Abstract
Introduction Temporomandibular disorders (TMD) are a common source of facial pain, resulting from an interaction of biopsychosocial factors. However, social risk factors related to TMD have been researched very little, particularly in patients attending a tertiary care service.
Aims To review sociodemographic trends among patients referred to a UK tertiary TMD clinic for specialist management. To provide an insight into the sociodemographic risk factors associated with TMD in patients referred for specialist input and to discuss the surrounding literature.
Methods Retrospective review of notes of patients referred to a UK tertiary TMD clinic. Trends in areas of deprivation from which patients came from were quantified into deciles using the English Multiple Indices of Deprivation.
Results The mean age of patients was 41.1 years, with women being overrepresented compared to men. Most patients were referred by their general dental practitioner, although a variety of secondary care specialties also referred to this service. A disproportionate number of patients came from the highest decile of deprivation, a trend seen throughout the entire sample and in patients seen by dental professionals specifically. There was no apparent association between this and longer symptom duration.
Conclusion Women and those from areas with the highest levels of deprivation were overrepresented in this tertiary clinic setting. Dentists should maintain an awareness of the risk factors for TMD development as well as those which may complicate its management in cases requiring specialist input.
Key points
-
Development of chronic TMD is multifactorial; complex social situations driving pain may be under-appreciated.
-
Social factors associated with TMD have been researched very little, particularly in the specialist setting.
-
Women and those from higher deprivation areas were seen in greater numbers in this tertiary referral centre.
Similar content being viewed by others
Introduction
With an incidence (the number of new cases occurring in a population at risk during a specified time period) of up to 4%1 and a prevalence (the number of events in a given population at a designated time) reported as high as 25%, temporomandibular disorders (TMD) are a common group of clinical features.2They arise from varying degrees of dysfunction of the temporomandibular joint, its associated structures and muscles of mastication.2
Long viewed as a simple mechanical joint disease, it is now accepted that TMD is a complex chronic pain disorder.3,4,5 Research has been heavily focused on biological aetiologies6,7 and treatment centred around physical interventions, such as splinting and physiotherapy.5 Crucially, however, chronic pain is characterised not just by biological dysfunction, but by psychological and socioeconomic elements.8 Data from chronic pain conditions other than TMD show added benefits from a multidisciplinary management approach, focusing on addressing underlying psychosocial factors alongside biological intervention.9 Although there is little evidence analysing the impact of this directly in TMD, this strategy has started to be utilised in treatment as the multifactorial aetiology of the disorder shares much in common with the conditions where this approach is advantageous.10
However, a thorough understanding of the complex social background that drives TMD is required for this multidisciplinary management strategy to be successful. Studies of other chronic pain disorders, of which TMD patients are at an increased risk,11have established that those who are more deprived are more likely to suffer from chronic pain and its adverse effects.11,12A small number of studies have begun to investigate this, specifically in relation to TMD, providing inconsistent results.8,13,14Women suffer disproportionately from TMD, both in frequency and severity.1,15 Findings from other chronic pain conditions, of which women also suffer from more in general,16 suggest that social factors play a large role in this gender bias. This service evaluation aims to highlight sociodemographic trends contributing to TMD among patients referred for specialist input at a tertiary clinic.
Methods
Case notes of all newly referred patients attending a UK tertiary TMD clinic over a period of 86 weeks from January 2018 to August 2019 were reviewed as part of a retrospective service evaluation registered with the local audit office. Yorkshire and the Humber Sheffield Research Ethics Committee confirmed this was a service evaluation and therefore ethical approval was not necessary. The evaluation was registered with Sheffield Teaching Hospitals Clinical Effectiveness Unit.
Referrals to the clinic were for TMD patients whose referring clinicians felt warranted specialist input, for example those with refractory symptoms or diagnostic uncertainty with a provisional referral diagnosis of likely TMD. Adult patients aged 16 or over with a confirmed diagnosis of TMD at the specialist clinic were included in this study. Those referred for conditions other than TMD or diagnosed with another condition as the primary source of their facial pain at the tertiary clinic were excluded. Although primarily an adult clinic, paediatric patients were occasionally referred by paediatric secondary care services and were excluded from this study as their social situations are not of their own determination.
