Abstract
Increased sympathetic noradrenergic signaling is crucially involved in fear and anxiety as defensive states. MicroRNAs regulate dynamic gene expression during synaptic plasticity and genetic variation of microRNAs modulating noradrenaline transporter gene (SLC6A2) expression may thus lead to altered central and peripheral processing of fear and anxiety. In silico prediction of microRNA regulation of SLC6A2 was confirmed by luciferase reporter assays and identified hsa-miR-579-3p as a regulating microRNA. The minor (T)-allele of rs2910931 (MAFcases = 0.431, MAFcontrols = 0.368) upstream of MIR579 was associated with panic disorder in patients (pallelic = 0.004, ncases = 506, ncontrols = 506) and with higher trait anxiety in healthy individuals (pASI = 0.029, pACQ = 0.047, n = 3112). Compared to the major (A)-allele, increased promoter activity was observed in luciferase reporter assays in vitro suggesting more effective MIR579 expression and SLC6A2 repression in vivo (p = 0.041). Healthy individuals carrying at least one (T)-allele showed a brain activation pattern suggesting increased defensive responding and sympathetic noradrenergic activation in midbrain and limbic areas during the extinction of conditioned fear. Panic disorder patients carrying two (T)-alleles showed elevated heart rates in an anxiety-provoking behavioral avoidance test (F(2, 270) = 5.47, p = 0.005). Fine-tuning of noradrenaline homeostasis by a MIR579 genetic variation modulated central and peripheral sympathetic noradrenergic activation during fear processing and anxiety. This study opens new perspectives on the role of microRNAs in the etiopathogenesis of anxiety disorders, particularly their cardiovascular symptoms and comorbidities.
Similar content being viewed by others
Introduction
Anxiety disorders are a group of frequent mental disorders starting early in life and resulting from complex gene-by-environment interactions1,2. Among them, panic disorder (PD) with agoraphobia (AG) is characterized by marked heritability as well as disproportionate generalization of fear to stimuli and contexts not necessarily predictive for actual danger3,4,5. Its clinical syndromes such as panic attacks or anxious apprehension therefore reflect defensive states equivalent to those elicited by actual danger as part of the defensive motivational system as defined by Research Domain Criteria (RDoC)6.
The sympathetic noradrenergic system has repeatedly been linked to fear, anxiety, and panic due to its activation in defensive states7. Symptoms of autonomic arousal and sympathetic noradrenergic activation such as tachycardia, sweating/increased skin conductance, or trembling are observed during acute threat as well as pathological states of fear, including PD8,9. Likewise, symptoms of noradrenergic excess in pheochromocytoma or symptoms elicited by alpha 2-adrenergic receptor antagonist challenge resemble symptoms of sympathetic noradrenergic activation during panic attacks10,11 and reports on increased noradrenaline levels during panic attacks may explain these observations12.
Central noradrenergic signaling affects multiple processes related to the development of anxiety disorders13. Arousal, memory formation, consolidation, and retrieval are involved in defensive responding and fear conditioning14. They have been linked to (pre-)motor cortex, medial prefrontal cortex/anterior cingulate cortex, anterior insula, amygdala, hippocampus, and thalamus function15,16,17. Fine-tuning of these neural systems of the defensive motivational system by the noradrenergic system may therefore represent an intermediate phenotype of altered central noradrenergic signaling during fear processing and sympathetic noradrenergic activation.
The noradrenaline transporter SLC6A2 mediates the reuptake of noradrenaline into presynaptic nerve terminals and is therefore a crucial regulator of the noradrenergic system at the synaptic cleft18. However, studies focusing on genetic variations spanning SLC6A2 failed to show a robust and consistent association with trait anxiety or PD so far19,20,21,22.
