Abstract
Objectives To evaluate the oral health status and knowledge of only children (OC) and non-only children (NOC), and to explore potential reasons for the differences.
Materials and methods This cross-sectional sampling survey included 3,731 children between the ages of 12 and 15 years. The oral health of the subjects was examined, according to the Basic Methods of Oral Health Survey (fifth edition) recommended by the World Health Organisation, and their eating habits, oral health knowledge and oral habits were recorded. EpiData software was used to input data, and SPSS version 19.0 software was used for analysis and comparison.
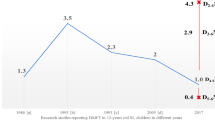
Results The incidence of dental caries and the decayed, missing and filled teeth index (DMFT) in OC (53.2% and 1.53, respectively) were significantly lower than those in NOC (56.2% and 1.86, respectively) (P <0.05). These values were highest in female NOC (63.7%). Gingival bleeding in NOC (78.9%) was significantly higher than that in OC (74.1%) and the difference was statistically significant (P <0.05). The pit and fissure sealant rate of the OC (17.9%) was better than that of the NOC (11.0%), and the difference was statistically significant (P <0.05). There were no significant differences in the oral health attitudes between the two groups, while the scores of the OC were higher than that of the NOC on eight questions of oral health knowledge and awareness, with statistically significant differences for five of the questions (P <0.05). In terms of oral behavioural habits and related factors, the OC scored better than the NOC.
Conclusions Our results show that the oral health status of NOC, especially female children, is worrying. When formulating health-related policies, it is necessary to consider these inequalities in adolescents and to provide more resources to the relatively vulnerable adolescents.
Key points
-
The oral health of non-only children is worse than that of only children in China.
-
More attention should be paid to the oral health of non-only children after the implementation of the Universal Two-Child policy in China.
-
Increasing the acquisition of oral health knowledge is one of the effective ways to improve the oral health of non-only children.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 24 print issues and online access
$259.00 per year
only $10.79 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout








Similar content being viewed by others
References
Greenhalgh S, Bongaarts J. Fertility policy in China: future options. Science 1987; 235: 1167-1172.
Hesketh T, Zhou X, Wang Y. The End of the One-Child Policy: Lasting Implications for China. JAMA 2015; 314: 2619-2620.
Spruijt E, de Goede M. Transitions in family structure and adolescent well-being. Adolescence 1997; 32: 897-911.
Heddini A, Cars O, Qiang S, Tomson G. Antibiotic resistance in China-a major future challenge. Lancet 2009; 373: 30.
Cameron L, Erkal N, Gangadharan L, Meng X. Little emperors: behavioural impacts of China's One-Child Policy. Science 2013; 339: 953-957.
Peng Z, Zheng Z, Han H et al. Imbalance in obesity and mental health among "little emperors" in China. PLoS One 2019; DOI: 10.1371/journal.pone.0207129.
Han Y W, Wang X. Mobile microbiome: oral bacteria in extra-oral infections and inflammation. J Dent Res 2013; 92: 485-491.
Lockhart P B, Brennan M T, Sasser H C, Fox P C, Paster B J, Bahrani-Mougeot F K. Bacteraemia associated with toothbrushing and dental extraction. Circulation 2008; 117: 3118-3125.
Marques da Silva R, Caugant D A, Josefsen R, Tronstad L, Olsen I. Characterization of Streptococcus constellatus strains recovered from a brain abscess and periodontal pockets in an immunocompromised patient. J Periodontol 2004; 75: 1720-1723.
Ohlrich E J, Cullinan M P, Leichter J W. Diabetes, periodontitis, and the subgingival microbiota. J Oral Microbiol 2010; DOI: 10.3402/jom.v2i0.5818.
Peres K G, Nascimento G G, Peres M A et al. Impact of Prolonged Breastfeeding on Dental Caries: A Population-Based Birth Cohort Study. Pediatrics 2017; DOI: 10.1542/peds.2016-2943.
Hu J, Jiang W, Lin X et al. Dental Caries Status and Caries Risk Factors in Students Ages 12-14 Years in Zhejiang, China. Med Sci Monit 2018; 24: 3670-3678.
Llena C, Calabuig E. Risk factors associated with new caries lesions in permanent first molars in children: a 5-year historical cohort follow-up study. Clin Oral Investig 2018; 22: 1579-1586.
World Health Organisation. Oral Health Surveys: Basic Methods. 5th ed. Geneva: World Health Organisation, 2013.
Li S, Chen R, Cao Y, Li J, Zuo D, Yan H. Sexual knowledge, attitudes and practices of female undergraduate students in Wuhan, China: the only-child versus students with siblings. PLoS One 2013; DOI: 10.1371/journal.pone.0073797.
Nowicki D, Vogel R I, Melcer S, Deasy M J. The gingival bleeding time index. J Periodontol 1981; 52: 260-262.
Crocombe L A, Allen P, Bettiol S, Babo Soares L F. Parental Education Level and Dental Caries in School Children Living in Dili, Timor-Leste. Asia Pac J Public Health 2018; 30: 128-136.
Wang Y, Fong V L. Little emperors and the 4:2:1 generation: China's singletons. J Am Acad Child Adolesc Psychiatry 2009; 48: 1137-1139.
Ekstrand K R, Christiansen J, Christiansen M E. Time and duration of eruption of first and second permanent molars: a longitudinal investigation. Community Dent Oral Epidemiol 2003; 31: 344-350.
Kucukyilmaz E, Savas S. Evaluation of Different Fissure Sealant Materials and Flowable Composites Used as Pit-and-fissure Sealants: A 24-Month Clinical Trial. Pediatr Dent 2015; 37: 468-473.
Yang J, Hou X, Wei D, Wang K, Li Y, Qiu J. Only-child and non-only-child exhibit differences in creativity and agreeableness: evidence from behavioural and anatomical structural studies. Brain Imaging Behav 2017; 11: 493-502.
Maltby J, Paterson K, Day L, Jones C, Kinnear H, Buchanan H. Social ranking effects on tooth-brushing behaviour. Br J Health Psychol 2016; 21: 374-388.
Walsh T, Worthington H V, Glenny A M, Marinho V C, Jeroncic A. Fluoride toothpastes of different concentrations for preventing dental caries. Cochrane Database Syst Rev 2019; DOI: 10.1002/14651858.CD007868.pub3.
Pollick H. The Role of Fluoride in the Prevention of Tooth Decay. Pediatr Clin North Am 2018; 65: 923-940.
Cury J A, Tenuta L M. Evidence-based recommendation on toothpaste use. Braz Oral Res 2014; DOI: 10.1590/S1806-83242014.50000001.
Funding
This survey was funded by a grant from the Scientific Research Fund of the National Health Commission of the People's Republic of China (201502002) and conducted by the Department of Preventive Dentistry, Hospital of Stomatology, China Medical University, China.
Author information
Authors and Affiliations
Contributions
Professor Zhenfu Lu acquired the funding for the project and played a role in the design of the study. Dr Kaiqiang Zhang was involved in drafting and revising the manuscript. Dr Jian Li participated in the collection and analysis of the data. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
The authors of this article declare that they have no competing interests. Ethical approval: all procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. Informed consent: informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Zhang, K., Li, J. & Lu, Z. Oral health status and knowledge of only and non-only children in China. Br Dent J (2021). https://doi.org/10.1038/s41415-021-3477-y
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41415-021-3477-y