Abstract
The continuous emergence of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) variants poses challenges to the effectiveness of neutralizing antibodies. Rational design of antibody cocktails is a realizable approach addressing viral immune evasion. However, evaluating the breadth of antibody cocktails is essential for understanding the development potential. Here, based on a replication competent vesicular stomatitis virus model that incorporates the spike of SARS-CoV-2 (VSV-SARS-CoV-2), we evaluated the breadth of a number of antibody cocktails consisting of monoclonal antibodies and bispecific antibodies by long-term passaging the virus in the presence of the cocktails. Results from over two-month passaging of the virus showed that 9E12 + 10D4 + 2G1 and 7B9-9D11 + 2G1 from these cocktails were highly resistant to random mutation, and there was no breakthrough after 30 rounds of passaging. As a control, antibody REGN10933 was broken through in the third passage. Next generation sequencing was performed and several critical mutations related to viral evasion were identified. These mutations caused a decrease in neutralization efficiency, but the reduced replication rate and ACE2 susceptibility of the mutant virus suggested that they might not have the potential to become epidemic strains. The 9E12 + 10D4 + 2G1 and 7B9-9D11 + 2G1 cocktails that picked from the VSV-SARS-CoV-2 system efficiently neutralized all current variants of concern and variants of interest including the most recent variants Delta and Omicron, as well as SARS-CoV-1. Our results highlight the feasibility of using the VSV-SARS-CoV-2 system to develop SARS-CoV-2 antibody cocktails and provide a reference for the clinical selection of therapeutic strategies to address the mutational escape of SARS-CoV-2.
Similar content being viewed by others
Introduction
Coronavirus disease 2019 (COVID-19) is caused by the infection of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) and has been a persistent and large-scale pandemic around the world, causing hundreds of millions of infections and millions of deaths [1,2,3]. SARS-CoV-2 encodes an exoribonuclease in nonstructural protein 14 (nsp14-ExoN) that is proposed to have the function of nucleotide proofreading [4]. However, the virus is still in fast mutation. The World Health Organization (WHO) labeled several SARS-CoV-2 variants as variant of concern (VOC) and variant of interest (VOI) based on their potential transmissibility and risk. At present, there are five VOCs, B.1.1.7 (Alpha), B.1.351 (Beta), P.1 (Gamma), B.1.617.2 (Delta) and B. 1.1.529 (Omicron), respectively [5, 6]. These variants contain mutations that contribute to the profile alteration of the virus such as L452R, S477N, T478K, E484K and N501Y. The L452R stabilized the conformation of the S protein [7] and led to an increased affinity between the virus and angiotensin converting enzyme 2 (ACE2) [8]. Substitution in S477 with asparagine (N) resulted in an additional glycosylation of receptor binding domain (RBD) [9]. The basic charged lysine (K) substitution in T478 is thought to increase the electrostatic potential of spike (S) protein [10]. These mutations, individually or in combination, are high likely to give rise to the immune escape of virus from vaccines and neutralizing antibodies [11, 12].
Abundant neutralizing antibodies targeting conserved epitopes of the S protein have been identified in the recent two years [13, 14], but mutations at key sites may still lead to the loss of activity. The emergence of Omicron variant with numerous and scattered mutations in the N-terminal domain (NTD) and RBD renders no effective to the existing neutralizing antibodies [15, 16]. Researchers compared the activity of antibodies in clinic against the Omicron and found that most of them lost neutralization activity except Sotrovimab (VIR-7831) and DXP-604 retained partial activity [17]. Another study came to a similar conclusion that only Brii-198 had better neutralization against Omicron compared to D614G virus [18], which raised concerns about the feasibility of using a single neutralizing antibody to address the mutation of SARS-CoV-2.
The combinational use of antibodies targeting different epitopes is a widely accepted strategy. Antibodies in different epitopes can bind to S protein simultaneously, thus the virus is more difficult to break through. Besides, antibodies in different epitopes may have diverse mechanisms. The combination of CoV2-06 and CoV2-14 was effective in preventing infection by SARS-CoV-2 variants, which was far superior to the two antibodies alone [19]. The combination of REGN10987 and REGN10933 protected hamsters and non-human primates prophylactically and therapeutically, and effectively reduced viral load and pathological changes [20]. However, combinations by less breadth antibodies still present an escape risk. Besides, antibody combinations designed based on current variants always exhibit broad neutralizing activity, but their breadth is difficult to fully understand and does not provide guidance for future variants.
In this study, we formulated several sets of antibody cocktails from our SARS-CoV-2 antibody repertoire and evaluated the viral escape ability from these cocktails in a replication-competent vesicular stomatitis virus model with S protein replacement (VSV-SARS-CoV-2) through long-term passaging [21]. VSV is of low pathogenicity and causes only mild symptoms in animals and human individuals, making it a safe research model [22, 23]. The glycoprotein of VSV is an envelope protein that mediates receptor binding and viral membrane fusion, similar in function to the S protein of SARS-CoV-2, thus the virus can be used as a pseudotyped substitute for lethal viruses. Considering the combination of two or more antibodies may potentially complicate the product components, introduce complex manufacturing procedures, and increase production costs, we developed some of these monoclonal antibodies into a bunch of bispecific antibodies using our BAPTS bispecific antibodies development platform [24, 25].
