Abstract
Aim The study aimed to test the effectiveness and acceptability of a smartphone application used in conjunction with a movement sensor toothbrushing attachment for promoting plaque control.
Method One hundred and eight dental practice patients were recruited to the study from two general dental practices. Participants were randomised to test and control groups, and both groups offered oral hygiene instruction according to a single protocol. Test participants were given the smartphone device and toothbrush attachment. Control patients were not. After two and four weeks, full mouth plaque scores of the mouths of both test and control participants were measured. A comprehensive questionnaire administered to the test group assessed participants' views about the acceptability of the smartphone device and application.
Results Full mouth plaque scores declined from 40.1 to 11.7, a reduction of 70% in the test group compared to a reduction from 29.1 to 20.5 (30%) in the control group. The device was found to be very well accepted. Participants were conscious of improving their brushing and improving their knowledge of how to brush well. They also reported enjoyment and fun being derived from use of the device and found it simple to use.
Conclusion Providing immediate day-to-day feedback to dental patients about their brushing results in dramatic improvements in oral hygiene and highly significant reductions in plaque levels, in at least the short-term; beyond that seen in previous toothbrushing interventions with adult patients.
Similar content being viewed by others
Listen to the author talk about the key findings in this paper in the associated video abstract. Available in the supplementary information online
Key points
-
This application was twice as effective for reducing plaque levels as any previous intervention tested by RCT.
-
Patients enjoy and are interested and motivated by the information that the application gives them.
-
The application is potentially a groundbreaking evaluation tool for use in oral health promotion research.
Introduction
Effective twice daily toothbrushing with a fluoride toothpaste is accepted as the primary method for preventing tooth loss1,2 due to the protective effect of removing plaque on the progression of periodontal disease3,4 and the anti-caries effect of applying fluoride topically to the tooth surfaces.5,6 In addition, brushing one's teeth gives an individual conformity to the social norm of personal hygiene.7 Twice daily toothbrushing is universally recommended in the UK and has been advocated by the dental professional bodies for more than 50 years.8,9,10 Evidence shows also that the vast majority of the population claim to brush their teeth at least on a daily basis, and yet, only a decade ago, 33% of the population still had some signs of periodontal disease, a cardinal sign of the presence of plaque.10 It is, therefore, apparent that the toothbrushing which is being carried out is often ineffective or incomplete.
Bandura11 showed in the 1970s that a person's sense of self-efficacy, in other words their belief in their own ability to do something well, predicts how well they actually perform, and this theory has been shown to be relevant to oral health-related behaviours.12,13 Thus, the more a person receives feedback that they are performing well, the more likely they are to perform well in the future due to their developing sense of 'mastery'. Thus, the efficacy and effectiveness of task completion improves, and continues to improve, or be sustained at a high level of proficiency.
The means of developing this mastery has been the topic of psychological research for very many years. In the past two decades, the technique of motivational interviewing, autonomy support, and a 'strengths-based' approach have been noted as the most acceptable way to change health-related behaviours,14,15,16 as these techniques do not alienate or 'victim blame' the subject of an intervention. It has been repeatedly shown in reviews of oral health promotion that application of key behavioural change theories is a cornerstone of success.10
In order to bring about positive behaviour changes related to health, and to address widespread public health issues, interventions are required which are inexpensive, effective in promoting self-efficacy and most importantly, acceptable to the recipients and fit with social norms. This study, therefore, aimed to test the effectiveness and acceptability of a smartphone application and movement sensor toothbrushing attachment for promoting plaque control.
Materials and method
All patients involved in the study were given written information sheets and verbal reassurance to assure them that joining the study, or not, would not affect their normal treatment in any way. It also gave them the opportunity to ask questions before giving written, informed consent to join the study. The study was approved by the South West Frenchay research ethics committee.
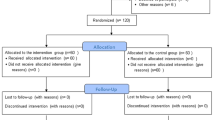
Patients were randomised into the test and control groups at each of the dental practices. Test and control participants were examined at baseline and given standard oral hygiene instructions and a 'goody bag'. Half of these contained Brushlink devices and half did not. The allocation of devices was carried out using random number allocation at each of the practices. If the bag a patient was given contained the Brushlink device (Fig. 1), the smartphone application and instructions for its use were given to the patient as well as the normal hygiene instructions. If there was no Brushlink device in the goody bag, normal oral hygiene instructions alone were given. The oral hygiene protocol, for both test and control patients, consisted of advice on brushing twice a day with a manual or electric toothbrush for two minutes with fluoride toothpaste. Advice about and a demonstration of the correct angulation of the brush head against the gum line (45°) was given and the importance of ensuring the cleanliness of each individual tooth was stressed. Advice about cleaning with interdental brushes and floss was also given where appropriate.
