Abstract
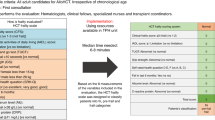
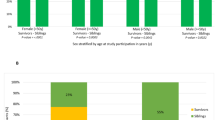
This prospective study designs an HCT Frailty Scale to classify alloHCT candidates into groups of frail, pre-frail, and fit, and to be implemented in the first consultation at no additional cost. The present scale is composed of the following eight variables: Clinical Frailty Scale, Instrumental Activities of Daily Living, Timed Up and Go Test, Grip Strength, Self-Health Rated, Falls, Albumin, and C-Reactive Protein. The Frailty score of a patient is the weighted sum of scores for each item, with weights assigned according to the hazard ratios of a multivariable Cox proportional hazards model estimated and validated with data on OS as the dependent variable, and the scores of the eight variables as explanatory ones, from 298 adults split into training (n = 200) and validation (n = 98) sets. For clinical use, the scale scores were transformed into three categories: scale score ≤1: fit; 1<scale score ≤5.5: pre-frail; scale score >5.5 frail. The estimated probabilities of 1-year OS in each group of frailty, were, respectively: 83.7%, 48.5%, and 16.5% (p < 0.001). In the validation cohort, the respective values were 90.3%, 69.5%, and 46.2% (p < 0.001). Pending further external validations, the HCT Frailty Scale is a low cost-highly informative prognostic signal of outcomes at the pre-transplant stage.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Copelan EA. Hematopoietic stem-cell transplantation. N. Engl J Med. 2006;354:1813–26.
Majhail NS, Farnia SH, Carpenter PA, Champlin RE, Crawford S, Marks DI, et al. Indications for autologous and allogeneic hematopoietic cell transplantation: guidelines from the American Society for blood and marrow transplantation. Biol Blood Marrow Transpl. 2015;21:1863–9.
Duarte RF, Labopin M, Bader P, Basak GW, Bonini C, Chabannon C, et al. Indications for haematopoietic stem cell transplantation for haematological diseases, solid tumours and immune disorders: current practice in Europe, 2019. Bone Marrow Transpl. 2019;54:1525–52.
Passweg JR, Baldomero H, Chabannon C, Basak GW, Corbacioglu S, Duarte R, et al. The EBMT activity survey on hematopoietic-cell transplantation and cellular therapy 2018: CAR-T’s come into focus. Bone Marrow Transplant. 2020;55:1604–13.
Pasquini MC, Srivastava A, Ahmed SO, Aljurf M, Atsuta Y, Doleysh C, et al. Worldwide Network for Blood and Marrow Transplantation (WBMT) recommendations for establishing a hematopoietic cell transplantation program (Part I): Minimum requirements and beyond. Hematol Oncol Stem Cell Ther. 2020;13:131–42.
Artz AS, Pollyea DA, Kocherginsky M, Stock W, Rich E, Odenike O, et al. Performance status and comorbidity predict transplant-related mortality after allogeneic hematopoietic cell transplantation. Biol Blood Marrow Transpl. 2006;12:954–64.
Sorror ML, Maris MB, Storb R, Baron F, Sandmaier BM, Maloney DG, et al. Hematopoietic cell transplantation (HCT)-specific comorbidity index: a new tool for risk assessment before allogeneic HCT. Blood. 2005;106:2912–9.
Abel GA, Klepin HD. Frailty and the management of hematologic malignancies. Blood. 2018;131:515–24.
Hegde A, Murthy HS. Frailty: the missing piece of the pre- hematopoietic cell transplantation assessment? Bone Marrow Transpl. 2018;53:3–10.
Morley JE, Vellas B, van Kan GA, Anker SD, Bauer JM, Bernabei R, et al. Frailty consensus: a call to action. J Am Med Dir Assoc. 2013;14:392–7.
Xue QL. The frailty syndrome: definition and natural history. Clin Geriatr Med. 2011;27:1–15.