Materials and methods
Monoclonal antibody preparation
Plasmids pcDNA3.4 comprising heavy chains and light chains of antibodies were transiently expressed in ExpiCHO-S cells using the ExpiCHO™ expression system (Thermo Fisher). Briefly, the cells were expanded to 6 × 106/mL the day before transfection and were then diluted to 3 × 106/mL by ExpiCHO™ expression medium (Gibco). Plasmids were diluted to 20 μg/mL by cold OptiPRO medium (Gibco) and transfected into the ExpiCHO-S cells 17 h later according to the manufacturer’s instructions. The transfected cells were placed in a 37 °C, 8% CO2 shaker, followed by Max Titer feeding 18 h later. Then, the cells were transferred to a 32 °C, 5% CO2 atmosphere. On day 5, the second Max Titer feeding was performed. When the cell viability was reduced to about 90%, the medium was collected and centrifuged at 300 × g for 10 min. The supernatant was subsequently further centrifuged at 7,000 × g for 30 min to remove the cell debris. After filtered through 0.22 μm membranes (Millipore), the medium that containing antibodies was submitted to MabSelect Sure affinity purification. The full-length IgG antibodies were eluted with 100 mM citric acid (pH 3.0). Purified antibodies were stored in a cocktailed buffer consisting of 10 mM Histidine-HCl, 9% trehalose, and 0.01% polysorbate 80.
Epitope binning
Competition enzyme-linked immunosorbent assay (ELISA) was performed to explore the epitope correlation of two antibodies. Briefly, the first antibody at the concentration of 2 μg/mL was coated on plates (BEAVER) and incubated at 4 °C overnight. Then, excess antibodies were washed away by PBS and blocked by 3% skim milk. SARS-CoV-2 S1 protein (Sino Biological) was biotinylated using an EZ-Link™ Sulfo-NHS-LC-LC-Biotin kit (ThermoFisher), followed by mixing with 50 μg/mL of the second competition antibodies or PBS blank control. After incubation at 37 °C for 1 h, plates were washed three times with PBS and the diluted Ultrasensitive Streptavidin-Peroxidase Polymer (Sigma) was added (1:2000) subsequently. Then the plates was incubated at 37 °C for 1 h again. TMB Single-Component Substrate Solution (Solarbio) was used to detect the S1 binding with the coated first antibodies. The absorbance at 450 nm was measured in an Infinite M200 PRO Multimode Microplate Reader (TECAN). Competitive percentage of two antibodies was calculated with reference to the PBS blank control.
Bispecific antibody design and preparation
Based on our Bispecific Antibody by Protein Trans-splicing (BAPTS) platform, fragment A and fragment B of from two antibodies with poor epitope clash were chose to generate bispecific antibodies as previous described [24]. In brief, three plasmids pCDNA3.4 carrying full-length of heavy chain A, light chain A, and Fc region of heavy chain B jointing C-terminal of half intein were co-transfected into ExpiCHO-S cells to express fragment A; two plasmids pCDNA3.4 carrying light chain B and Fab region of heavy chain B jointing N-terminal of half intein were co-transfected to express fragment B. Fragment A and fragment B were purified using HiTrap KappaSelect or HiTrap LambdaSelect (Cytiva). Glycine (100 mM, pH2.5) or acetic acid (100 mM, pH3.0) was used as elution buffer. For generating bispecific antibodies, fragment A and fragment B were mixed in a mole ratio of 1:1.6. The reaction happened in the presence of 2 mM Tris-(2-carboxyethyl)-phosphine and terminated by 2 mM dehydroascorbic acid after reaction for 4 h at room temperature. The formed BsAbs were preliminary processed by Protein A resin (GE Healthcare) and subsequently purified employing HiTrap Capto MMC ImpRes (Cytiva). A linear elution scheme was tailored for Capto MMC purification, from 10 mM phosphate +10 mM Tris+50 mM NaCl (pH6.0) to 10 mM phosphate +10 mM Tris (pH9.0). The obtained BsAbs with purity >98%, which was confirmed by size exclusion chromatography, were concentrated and stored at −80 °C.
Antigen-binding and ACE2 competition ELISA
For quantifying the binding ability of neutralizing antibodies to SARS-CoV-1, the SARS-CoV-1 S protein (SinoBiological) was diluted to 1.0 μg/mL with ELISA Coating Buffer (Solarbio) and added to 96-well ELISA plates with 100 μL per well, and then placed in a 4 °C condition for overnight incubation. The next day, the plates were washed 4 times with 200 μL of PBST each time, followed by blocking with 200 μL of 3% skim milk. Neutralizing antibodies were diluted to 0.1 μg/mL in 1% bull serum albumin (Sigma) solution and 100 μL was added to each well. Subsequently, plates were incubated at 37 °C for 1 h. After further wash, 100 μL of goat anti-human IgG (Fc specific)-Peroxidase antibody (1: 5000 dilution, Sigma) was added and incubated for another 1 h at 37 °C. Then 100 μL of TMB substrate (Solarbio) was added and incubated in the dark for 15 min to visualize the binding of the antibody to the SARS-CoV-1 antigen. The chromogenic reaction was terminated by adding 50 μL of stop buffer (Solarbio) and the absorbance at 450 nm was immediately read in the microplate reader (TECAN).
For investigating competitive binding of antibodies in the cocktail to trimeric SARS-CoV-2 S protein, recombinant hACE2-Fc protein was biotinylated using the EZ-Link sulfo-nhs-biotin kit (ThermoFisher) according to the manufacturer’s instructions. ELISA plates were coated with SARS-CoV-2 S protein in the same way as described above. The work concentration of biotinylated ACE2 was optimized, and the 80% of maximal effect (EC80) concentration of antigen binding was used for this experiment. Equal volumes of antibodies and biotinylated ACE2 (50 μL: 50 μL) were mixed and added into the plates. Detection was performed with Ultrasensitive Streptavidin−Peroxidase Polymer (1: 2000, Sigma). PBS and non-biotinylated ACE2 protein substituted for competing antibodies served as blank control and positive control, respectively.