All participants were given appointments for oral hygiene assessments at two and four weeks after joining the trial. Before patient examination, a pre-trial calibration session was performed by two examiners on five healthy volunteer patients. The number of teeth present in the oral cavity and FMPS (full mouth plaque scores) were recorded twice a day to obtain acceptable intra-and inter-examiner parameter assessment reproducibility. The use of FMPS, which are routinely used in dental practice and the use of specific periodontal probes UNC15, along with the calibration session ensured an acceptable level of examiner agreement. The presence of plaque (present/not present) was recorded for the mesial, buccal, distal and lingual/palatal surface for all standing teeth, giving four surfaces investigated in total per tooth. The number of plaque-affected tooth sites was expressed as a percentage of the total number of sites in the mouth, to give the full mouth plaque score.
The patient's views of the acceptability of the Brushlink device were assessed by the means of comprehensive post-intervention questionnaire, which included the opportunity for open comments. This part of the study was carried out during the patient's general dental or hygiene appointment. Of the 103 patients that took part in the study 41 agreed to give acceptability feedback.
Results
One hundred and eight people were recruited to the study. Five patients did not complete the clinical trial part of the study. Two in the test group discovered they were unable or unwilling to manage the device and two found that the travel to the practice for assessments did not fit with their scheduled lifestyle. One participant was unable to complete the trial due to illness. Table 1 shows the age and gender of the study participants and the age distribution of the test and control group. All of the participants in the acceptability study were members of the test group. Figure 2 shows the plaque levels in test and control groups at each visit.
At baseline, the average plaque score of the test group was 40.12. In the control group, the comparative figure was 29.06. Table 2 shows that after two weeks the test group plaque score had reduced to 20.98; a reduction of almost 50%. The control group score was 22.82 which was a 22% decline from baseline. After a further two weeks, at the third visit, the test groups plaque score had declined from the baseline score of 40.12 to 11.66; a further 45% decline from the mid-trial level and 70% decline from baseline. The comparable reductions in the control group were to 22.82, a reduction of 20% from baseline at week two, and 20.49 at four weeks which represented a 29% decline from baseline (see Table 3).
With regard to the patient acceptability of the smartphone device, Box 1 indicates the responses to the questions 'How was your experience with Brushlink?' and 'How likely are you to recommend Brushlink?'. There were no significant differences in the acceptability between males and females or people of different age categories (p >0.05).
Open comments made in the acceptability questionnaire fell into four themes, these being: i) appreciation about learning the technical aspects of how to brush well; ii) emotional responses encompassing affection for the device and its sense of fun; iii) regulation of timing and regularity of brushing; iv) ease of use. Comments illustrative of these themes are presented in the following sections.
Brushing
'I didn't even know I had to angle the brush before Brushlink'
'I found it helped brush better (sic) and angled my brush differently'.
Emotional response
'Generally love it'
'Makes brushing your teeth more of a fun and interesting experience'
'I think it would be great for kids'.
Timing
'I liked that you brushed for two minutes without even knowing'
'I didn't know if I was brushing evenly for two minutes so this really helped'.
Ease of use
'So simple to set-up and use. Great visual aid'
'Really easy to use'
'Superb innovative device'
'Clever and simple to use'.
Discussion
Although there are approximately 31,000 health behaviour-related apps available for download, very few have been tested in randomised controlled trials in the intervention setting, with adequately powered samples.17 Most of the scientific literature concerning the use of apps to promote or sustain health have been small pilot or feasibility studies. Only two studies, neither of them RCTs, have been reported in the dental literature. Given the growing societal trend of increasing demand for health-related apps and increasing consumer acceptance of technology to support healthy behaviours, it is timely to undertake proper scientific enquiry into the effectiveness, efficiency and acceptability of oral health-related apps. However, given the capacity of modern technology to offer interventions to large populations at minimal cost, the current lack of well-designed RCT trials in both general and dental health is concerning. Research should therefore focus on conducting rigorous RCTs with a sufficient sample size to determine their true utility.
By undertaking such a study, we have demonstrated that a smartphone app, in conjunction with a small toothbrushing device, is highly effective in promoting toothbrushing. The plaque reductions achieved in the study showed that oral health advice in the dental surgery was significantly more effective when given in conjunction with the app technology (70% plaque reduction compared to 30%). The plaque reductions achieved were more than twice the 30%, which systematic reviews and meta analyses have shown are generally achieved in surgery-based toothbrushing trials.18,19 This is an important result given that twice daily brushing with a fluoride toothpaste has repeatedly been demonstrated to be the most effective and evidence-based method of reducing dental disease and is recommended in all three recent oral health-related NICE guidelines.
Given the potential scalability of the use of technology like this app, the possibilities of achieving a paradigm shift in oral health-related behaviour change are very promising but as yet, untapped. Furthermore, the most important outcome of this proof of functionality and acceptability is its potential for use in oral health research. For decades, researchers have struggled with the problem that, although oral hygiene is a key to positive oral health, we have hitherto been unable to measure it other than through self-reported data, with its inherent and notorious unreliability. Almost all oral health education and public interventions have relied on such data to assess effectiveness. The Brushlink app, reported here, offers researchers the ability to collect real time, person specific and accurate behavioural data; thereby, at last, giving researchers a means of running large trials of interventions without the need for mass dental examinations of research participants, which are highly expensive, often impractical and are prone to examiner bias.