In order to bridge the gap between a high heritability but low effect size of single genetic variations, emerging attention has been paid to epigenetic regulation of genes and gene networks23. One important, yet understudied mechanism is posttranscriptional repression of gene expression by microRNAs. MicroRNAs are small, non-coding RNA molecules forming incomplete antisense binding to multiple target mRNAs, counteracting expression of multiple genes, and thereby regulating genes on a genetic network level24,25. Previous studies have demonstrated the role of microRNAs in synaptic plasticity, memory formation, fear conditioning, behavior as well as mental disorders, including PD and related traits26,27,28,29,30,31,32.
We hypothesized that genetic variants of microRNAs regulating SLC6A2 leading to higher microRNA and lower SLC6A2 expression contribute to pathological fear processing in intermediate phenotypes of sympathetic noradrenergic activation and defensive reactivity. For this purpose, we (1) experimentally analyzed which microRNAs regulated SLC6A2 expression, (2) studied which single-nucleotide polymorphisms (SNPs) of microRNA genes regulating SLC6A2 expression were associated with PD and trait anxiety, (3) experimentally analyzed whether the risk genotype modulated expression of its microRNA and whether this microRNA regulated other anxiety candidate genes, and (4) studied whether the risk genotype modulated sympathetic noradrenergic central fear processing and peripheral cardiovascular parameters.
Materials and methods
Luciferase reporter and promoter activity assay
Repression of SLC6A2 expression by microRNAs was analyzed in vitro as previously described32. In short, pEZX-MT01 and -MT06 dual firefly/renilla luciferase reporter vectors (GeneCopoeia, Rockville, USA) containing either the 3’-untranslated region (3'UTR) of human SLC6A2 (HmiT017397-MT01), human GLRB (HmiT007719-MT06), human NPY5R (HmiT011908-MT06), and human HTR2B (HmiT009121-MT06) or no 3’UTR fused to the firefly luciferase (CmiT000001-MT01 or -MT06) were used. Three pmol of small RNA molecules mimicking endogenous microRNAs (mirVana microRNA mimics, Thermo Fisher Scientific, Waltham, USA) were cotransfected along with 40 ng of pEZX-MT01 dual firefly/renilla luciferase reporter vectors containing the 3’UTR of interest in HEK293 cells split into a 96-well plate 4 h prior to transfection with a confluency of about 60%, using the Attractene Transfection Kit (Qiagen, Venlo, Netherlands). Cells were tested for contamination with mycoplasma on a regular basis. Post-transfection, cells were incubated for 40–48 h and luciferase activity was assessed using the LucPair Duo-Luciferase Assay Kit (GeneCopoeia, Rockville, USA) and an EnVision 2104 Multilabel Reader (PerkinElmer, Waltham, MA). Assays were repeated three times in technical triplicates for each microRNA tested in each single experiment. Luciferase activity suppression by each tested microRNA was normalized as follows. (I) Luciferase activity was normalized to the renilla activity of each well and than averaged in technical triplicates (termed relative luciferase activity), thereby normalizing for different transfection efficiencies in different wells. (II) Relative luciferase activity of a microRNA was normalized to the relative luciferase activity of microRNA-untransfected control conditions for the same vector (termed maximal luciferase activity), thereby normalizing for unspecific effects on the cellular level upon cotransfection of a microRNA. (III) Maximal luciferase activity of each microRNA tested on a 3’UTR vector of interest was normalized to the maximal luciferase activity of the same microRNA on a control vector containing no 3’UTR (termed normalized luciferase activity), thereby normalizing for unspecific microRNA binding and effects at other parts of the vector sequence than the 3’UTR of interest.
Regulation of promoter activity by risk genotype of MIR579 rs2910931 was assessed as previously reported33. In brief, single-stranded DNA oligonucleotides containing the different alleles rs2910931 along with a −20/+20 bp upstream/downstream flanking region were tested for modulation of relative luciferase activity using pGL4.23 as the firefly expressing reporter and pGL4.74 as the renilla expressing control (Promega Corporation, Madison, USA). Details of the primer design are given in supplemental methods.
