Abstract
Deletion and duplication of 16p11.2 (BP4–BP5) have been associated with an increased risk of intellectual disability and psychiatric disorder. This is the first study to compare the frequency of a broad spectrum of psychiatric disorders in children with 16p11.2 deletion and duplication. We aimed to evaluate (1) the nature and prevalence of psychopathology associated with copy number variation (CNV) in children with 16p11.2 by comparing deletion and duplication carriers with family controls; (2) whether deletion and duplication carriers differ in frequency of psychopathology. 217 deletion carriers, 77 deletion family controls, 114 duplication carriers, and 32 duplication family controls participated in the study. Measures included standardized research diagnostic instruments. Deletion carriers had a higher frequency of any psychiatric disorder (OR = 8.9, p < 0.001), attention deficit hyperactivity disorder (ADHD) (OR = 4.0, p = 0.01), and autism spectrum disorder (ASD) (OR = 39.9, p = 0.01) than controls. Duplication carriers had a higher frequency of any psychiatric diagnosis (OR = 5.3, p = 0.01) and ADHD (OR = 7.0, p = 0.02) than controls. The prevalence of ASD in child carriers of deletions and duplications was similar (22% versus 26%). Comparison of the two CNV groups indicated a higher frequency of ADHD in children with the duplication than deletion (OR = 2.7, p = 0.04) as well as a higher frequency of overall psychiatric disorders (OR = 2.8, p = 0.02) and psychotic symptoms (OR = 4.7, p = 0.02). However, no differences between deletion and duplications carriers in the prevalence of ASD were found. Both deletion and duplication are associated with an increased risk of psychiatric disorder, supporting the importance of early recognition, diagnosis, and intervention in these groups.
Similar content being viewed by others
Introduction
Copy number variations (CNVs) in 16p11.2 (deletion and duplication) between break points 4 and 5 (BP4–BP5) (600 kb, chr16; 29.6–30.2 mb-HG19) occur at a frequency of ~3 in 10,0001. Around 71% of the 16p11.2 deletions occur de novo while the majority of the 16p11.2 duplications (70%) are familial2. This is consistent with the notion that 16p11.2 deletions have a greater impact on functioning, resulting in reduced fecundity3. Both 16p11.2 deletion and duplication have been associated with the risk for autism spectrum disorder (ASD). Evidence comes from studies of individuals with ASD4,5,6,7,8,9,10,11 with a meta-analysis of 3613 cases reporting a prevalence of 0.50% (95%CI: 0.31–0.82%) for the 16p11.2 deletion and of 0.25% (96%CI: 0.14–0.56%) for the duplication12. The 16p11.2 duplication, but not deletion, has been linked to risk of schizophrenia in a meta-analysis of 16,772 cases reporting a prevalence of 0.35% (95%CI: 0.27–0.45%) in cases compared to 0.03% in controls (95%CI: 0.02–0.05%)13. This has been supported by comparisons of schizophrenia patients and controls13 and parent–proband trios14. The effect of these CNVs on mean IQ is a decrease of approximately two standard deviations for the deletion and one standard deviation for the duplication2,15,16. Apart from ASD, studies of 16p11.2 deletion carriers indicate high frequencies of attention deficit hyperactivity disorder (ADHD) (19%15 to 38%17), anxiety disorders (6%15 to 25%18), mood disorders (15%18), oppositional defiant disorder (ODD), and other disruptive disorders (13%15 to 39%3). For carriers with the duplication, high rates of ADHD (30%3) have been reported.