Conclusion
In conclusion, this is the first RCT trial of an oral hygiene app. It has shown the app to be twice as effective as conventional oral hygiene advice and instruction. The app has the potential to promote population oral health and has offered researchers a very valuable research tool.
Change history
24 January 2020
Author's correction note: The authors here provide a note to further explain some sections of the paper that may have caused confusion. A decision was made that as this was a trial to compare the effectiveness of two interventions (oral health advice, with and without the Brushlink device) in pro...
References
Kressin N R, Boetimar V, Nunn M E, Spiro A 3rd. Increased preventive practices lead to greater tooth retention. J Dent Res 2003; 82: 223-227.
Al-Shammar K F, Al khabbaz A K, Al-Ansari J M, Neiva R, Wang H L. Risk indicators for tooth loss due to periodontal disease.J Periodontol 2005; 76: 1910-1918.
Axelsson P, Nystrom B, Lindhe J. The long-term effect of a plaque control program on tooth mortality, caries and periodontal disease in adults. Results after 30 years of maintenance.J Clin Periodontol 2004; 31: 749-757.
van der Weijden F, Slot D E. Oral hygiene in the prevention of periodontal diseases: the evidence.Periodontology 2000 2011; 55: 104-123.
Walsh T, Worthington H V, Glenny A M, Appelbe P, Marinho V, Shi X. Flouride toothpastes of different concentrations for preventing dental caries in children and adolescents.Cochrane Database Syst Rev 2010; 20: CD007868.
dos Santos A P, Nadanovsky P, de Oliviera B H. A systematic review and meta-analysis of the effects of fluoride toothpastes on the prevention of dental caries in the primary dentition of preschool children.Community Dent Oral Epidemiol 2013; 41: 1-12.
Godin G, Kok G. The theory of planned behaviour: a review of its applications to health-related behaviours.Am J Health Promot 1996; 11: 87-98.
Public Health England. Delivering better oral health: an evidence based toolkit. 2014. Available at https://www.gov.uk/government/publications/delivering-better-oral-health-an-evidence-based-toolkit-for-preventiona (accessed March 2019).
National Institute for Clinical and Healthcare Excellence. Oral Health: local authority and partners: public health guideline [PH55]. 2014. Available at https://www.nice.org.uk/guidance/ph55 (accessed March 2019).
National institute for Clinical and Healthcare Excellence. Oral health promotion: general dental practice. NICE guideline [NG30]. 2015. Available at https://www.nice.org.uk/guidance/ng30 (accessed March 2019).
Bandura A. Self-efficacy: toward a unifying theory of behavioral change. Psychol Rev 1977; 84: 191-215.
Tedesco L A, Keffer M A, Fleck-Kandath C. Self-efficacy, reasoned action, and oral health behaviour reports: a social cognitive approach to complianceJ Behav Med 1991; 14: 341-355.
Anagnostopoulos F, Buchanan H, Frousiounioti S, Niakas D, Potamianos G. Self-efficacy and oral hygiene beliefs about toothbrusing in dental patients a model-guided study.Behav Med 2011; 37: 132-139.
Miller W R, Rollnick S. Motivational Interviewing: Preparing People for Change. New York: Guildford Press, 2002.
Rollnick S, Miller W R. What is motivational interviewing. Behav Cogn Psychother 1995; 23: 325-334.
Zimmerman M A. Resistency theory: a strengths-based approach to research and practice for adolescent health.Health Educ Behav 2013; 40: 381-383.
Payne H E, Lister C, West J H, Bernhardt J M. Behavioural functionality of mobile apps in heath interventions: a systematic review of the literature.JMIR Mhealth Uhealth 2015; 3: e20.
Kay E J, Locker D. Is dental health education effective? A systematic review of current evidence.Community Dent Oral Epidemiol 1996; 24: 231-235.
Kay E, Vascott D, Hocking A, Nield H, Dorr C, Barrett H. A review of approaches for dental practice teams for promoting health.Community Dent Oral Epidemiol 2016; 44: 313-330.
Conflict of interests
Elizabeth Kay is a member of the Brushlink Scientific Committee but has no financial or commercial connection with, or interest in, the company.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Kay, E., Shou, L. A randomised controlled trial of a smartphone application for improving oral hygiene. Br Dent J 226, 508–511 (2019). https://doi.org/10.1038/s41415-019-0202-1
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41415-019-0202-1
This article is cited by
-
Effectiveness of an online application of the health action process approach (HAPA) theory on oral hygiene intervention in young adults with fixed orthodontic appliances: a randomized controlled trial
BMC Oral Health (2022)
-
Does personalised text messaging influence patients' caries risk?
Evidence-Based Dentistry (2020)