Prediction and validation of microRNA binding at the 3’UTR of SLC6A2
Repression of SLC6A2 gene expression by microRNAs was predicted in silico using TargetScanHuman 6.234, DIANA microT-CDS35, and miRDB36. Predicted microRNAs were validated by means of dual firefly/renilla luciferase reporter assays considering previous results32 when showing either a score <−0.275 for TargetScan (site-specific context score), >0.75 for Diana microT-CDS, or >70 for mirDB. Of the 43 microRNAs tested (supplemental Table 2), 10 microRNAs showed a repression of normalized luciferase activity to <85% and no overlap of their 95% confidence interval (CI) with that of negative control ath-miR-159a, highly suggesting a functional relevance in vivo. These microRNAs were considered to be candidates for further genetic and functional analysis.
Samples
Detailed descriptions of all samples have been published9,16,33,37. Sample characteristics are summarized in supplementary table 1. Briefly, unrelated German PD patients (n = 506, mean age 35.2 ± 10.7 years, 70% female) from the BMBF “Panic-Net” study wave 1 (diagnosis of PD/AG 100%) and wave 2 (diagnosis of PD/AG 87%) were recruited at multiple locations across Germany. Diagnosis was established using the Composite International Diagnostic Interview according to Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition (DSM-IV) criteria38. For genetic association analyses, independent controls (n = 506, mean age 30.5 ± 8.3, 70% female), screened for absence of Axis I disorders by experienced psychologists on the basis of the Mini International Neuropsychiatric Interview according to the criteria of DSM-IV39, were selected from the CRC-TRR-58 MEGA study in order to achieve 1:1 matching for sex and age. Genetic association analyses with dimensional anxiety traits were performed using the Agoraphobic Cognitions Questionnaire (ACQ)40 as well as Anxiety Sensitivity Index (ASI)41 and the complete CRC-TRR-58 MEGA study sample (n = 3112). Individuals with ASI or ACQ scores deviating more than three standard deviations (SDs) from the mean were excluded prior to analysis. For the analysis of functional magnetic resonance imaging (fMRI) in a healthy control sample, genotype information was available in n = 40 of n = 60 participants. Further details concerning this sample have been published42. Data on genotype and the behavioral avoidance test (BAT) were available in n = 276 patients PD/AG patients of the BMBF “Panic-Net” study wave 1. Further details concerning this sample have been published9.
All participant had given their written informed consent according to the Helsinki guidelines in their updated form. The CRC-TRR-58 MEGA study was approved by the Ethics committee of the Medical Faculty of the Julius-Maximilans-University Würzburg (EK 7/08). The BMBF “PanicNet” RCT project was approved by the Ethics Committees of the Medical Faculty of the Technische Universität Dresden (EK 164082006) and the German Psychological Society (AH11.2009) for wave I and II, respectively. Neuroimaging was approved by the Ethics Committee of the Medical Faculty of the Rheinisch-Westfaelische Technische Hochschule University Aachen (EK 073/07).
Genotyping
Genomic DNA of all attendees was extracted from venous blood by a routine desalting method. Genotyping of samples for SNPs of microRNA genes regulating SLC6A2 expression was performed using competitive allele-specific polymerase chain reaction (KASP; LGC Group Ltd., Teddington, UK). All samples were subjected to a stringent quality-control pipeline, accounting for call rates >0.99, Hardy–Weinberg equilibrium (HWE) >0.1, minor allele frequency (MAF) > 0.1, and principal component analysis more than four-fold SD of the first three principal components.
Analysis on the level of central and peripheral systems of fear processing and anxiety
Acquisition of fMRI data in subjects completing a one-session differential fear conditioning and extinction task has been described previously42,43. Briefly, visually presented colored geometrical forms served as conditioned stimulus (CS) during multi-trial familiarization (F), acquisition (A), and extinction (E) phases of the task. White noise adjusted to individual perception of aversiveness served as the unconditioned stimulus (US). The US was pseudorandomly paired with one of the CS during acquisition such that equal proportions of CS+paired and CS+unpaired trials were obtained during acquisition. Only CS+unpaired trials were used for further analyses to avoid confounding between CS+ and US processing. The acquisition and extinction phase were split into halves to assess time-dependent processes. Of n = 60 quality-controlled fMRI datasets, genetic information was available for n = 40 subjects.