Clinic notes of all new attendees during this timeframe were reviewed to confirm a TMD diagnosis. Following this, notes were investigated for: age; sex; postcode; speciality of the referring clinician; number of specialties seen regarding TMD before referral; and duration of symptoms at the time of the initial clinic appointment.
Patients were categorised into deciles of deprivation by their postcode, using the 2019 English Indices of Multiple Deprivation (IMDs).17 The UK Government's Ministry of Housing, Communities and Local Government calculate IMDs using seven domains of deprivation: income; employment; education; health; crime; barriers to housing; and living environment.17Assessed at the local level, this is quantified into deciles with a score of one representing the most deprived decile and a score of ten representing the least deprived decile. This provides a comprehensive measure of deprivation that can be used to directly compare small areas.18
Results
A total of 180 new patients attended the clinic over the 86-week period. TMD was excluded in 15 patients and 2 patients were aged under 16, producing 163 patients overall, of whom 139 (85.2%) identified as women and 24 (14.7%) identified as men (Fig. 1). Patients ranged from ages 16-78, with a mean age of 41.1 years (SD ± 15.9) (Fig. 2). There was little difference between the distribution and mean when evaluating men and women separately; women's mean age was 41.2 years (SD ±15.9, range 16-78) compared to the men's of 40.5 years (SD ± 16.2, range 16-72).
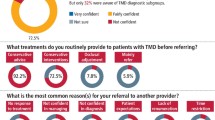
The majority, 86 patients (52.8%), were referred from their general dental practitioner (GDP), followed by general medical practitioners (39 patients; 23.9%) (Fig. 3). The remaining 38 patients were referred by various secondary care specialists including rheumatology, oral surgery and oral and maxillofacial surgery specialists (Fig. 3). Prior to referral, 50 patients (30.7%) either did not report to have seen a qualified dental professional regarding their TMD or this information was not recorded.
Patients from the areas of greatest deprivation were overrepresented (38 patients in the first IMD decile; 23.3%) compared to other deciles of deprivation (Fig. 4). The same trend was seen when assessing female and male patients separately. There was also no trend variation in the 113 patients seen by qualified dental professionals compared to the total sample, with 29 of these patients (25.7%) coming from areas with the highest deprivation level.
There was no clear trend between deprivation and the number of patients who saw a qualified dental professional before referral to the clinic, nor was there any obvious relationship between deprivation status and the total number of clinicians seen before referral. The notes of 21 patients did not precisely record the duration of symptoms; however, there was a distinct difference in the duration of symptoms with patients living in the least deprived areas having the longest median symptom duration (60 months, n = 142) (Fig. 5). No difference in symptom duration was noted between men and women (median 24 months each, n = 142).
Discussion
Socioeconomic factors such as poverty and education have a critical impact on individuals' health.19These social determinants of health might be important in the development and management of TMD, as has been shown in other chronic pain conditions.20 Despite this, the social factors of patients referred to tertiary care for TMD in the UK have not been evaluated previously.
Sex
Women are consistently reported to comprise around 60-80% of TMD patients.21,22 In our results, based in a tertiary setting, female prevalence was slightly outside this range (85.2%) and therefore, although broadly corresponding with the literature, were at the extreme end (Fig. 1). Recent prospective work analysing a large primary care population reinforces this female predisposition, finding women have over double the odds of suffering from and developing TMD.23 It has been hypothesised in other work that women may be overrepresented in cross-sectional research as they are at higher risk of developing chronic TMD, explaining the higher prevalence seen when looking at data at one time period.1,3,24 However, in our study, no difference in symptom duration was noted between sexes which suggests other factors may be contributing to the higher prevalence of women.