Interestingly, these chromosomal rearrangements have been associated with mirrored physical phenotypic effects. The 16p11.2 deletion has been associated with the risk of morbid obesity and large head circumference, while the 16p11.2 duplication has been associated with low body mass index (BMI) and small head circumference2,18,19. Taking into account evidence suggesting links between small head circumference and schizophrenia20,21 and large head circumference with autism22,23, it has been suggested that these mirrored phenotypic effects (overgrowth versus undergrowth phenotype) extend to include psychopathology24, although this has not yet been formally evaluated. More specifically, it has been suggested that differences in gene dosage associated with a single set of genes within 16p11.2 (deletion) versus three copies (duplication) may mediate risk of ASD versus schizophrenia25,26. The 16p11.2 CNV has been presented as an example of this theory, such that deletion carriers may be at increased risk of ASD in particular, whilst duplication carriers are at risk of ASD and schizophrenia2,18,26.
Despite strong evidence that 16p11.2 deletions and duplications are associated with an increased risk of psychiatric conditions, the majority of studies are based on limited and non-systematic assessments (e.g., medical records). Although informative, such records are less suited to systematic evaluation of large samples, because of differences between medical centers and clinicians in diagnostic methods used and clinical documentation. With the exception of schizophrenia and ASD, previous studies have been based on relatively small samples, without the availability of control samples to allow comparisons.
Here, we report the largest study to date using detailed systematically performed psychiatric assessments to determine the nature and prevalence of psychopathology in children with deletion or duplication of 16p11.2. We hypothesized that children with 16p11.2 deletion and duplication have a higher frequency of psychiatric disorder than family controls. We also hypothesized that deletion carriers would be more severely affected than duplication carriers, based on findings that the deletion is more likely to arise de novo, whereas the duplication is more frequently inherited. Finally, given the evidence that the 16p11.2 CNV is associated with a mirror phenotype of head and body size, we hypothesized that the children with 16p11.2 deletion have a higher frequency of ASD compared to those with 16p11.2 duplication while children with 16p11.2 duplication have a higher frequency of psychotic symptoms than those with 16p11.2 deletion.
Materials/subjects and methods
Sample
This study combined child samples (age <18 years old) recruited through Medical Genetics clinics and collected in Europe (EU) and the US (Table 1). The samples were provided from the ECHO study, the 16p11.2 European Consortium, the IMAGINE-ID study, and the Simons VIP Consortium (Table 2). The sample characteristics of the ECHO study, 16p11.2 European Consortium, and the Simons VIP Consortium have been described elsewhere2,15. The study methodology and sample assessment of the UK ECHO study and IMAGINE-ID project are identical. A subset of these families (i.e., from the Simon’s VIP cohort) has been described in prior studies in terms of their IQ, ASD, and schizophrenia diagnoses2,27.
Carrier status for the 16p11.2 deletion or duplication was confirmed for all individuals through clinical chromosome microarrays, medical records and/or confirmation in a research laboratory. All participants had a CNV in 16p11.2 BP4–BP5 region, excluding those in the adjacent region. Family members (siblings) who did not carry the CNV participated as family controls (controls) (Table 1). To assess potential recruitment bias in children, as a supplementary analysis, we further divided the carriers into (a) probands (individuals who first came to the attention of medical services) and (b) relative carriers (i.e., their siblings who were identified and diagnosed following CNV diagnosis of the proband) and compared the frequencies of psychiatric diagnoses between these two groups. Current analyses included individuals ≥3 years old in order to standardize diagnoses, especially for ASD, in very young children15.
The study was approved by the appropriate local ethics committees and institutional review boards. Each participant and his or her caregiver, when appropriate, provided informed written consent/assent to participate prior to recruitment.
Psychiatric assessments
Assessments were performed using research diagnostic instruments as previously reported2 under the supervision of experienced and licensed clinicians who gave the best estimate clinical and research DSM-IV-TR (Table 2). Only diagnoses that were available for all participating sites were examined. Only 2% of children with deletion and duplication were diagnosed with any syndromal psychotic disorder versus 0% of controls. Therefore, psychotic symptoms were examined instead.
IQ scores have already been reported for this sample2. We present the full-scale IQ scores and comparisons of psychopathology for subgroups of carriers with and without intellectual disability (ID, as defined by IQ ≤ 70).