Kanate AS, Perales MA, Hamadani M. Eligibility criteria for patients undergoing allogeneic hematopoietic cell transplantation. J Natl Compr Canc Netw. 2020;18:635–43.
Salas MQ, Atenafu EG, Bascom O, Wilson L, Lam W, Law AD, et al. Pilot prospective study of Frailty and Functionality in routine clinical assessment in allogeneic hematopoietic cell transplantation. Bone Marrow Transpl. 2021;56:60–9.
Rockwood K, Song X, MacKnight C, Bergman H, Hogan DB, McDowell I, et al. A global clinical measure of fitness and frailty in elderly people. CMAJ. 2005;173:489–95.
Lawton MP, Brody EM. Assessment of older people: self-maintaining and instrumental activities of daily living. Gerontologist. 1969;9:179–86.
Bohannon RW. Hand-grip dynamometry predicts future outcomes in aging adults. J Geriatr Phys Ther. 2008;31:3–10.
Podsiadlo D, Richardson S. The timed “Up & Go”: a test of basic functional mobility for frail elderly persons. J Am Geriatr Soc. 1991;39:142–8.
Mavaddat N, Parker RA, Sanderson S, Mant J, Kinmonth AL. Relationship of self-rated health with fatal and non-fatal outcomes in cardiovascular disease: a systematic review and meta-analysis. PLoS One. 2014;9:e103509.
Mohile SG, Dale W, Somerfield MR, Schonberg MA, Boyd CM, Burhenn PS, et al. Practical assessment and management of vulnerabilities in older patients receiving chemotherapy: ASCO guideline for geriatric oncology. J Clin Oncol. 2018;36:2326–47.
Yamamoto W, Fujii E, Matsumoto K, Yamamoto E, Aoki J, Tanaka M, et al. Prognostic value of pretransplant serum C-reactive protein in patients receiving reduced-intensity conditioning allogeneic hematopoietic stem cell transplantation. Int J Hematol. 2016;103:444–52.
Chee L, Tacey M, Lim B, Lim A, Szer J, Ritchie D. Pre-transplant ferritin, albumin and haemoglobin are predictive of survival outcome independent of disease risk index following allogeneic stem cell transplantation. Bone Marrow Transpl. 2017;52:870–7.
Muffly LS, Kocherginsky M, Stock W, Chu Q, Bishop MR, Godley LA, et al. Geriatric assessment to predict survival in older allogeneic hematopoietic cell transplantation recipients. Haematologica. 2014;99:1373–9.
Deschler B, Ihorst G, Schnitzler S, Bertz H, Finke J. Geriatric assessment and quality of life in older patients considered for allogeneic hematopoietic cell transplantation: a prospective risk factor and serial assessment analysis. Bone Marrow Transpl. 2018;53:565–75.
Rosko AE, Huang Y, Benson DM, Efebera YA, Hofmeister C, Jaglowski S, et al. Use of a comprehensive frailty assessment to predict morbidity in patients with multiple myeloma undergoing transplant. J Geriatr Oncol. 2019;10:479–85.
Nawas MT, Andreadis C, Martin TG, Wolf JL, Ai WZ, Kaplan LD, et al. Limitation in patient-reported function is associated with inferior survival in older adults undergoing autologous hematopoietic cell transplantation. Biol Blood Marrow Transpl. 2019;25:1218–24.
Olin RL, Fretham C, Pasquini MC, Arora M, Bhatt VR, Derman B, et al. Geriatric assessment in older alloHCT recipients: association of functional and cognitive impairment with outcomes. Blood Adv. 2020;4:2810–20.
Lin RJ, Elko TA, Devlin SM, Shahrokni A, Jakubowski AA, Dahi PB, et al. Impact of geriatric vulnerabilities on allogeneic hematopoietic cell transplantation outcomes in older patients with hematologic malignancies. Bone Marrow Transpl. 2020;55:157–64.