Previous work suggests that women are more likely to develop chronic symptoms and suffer greater levels of TMD, potentially explaining the bias.15,25 Although biological mechanisms have been suggested to explain this preference of women,26it is crucial to consider wider social factors as biopsychosocial management could help prevent chronic symptoms in other patients with similar backgrounds.10
As with TMD, women are consistently shown to suffer from higher degrees of chronic pain conditions, such as fibromyalgia and tension headaches.16 Gender roles are likely to be an important contributor to this. Although work has shown that women are more likely to report pain, when sex-specific pain thresholds are set, women show a more equal degree of pain tolerance to men, further enforcing these societal roles.27 It is feasible that this applies to TMD, but specific studies would be needed to corroborate this.
It is suggested that women access health services to a higher degree than men, which has been previously labelled 'health-seeking behaviour'.28,29 Perhaps driven by multiple factors beyond simple biological variations in health needs,29 increased health-seeking behaviour may also help explain why our tertiary clinic sample was overrepresented with women compared to the literature. To access the services of the tertiary clinic, patients must have actively sought out care and then been referred through their GDP or other providers, alongside attending the tertiary clinic appointment. All of this requires a more active role on behalf of the patient compared to sampling symptoms from a general population, which is how many prevalence estimates around TMD are made.
Age
Age distribution in TMD is also well-established in the literature with peaks in prevalence occurring around middle-age, supported by large prospective studies finding that incidence peaks around 40-50 years old before falling steadily.1,30 The results in this service evaluation correlate to this age distribution seen in the literature, with a normally distributed spread of ages peaking between 30-50 years old (Fig. 2). Together with sex, these similarities are an indication that the sample analysed in our study is consistent with the general TMD population.
Deprivation
Deprivation has repeatedly been shown to lead to higher prevalence12,31 and increased levels of pain in other chronic pain conditions.32,33 TMD may therefore be expected to be overrepresented in more deprived populations, particularly in a specialist clinic dealing with complex cases as seen in this service evaluation. However, research into deprivation among TMD patients has yielded mixed results. A multivariate analysis in Brazil also showed that a lower economic class was significantly associated with TMD pain.34 This is reinforced in an international study showing a significant association between higher TMD rates in those with lower parental education and estimated familial income, after adjusting for confounders.13 However, neither of these studies used a standard assessment of deprivation to objectively assess this.
A recent UK-based study found a significant association between greater deprivation measured with IMDs among patients referred to both a district general hospital and tertiary centre for TMD.35 Despite not exploring these results further, this aligns with the observation from this service evaluation that patients from areas of higher deprivation were more likely to attend this specialist TMD centre. However, it must be highlighted that, despite their benefits, IMDs allow for comparison of the most deprived areas versus least deprived areas; they are not suitable to make statements regarding the socioeconomic status of individuals.18
Conversely, another multicentre, US-based prospective study failed to show any significant association between TMD and income or education level.3,36 The work in question assessed symptoms within the general population, unlike this service evaluation which reviewed patients actively seeking care. It has been proposed that higher levels of deprivation might be correlated with care-seeking behaviour,37 which may partially explain the overrepresentation of patients from more deprived areas in this service evaluation. It is important to consider that the US population studied in the work cited above might not necessarily reflect the demographics seen in the group of patients included in this service evaluation. Reinforcing this point is a cross-sectional Finnish paper which also found no significant association between socioeconomic status and TMD.14 In contrast to the diverse region in which this clinic is based, the effect of deprivation on TMD is likely understated in this data as the authors highlight the 1,900 participants were recruited from an area with minimal socioeconomic variation.
Alongside potentially contributing to its onset, deprivation may also play a role in the severity of TMD. The higher proportion of patients from areas of highest deprivation (Fig. 4) seen in our results may be due to this group experiencing more severe TMD pain to necessitate specialist input. A Spanish regression analysis supports this, as it showed a significant association between lower levels of income, occupation and education with severity of TMD pain.8
Another way in which deprivation may be linked to TMD is the effect on patients' ability to effectively move through the healthcare system. Barriers to dental care, exacerbated by deprivation,38 may impede the ability of patients to receive TMD treatment in the community and prolong their symptoms leading to chronic pain symptoms. However, this trend was not seen in this service evaluation (Fig. 5). This might be explained by the availability of free dental care for those who are most financially vulnerable in England, contributing to more equitable treatment. Nonetheless, data regarding duration of symptoms was not able to be included for analysis for 21 patients as the notes had not recorded this precisely, highlighting a need for improved record keeping.
