Abstract
Introduction Mandibular replacement appliances (MRAs) can be used in the treatment of snoring, mild to moderate obstructive sleep apnoea and as a second-line treatment where continuous positive airway pressure (CPAP) fails. There is currently a paucity of evidence as to how long these appliances last.
Aims Assess the replacement rate for MRAs using this as a proxy for lifespan; estimate the period prevalence of temporomandibular joint disorder (TMJD) and bruxism in the study population.
Methods Prospective observational study as part of service evaluation. Data from consecutive patients seeking a replacement MRA were collected over a three-month period, yielding a sample of 60. The mean time between the provision of appliances was calculated in months. Reasons for replacement were sought, collated and categorised. Patients were asked to report any TMJD symptoms and bruxing.
Results The mean replacement rate was 36.7 months. The main reasons for replacement were: device condition; fit and reduced effectiveness; and other minor reasons reported. Period prevalence of TMJD was 6.7%; bruxism was reported in 5% of patients.
Conclusions A 'lifespan' of ust over three years for thermoplastic MRAs is estimated. The main reasons for replacement were: condition, poor fit and reduced effectiveness. MRAs do not appear to increase the frequency of TMJD and bruxism.
Similar content being viewed by others
Key points
-
Provides the first known estimate of thermoplastic mandibular repositioning appliance 'lifespan' and sets a benchmark for this.
-
Suggests patients can expect on average, 3 years between replacement of a thermoplastic mandibular repositioning appliance.
-
Collates the most common reasons for appliance replacement.
-
Indicates that these appliances do not seem to increase the frequency of TMJ issues or bruxism beyond comparable patient populations.
Introduction
Sleep disordered breathing (SDB) has many forms and causes. In its obstructive form it covers a spectrum of respiratory function from uninhibited breathing, through snoring, to frank choking episodes. Obstructive sleep apnoea/hypopnoea syndrome (OSAHS) occurs during sleep when there is a partial (hypopnoea) or complete (apnoea) blockage in the airway of a sufferer. OSAHS is estimated to affect 3-7% of males and 2-5% of females.1
Sleep arousal may be below the threshold of consciousness and can lead to uncontrolled daytime sleepiness, poor concentration, diminished cognitive function, mood changes, reduced quality of life and relationship problems.2 There are associations between OSAHS and vascular conditions, with sufferers showing significant improvement in blood pressure when optimal treatment is carried out.3 Males with severe OSAHS have approximately a threefold increase in risk from fatal or non-fatal vascular incidents.4 However, a causal link with vascular incidents such as myocardial infarction and stroke still awaits clarification.
Direct management aims to maintain upper airway patency. Mandibular repositioning appliances (MRAs) aim to achieve this, mainly at the oropharyngeal level, by positioning the mandible and tongue forwards The use of continuous positive airway pressure (CPAP), which uses air to maintain patency, is the first line or 'gold standard' treatment.5 MRAs are used where patients experience symptom-free snoring and/or mild to moderate OSAHS. In more severe OSAHS cases they are an adequate second line treatment where CPAP is not tolerated.6 Management is anticipated to be lifelong.
The orthodontic department at the Victoria Hospital, Kirkcaldy provides a Scotland-wide service for the provision of mandibular repositioning devices (MRAs). These are provided strictly on referral, with a medical diagnosis and management plan for disruptive snoring and/or OSAHS. It is imperative that appropriate diagnosis and planning is made by a suitably qualified medical practitioner before MRA provision. It is possible for MRAs to reduce overt snoring symptoms but mask the signs of obstructive sleep apnoea/hypopnoea syndrome.
'How long will this appliance last?' is a common question. Commercial manufacturers give various estimates from three to 24 months for off-the-shelf devices, to an eight-year warranty for a custom-made metal device.7 NHS online previously indicated an 18-month lifespan but gave no reference to any related evidence or material/design type.8 This now appears to have been withdrawn and there would seem to be a paucity of published evidence directly addressing this issue.8,9
The issue of side effects with particular regard to temporomandibular joint dysfunction (TMJD), in all its guises, and bruxism, are of concern due to the mode of action of an MRA. Studies report a wide range of detectable TMJD frequency in the general population (20-75%).10 The estimates for those under treatment for OSAHS with an appliance vary: 0-5.5%, to 37%.11,12 These wide ranges may be explained by the relative sensitivities of the diagnostic techniques employed, particularly for research purposes. The percentage frequency for bruxism has rather more concordant estimates: 8% and 12.8% during sleep.13,14 Changes to the occlusal relationship of the dentition have been estimated over longer periods (mean 7.4 years) but there was no mention as to whether patients had considered these changes to be unfavourable.15
Aims and objectives
Estimate the replacement rate of MRAs using this as a proxy for 'lifespan' and record the most common reasons for replacement in order to: set initial benchmarks; assess service demand and variables which may increase frequency of replacement; and aid patient communication. Another objective was to assess the level of TMJD and bruxism in the study population.
