Abstract
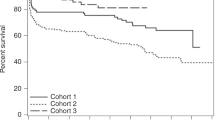
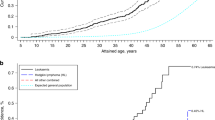
The aim of this retrospective study was to determine the incidence and the clinical outcome of secondary oral cancer (SOC) and to assess potential risk factors in a large cohort of patients (n = 908), who received allogeneic hemopoietic cell transplantation (HCT) either for a malignant (n = 733) or nonmalignant hematologic disease (n = 175). The median follow-up of 438 transplant survivors was 17 years. Twelve patients developed SOC at a median of 13.5 years since HCT and at a median age of 47 years. The 35-year cumulative incidence function of SOC development was 3.47%. In univariate analysis, factors associated with increased incidence of SOC were reduced intensity conditioning and chronic graft-versus-host disease (cGvHD). On multivariate analysis, nonmalignant disease and duration of oral cGvHD ≥15 months were independent risk factors for SOC development. Nonmalignant disease recipients had 3.94× higher than expected rate of SOC (95% confidence interval, 1.50–10.39%, p = 0.0055). Recipients whose oral cGvHD persisted for more than ≥15 months had 58.6× higher than expected rate of SOC (95% confidence interval, 13.3–258.1%), p < 0.0001). This study demonstrates that oral cGvHD and a diagnosis of nonmalignant hematologic disease are strong risk factors in the SOC development.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Baker KS, DeFor TE, Burns LJ, Ramsay NK, Neglia JP, Robison LL. New malignancies after blood or marrow stem cell transplantation in children and adults: incidence and risk factors. J Clin Oncol. 2003;21:1352–8.
Majhail NS, Brazauskas R, Rizzo JD, Sobecks RM, Wang Z, Horowitz MM, et al. Secondary solid cancers after allogeneic hematopoietic cell transplantation using busulfan–cyclophosphamide conditioning. Blood. 2011;117:316–22.
Curtis RE, Rowlings PA, Deeg HJ, Shriner DA, Sociè G, Travis LB, et al. Solid cancers after bone marrow transplantation. N Engl J Med. 1997;336:897–904.
Bhatia S, Louie AD, Bhatia R, O’Donnell MR, Fung H, Kashyap A, et al. Solid cancers after bone marrow transplantation. J Clin Oncol. 2001;19:464–71.
Shimada K, Yokozawa T, Atsuta Y, Kohno A, Maruyama F, Yano K, et al. Solid tumors after hematopoietic stem cell transplantation in Japan: incidence, risk factors and prognosis. Bone Marrow Transplant. 2005;36:115–21.
Gallagher G, Forrest DL. Second solid cancers after allogeneic hematopoietic stem cell transplantation. Cancer. 2007;109:84–92.
Sociè G, Henry-Amar M, Bacigalupo A, Hoes J, Tichelli A, Lijungman P, et al. Malignant tumors occurring after treatment of aplastic anemia. European Bone Marrow Transplantation-Severe Aplastic Anaemia Working Party. N Engl J Med. 1993;329:1152–7.
Rizzo JD, Curtis RE, Sociè G, Sobocinski KA, Gilbert E, Landgren O, et al. Solid cancers after allogeneic hematopoietic cell transplantation. Blood. 2009;113:1175–83.
Shah AT, Wu E, Wein RO. Oral squamous cell carcinoma in post-transplant patients. Am J Otolaryngol. 2013;34:176–9.
Chen MH, Chang PM, Li WY, Hsiao LT, Hong YC, Liu CY, et al. High incidence of oral squamous cell carcinoma independent of HPV infection after allogeneic hematopoietic SCT in Taiwan. Bone Marrow Transplant. 2011;46:567–72.
Curtis RE, Metayer C, Rizzo JD, Sociè G, Sobocinski KA, Flowers ME, et al. Impact of chronic GvHD therapy on the development of squamous-cell cancers after hematopoietic stem-cell transplantation: an international case-control study. Blood. 2005;105:3802–11.
Szeto CH, Shek TW, Lie AK, Au WY, Yuen AP, Kwong YL. Squamous cell carcinoma of the tongue complicating chronic oral mucosal graft-versus-host disease after allogenic hematopoietic stem cell transplantation. Am J Hematol. 2004;77:200–2.
Bacigalupo A, Ballen K, Rizzo D, Giralt S, Lazarus H, Ho V, et al. Defining the intensity of conditioning regimens: working definitions. Biol Blood Marrow Transplant. 2009;15:1628–33.
Khabori MA, El-Emary M, Xu W, Guyatt G, Galal A, Kuruvilla J, et al. Impact of intensity of conditioning therapy in patients aged 40-60 years with AML/myelodysplastic syndrome undergoing allogeneic transplantation. Bone Marrow Transplant. 2011;46:516–22.
Glucksberg H, Storb R, Fefer A, Buckner CD, Neiman PE, Clift RA, et al. Clinical manifestations of graft-versus- host disease in human recipients of marrow from HL-A-matched sibling donors. Transplantation. 1974;18:295–304.