Surface plasmon resonance (SPR)
The BIAcore 8 K system was used to detect the binding of antibodies to the S trimer of SARS-CoV-2 WA1/2020 (AcroBiosystems). The S protein trimer was covalently coupled to the CM5 sensor chip using an amino coupling kit (Cytiva). After the response value reached about 70 relative unit (RU), the coupling was stopped and the excess S protein was washed away, followed by blocking unbound sites with ethanolamine (Cytiva). Antibodies were diluted to 50 μg/mL with HBS-EP buffer (Cytiva). In order to detect whether more than one antibodies can bind to S protein simultaneously, the first antibody was loaded into the system and flowed for 600 s to meet saturated binding. Then the second antibody was loaded into the identical channel and flowed for another 600 s. If there was a third or more antibody, it was proceeded in the same way. Channels flowing with the same antibody as previous rounds were used as control. The simultaneous binding of antibodies was judged by the accumulation of response values from different rounds of flow.
VSV passaging
The replication competent vesicular stomatitis virus incorporating the spike of SARS-CoV-2 (VSV-SARS-CoV-2) was generated as described previously [26], under the technical guidance of Professor Tao Sun of Shanghai Jiao Tong University. For testing the breadth of antibody cocktails, Vero E6 cells were seeded into 96-well plates with 2.5 × 104 cells per well. The next day, antibodies were 5-fold serially diluted starting from 100 μg/mL in DMEM medium supplementing 10% FBS (Gibco). Wells without antibodies or containing the same concentrations of REGN10933 were set as control. Then 50 μL of the antibody dilution was mixed with 50 μL of VSV-SARS-CoV-2 in the final multiplicity of infection (MOI) of 0.01. After incubated at room temperature for 30 min, the virus-antibody mixture was added to the cells and grown for two days at 37 °C, 5% CO2. The cytopathic effect (CPE) of cells was examined under a microscope (Nikon). If the CPE in a well reached 20%, the virus was considered to have broken through the protection of antibodies. The medium supernatant of the wells with the highest antibody concentration that has been broken was collected and was diluted 12 times for the next round of passaging. After the virus broke through the highest antibody concentration wells or reached the designed endpoint, the medium supernatant was collected for next generation sequencing. Single nucleotide polymorphisms (SNP) of the S region was analyzed according to the sequencing results.
VSV characterization
The replication rates of mutant viruses were measured according to the increase in number of viral particles in one generation. In 24-well plates, 1 × 105 Vero E6 cells were seeded per well and cultured for 24 h. The next day, each mutant VSV-SARS-CoV-2 was added to the cells with duplicates at MOI = 0.01 per well. Then the plates were gently tapped to mix the virus evenly, followed by incubation for another 12 h. Cells were disassociated from the plate using 100 μL of trypsin (Gibco) and fixed by 4% paraformaldehyde (Solarbio) at the time points of 0 h, 1 h, 2 h, 3 h, 4 h and 5 h. The virus particles that have infected cells were quantified by analyzing the green fluorescent protein reporter that was comprised into the viral genome in a flow cytometer. The replication rate of the virus was calculated based on the mean fluorescence intensity.
For investigating the ACE2 susceptibility of mutant VSV-SARS-CoV-2, Vero E6 cells were seeded into 96-well plates at 2.5 × 104 cells per well. The next day, the recombinant ACE2-Fc protein which was obtained from ExpiCHO™ expression system (Thermo Fisher) was fivefold serially diluted in DMEM medium supplementing 10% FBS (Gibco). The VSV-SARS-CoV-2 viruses were diluted by medium and mixed with equal volume of ACE2-Fc dilutions. The final MOI was 0.01. Then, 100 μL of the mixture was added to the cells, followed by further incubation at 37 °C under 5% CO2 condition for 48 h. Under a microscope (Nikon), the CPE of the cells was checked and the IC50 values were calculated according to the equation of IC50 = Antilog (D - C × (50 - B) / (A - B)). Where A means percent inhibition higher than 50%, B represents percent inhibition less than 50%, C is log10 (dilution factor), and D is log10 (sample concentration) that the inhibition is less than 50%.
Pseudovirus neutralization
The pseudovirus neutralization study was performed as described previously [21]. In brief, 293T-ACE2 cells were plated at a density of 1 × 104 cells per well into a 96-well white transparent bottom plate, and cultured overnight at 37 °C in 5% CO2. Serial 10-fold dilutions of neutralizing antibodies were mixed with pseudoviruses. After incubation at 37 °C for 30 min, the mixture was added into the 293T-ACE2 cells. The medium was replaced with fresh medium 6 h later. All operations involving pseudoviruses were performed in a biosafety level 2 laboratory in the School of Pharmacy, Shanghai Jiao Tong University. After further culturing for 48 h, 50 μL of ONE-Glo luciferase substrate (Promega) was added to each well, and the fluorescence intensity was detected on a microplate reader (TECAN) immediately. Data were analyzed using GraphPad Prism software and the neutralization efficiencies of antibodies were calculated according to the four-parameter nonlinear fitting results.