Limitations and future work
The nature of this service evaluation prevents determination of causal links and wider generalisability. To assess if deprivation is to be causally linked with TMD in the UK, prospective cross-sectional research studies are needed. This type of work could also identify if referring clinicians are aware of the trends observed in this study when considering specialist input, which would aid interpretation of these findings.
TMD is a broad term, encompassing multiple pathologies.39 Due to the small sample size, it was not possible to assess trends within the different subcategories of TMD. Prospective work with larger sample sizes could group patients by their suspected aetiology to reduce the risk of confounders. Our sample contained a mixture of patients referred by medical and dental professionals. Although no variation in deprivation trend was seen, research with large sample sizes could separate these more distinctly and identify any causal links.
This service evaluation was conducted in one tertiary referral centre in the UK which treats TMD patients requiring specialist input and may not be representative of the general population. Nonetheless, these are unique points of this work in a group that has not been investigated in this manner before, providing a foundation for future research.
Collecting data retrospectively meant that there was no control over what was documented. Although age, sex and deprivation were assessed, important demographic factors such as income were often omitted. It is understandable that not all patients will be able to provide a precise time of onset for their symptoms; however, this highlights a need for improved record keeping.
An objective measure to diagnose TMD was not used due to demands of the clinic from which the study drew from; however, diagnoses were made were made with expert judgement by a consultant oral surgeon. The Diagnostic Criteria for Temporomandibular Disorders (DC/TMD) is the current gold standard,39yet its length poses a challenge in busy NHS clinics where clinical pressure must be balanced. A pragmatic approach was taken where a careful history was obtained followed by relevant examinations. Other causes of facial pain were excluded and patients were assessed holistically to identify any other factors that may be relevant. Once TMD was diagnosed, pathology was localised to the musculature, joints, or a combination of both to ensure the most specific diagnosis was made as possible. A suitable alternative for objective diagnoses developed alongside the DC/TMD that could be used in absence of specialist experience is a quick three-item and six-item screening tool with 97% specificity and 99% sensitivity for TMD.40
Conclusion
This service evaluation highlights sociodemographic contributors to TMD in UK patients referred to a tertiary care clinic. It is clear that TMD is in part driven by a complex interaction of multiple social factors and is linked to demographics like age and sex. Research and greater understanding of these factors might further aid dentists and other healthcare professionals with TMD management, setting appropriate goals for treatment and creating realistic expectations for patients. Furthermore, the exact link between deprivation and TMD is still uncertain and well-designed, prospective research studies with consistent methodologies are needed. Greater understanding of TMD risk factors may also aid prevention and reduce the burden of TMD in patients at risk.
References
Slade G D, Bair E, Greenspan J D et al. Signs and symptoms of first-onset TMD and sociodemographic predictors of its development: The OPPERA prospective cohort study. J Pain 2013; DOI: 10.1016/j.jpain.2013.07.014.
Murphy M K, MacBarb R F, Wong M E, Athanasiou K A. Temporomandibular Disorders: A Review of Etiology, Clinical Management, and Tissue Engineering Strategies. Int J Oral Maxillofac Implants 2013; DOI: 10.11607/jomi.te20.
Slade G D, Ohrbach R, Greenspan J D et al. Painful Temporomandibular Disorder: Decade of Discovery from OPPERA Studies. J Dent Res 2016; 95: 1084-1092.
Osiewicz M, Lobbezoo F, Ciapała B, Pytko-Polończyk J, Manfredini D. Pain Predictors in a Population of Temporomandibular Disorders Patients. J Clin Med 2020; 9: 452.
Durham J. Oral surgery: Part 3. Temporomandibular disorders. Br Dent J 2013; 215: 331-337.
Manfredini D, Lobbezoo F. Relationship between bruxism and temporomandibular disorders: A systematic review of literature from 1998 to 2008. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2010; DOI: 10.1016/j.tripleo.2010.02.013.
