic pancreatitis patients have a particularly high risk of pancreatic cancer,1 possibly due to sustained pancreatic inflammation. These patients generally exhibit poor lifestyle choices with a high frequency of tobacco smoking and high alcohol consumption.9 As these substances are closely associated with pancreatic cancer, they may mitigate a potential anticancer effect of antihypertensive drugs.
Despite some important strengths including the population-based design and a high positive predictive value of chronic pancreatitis diagnoses in the Danish National Patient Registry,10 some limitations should be noted. Confounding by indication may have affected our estimates, as users of antihypertensive drugs may have more comorbidity than non-users and thus potentially a higher baseline risk of pancreatic cancer. However, users of antihypertensive drugs may also have better compliance with medical treatments and healthy lifestyle choices than non-users. This is supported by a lower prevalence of alcohol-related and smoking-related diseases among users of several classes of antihypertensive drugs compared with the entire population, which may mitigate the effect of higher comorbidity levels. Pancreatic cancer was a rare event, so some of the confidence intervals were wide. However, the estimates appeared to be centred around the null, limiting concerns of imprecise estimates. We had information on redeemed prescriptions, but not actual drug consumption. As compliance with prescription drugs among chronic pancreatitis patients may be impaired, some misclassification of exposure may be present. Such misclassification would be non-differential, biasing our estimates towards the null. We had limited information on consumption of alcohol and exposure to tobacco smoking, as this information was captured using proxy diagnoses. Because such diagnoses are under-recorded in the Danish National Patient Registry, residual confounding from these substances may be present. However, we have previously shown that the alcohol-related diagnoses recorded in the Danish National Patient Registry are a valid proxy for alcoholism in chronic pancreatitis, whereas the smoking-related diagnoses are not an optimal proxy.10 Also, our exposure definitions implied that patients with few prescriptions had equivalent exposure to patients with many prescriptions. Such an exposure definition is unable to capture a potential dose-response relationship, which should be examined in a larger study.
In summary, our study suggested little evidence of an association between the use of antihypertensive drugs and pancreatic cancer risk in patients with chronic pancreatitis. Our findings warrant confirmation in larger studies.
References
Kirkegård, J., Mortensen, F. V. & Cronin-Fenton, D. Chronic pancreatitis and pancreatic cancer risk: a systematic review and meta-analysis. Am. J. Gastroenterol. 112, 1366–1372 (2017).
Masamune, A., Hamada, S., Kikuta, K., Takikawa, T., Miura, S., Nakano, E. et al. The angiotensin II type I receptor blocker olmesartan inhibits the growth of pancreatic cancer by targeting stellate cell activities in mice. Scand. J. Gastroenterol. 48, 602–609 (2013).
Zhang, D., Ma, Q., Wang, Z., Zhang, M., Guo, K., Wang, F. et al. beta2-adrenoceptor blockage induces G1/S phase arrest and apoptosis in pancreatic cancer cells via Ras/Akt/NFkappaB pathway. Mol. Cancer 10, 146 (2011).
Mandilaras, V., Bouganim, N., Yin, H., Asselah, J. & Azoulay, L. The use of drugs acting on the renin-angiotensin system and the incidence of pancreatic cancer. Br. J. Cancer 116, 103–108 (2017).
Mc Menamin, U. C., Murray, L. J., Cantwell, M. M. & Hughes, C. M. Angiotensin-converting enzyme inhibitors and angiotensin receptor blockers in cancer progression and survival: a systematic review. Cancer Causes Control 23, 221–230 (2012).
Udumyan, R., Montgomery, S., Fang, F., Almroth, H., Valdimarsdottir, U., Ekbom, A. et al. Beta-blocker drug use and survival among patients with pancreatic adenocarcinoma. Cancer Res. 77, 3700–3707 (2017).
Kirkegård, J., Lund, J. L., Mortensen, F. V. & Cronin-Fenton, D. Statins and pancreatic cancer risk in patients with chronic pancreatitis: a Danish nationwide population-based cohort study. Int. J. Cancer (2019). [Epud ahead of print]
Gagne, J. J., Glynn, R. J., Avorn, J., Levin, R. & Schneeweiss, S. A combined comorbidity score predicted mortality in elderly patients better than existing scores. J. Clin. Epidemiol. 64, 749–759 (2011).
Yadav, D. & Whitcomb, D. C. The role of alcohol and smoking in pancreatitis. Nat. Rev. Gastroenterol. Hepatol. 7, 131–145 (2010).
Kirkegård, J., Mortensen, M. R., Johannsen, I. R., Mortensen, F. V. & Cronin-Fenton, D. Positive predictive value of acute and chronic pancreatitis diagnoses in the Danish National Patient Registry: a validation study. Scand. J. Public Health 1403494818773535 (2018). [Epud ahead of print]
Acknowledgements
We thank the faculty members at Department of Epidemiology, Gillings School of Global Public Health, University of North Carolina, USA, for providing invaluable comments to the lead author during his research stay.
Author information
Authors and Affiliations
Contributions
Study design and conception: J.K., F.V.M. and D.C.F. Acquisition, analysis and interpretation of the data: J.K., F.V.M. and D.C.F. Paper drafting: J.K. Critical revisions of the paper: J.K., F.V.M. and D.C.F. All authors approved the final paper.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
This study was approved by the Danish Data Protection Agency. No ethics committee approval is required for register-based studies in Denmark.
Funding
This study was supported by the Danish Cancer Society, “Agnes og Poul Friis Fond”, “Grosserer A.V. Lykfeldt og hustrus Legat”, “Grosserer M. Brogaard og hustrus Mindefond”, “Knud og Edith Eriksens Mindefond” and “Købmand Sven Hansen og Hustru Ina Hansens Fond”.
Data availability
The data underlying this paper cannot be shared without violation of Danish law. Researchers can obtain data themselves by applying at www.sundhedsdatastyrelsen.dk (Danish Health Data Authority).
Additional information
Note: This work is published under the standard license to publish agreement. After 12 months the work will become freely available and the license terms will switch to a Creative Commons Attribution 4.0 International (CC BY 4.0).
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Kirkegård, J., Mortensen, F.V. & Cronin-Fenton, D. Antihypertensive drugs and pancreatic cancer risk in patients with chronic pancreatitis: a Danish nationwide population-based cohort study. Br J Cancer 121, 622–624 (2019). https://doi.org/10.1038/s41416-019-0562-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41416-019-0562-y