Sample
Sample frame: all patients attending MRA clinics from the start of April 2016 to the end of June 2016 were potential candidates for inclusion. Subsequently, those who were medically (re)referred for a replacement MRA were included for audit. This yielded a sample of 60 patients with 76 replacement appliances, all made within the departmental laboratory. There were no exclusions.
Methods
Prospective observational study as part of service evaluation. Data were collected from all patients to have replacement MRAs at time of attendance:
Time between replacements in months
Demographic data: age, gender
Medical diagnosis of OSAHS versus snoring only
Reasons for replacement in patient's own words, these were collated with similar descriptors then categorised
Self-reported current appliance effectiveness
Appliance design
Self-reported temporomandibular joint dysfunction with palpation, where appropriate
Self-reported bruxism.
Data were entered into a Microsoft Excel worksheet and descriptive statistics were generated.
Results
Sixty patients were (re)referred in the time period for replacement appliances. This equates to 20 returners per month. Fourteen had records available to record multiple attendances, thus the total number of appliances was 76. The mean replacement rate was 36.7 months (range: 4-216). Demographic data indicated a male to female ratio of 2:1; mean male age of 54.1, range 29-79; mean female age of 53.6, range 34-73. Exactly half the attendees had a medical diagnosis of OSAHS with almost no difference in replacement rate versus snorers (Table 1).
From the patient descriptions of their current MRA, eight categories were generated to highlight the reasons for replacement (Table 2). Of the 14 patients who had previous replacements, half reported the same reason. The maximum number of replacements recorded for a single patient was three. MRAs were reported as still being effective in 54% of the sample.
The majority of appliances for replacement (91% n = 69) were of a thermoplastic monobloc design. Seven patients had different materials or designs with one patient replacing an ineffective over-the-counter chin-strap device. All were replaced with a custom-made thermoplastic monobloc MRA (ctmMRA), with one exception which utilised a Herbst style CoCr design (this was eventually replaced with a ctmMRA).
The period prevalence of self-reported TMJD was 6.7% (n = 4); two patients reported a pre-existing TMJD condition and two had a diagnosis of OSAHS. The period prevalence of self-reported bruxism was 5% (n = 3).
Discussion
The demographics of the returning patients demonstrated a higher male ratio, approximately in line with epidemiological estimates of OHSAS sufferers.1To determine the actual lifespan of these appliances is possible but would require intra-oral telemetry. The presumption that MRAs are worn every night is erroneous but how much value telemetry would provide to service provision or patient experience is debatable. It is contended that a mean three-year replacement rate is entirely reasonable given the materials used, and is a pragmatic proxy for lifespan.
The most common reasons for seeking a replacement are related to patients' perceptions of the appliance condition, followed by its fit. The ctmMRA is made from polyvinyl acetate-ethylene and is susceptible to staining, abrasion from teeth and brushes/dentifrice. Warping over time reduces the close fit of the appliance; in turn this adversely affects retention. There is, however, no material currently available which provides the balance of longevity, comfort and ease of use and manufacture. For a small minority of patients, the condition of the appliance did not seem to be an issue and only loss triggered a replacement request.
Paradoxically, just over half the returning patients reported that their MRA was still working; other drivers for replacement such as the condition of the device are perceived as almost equally important in triggering a replacement request. Treatment was not refused on the grounds that the current device was still effective. Patients were encouraged to use all devices either until ineffective and/or as a spare, with the expectation that this would extend time between attendances.
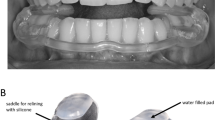
There was insufficient data to allow comparison between differing designs and materials for MRAs. Anyone seeking such a device will find a myriad of appliance designs purporting to be of help (Fig 1 and Fig 2). Currently the most effective material and design combination would appear to be the custom-made thermoplastic monobloc.16 In terms of patient preference, in a crossover randomised clinical trial, almost all patients reverted to a monobloc design versus a Herbst-style articulated appliance.17 A recent review confirms the lack of 'robust' evidence between appliance designs.18
TMJD is susceptible to the effects of definition and diagnostic techniques. Durham, for example, reports rates of detection of up to 75%, but that only 2-4% of patients attend for treatment.11 In this population we would be unable to justify additional diagnostic measures such as radiographs on the basis of screening out putative but asymptomatic TMJD. The levels of reported TMJD and bruxism in this study appear to be comparable with published estimates in analogous populations: TMJD ~ 19% prevalence at baseline, reducing to 8.4% at 1.13 years after initiating device wear; 3.5% mean annual incidence.19,20 Bruxing prevalence is estimated at 8% (self-reported).13 MRAs do not raise the frequency of TMJD in the SDB population and do not seem to in this study population.19 TMJD is associated more with the severity of OHSAS and other factors.20 Bruxism did not coexist with TMJD in any patient in this study. Both TMJD and bruxism were associated with a drop-off in mean time between replacements: 27 and 27.3 months, respectively, versus mean, however the numbers involved here may be too few to draw definitive conclusions.
Differences in occlusal relationships were not considered, as there were too many potential confounding factors to derive valid results. Potential confounders are: amount of actual versus reported usage; magnitude of protrusion; magnitude of opening; design type/material; age of patient; and starting occlusal relationships. Further research in this area would need to control for these and indicate whether this was of material concern to patients, and to what degree. It was not within the remit of this evaluation to explore MRA efficacy.