Statistical analysis
Data analysis was conducted using Stata (version 13)28. Descriptive statistics were calculated to assess the frequency of psychiatric disorder. Random effects logit models were performed to determine whether group status (e.g., probands versus controls) (independent variable) was associated with an increased risk for psychiatric disorder (dependent variable: 0 = no diagnosis, 1 = diagnosis present) while accounting for familial clustering (i.e., the family that each individual belongs to). Odds ratios (ORs) and 95% confidence intervals (95%CIs) were derived and adjusted for age, sex, and cohort status (i.e., EU versus US)2. In cases where the maximum likelihood estimates tended to infinity (i.e., rare outcomes/zero values), Firth’s method29 was used30. To assess recruitment bias, we repeated these analyses comparing probands versus relative carriers. In order to reduce the number of statistical comparisons, anxiety disorders were included in the analyses as a summary variable (i.e., any anxiety disorder). We tested the associations between psychopathology and gender, inheritance status and ID using the phi coefficient.
Results
Table 1 shows the descriptive statistics of the sample by cohort status (i.e., EU and US).
Deletion carriers versus family controls
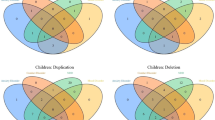
217 carriers and 77 controls were included in the analyses. 48% of the carriers met criteria for at least one psychiatric disorder (Table 3, S-Table 1, Fig. 1). This prevalence was higher than for controls (17%, OR = 8.9, p < 0.001). The most prevalent diagnosis in the carriers was ADHD (29%). This prevalence was higher than in controls (13%, OR = 4.0, p = 0.01). ASD was the second most common diagnosis in carriers (22%), which was higher than in controls (0%, OR = 39.9, p = 0.01). ID was also more frequent among carriers (30%) than controls (0%, OR = 58.7, p = 0.004). No significant differences were found in the prevalence of anxiety disorders, ODD/CD, and psychotic symptoms in deletion carriers compared to controls. Male children with deletions were more likely than females to be diagnosed with any psychiatric disorder, ASD and ID, and individuals with inherited deletion were more likely to have ID (S-Table 2).
Duplication carriers versus family controls
114 carriers and 32 controls were included in the analyses. 63% of the carriers had at least one psychiatric disorder (Table 3, S-Table 1, Fig. 1). This frequency was higher than for controls (31%, OR = 5.3, p = 0.01, Table 3). ADHD was the most common diagnosis in the carriers (42%) and was elevated compared to controls (19%, OR = 7.0, p = 0.02). There were no differences in the prevalence of anxiety disorders, ASD, ODD/CD, and psychotic symptoms between carriers and controls. ID was higher in carriers (34%) than controls (3%, OR = 56.7, p = 0.03). Males were more likely to be diagnosed with ODD/CD, and individuals with ID to be diagnosed with ASD (S-Table 2).
Deletion versus duplication carriers
Duplication carriers had higher frequencies of any diagnosis (OR = 2.8, p = 0.02), ADHD (OR = 2.7, p = 0.04) and psychotic symptoms (OR = 4.7, p = 0.02) than deletion carriers. No other differences were found (Table 3).
Assessment of potential recruitment bias
No differences were found between probands and relative carriers with the deletion in the prevalence of psychiatric disorders (S-Table 3). However, probands with the duplication had higher frequencies of any psychiatric disorder than relative carriers (OR = 3.9, p = 0.01).
Discussion
Psychiatric disorders in children with 16p11.2 deletion and duplication
Our findings indicate that the mental health consequences of the 16p11.2 deletion and duplication are broad, similar to findings in other CNVs (e.g., 22q11.2 deletion syndrome31,32).