Results
Selection of antibodies for combinational use
In our previous study [21], we identified a broad-spectrum neutralizing antibody 2G1 that targets the tip of RBD through a small contact surface from our SARS-CoV-2 antibody repertoire, which makes it less possible in epitope clash with other antibodies and thus suitable for combinational use. We performed competition ELISA to map the epitope information of antibodies. As expected, all of the tested antibodies competed with themselves (Fig. 1a). Antibodies in the repertoire could be roughly divided into three groups according to their competition relation, of which antibody 2G1 was in the group 3.
a Epitope mapping of the antibody repertoire using a competition ELISA. A heatmap was used to show the competition percentages between two antibodies. The epitopes of antibodies were roughly classified into three groups according to their competitive relations. b Binding to SARS-CoV-1 S protein by antibodies in the repertoire. Trimeric SARS-CoV-1 S protein was coated on 96-well ELISA plates and incubated with 0.1 μg/mL of neutralizing antibodies. The binding was detected using a HRP-labeled goat anti-human IgG (Fc specific) antibody. c Concentration-dependent neutralization of SARS-CoV-1 pseudovirus by neutralizing antibodies. Serial diluted antibodies were incubated with the virus and used to infect 293T-ACE2 cells. The infection was quantified using a fluorescence quantification kit. Data from two replicates are shown as mean ± S.D. d Antibodies competitively blocked the ACE2 binding to SARS-CoV-2 S trimer as measured by ELISA. Recombinant human ACE2 protein and phosphate buffer solution (PBS) were used as controls.
Then, we examined whether these antibodies could cross bind to SARS-CoV-1 as the ability the binding to the Sarbecovirus could be a reflection of conserved activity by an anti-SARS-CoV-2 antibody. As shown in Fig. 1b, all antibodies in group 1 and 2, but not in group 3, efficiently bound to SARS-CoV-1 S protein at the concentration of 0.1 μg/mL. We then performed pseudo-typed SARS-CoV-1 virus neutralization (Fig. 1c). Antibodies 7G10, 8G4, 9E12, 9D11, 8C12 and 9A6 showed high neutralizing activity to SARS-CoV-1, while most of them were in epitope group 1. Subsequently, we explored the ACE2 competition profile of these antibodies and found that antibodies in group 1 and 3 showed excellent ACE2 competition while the group 2 antibodies had little or negligeable level of the competition (Fig. 1d).
These results revealed certain regularities. Antibodies in group 1 were able to bind to SARS-CoV-1 spike and neutralized the virus by blocking ACE2 interaction. The group 2 antibodies targeted non-ACE2 epitope in the spike of SARS-CoV-1 but were incapable of neutralizing the virus. The group 3 antibodies only showed SARS-CoV-2 binding and neutralizing ability, instead of SARS-CoV-1. To minimize the possibility of epitope clash, we intended to select antibodies from the group 1and 2 to make up combinations with 2G1. Finally, antibodies 9E12, 9D11, 8G4 and 11F7 from group 1 and antibodies 10D4 and 7B9 from group 2 were selected. Then, we used two formulating strategies, one was two monoclonal antibodies paired with 2G1, another was a bispecific antibody paired with 2G1. We designed bispecific antibodies 7B9-9D11, 10D4-8G4 and 10D4-11F7 using the BAPTS platform [24]. Eventually, four antibody cocktails were generated, including 9E12 + 10D4 + 2G1, 7B9-9D11 + 2G1, 10D4-8G4 + 2G1 and 10D4-11F7 + 2G1.
Testing the tolerance of antibody cocktails by long-term virus passaging
We then used a VSV-SARS-CoV-2 system that can generate random mutations during replication to investigate the antimutagenic potential of the four cocktails (Fig. 2a). The virus in this investigation experienced over 30 passages, and the entire 30 passaging cycles costed more than 60 days, which offered the virus an opportunity generating sufficient mutations in adequate time. The VSV-SARS-CoV-2 broke through the protection of monotherapy by 9E12, 10D4 and 2G1 at the 9th, 1st and 4th passages, respectively (Fig. 2b). The emergency use authorization (EUA) antibody REGN10933, which has a similar epitope with 2G1, was used as a control [21]. The virus broke through REGN10933 at the 3rd passage. As for the three bispecific antibodies, 10D4-8G4 lost activity at the 4th passage, 10D4-11F7 lost neutralization at the 1st passage. By contrast, 7B9-9D11 showed outstanding tolerance and was not broken through even at the designed endpoint of the 30th passage, despite the reduced neutralization.
a The passaging scheme of the long-term protection of antibody cocktails in a Vero E6 cell model. b Antibody cocktails were fivefold serially diluted from 100 μg/mL and mixed with VSV-SARS-CoV-2 before infecting Vero E6 cells. After 48 h, the cytopathic effect in each well was examined and medium from the highest concentration wells that the viruses showed positive infection was collected for the next round of passage. An authorized antibody REGN10933 was used as control. c Comparison of the replication rates of VSV-SARS-CoV-2 virus that broke through the protection of antibody cocktail. The replication rates were calculated according to the mean fluorescence intensity measured by flow cytometry. d Simultaneous binding of antibodies to WA1/2020 S trimer as measured by surface plasmon resonance. The simultaneous binding was confirmed by the accumulation of response values from different rounds of flow.
Combinational therapy by 9E12 + 10D4 significantly enhanced the anti-mutation ability and prevented the infection of the virus until the 29th passage (Fig. 2b). The triple combination by 9E12 + 10D4 + 2G1 showed more stronger resistance to viral mutation and had not been broken through even at the 33rd passage. The 7B9-9D11 + 2G1 cocktail showed not only outstanding tolerance, but also good neutralizing activity. The results indicated that the antibody cocktails we designed improved tolerance to virus from monotherapy substantially. However, not all combinations were promising in dealing with mutational escape. Combinations by 10D4-8G4 + 2G1 and 10D4-11F7 + 2G1 increased resistance to mutations merely, and were broken through at 5th and 7th, respectively.