Acquisition of BAT data has been described previously9. Briefly, PD/AG patients were asked to stay in a closed and dark test chamber for approximately 10 min, thus inducing agoraphobic anxiety and avoidance behavior. Autonomic (heart rate) and subjective readouts (reported fear) were collected prior, during, and after exposure. Active avoidance (escaping the test chamber) was noted. Patients without AG were excluded owing to the specificity of the test to agoraphobic fear and avoidance. Furthermore, patients with missing subjective and physiological data due to complete avoidance of exposure to the test chamber or technical equipment failures were excluded, resulting in a final sample of 276 patients.
More details are given in supplemental methods.
Statistical analysis
Statistical analyses using Student’s t test were conducted as implemented in Prism 6 (Graph-Pad, La Jolla, USA) or SPSS 24 (IBM, Armonk, USA). Statistical analyses of genotype data were performed using SPSS 24 applying chi-square-tests for deviation from HWE as well as case–control associations of allele or genotype counts and linear regression as well as multivariate analysis of variance (ANOVA) for gene dosage effects on ASI or ACQ. We achieve a power of 63% to detect polymorphisms conveying a relative risk of 1.5 to develop PD assuming a MAF of 0.0544. Correction for n-multiple tests was conducted using Sidák’s approach and corrected p values are given as pc = 1− (1 – p)n. All tests were conducted two sided.
Statistical analysis of fMRI data was conducted as described previously16. On the group level, contrast images for CS+unpaired and CS− of the first and second halves of the acquisition and extinction phase were entered into a flexible factorial design treating subjects as random variables and the fMRI center as a covariate. Contrasts of interest were the main effect of genotype group during first and second halves of acquisition and extinction, as well as the interaction effect of group × CS (CS + unpaired vs. CS−) for each phase. In case of significant F tests, t tests were used to localize the direction of effects. Monte-Carlo simulation was adopted to establish a voxel contiguity threshold to correct for multiple comparisons at the level of p < 0.05 (family-wise error corrected (FWE))45. Assuming an individual voxel type I error of p < 0.005, a cluster extent of 142 contiguous resampled voxels allowed to correct for multiple voxel comparisons at p < 0.05. As this cluster-based threshold might not detect effects in smaller regions, region-of-interest analyses were performed for the amygdala using the automated anatomic labeling atlas to generate two unilateral masks with small volume correction at p < 0.05 FWE-corrected, using a cluster-forming threshold of p < 0.001 uncorrected46. Beta values from significant clusters were extracted and used for bar graph visualization. Detailed information is provided in supplemental methods.
In order to test avoidance behavior during the BAT, the frequency of active avoidance as well as the duration of tolerated exposure in active escapers were analyzed as a function of genotype using chi-square tests and a model of variance. The genotype effect on reported fear and heart rate response was tested applying a mixed model of variance including genotype and avoidance (active vs. no avoidance) as a between-subject factor and BAT phase (anticipation vs. exposure vs. recovery) as a within-subject factor. All p values correspond to two-sided testing.
Results
Association analysis with PD and trait anxiety of SNPs of microRNAs regulating SLC6A2 expression
TagSNPs with a MAF > 0.1 were determined for each of the ten candidate microRNA genes identified by means of luciferase reporter assays (Fig. 1) in a flanking region of 2000 bp upstream and 500 bp downstream47. No SNPs were identified for MIR532, MIR664B, MIR3921, and MIR4781. For the purpose of completeness, rs7194256 located in the 3’UTR of SLC6A2 was also included in order to assess modulation of microRNA binding at the 3’UTR of SLC6A2. The linkage disequilibrium structure is shown in supplementary figure 1 to 6. Genotyping of rs12151009 tagging MIR330 failed quality-control criteria and was excluded. Seventeen SNPs were left for further analyses.