Lee SJ, Vogelsang G, Flowers ME. Chronic graft-versus-host disease. Biol Blood Marrow Transplant. 2003;9:215–33.
Funk GF, Karnell LH, Robinson RA, Zhen WK, Trask DK, Hoffman HT. Presentation, treatment, and outcome of oral cavity cancer: a National Cancer Data Base report. Head Neck. 2002;24:165–80.
Mello FW, Melo G, Pasetto JJ, Barcellos Silva CA, Warnakulasuriya S, Correa Rivero ER. The synergistic effect of tobacco and alcohol consumption on oral squamous cell carcinoma: a systematic review and meta-analysis. Clin Oral Investig. 1019;23:2849–59.
Warnakulasuriya S. Controversial factors on causation of oral cancer. In: Warnakulasuriya S, Greenspan JS, editors. Text book of oral cancer. Springer Nature Switzerland AG; London, 2020. p. 439–48.
Gluckman E, Socie G, Devergie A, Bourdeau-Esperou H, Traineau R, Cosset JM. Bone marrow transplantation in 107 patients with severe aplastic anemia using cyclophosphamide and thoraco-abdominal irradiation for conditioning: long-term follow-up. Blood. 1991;78:2451–5.
Warnakulasuriya S. Global epidemiology of oral and oropharingeal cancer. Oral Oncol. 2009;45:309–16.
Santarone S, Pepe A, Meloni A, Natale A, Pistoia L, Olioso P, et al. Secondary solid cancer following hematopoietic cell transplantation in patients with thalassemia major. Bone Marrow Transplant. 2017;53:39–43.
Mawardi H, Elad S, Correa ME, Stevenson K, Woo S-B, Almazrooa R, et al. Oral epithelial dysplasia and squamous cell carcinoma following allogeneic hematopoietic stem cell transplantation: clinical presentation and treatment outcomes. Bone Marrow Transplant. 2011;46:884–91.
Leisenring W, Friedman DL, Flowers MED, Schwartz JL, Deeg HJ. Nonmelanoma skin and mucosal cancers after hematopoietic cell transplantation. J Clin Oncol. 2006;24:1119–26.
Themeli M, Petrikkos L, Waterhouse M, Bertz E, Lagadinou E, Zoumbos N, et al. Alloreactive microenvironment after human hematopoietic cell transplantation induces genomic alterations in epithelium through an ROS-mediated mechanism: in vivo and in vitro study and implications to secondary neoplasia. Leukemia. 2010;24:536–43.
Mehrotra R, Gupta DK. Exciting new advances in oral cancer diagnosis: avenues to early detection. Head Neck Oncol. 2011;3:33–41.
Guneri P, Epstein JB. Late stage diagnosis of oral cancer: components and possible solutions. Oral Oncol. 2014;50:1131–6.
Majhail NS, Rizzo JD, Lee SJ, Alijurf M, Atsuta Y, Bonfim C, et al. Recommended screening and preventive practices for long-term survivors after hematopoietic cell transplantation. Biol Blood Marrow Transplant. 2012;18:348–71.
Neville BW, Day TA. Oral cancer and precancerous lesions. CA Cancer J Clin. 2002;52:195–215.
Inamoto Y, Shah NN, Savani BN, Shaw BE, Abraham AA, Ahmed IA, et al. Secondary solid cancer screening following hematopoietic cell transplantation. Bone Marrow Transplant. 2015;50:1013–23.
Speight PM, Epstein J, Kujan O, Lingen MW, Nagao T, Ranganathan K, et al. Screening for oral cancer-a perspective from the Global Oral Cancer Forum. Oral Med Oral Pathol Oral Radiol. 2017;123:680–7.
Acknowledgements
The authors thank Prof. Saman Warnakulasuriya, Emeritus Professor, King’s College London, for his critical review of the paper and his suggestions.
Author information
Authors and Affiliations
Contributions
SS and PDB contributed patients, designed the study, analyzed the data, and wrote the manuscript; AN, GP, DV, and ADB contributed to data acquisition and analyzed the results; SA performed statistical study and contributed to the interpretation of the results. All authors read and critically reviewed the manuscript and approved the final version.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Santarone, S., Natale, A., Angelini, S. et al. Secondary oral cancer following hematopoietic cell transplantation. Bone Marrow Transplant 56, 1038–1046 (2021). https://doi.org/10.1038/s41409-020-01147-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41409-020-01147-z
This article is cited by
-
Oral microbial changes and oral disease management before and after the treatment of hematological malignancies: a narrative review
Clinical Oral Investigations (2023)
-
Long-term safety of photobiomodulation therapy for oral mucositis in hematopoietic cell transplantation patients: a 15-year retrospective study
Supportive Care in Cancer (2021)
-
Regarding chronic graft-versus-host disease in children and adolescents with thalassemia after hematopoietic stem cell transplantation
International Journal of Hematology (2021)