Jiménez-Silva A, Peña-Durán C, Tobar-Reyes J, Frugone-Zambra R. Sleep and awake bruxism in adults and its relationship with temporomandibular disorders: A systematic review from 2003 to 2014. Acta Odontol Scand 2017; 75: 36-58.
Blanco-Hungría A, Rodríguez-Torronteras A, Blanco-Aguilera A et al. Influence of sociodemographic factors upon pain intensity in patients with temporomandibular joint disorders seen in the primary care setting. Med Oral Patol Oral Cir Bucal 2012; DOI: 10.4317/medoral.17576.
Danilov A, Danilov A, Barulin A, Kurushina O, Latysheva N. Interdisciplinary approach to chronic pain management. Postgrad Med 2020; 132: 5-9.
Ahmed N, Poate T, Nacher-Garcia C et al. Temporomandibular joint multidisciplinary team clinic. Br J Oral Maxillofac Surg 2014; 52: 827-830.
Plesh O, Adams S H, Gansky S A. Temporomandibular joint and muscle disorder-type pain and comorbid pains in a national US sample. J Orofac Pain 2011; 25: 190-198.
Janevic M R, McLaughlin S J, Heapy A A, Thacker C, Piette J D. Racial and Socioeconomic Disparities in Disabling Chronic Pain: Findings from the Health and Retirement Study. J Pain 2017; 18: 1459-1467.
Hongxing L, Astrøm A N, List T, Nilsson I-M, Johansson A. Prevalence of temporomandibular disorder pain in Chinese adolescents compared to an age-matched Swedish population. J Oral Rehabil 2016; 43: 241-248.
Jussila P, Knuutila J, Salmela S et al. Association of risk factors with temporomandibular disorders in the Northern Finland Birth Cohort 1966. Acta Odontol Scand 2018; 76: 525-529.
Schmid-Schwap M, Bristela M, Kundi M, Piehslinger E. Sex-Specific Differences in Patients with Temporomandibular Disorders. J Orofac Pain 2013; 27: 42-50.
Fillingim R B, King C D, Ribeiro-Dasilva M C, Rahim-Williams B, Riley J L. Sex, Gender, and Pain: A Review of Recent Clinical and Experimental Findings. J Pain 2009; 10: 447-485.
Ministry of Housing, Communities and Local Government. English indices of deprivation 2019. Postcode Lookup. 2019. Available at https://imd-by-postcode.opendatacommunities.org/imd/2019 (accessed June 2020).
Ministry of Housing, Communities and Local Government. The English Indices of Deprivation 2019 Frequently Asked Questions (FAQs). 2019. Available at https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/853811/IoD2019_FAQ_v4.pdf (accessed September 2020).
Frieden T R. A framework for public health action: The health impact pyramid. Am J Public Health 2010; 100: 590-595.
Darnall B D, Carr D B, Schatman M E. Pain psychology and the Biopsychosocial Model of Pain Treatment: Ethical Imperatives and Social Responsibility. Pain Med 2017; 18: 1413-1415.
Gesch D, Bernhardt O, Alte D et al. Prevalence of signs and symptoms of temporomandibular disorders in an urban and rural German population: results of a population-based Study of Health in Pomerania. Quintessence Int 2004; 35: 143-150.
Ferreira C L P, da Silva M A M R, de Felício C M. Signs and symptoms of temporomandibular disorders in women and men. Codas 2016; 28: 17-21.
Häggman-Henrikson B, Liv P, Ilgunas A et al. Increasing gender differences in the prevalence and chronification of orofacial pain in the population. Pain 2020; 161: 1768-1775.
Garofalo J P, Gatchel R J, Wesley A L, Ellis E. Predicting chronicity in acute temporomandibular joint disorders using the research diagnostic criteria. J Am Dent Assoc 1998; 129: 438-447.
Kim T Y, Shin J S, Lee J et al. Gender difference in associations between chronic temporomandibular disorders and general quality of life in Koreans: A cross-sectional study. PLoS One 2015; DOI: 10.1371/journal.pone.0145002.