Data show mean repression of normalized firefly luciferase activity upon cotransfection of a dual luciferase reporter vector containing the 3’UTR of SLC6A2 with the microRNA as indicated and 95% confidence intervals. Data were normalized to same-well renilla activity as well as to the activity of a no 3’UTR-containing vector (n = 5 technical triplicates). The 95% confidence intervals of all microRNAs shown were outside the 95% confidence interval of the negative control microRNA ath-miR-159a (95% CI [98.2, 109.7]) and thus considered to be significantly regulating SLC6A2
Case–control association analysis with PD/AG and MAFs for each SNP are given in Table 1. Genotype frequencies of all SNPs resembled those of European reference samples (HapMap CEU and TSI) as well as the 1000Genomes project (MAF(T) = 0.3624), suggesting no confounding by sample- or population-specific effects. The minor (T)-allele of rs2910931 tagging MIR579 was nominally associated with PD/AG (pallelic = 0.004), as was the major (A)-allele of rs2582372 tagging MIR3662A (pallelic = 0.023). Upon correction for multiple testing, the allele count of rs2910931 still showed a trend toward significance (pc = 0.069). Association of rs2910931 with dimensional trait anxiety as analyzed by linear regression adjusted for sex and age showed a significant association between the number of minor (T)-alleles carried and ASI (beta = 0.371, p = 0.029, 95% CI [0.039, 0.702]) as well as ACQ scores (beta = 0.012, p = 0.041, 95% CI [0.000, 0.023]), in line with an additive genetic model. Multiway ANOVA suggested no interaction with sex or dichotomized age.
Regulation of MIR579 promoter activity by rs2910931 and anxiety candidate gene expression by hsa-miR-579-3p
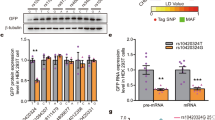
Rs2910931 is located within the putative promoter region 2 kB upstream of MIR579. Assessing promoter activity in vitro by means of luciferase reporter assays revealed a significantly higher relative luciferase activity for the minor (T)-allele compared to the major (A)-allele (Fig. 2a, p = 0.041). This result suggests a higher expression of MIR579 and hsa-miR-579-3p as well as decreased expression of SLC6A2 in vivo.
a Data show mean relative firefly luciferase activity under a minimal promoter sequence containing the (A)- and (T)-allele of rs2910931 upstream of MIR579 as indicated. Data were normalized to same-well renilla activity and are shown as mean and standard error (n = 7 technical triplicates, *p < 0.05 using a two-sided t test). b Data show mean repression of normalized firefly luciferase upon cotransfection with hsa-miR-579-3p and ath-miR159a (negative control) as indicated. Dual luciferase reporter assays contained the 3’UTR of the corresponding receptor genes as indicated. Data were normalized to negative-control-3’UTR relative firefly activity for each microRNA as indicated (n = 5 technical triplicates, *p < 0.05, ***p < 0.005)
Using TargetScan 6.2 and Diana microT-CDS, in silico prediction yielded high scores for 3’UTR binding of hsa-miR-579-3p for GLRB, HTR2B, and NPY5R, in line with regulation of possible anxiety candidate genes33,48,49. A significant repression of luciferase activity upon cotransfection of hsa-miR-579-3p was observed for vectors containing the 3’UTR of HTR2B and NPY5R (Fig. 2b).