ASD frequencies were higher in deletion carriers when compared to controls. In addition, almost half of the carriers with either the deletion or duplication were diagnosed with at least one psychiatric diagnosis, a frequency much higher than for non-carriers. This is similar to previously reported frequencies in medical records-based studies of individuals with 16p11.2 deletion33 and duplication3. ADHD was the most commonly diagnosed disorder affecting between 30 and 40% of deletion and duplication carriers, similar to the frequencies previously reported3,15,17,18. ID was present in about a third of deletion and duplication carriers and was also much more common than amongst controls. The frequency of anxiety and ODD/CD disorders and psychotic symptoms did not differ between carriers and controls, consistent with the previous studies15,18.
Previous studies in population-based samples of CNV carriers have found high frequencies of cognitive impairments and psychiatric symptoms24,34. This indicates that these high frequencies are not attributable to recruitment bias but are also representative of unselected CNV populations. Indeed, we generally did not find evidence of ascertainment bias effects on phenotypic assessment, as the frequencies of psychiatric diagnoses did not differ between probands and relative carriers. The only exception was our finding of higher frequencies of any psychiatric diagnoses in child duplication compared to relative carriers.
Although we found evidence for differences in the prevalence of psychotic symptoms, we did not find evidence for differences in the prevalence of ASD between 16p11.2 deletion and duplication carriers, for which we had more power. Thus, our findings do not provide support of a mirror phenotype for a psychiatric disorder. More generally, both deletion and duplication showed significant and overlapping psychopathology and any differences were of degree rather than suggesting contrasting mirror effects at the level of psychopathology.
Interestingly, we found associations between sex and any psychiatric disorder, ASD and ID in children with 16p11.2 deletion and ODD/CD in children with 16p11.2 duplication, indicating an increased risk for males. No other associations were found with ADHD or psychotic symptoms which agrees with a previous study that examined questionnaire responses18 as well as with findings related to another CNV on chromosome 22, resulting in 22q11.2 deletion syndrome32. These findings point to the possible negation of sex-related burden to some psychiatric disorders by these CNVs35. Apart from an increased risk of ASD in children with 16p11.2 duplication, psychiatric disorders did not occur more frequently in participants with ID in children with 16p11.2 deletion or duplication. Although this could reflect insufficient power, it could also indicate that these CNVs have pleiotropic effects on IQ and psychopathology36. Finally, there was an association between inherited status and higher risk of ID indicating that potential parental genetic and environmental effects might be negatively implicated on child intelligence. There were no other associations with inheritance status and psychiatric diagnoses, similar to a previous study15.
Strengths and limitations
This is the largest study to date to perform detailed phenotypic assessments on children with 16p11.2 deletion and duplication and compare the frequency of psychopathology with familial controls as well as between deletion and duplication carriers.
Our findings may be influenced by ascertainment bias. First, although we did not recruit individuals from psychiatric services, ascertainment was based on a phenotype significant enough to trigger clinical genetic testing (e.g., developmental delay). Second, although for many phenotypes we did not find evidence for recruitment bias in our analyses, we did find higher frequencies of any psychiatric diagnoses in child duplication probands compared to child relative carriers. We have previously explained our ascertainment strategies and limitations15,32. It is noteworthy that there were relatively high frequencies of psychopathology in familial controls. 17% and 31% of non-carrier child relatives of individuals with deletion and duplication, respectively, met criteria for at least one psychiatric diagnosis. The frequencies of ADHD (13% for deletion and 19% for duplication) and ASD (7% for duplication) were higher than we would expect from a population-based sample (5–7% and 1%, respectively). Potential explanations could be increased background environmental risk (e.g., the effect of family psychopathology), or perhaps the presence of polygenic or other additional genetic background effects that could also be a result of assortative mating. Irrespectively, our findings indicate that carriers of deletion or duplication of CNV at 16p11.2 who come to the attention of Medical Genetics services are at high risk of psychiatric disorder, and this is of importance for treating clinicians as well as the families themselves. If anything, our estimates represent an underestimate, given that the risks are elevated in our comparison sample of non-carrying familial controls.