Ribeiro-Dasilva M C, Line S R P, dos Santos M C L G et al. Oestrogen Receptor-α Polymorphisms and Predisposition to TMJ Disorder. J Pain 2009; 10: 527-533.
Robinson M E, Gagnon C M, Riley J L, Price D D. Altering gender role expectations: Effects on pain tolerance, pain threshold, and pain ratings. J Pain 2003; 4: 284-288.
Thompson A E, Anisimowicz Y, Mioedema B, Hogg W, Wodchis W P, Aubrey-Bassler K. The influence of gender and other patient characteristics on health care-seeking behaviour: A QUALICOPC study. BMC Fam Pract 2016; 17: 1-7.
Lim M T, Fong Lim Y M, Tong S F, Sivasampu S. Age, sex and primary care setting differences in patients' perception of community healthcare seeking behaviour towards health services. PLoS One 2019; DOI: 10.1371/journal.pone.0224260.
Von Korff M, Le Resche L, Dworkin S F. First onset of common pain symptoms: a prospective study of depression as a risk factor. Pain 1993; 55: 251-258.
Collin S M, Bakken I J, Nazareth I, Crawley E, White P D. Trends in the incidence of chronic fatigue syndrome and fibromyalgia in the UK, 2001-2013: a Clinical Practice Research Datalink study. J R Soc Med 2017; 110: 231-244.
Jordan K P, Thomas E, Peat G, Wilkie R, Croft P. Social risks for disabling pain in older people: A prospective study of individual and area characteristics. Pain 2008; 137: 652-661.
Brekke M, Hjortdahl P, Kvien T K. Severity of musculoskeletal pain: Relations to socioeconomic inequality. Soc Sci Med 2002; 54: 221-228.
Magalhães B-G, de-Sousa S-T, de Mello V-V-C et al. Risk factors for temporomandibular disorder: Binary logistic regression analysis. Med Oral Patol Oral Cir Bucal 2014; DOI: 10.4317/medoral.19434.
Hamad R, Clark A S, Pretty I A. The current referral patterns for temporomandibular joint disorders (TMD) in Greater Manchester. Community Dent Health 2020; 37: 242-246.
Maixner W, Diatchenko L, Dubner R et al. Orofacial pain prospective evaluation and risk assessment study - the OPPERA study. J Pain 2011; DOI: 10.1016/j.jpain.2011.08.002.
Willems S, Peersman W, De Maeyer P, Buylaert W, De Maeseneer J, De Paepe P. The impact of neighborhood deprivation on patients' unscheduled outofhours healthcare seeking behaviour: A cross-sectional study. BMC Fam Pract 2013; 14: 136.
QualityWatch. Root Causes: quality and inequality in dental health. 2017. Available at https://www.nuffieldtrust.org.uk/files/2018-10/1540139783_qualitywatch-root-causes-dental-health-report.pdf (accessed July 2020).
Schiffman E, Ohrbach R, Truelove E et al. Diagnostic Criteria for Temporomandibular Disorders (DC/TMD) for Clinical and Research Applications: recommendations of the International RDC/TMD Consortium Network* and Orofacial Pain Special Interest Group†. J Oral Facial Pain Headache 2014; 28: 6-27.
Gonzales Y M, Schiffman E, Gordon S M et al. Development of a brief and effective temporomandibular disorder pain screening questionnaire. J Am Dent Assoc 2011; 142: 1183-1191.
Author information
Authors and Affiliations
Contributions
Daniel Camfield, Claire LesleyWilson and Alison Loescher contributed to the design of the service evaluation, the analysis of results and the writing of the manuscript.
Corresponding author
Ethics declarations
The authors declare no conflicts of interest.
Rights and permissions
Open Access. This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0.© The Author(s) 2022
About this article
Cite this article
Camfield, D., Wilson, C. & Loescher, A. Sociodemographic trends in a UK temporomandibular joint disorder clinic. Br Dent J (2022). https://doi.org/10.1038/s41415-022-3932-4
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41415-022-3932-4