Polverelli N, Tura P, Battipaglia G, Malagola M, Bernardi S, Gandolfi L, et al. Multidimensional geriatric assessment for elderly hematological patients (>/=60 years) submitted to allogeneic stem cell transplantation. A French-Italian 10-year experience on 228 patients. Bone Marrow Transpl. 2020;55:2224–33.
Artz AS, Logan B, Zhu X, Akpek G, Bufarull RM, Gupta V, et al. The prognostic value of serum C-reactive protein, ferritin, and albumin prior to allogeneic transplantation for acute myeloid leukemia and myelodysplastic syndromes. Haematologica. 2016;101:1426–33.
Bouillon K, Kivimaki M, Hamer M, Sabia S, Fransson EI, Singh-Manoux A, et al. Measures of frailty in population-based studies: an overview. BMC Geriatr. 2013;13:64.
Fried LP, Tangen CM, Walston J, Newman AB, Hirsch C, Gottdiener J, et al. Frailty in older adults: evidence for a phenotype. J Gerontol A Biol Sci Med Sci. 2001;56:M146–56.
Rockwood K, Wolfson C, McDowell I. The Canadian Study of Health and Aging: organizational lessons from a national, multicenter, epidemiologic study. Int Psychogeriatr. 2001;13:233–7.
Fried LP, Ferrucci L, Darer J, Williamson JD, Anderson G. Untangling the concepts of disability, frailty, and comorbidity: implications for improved targeting and care. J Gerontol A Biol Sci Med Sci. 2004;59:255–63.
Cesari M, Gambassi G, van Kan GA, Vellas B. The frailty phenotype and the frailty index: different instruments for different purposes. Age Ageing. 2014;43:10–2.
Derman BA, Kordas K, Ridgeway J, Chow S, Dale W, Lee SM, et al. Results from a multidisciplinary clinic guided by geriatric assessment before stem cell transplantation in older adults. Blood Adv. 2019;3:3488–98.
Koll TT, Rosko AE. Frailty in hematologic malignancy. Curr Hematol Malig Rep. 2018;13:143–54.
Holmes HM, Des Bordes JK, Kebriaei P, Yennu S, Champlin RE, Giralt S, et al. Optimal screening for geriatric assessment in older allogeneic hematopoietic cell transplantation candidates. J Geriatr Oncol. 2014;5:422–30.
Chen X, Mao G, Leng SX. Frailty syndrome: an overview. Clin Inter Aging. 2014;9:433–41.
Hale M, Shah S, Clegg A. Frailty, inequality and resilience. Clin Med (Lond). 2019;19:219–23.
Acknowledgements
We thank Dr. Hans Messner, a cherished physician who pioneered stem cell transplantation at Princess Margaret Cancer Centre. He provided the guidance and resources to initiate this pilot study.
Author information
Authors and Affiliations
Contributions
MQS and RK collected the data, interpreted the results, and wrote the paper. RK and MQS designed the HCT Frailty scale. RK designed the GA and the study. SA provided valuable input into GA assessment and study design. EA did the statistical analysis, interpreted the results, and provided valuable input into the interpretation and reviewed the manuscript. IP, EAS, OB, LW, CC, ADL, WL, INB, DDHK, AG, AV, FVM, JHL, and JM provided valuable input into the interpretation and reviewed the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Salas, M.Q., Atenafu, E.G., Pasic, I. et al. Impact of hematopoietic cell transplant frailty scale on transplant outcome in adults. Bone Marrow Transplant 58, 317–324 (2023). https://doi.org/10.1038/s41409-022-01892-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41409-022-01892-3
This article is cited by
-
HCT frailty scale for younger and older adults undergoing allogeneic hematopoietic cell transplantation
Bone Marrow Transplantation (2023)
-
Impact of age on hospitalization and outcomes post allogeneic hematopoietic cell transplantation outcome, a single center experience
Annals of Hematology (2023)