The replication rate of a virus is in correlation with its transmissibility. In view of the good tolerance of combinations by 9E12 + 10D4 + 2G1 and 7B9-9D11 + 2G1, we collected the passaged viruses and measured their replication rates (Fig. 2c). The passaged viruses generally had lower growth rates than the WA1/2020 control. The slope of the replication curve of viruses from 9E12 + 10D4 + 2G1 and 7B9-9D11 + 2G1 were 0.120 (versus 0.220 in WA1/2020 control) and 0.148 (versus 0.193 in WA1/2020 control). Notably, although the virus broke through the protection of monotherapy by 2G1 quickly, the replication rate of the mutant virus was relatively slower (slope = 0.069 and 0.082). The slowed replication rates of these viruses might suggest less possibility of pandemic in the real world.
Subsequently, we verified whether antibodies in 9E12 + 10D4 + 2G1 and 7B9-9D11 + 2G1 cocktails could bind to S protein simultaneously using surface plasmon resonance (SPR). When 9E12, 10D4 and 2G1, or 7B9-9D11 and 2G1 flowed through the antigen-coated chip sequentially, the response signal increased accordingly, while that in the control channels remained unchanged, indicating that antibodies in both of the two cocktails could bind to S protein simultaneously (Fig. 2d).
ACE2 susceptibility of passaged VSV-SARS-CoV-2 viruses
The binding of S protein to ACE2 on the cell surface is a key step of virus invasion. Higher the affinity of S protein to ACE2 means the easier for the virus infecting cells. Meanwhile, the higher ACE2 affinity makes the virus easier to be neutralized by recombinant ACE2 protein in the medium. Thus, the susceptibility of viruses to recombinant ACE2 protein can be used to evaluate the difficulty of viruses invading cells. To further verify the reliability of the anti-mutational potential of the VSV-SARS-CoV-2 system in evaluating antibody cocktails, we examined the ACE2 susceptibility for 9E12 + 10D4 + 2G1 and 7B9-9D11 + 2G1. As shown in Fig. 3a and b, none of the mutant viruses had increased ACE2 susceptibility compared with the WA1/2020 control, indicating that mutations in these viruses did not increase the affinity to ACE2 and may not lead to an increased risk of transmission. Specifically, viruses from pressurized passaging by 9E12 + 10D4, 7B9-9D11 and 7B9-9D11 + 2G1 showed more than ninefold decreases in ACE2 sensitivity, and the 9E12 + 10D4 virus decreased by more than 27-fold. The reduced ACE2 susceptibility is correlated with the slowed cell invasion; this should be a contributive factor in the reduction of virus replication rates that observed in Fig. 2c. Reduced ACE2 susceptibility may result in degraded viral transmissibility without presenting an epidemic risk. Therefore, even though the mutant viruses escaped or weakened the protection of the two antibody cocktails, transmission of these viruses may not occur in nature due to the reduced transmissibility.
a–b After the viruses broke through the protection of 9E12 + 10D4 + 2G1 (a) and 7B9-9D11 + 2G1 (b), or reached the designed endpoint, the multi-passaged viruses were mixed with gradient diluted recombinant ACE2 protein and were used to infect Vero E6 cells. The cytopathic effect was observed and the antigenic affinity shift of the viral S protein was assessed according to the neutralizing alteration to recombinant ACE2.
Deep sequencing identifying key viral escape sites
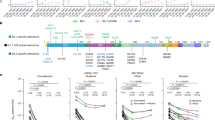
To understand how these two cocktails protect cells from mutant virus infection, we performed next generation sequencing to identify mutation sites in the S protein of the VSV-SARS-CoV-2 variants. Sole pressurized passaging by 9E12 generated three high proportion mutations, i.e., G485R, V503E and V615M (Fig. 4a). While both antibodies 10D4 and 2G1 generated only one mutation site, K529N and F486V, respectively. The more mutations the virus generates may mean that the antibody is more difficult to be broken through, which could explain why the virus required more passages to break through the protection of 9E12 than 10D4 or 2G1 (Fig. 2b). In the antibody cocktail by 9E12 + 10D4, the virus generated six mutation sites in S protein and two of them were in RBD region. Correspondingly, the virus did not break through 9E12 + 10D4 until the 29th passage (Fig. 2b), suggesting that 9E12 + 10D4 might be a relative tolerant combination that is difficult to be broken through. The virus in the 2 μg/mL wells of 9E12 + 10D4 + 2G1 developed three mutations including H69R, G485R, and R683G. Although the three mutations did not completely break through the protection of 9E12 + 10D4 + 2G1, it weakened the neutralizing efficacy moderately. In terms of the 7B9-9D11 + 2G1 cocktail, four and five mutation sites came about from the 7B9-9D11 and 7B9-9D11 + 2G1 viruses respectively to weaken the antibody activity (Fig. 4b).
a–b Virus-containing medium from pressurized culture in 9E12+10D4+2G1 (a) and 7B9-9D11+2G1 (b) was collected and the next generation sequencing was performed to identify nucleotide mutations in the spike gene. The single nucleotide polymorphism (SNP) was analyzed with sufficient sequencing depth coverage to ensure the reliability. The RBD region is colored in light green and mutation sites are colored in red.