Effects of rs2910931 on neural substrates of fear conditioning and extinction in healthy controls
Neural activation during fear conditioning and extinction was assessed by means of fMRI42. Genetic information was available in n = 40 of n = 60 participants. Owing to the limited sample size, carriers of at least one minor (T)-allele were considered to be at higher risk for anxiety-related measures (n = 25), leaving (AA)-carriers in the low-risk group (n = 15). Activation patterns were significantly modulated by rs2910931 as summarized in Table 2. A genotype main effect was observed in the late extinction phase. Post hoc t tests showed that subjects carrying at least one minor (T)-allele exhibited enhanced neural activation in brain regions related to sympathetic noradrenergic activation and fear processing such as the midbrain/periaqueductal gray (PAG), amygdala, and hippocampus, regardless of the CS presented. When carrying no minor (T)-allele, a pronounced deactivation was noted in these regions (Fig. 3a). Moreover, an interaction between genotype and CS presented was observed during the first half of the extinction phase. Minor (T)-allele carriers showed enhanced neural activation of higher-order cortical regions such as the supplementary motor area (SMA) and the middle cingulate gyrus upon presentation of the CS+, while those not carrying any (T)-allele showed enhanced neural activation upon presentation of the CS− (Fig. 3b).
Healthy controls (n = 40) were subjected to an experimental fear conditioning and extinction task. Activation of brain regions was analyzed by means of fMRI as a function of minor (T)-alleles of rs2910931 (TT+AT: n = 25; AA: n = 15). Beta values from significant clusters were extracted and used for bar graph visualization (a.u.). a Activation of midbrain/periaqueductal gray, amygdala, and hippocampus regardless of conditioned stimulus presented during the second half of the extinction phase as a function of rs2910931 genotype group. b Interaction of rs2910931 genotype group with the conditioned stimulus presented during the first half of the extinction phase. *p < 0.05, **p < 0.01, and ***p < 0.001. CS+ conditioned stimulus that was followed by the unconditioned stimulus (US); CS− conditioned stimulus that was never followed by the US
Functional characterization of rs2910931 effects on fear reactivity during the BAT in PD patients
To further corroborate the role of rs2910931 on sympathetic noradrenergic activation, PD patients subjected to the BAT provoking anxious apprehension were evaluated. Homozygotic carriers of (T)-alleles showed a significantly higher heart rate increase from the last minute of the anticipation to the first minute of the exposure phase (Fig. 4; F(2, 270) = 5.47, p = 0.005), irrespective of active avoidance behavior (genotype × behavior F(2, 270) = 0.32, p = 0.73). For AA-carriers, the heart rate increased from 76.70 ± 1.21 min−1 prior to exposure to 80.37 ± 1.63 min−1 upon exposure. AT-carriers showed an increase from 75.87 ± 0.99 to 78.15 ± 1.32 min−1 and TT-carriers from 74.10 ± 1.27 to 82.09 ± 2.01 min−1. During the anticipation and recovery phase, heart rates did not differ between genotype and avoidance groups. Overall active avoidance was significantly associated with higher heart rate reactivity (F(1, 270) = 30.01, p < 0.001), in line with previous findings.
Patients with panic disorder and agoraphobia (n = 276: n(AA) = 95, n(AT) = 129, n(TT) = 52) were subjected to experimental panic exposition using the behavioral avoidance test. Data show the mean difference with standard error of heart rates between the last minute of the anticipation phase and the first minute of the exposure phase during the behavioral avoidance test as a function of rs2910931 genotype. *p < 0.05
Discussion
Regulation of gene expression by microRNAs is an important mechanism in neuronal plasticity. Indeed, the role of microRNAs in mental disorders has become an emerging field of research29,30. MicroRNAs act on gene networks, making candidate gene-based evaluation of microRNAs a promising approach to identify network regulators of high pathogenic relevance. MicroRNA regulation of SLC6A2 expression was probed for several reasons. SLC6A2 is a main regulator of noradrenaline homeostasis by rapidly removing it from the synaptic cleft and the noradrenergic system has been linked with mechanisms of defensive states involved in fear processing and general arousal.
Here we present evidence for the impact of genetic variation of microRNA regulation of SLC6A2 on the RDoC defensive motivational system in fear and anxiety. Our results suggest that (I) the minor (T)-allele of rs2910931 upstream of MIR579 leads to increased expression of hsa-miR-579-3p and more effective repression of SLC6A2 expression along with higher synaptic noradrenaline levels in vivo resulting in (II) higher trait anxiety in healthy individuals possibly due to increased activation of midbrain and limbic areas during fear processing and (III) association with PD mediated by increased sympathetic noradrenergic arousal when entering contexts of potential threat.