Finally, the assessments at all sites were made by experienced clinicians and highly trained and clinically supervised psychologists. However, there were differences in the frequencies of psychiatric diagnoses and ID and although we adjusted for cohort status, we cannot exclude that potentially different diagnostic practices between the sites and countries in this study might have played a role in our findings. Further research is needed to examine psychopathology associated with these CNVs in population-based samples as well as to understand their longitudinal course.
Clinical implications and future directions
This study clearly indicates that the phenotypic effects of the 16p11.2 deletion and duplication extend to include non-ASD psychopathology. The high frequency of psychiatric disorders, especially ADHD, in childhood indicates the need for recognition, diagnosis, and treatment early in development. Longitudinal studies are needed to examine the natural history of these disorders and whether specific types of treatment (e.g., stimulant medication for ADHD) are beneficial37. Not all children met criteria for a psychiatric disorder, supporting previous literature indicating that there is a spectrum of manifestations of the 16p11.2 deletions and duplications7, similar to other CNVs (e.g., 22q11.2DS32).
Future studies could examine the extent to which assortative mating plays a role in psychiatric risk in children from families where a CNV is inherited compared to where it occurs de novo. Further exploration of the extent to which background genetic as well as environmental risk factors contribute to the risk of psychiatric disorder in carriers with a de novo versus an inherited CNV is also important.
Conclusions
We examined the frequency of psychopathology in children with 16p11.2 deletion and duplication. Our findings indicate a high frequency of psychopathology compared to familial controls and suggest the importance of recognition, diagnosis, and intervention in early development. The frequency of psychotic symptoms and ASD is similar in deletion and duplication carriers, indicating that mirrored physical effects of deletion and duplication do not extend to psychopathology.
Change history
05 March 2019
One of the co-authors, Marianne B.M. van den Bree has had her name incorrectly abbreviated by citation manager. It was stated as “Bree MBMVD14”, but has been updated to “van den Bree, M.B.M.” in the HTML, PDF, and XML versions of this article.
References
Weiss, L. A. et al. Association between microdeletion and microduplication at 16p11.2 and autism. N. Engl. J. Med. 358, 667–675 (2008).
D’Angelo, D. et al. Defining the effect of the 16p11. 2 duplication on cognition, behavior, and medical comorbidities. JAMA Psychiatry 73, 20–30 (2016).
Rosenfeld, J. A. et al. Speech delays and behavioral problems are the predominant features in individuals with developmental delays and 16p11.2 microdeletions and microduplications. J. Neurodev. Disord. 2, 26–38 (2010).
Kumar, R. A. et al. Recurrent 16p11.2 microdeletions in autism. Hum. Mol. Genet. 17, 628–638 (2008).
Weiss, L. A. et al. Association between microdeletion and microduplication at 16p11. 2 and autism. N. Engl. J. Med. 358, 667–675 (2008).
Guilmatre, A. et al. Recurrent rearrangements in synaptic and neurodevelopmental genes and shared biologic pathways in schizophrenia, autism, and mental retardation. Arch. Gen. Psychiatry 66, 947–956 (2009).
Glessner, J. T. et al. Autism genome-wide copy number variation reveals ubiquitin and neuronal genes. Nature 459, 569–573 (2009).
Marshall, C. R. et al. Structural variation of chromosomes in autism spectrum disorder. Am. J. Hum. Genet. 82, 477–488 (2008).
Sebat, J. et al. Strong association of de novo copy number mutations with autism. Science 316, 445–449 (2007).
van der Zwaag, B. et al. Gene-network analysis identifies susceptibility genes related to glycobiology in autism. PLoS ONE 4, e5324 (2009).
Shen, Y. et al. Clinical genetic testing for patients with autism spectrum disorders. Pediatrics 125, e727–e735 (2010).