Conclusions
This audit sets a three-year replacement 'lifespan' as the baseline figure with which to benchmark future studies and is not considered to be overly burdensome on service demand. It is a figure which can be clearly communicated to patients, providing a realistic and practical expected mean average interval between replacement MRAs. The most common reasons for replacement were the perceived condition of the appliance, poor fit, and diminished effectiveness. Custom-made thermoplastic monobloc MRAs do not appear to be associated with an increase in self-reported TMJD or bruxism in this study population when compared to general or analogous population estimates. Studies to compare the longevity of various MRA designs and materials are needed, where numbers permit.
References
Punjabi N M. The epidemiology of adult obstructive sleep apnea. Proc Am Thorac Soc 2008; 5: 136-143.
Scottish Intercollegiate Guidelines Network. Management of obstructive sleep apnoea/hypopnoea syndrome in adults. 2015.
Robinson G, Stradling J, Davies R. Sleep 6: obstructive sleep apnoea/hypopnoea syndrome and hypertension. Thorax 2004; 59: 1089-1094.
Marin J M, Carrizo S J, Vicente E, Agusti A G. Long-term cardiovascular outcomes in men with obstructive sleep apnoea-hypopnoea with or without treatment with continuous positive airway pressure: an observational study. Lancet 2005; 365: 1046-1053.
Lim J, Lasserson T J, Fleetham J, Wright J. Oral appliances for obstructive sleep apnoea. Cochrane Database Syst Rev 2006; CD004435. DOI: 10.1002/14651858.CD004435.pub3.
National Institute for Health and Care Excellence. Obstructive sleep apnoea syndrome: Scenario: management of sleep apnoea. 2015. Available at https://cks.nice.org.uk/obstructive-sleep-apnoea-syndrome#!scenario (accessed August 2019).
British Snoring & Sleep Apnoea Asssociation. Somnowell. Available at https://britishsnoring.co.uk/shop/mandibular_advancement_devices/somnowell.php (accessed August 2019).
NHS. Conditions: Snoring. 2017. Available at https://www.nhs.uk/conditions/snoring/ (accessed August 2019).
NHS. Conditions: Sleep Apnoea. 2019. Available at https://www.nhs.uk/conditions/sleep-apnoea/ (accessed August 2019).
Durham J. Oral surgery: part 3. Temporomandibular disorders. Br Dent J 2013; 215: 331-337.
Ferguson K A, Cartwright R, Rogers R, Schmidt-Nowara W. Oral appliances for snoring and obstructive sleep apnea: a review. Sleep 2006; 29: 244-262.
Hoffstein V. Review of oral appliances for treatment of sleep-disordered breathing. Sleep Breath 2007; 11: 1-22.
Balasubramaniam R, Klasser G D, Cistulli P A, Lavigne G J. The link between sleep bruxism, sleep disordered breathing and temporomandibular disorders: an evidence-based review. J Dent Sleep Med 2014; 1: 27-37.
Manfredini D, Winocur E, Guarda-Nardini L, Paesani D, Lobbezoo F. Epidemiology of bruxism in adults: a systematic review of the literature. J Orofac Pain 2013; 27: 99-110.
de Almeida F R, Lowe A A, Otsuka R, Fastlicht S, Farbood M, Tsuiki S. Long-term sequellae of oral appliance therapy in obstructive sleep apnea patients: Part 2. Study-model analysis. Am J Orthod Dentofacial Orthop 2006; 129: 205-213.
Quinnell T G, Bennett M, Jordan J et al. A crossover randomised controlled trial of oral mandibular advancement devices for obstructive sleep apnoea-hypopnoea (TOMADO). Thorax 2014; 69: 938-945.
Bloch K E, Iseli A, Zhang J N et al. A randomized, controlled crossover trial of two oral appliances for sleep apnea treatment. Am J Respir Crit Care Med 2000; 162: 246-251.
Basyuni, S, Barabas, M, Quinnell T. An update on mandibular advancement devices for the treatment of obstructive sleep apnoea hypopnoea syndrome. J Thorac Dis 2018; 10 (Spec Iss): S48-S56.
Perez C V, de Leeuw R, Okeson J P et al. The incidence and prevalence of temporomandibular disorders and posterior open bite in patients receiving mandibular advancement device therapy for obstructive sleep apnea. Sleep Breath 2013; 17: 323-332.
Sanders A E, Essick G K, Fillingim R et al. Sleep apnea symptoms and risk of temporomandibular disorder: OPPERA cohort. J Dent Res 2013; 92 (Spec Iss): S70-S77.
Acknowledgements
The authors gratefully acknowledge James Harrison (Lead Technician) and Lesley Spears (Clinical Photographer) for their assistance with the appliance images.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ho-A-Yun, J., Sharma, P. The 'lifespan' of mandibular repositioning appliances. Br Dent J 227, 470–473 (2019). https://doi.org/10.1038/s41415-019-0730-8
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41415-019-0730-8