It is worth noting that the mutation sites of the viruses resistant to cocktails were not the addition of mutations from that of single antibodies. This may imply that more than one scheme for the virus to escape and be involved in the overall conformational change of the S protein. Besides, most of these mutations are not found in VOC strains. This suggested that even if an antibody neutralizes most of the current variants, there might be still unknown mutations that can escape. Therefore, the anti-mutational potential of antibody combinations designed based on the current variants still needs to be explored reliably.
All these antibodies in our repertoire recognize the RBD region; however, there occurred non-RBD mutations. Studies suggested that mutations in the non-epitope region likely represent tissue culture adaptations [27, 28]. We also infer that these mutations may together change the S protein in conformation and thus reduce antibody binding.
Verifying the breadth of cocktails picked from VSV-SARS-CoV-2 passaging
Using a replication incompetent pseudovirus neutralizing system, we tested the activity of both 9E12 + 10D4 + 2G1 and 7B9-9D11 + 2G1 cocktails against all current VOC and VOI strains, as well as the SARS-CoV-1. As for monoclonal antibodies, 9E12 showed good neutralization against variants except for Omicron (BA.1); 10D4 inhibited the infection of most variants, especially the Omicron (half maximal inhibitory concentration IC50 = 1.4180 μg/mL), but its neutralization efficiency was relatively low, the IC50 values were generally over 0.1 μg/mL; 2G1 ultra-potently neutralized most variants, but had minimized activity against Omicron and had no activity against SARS-CoV-1 (Fig. 5a). By contrast, the combinations of 9E12 + 10D4 and 10D4 + 2G1 not only neutralized Omicron, but also improved the efficiency against other variants. The 9E12 + 2G1 presented both high efficiency and the ability to neutralize SARS-CoV-1. Furthermore, the combination by 9E12 + 10D4 + 2G1 showed good neutralization to all variants, which was not achieved by monoclonal antibodies. Similar results were also observed on the 7B9-9D11 + 2G1 cocktail (Fig. 5b). Antibody 2G1 increased the anti-viral efficiency and bispecific antibody 7B9-9D11 improved the anti-viral breadth.
a–b Antibody cocktails 9E12+10D4+2G1 (a) and 7B9-9D11+2G1 (b) were tenfold serially diluted from 101 μg/mL to 10−5 μg/mL and incubated with pseudo-typed viruses for 30 min, and then the mixture was added into a plate seeded with 293T-ACE2 cells. The infection of viruses to cells was quantified 48 h later.
Discussion
With the continuous emergency of SARS-CoV-2 variants, there are more and more mutations occurred in the S region. The latest emerged variant Omicron sublineages have at least 30 substitutions in S region, which remarkably remodeled the S conformation [16]. The cryo-electron microscope structure revealed that mutations in Omicron enhanced the interaction between adjacent “up” and “down” conformation RBDs, which makes the S protein more stable and less conformational diversity [17]. Besides, mutations in Omicron also increased affinity with ACE2 and facilitated evasion from immunotherapy by neutralizing antibodies [29, 30]. In fact, immune escape has been reported not only for Omicron but also for all VOC strains [31,32,33,34]. Antibody cocktails with breadth can effectively solve this issue. Several studies evaluated the antibody breadth using the VSV-SARS-CoV-2 system;[35, 36] however, inadequate round of passaging is difficult to determine the tolerance of antibody cocktails accurately. We designed four cocktails, including monoclonal antibodies and bispecific antibodies, and explored their antiviral tolerance in the VSV-SARS-CoV-2 system. The experimental duration was more than 60 days thus the virus was allowed to produce enough mutations. We found that cocktails by 9E12 + 10D4 + 2G1 and 7B9-9D11 + 2G1 were able to protect Vero E6 cells from infection even experienced 30 passages. Although the virus reduced neutralizing activities by generating mutations, both ACE2 sensitivity and replication rate of the mutant virus decreased correspondingly, suggesting that these mutations may not become epidemic strains.
The replication period of the VSV from invading cells to the release of virus particles costs 6-8 h [37]. Which means a single round of passaging can finish 3–4 such cycles at the MOI of 0.01. Thus, 30 passaging is sufficient to finish about 100 such cycles. In particular, these cycles were proceeded under the pressure of neutralizing antibodies. IgG antibody is secreted at least 4 days after human infection with SARS-CoV-2 [38] and the virual mutational escape happens less frequently because by the time the IgG antibody is secreted there is already a high viral titer. REGN10933 was broken through at the 3rd passaging in our results, while the first prevalent variant Beta that breaking through REGN10933 in the ture world was discovered half a year after REGN10933 was developed. It would be better to passage the virus until breakthrough, but how many passes it takes is unpredictable.
Based on our deep sequencing results of the S protein of VSV-SARS-CoV-2, we found that more mutations the virus needs to generate to break through the protection of more tolerated antibodies. The virus produced four mutations to break through the protection of 9E12, while only one mutation to break through 10D4 or 2G1. This was positively correlated with the rounds of passaging for their breakthrough. RBD antibodies can be classified into four types according to their germlines and antigen-binding models [7]. A number of antibodies in class 3 and class 4 with binding sites outside the RBD-ACE2 interface showed broad neutralization. Novel epitope antibodies targeting the back of the RBD-ACE2 interface identified recently and showed Omicron variant neutralization, which were called class 5 antibodes [16]. However, the breadth of a single antibody is always limited. In our study, although the virus generated mutations in the 9E12 + 10D4 + 2G1 and 7B9-9D11 + 2G1 cocktail samples, the two cocktails showed good neutralization from beginning to end. This result solidified the use of antibody cocktails to achieve a broad-spectrum anti-SARS-CoV-2 purpose.