Walsh, K. M. & Bracken, M. B. Copy number variation in the dosage-sensitive 16p11.2 interval accounts for only a small proportion of autism incidence: a systematic review and meta-analysis. Genet. Med. 13, 377–384 (2011).
Rees, E. et al. Analysis of copy number variations at 15 schizophrenia-associated loci. Br. J. Psychiatry 204, 108–114 (2013).
Kirov, G. et al. De novo CNV analysis implicates specific abnormalities of postsynaptic signalling complexes in the pathogenesis of schizophrenia. Mol. Psychiatry 17, 142–153 (2012).
Hanson, E. et al. The cognitive and behavioral phenotype of the 16p11.2 deletion in a clinically ascertained population. Biol. Psychiatry 77, 785–793 (2015).
Hippolyte, L. et al. The number of genomic copies at the 16p11. 2 locus modulates language, verbal memory, and inhibition. Biol. Psychiatry 80, 129–139 (2016).
Shinawi, M. et al. Recurrent reciprocal 16p11.2 rearrangements associated with global developmental delay, behavioural problems, dysmorphism, epilepsy, and abnormal head size. J. Med. Genet. 47, 332–341 (2010).
Zufferey, F. et al. A 600 kb deletion syndrome at 16p11.2 leads to energy imbalance and neuropsychiatric disorders. J. Med. Genet. 49, 660–668 (2012).
Jacquemont, S. et al. Mirror extreme BMI phenotypes associated with gene dosage at the chromosome 16p11.2 locus. Nature 478, 97–102 (2011).
Sacker, A., Done, D. J. & Crow, T. J. Obstetric complications in children born to parents with schizophrenia: a meta-analysis of case-control studies. Psychol. Med. 26, 279–287 (1996).
McNeil, T. F., Cantor-Graae, E. & Ismail, B. Obstetric complications and congenital malformation in schizophrenia. Brain Res. Brain Res. Rev. 31, 166–178 (2000).
Fidler, D. J., Bailey, J. N. & Smalley, S. L. Macrocephaly in autism and other pervasive developmental disorders. Dev. Med. Child Neurol. 42, 737–740 (2000).
Gillberg, C. & De Souza, L. Head circumference in autism, Asperger syndrome, and ADHD: a comparative study. Dev. Med. Child Neurol. 44, 296–300 (2002).
Stefansson, H. et al. CNVs conferring risk of autism or schizophrenia affect cognition in controls. Nature 505, 361–366 (2014).
Crespi, B. & Badcock, C. Psychosis and autism as diametrical disorders of the social brain. Behav. Brain Sci. 31, 241–261 (2008).
Crespi, B., Stead, P. & Elliot, M. Comparative genomics of autism and schizophrenia. Proc. Natl. Acad. Sci. USA. 107(suppl 1), 1736–1741 (2010).
Moreno-De-Luca, A. et al. The role of parental cognitive, behavioral, and motor profiles in clinical variability in individuals with chromosome 16p11. 2 deletions. JAMA Psychiatry 72, 119–126 (2015).
StataCorp. Stata Statistical Software: Release 11 (Statcorp LP, College Station, TX, 2009).
Firth, D. Bias reduction of maximum likelihood estimates. Biometrika 80, 27–38 (1993).
Heinze, G. & Schemper, M. A solution to the problem of separation in logistic regression. Stat. Med. 21, 2409–2419 (2002).
Schneider, M. et al. Psychiatric disorders from childhood to adulthood in 22q11.2 deletion syndrome: results from the International Consortium on Brain and Behavior in 22q11.2 Deletion Syndrome. Am. J. Psychiatry 171, 627–639 (2014).
Niarchou, M. et al. Psychopathology and cognition in children with 22q11.2 deletion syndrome. Br. J. Psychiatry 204, 46–54 (2014).
Hanson, E. et al. Cognitive and behavioral characterization of 16p11.2 deletion syndrome. J. Dev. Behav. Pediatr. 31, 649–657 (2010).