At the time of designing these antibody cocktails, we did not know the neutralizing activity of these cocktails against VOC and VOI strains in advance. Through the pressurized culture against VSV-SARS-CoV-2, we obtained the 9E12 + 10D4 + 2G1 and 7B9-9D11 + 2G1 cocktails with good tolerance. To our surprise, the two cocktails neutralized all current VOC and VOI strains, as well as SARS-CoV-1 in the pseudovirus system, which validated the reliability of using our VSV-SARS-CoV-2 system for screening and exploring antibody cocktails with breadth.
Taken together, our study provided an approach to develop SARS-CoV-2 antibody cocktails with breadth and the feasibility of reasonably design of antibody cocktails to increase the anti-viral tolerance, which may work up the clinical solutions for tackling SARS-CoV-2 evasion.
References
Finelli L, Gupta V, Petigara T, Yu K, Bauer KA, Puzniak LA. Mortality among US patients hospitalized with SARS-CoV-2 infection in 2020. JAMA Netw Open. 2021;4:e216556.
Erikstrup C, Hother CE, Pedersen OBV, Molbak K, Skov RL, Holm DK, et al. Estimation of SARS-CoV-2 infection fatality rate by real-time antibody screening of blood donors. Clin Infect Dis. 2021;72:249–53.
Giovanetti M, Benedetti F, Campisi G, Ciccozzi A, Fabris S, Ceccarelli G, et al. Evolution patterns of SARS-CoV-2: Snapshot on its genome variants. Biochem Biophys Res Commun. 2021;538:88–91.
Smith EC, Blanc H, Surdel MC, Vignuzzi M, Denison MR. Coronaviruses lacking exoribonuclease activity are susceptible to lethal mutagenesis: evidence for proofreading and potential therapeutics. PLoS Pathog. 2013;9:e1003565.
Tao K, Tzou PL, Nouhin J, Gupta RK, de Oliveira T, Kosakovsky Pond SL, et al. The biological and clinical significance of emerging SARS-CoV-2 variants. Nat Rev Genet. 2021;22:757–73.
Magazine N, Zhang T, Wu Y, McGee MC, Veggiani G, Huang W. Mutations and evolution of the SARS-CoV-2 Spike Protein. Viruses. 2022;14:640.
Barnes CO, Jette CA, Abernathy ME, Dam KA, Esswein SR, Gristick HB, et al. SARS-CoV-2 neutralizing antibody structures inform therapeutic strategies. Nature. 2020;588:682–7.
Liu ZM, VanBlargan LA, Bloyet LM, Rothlauf PW, Chen RE, Stumpf S, et al. Identification of SARS-CoV-2 spike mutations that attenuate monoclonal and serum antibody neutralization. Cell Host Microbe. 2021;29:477–88.
Watanabe Y, Allen JD, Wrapp D, McLellan JS, Crispin M. Site-specific glycan analysis of the SARS-CoV-2 spike. Science. 2020;369:330–3.
Shang J, Ye G, Shi K, Wan YS, Luo CM, Aihara H, et al. Structural basis of receptor recognition by SARS-CoV-2. Nature. 2020;581:221–4.
Wang ZJ, Schmidt F, Weisblum Y, Muecksch F, Barnes CO, Finkin S, et al. mRNA vaccine-elicited antibodies to SARS-CoV-2 and circulating variants. Nature. 2021;592:616–22.
Hoffmann M, Arora P, Gross R, Seidel A, Hornich BF, Hahn AS, et al. SARS-CoV-2 variants B.1.351 and P.1 escape from neutralizing antibodies. Cell. 2021;184:2384–93.
Kreye J, Reincke SM, Kornau HC, Sanchez-Sendin E, Corman VM, Liu HJ, et al. A therapeutic non-self-reactive SARS-CoV-2 antibody protects from lung pathology in a COVID-19 Hamster model. Cell. 2020;183:1058–69.
Brouwer PJM, Caniels TG, van der Straten K, Snitselaar JL, Aldon Y, Bangaru S, et al. Potent neutralizing antibodies from COVID-19 patients define multiple targets of vulnerability. Science. 2020;369:643–50.
Cai Y, Zhang J, Xiao T, Lavine CL, Rawson S, Peng H, et al. Structural basis for enhanced infectivity and immune evasion of SARS-CoV-2 variants. Science. 2021;373:642–8.
Yin W, Xu Y, Xu P, Cao X, Wu C, Gu C, et al. Structures of the Omicron spike trimer with ACE2 and an anti-Omicron antibody. Science. 2022;375:1048–53.
Cui Z, Liu P, Wang N, Wang L, Fan K, Zhu Q, et al. Structural and functional characterizations of infectivity and immune evasion of SARS-CoV-2 Omicron. Cell. 2022;185:860–71.
Gobeil SM, Henderson R, Stalls V, Janowska K, Huang X, May A, et al. Structural diversity of the SARS-CoV-2 Omicron spike. Mol Cell. 2022;82:2050–68.
Ku Z, Xie X, Davidson E, Ye X, Su H, Menachery VD, et al. Molecular determinants and mechanism for antibody cocktail preventing SARS-CoV-2 escape. Nat Commun. 2021;12:469.
Baum A, Ajithdoss D, Copin R, Zhou A, Lanza K, Negron N, et al. REGN-COV2 antibodies prevent and treat SARS-CoV-2 infection in rhesus macaques and hamsters. Science. 2020;370:1110–5.
Ma H, Guo Y, Tang H, Tseng CK, Wang L, Zong H, et al. Broad ultra-potent neutralization of SARS-CoV-2 variants by monoclonal antibodies specific to the tip of RBD. Cell Discov. 2022;8:16.