Männik, K. et al. Copy number variations and cognitive phenotypes in unselected populations. JAMA 313, 2044–2054 (2015).
Niarchou, M., Martin, J., Thapar, A., Owen, M. J. & van den Bree, M. The clinical presentation of attention deficit‐hyperactivity disorder (ADHD) in children with 22q11. 2 deletion syndrome. Am. J. Med. Genet. B Neuropsychiatr. Genet. 168, 730–738 (2015).
O’Donovan, M. C., Kirov, G. & Owen, M. J. Phenotypic variations on the theme of CNVs. Nat. Genet. 40, 1392–1393 (2008).
Gothelf, D. et al. Methylphenidate treatment for attention-deficit/hyperactivity disorder in children and adolescents with velocardiofacial syndrome: an open-label study. J. Clin. Psychiatry 64, 1163–1169 (2003).
Angold, A. et al. The Child and Adolescent Psychiatric Assessment (CAPA). Psychol Med. 25, 739–753 (1995).
Goyette, C. H., Conners, C. K. & Ulrich, R. F. Normative data on revised Conners parent and teacher rating scales. J. Abnorm. Child Psychol. 6, 221–236 (1978).
Shaffer, D., Fisher, P., Lucas, C. P., Dulcan, M. K. & Schwab-Stone, M. E. NIMH Diagnostic Interview Schedule for Children Version IV (NIMH DISC-IV): description, differences from previous versions, and reliability of some common diagnoses. J. Am. Acad. Child Adolesc. Psychiatry 39, 28–38 (2000).
Lord, C., Rutter, M. & Couteur, A. Autism Diagnostic Interview-Revised: a revised version of a diagnostic interview for caregivers of individuals with possible pervasive developmental disorders. J. Autism Dev. Disord. 24, 659–685 (1994).
Derogatis, L. R., Lipman, R. S. & Covi, L. SCL-90: an outpatient psychiatric rating scale—premliminary report. Psychopharmacol. Bull. 9, 13–28 (1973).
Hurley, R. S., Losh, M., Parlier, M., Reznick, J. S. & Piven, J. The broad autism phenotype questionnaire. Journal of autism and developmental disorders. 37, 1679–1690 (2017).
Constantino, J. N. et al. Validation of a brief quantitative measure of autistic traits: comparison of the social responsiveness scale with the autism diagnostic interview-revised. J. Autism Dev. Disord. 33, 427–433 (2003).
Acknowledgements
The authors are extremely grateful to all the families that participated in this study as well as to support charity Unique for their help and the research teams. This study was funded by the Wellcome Trust (110222/Z/15/Z) (M.N.), IMAGINE grant (MR/N022572/1 and MR/L011166/1), DEFINE Wellcome Trust Strategic Award, Medical Research Council Centre grant (G0801418), Medical Research Council Programme Grant (G0800509), and the Simons Foundation (Simons VIP).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Niarchou, M., Chawner, S.J.R.A., Doherty, J.L. et al. Psychiatric disorders in children with 16p11.2 deletion and duplication. Transl Psychiatry 9, 8 (2019). https://doi.org/10.1038/s41398-018-0339-8
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41398-018-0339-8
This article is cited by
-
Experiences and concerns of parents of children with a 16p11.2 deletion or duplication diagnosis: a reflexive thematic analysis
BMC Psychology (2024)
-
Evaluation of 100 Dutch cases with 16p11.2 deletion and duplication syndromes; from clinical manifestations towards personalized treatment options
European Journal of Human Genetics (2024)
-
Pervasive alterations of intra-axonal volume and network organization in young children with a 16p11.2 deletion
Translational Psychiatry (2024)
-
Neurocognitive profiles of 22q11.2 and 16p11.2 deletions and duplications
Molecular Psychiatry (2024)
-
Neurodevelopmental disorders and cancer networks share pathways, but differ in mechanisms, signaling strength, and outcome
npj Genomic Medicine (2023)