Chen M, Zhang XE. Construction and applications of SARS-CoV-2 pseudoviruses: a mini review. Int J Biol Sci. 2021;17:1574–80.
Case JB, Rothlauf PW, Chen RE, Kafai NM, Fox JM, Smith BK, et al. Replication-competent vesicular stomatitis virus vaccine vector protects against SARS-CoV-2-mediated pathogenesis in mice. Cell Host Microbe. 2020;28:465–74.
Han L, Chen JS, Ding K, Zong HF, Xie YQ, Jiang H, et al. Efficient generation of bispecific IgG antibodies by split intein mediated protein trans-splicing system. Sci Rep.-Uk. 2017;7:8360.
Zong H, Han L, Chen J, Pan Z, Wang L, Sun R, et al. Kinetics study of the natural split Npu DnaE intein in the generation of bispecific IgG antibodies. Appl Microbiol Biotechnol. 2022;106:161–71.
Tang HE, Ke Y, Wang L, Wu MY, Sun T, Zhu JW. Recombinant decoy exhibits broad protection against omicron and resistance potential to future variants. Pharmaceuticals (Basel). 2022;15:1002.
Dieterle ME, Haslwanter D, Bortz RH, Wirchnianski AS, Lasso G, Vergnolle O, et al. A replication-competent vesicular stomatitis virus for studies of SARS-CoV-2 spike-mediated cell entry and its inhibition. Cell Host Microbe. 2020;28:486–96.
Lau SY, Wang P, Mok BWY, Zhang ANJX, Chu H, Lee ACY, et al. Attenuated SARS-CoV-2 variants with deletions at the S1/S2 junction. Emerg Microbes Infec. 2020;9:837–42.
Gobeil SM, Henderson R, Stalls V, Janowska K, Huang X, May A, et al. Structural diversity of the SARS-CoV-2 Omicron spike. Mol Cell. 2022;82:2050–68.
Araf Y, Akter F, Tang YD, Fatemi R, Parvez MSA, Zheng C, et al. Omicron variant of SARS-CoV-2: Genomics, transmissibility, and responses to current COVID-19 vaccines. J Med Virol. 2022;94:1825–32.
Collier DA, De Marco A, Ferreira I, Meng B, Datir RP, Walls AC, et al. Sensitivity of SARS-CoV-2 B.1.1.7 to mRNA vaccine-elicited antibodies. Nature. 2021;593:136–41.
Madhi SA, Baillie V, Cutland CL, Voysey M, Koen AL, Fairlie L, et al. Efficacy of the ChAdOx1 nCoV-19 Covid-19 vaccine against the B.1.351 Variant. N Engl J Med. 2021;384:1885–98.
Alter G, Yu J, Liu J, Chandrashekar A, Borducchi EN, Tostanoski LH, et al. Immunogenicity of Ad26.COV2.S vaccine against SARS-CoV-2 variants in humans. Nature. 2021;596:268–72.
Planas D, Veyer D, Baidaliuk A, Staropoli I, Guivel-Benhassine F, Rajah MM, et al. Reduced sensitivity of SARS-CoV-2 variant Delta to antibody neutralization. Nature. 2021;596:276–80.
Case JB, Rothlauf PW, Chen RE, Liu Z, Zhao H, Kim AS, et al. Neutralizing antibody and soluble ACE2 inhibition of a replication-competent VSV-SARS-CoV-2 and a clinical isolate of SARS-CoV-2. Cell Host Microbe. 2020;28:475–85.
Weisblum Y, Schmidt F, Zhang F, DaSilva J, Poston D, Lorenzi JC, et al. Escape from neutralizing antibodies by SARS-CoV-2 spike protein variants. Elife. 2020;9:e61312.
Timm C, Gupta A, Yin J. Robust kinetics of an RNA virus: Transcription rates are set by genome levels. Biotechnol Bioeng. 2015;112:1655–62.
Lagunas-Rangel FA, Chavez-Valencia V. What do we know about the antibody responses to SARS-CoV-2? Immunobiology. 2021;226:152054.
Acknowledgements
We would like to acknowledge following organizations and individuals for their assistances in the preparation of the manuscript: Professor Tao Sun of SJTU for providing technical and material supports in generating the VSV-SARS-CoV-2 system. This work was funded by the National Natural Science Foundation of China (81773621, 82073751 to JWZ); the National Science and Technology Major Project “Key New Drug Creation and Manufacturing Program” of China (No.2019ZX09732001-019 to JWZ); the Key R&D Supporting Program (Special support for developing medicine for infectious diseases) from the Administration of Chinese and Singapore Tianjin Eco-city to Jecho Biopharmaceuticals Ltd. Co.; Zhejiang University special COVID-19 grant 2020XGZX099 and Shanghai Jiao Tong University “Crossing Medical and Engineering” grant 20×190020003 to JWZ.
Author information
Authors and Affiliations
Contributions
LH, YQX and JWZ conceived the study and designed the experiments. HM, HFZ, JJL, YLY, YK, YJL, HNT and LW conducted the experiments. HM and JWZ wrote and revised the manuscript. SSW, YSY, MYW, YLB, BHZ, HYY, HJ and TS provided technical assistance. TS All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ma, H., Zong, Hf., Liu, Jj. et al. Long-term passaging of pseudo-typed SARS-CoV-2 reveals the breadth of monoclonal and bispecific antibody cocktails. Acta Pharmacol Sin 44, 1455–1463 (2023). https://doi.org/10.1038/s41401-022-01043-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41401-022-01043-w