Our data suggest that dysbalancing fine-tuning of synaptic noradrenaline homeostasis interferes with successfully establishing fear-inhibitory memory traces and top–down inhibition of defensive responses mediated by brain areas (midbrain/PAG, amygdala) related to sympathetic noradrenergic activation during safety learning17,50,51. Moreover, higher-risk (T)-allele carriers showed enhanced recall of the conditioned fear memory during the first half of extinction training as indicated by stronger activation of brain areas like the SMA, commonly associated with fear expression15. Taken together, both processes result in pathological arousal and may ultimately contribute to anxiety disorders, sharing increased sympathetic noradrenergic signaling as a common mechanism. This hypothesis was corroborated for PD patients by showing increased sympathetic noradrenergic arousal when undergoing the BAT. Homozygous (T)-allele carriers showed a significantly higher heart rate increase upon agoraphobic fear-provoking exposure to the test chamber. This result is in accordance with a pronounced noradrenaline-mediated autonomic fear response, as supported by previous studies10,11,13.
Several limitations apply to our study. While circulating levels of hsa-miR-579 were related to bevacizumab-induced cardiotoxicity52, expression of MIR579 has not yet been described in the human brain53 and no neuronal function has been defined so far. Expression quantitative trait loci have been reported for rs2910931 in skin and thyroid tissue (data obtained from the GTEx portal on 24 July 2018), but not for brain tissue or for MIR57954 as well as no corresponding functional annotation55. However, expression in tissues subject to noradrenergic regulation such as the adrenal gland was reported as well as a high probability of transcription start site modulation in the heart of the region flanking MIR579, thereby further linking MIR579 to noradrenergic signaling55. MIR579 is intronic in the zink finger RNA-binding protein ZFR and polyadenylation was suggested to modulate a negative feedback loop between both56, possibly also relevant at the synapse. We provide additional evidence for a regulatory role of hsa-miR-579-3p at the noradrenergic as well as the serotonergic synapse, by showing regulation of the neuropeptide Y receptor 5 (NPYR5) with neuropeptide Y being a co-transmitter of noradrenaline, and the serotonin receptor 2B (5HTR2B). Our data thus give a first glimpse into molecular mechanisms by which MIR579 may act on endophenotypes as well as clinical phenotypes of fear and anxiety, e.g., by regulating not only SLC6A2 but also other genes involved in fear and anxiety. Future studies adopting next-generation sequencing may give more detailed insight into the relevance of genetic variations at MIR579 and its flanking region as well as the gene network regulated by it. They may also address the exact mechanisms of hsa-miR-579-3p binding at the mRNA in more detail by using binding-site-directed nucleotide mutagenesis, thereby additionally allowing to assess the role of rare genetic variants at these nucleotides. Conservation of MIR579 has only been confirmed among Homo sapiens, Pan troglodytes, Pongo pygmaeus, and Macaca mulatta and its seed sequence in SLC6A2 is only incompletely conserved in more distantly related species, such as mice or rat. Validation of MIR579 functions in mice or rats is therefore not possible. Studies applying cross-linked immunoprecipitation and next-generation sequencing as well as lentivirus-mediated gene overexpression and silencing will allow to identify the gene network regulated by MIR579. Further studies may specifically assess the functional role of rs2910931 by simultaneous quantification of MIR579 and target gene as well as protein expression levels in postmortem brain tissue, neuronal stem cells, or human heterologous expression systems. Although genetic association of rs2910931 with the categorical phenotype PD kept a trend toward significance upon correction for multiple testing and was supported by the association with dimensional anxiety traits, these results need to be considered exploratory. Limited power of the sample in light of the small effect sizes of single genetic variations may account for this, making replication of study results in larger samples a prerequisite to draw final conclusions. Nevertheless, the consistent association with functional central and peripheral endophenotypes of defensive states such as fear conditioning and extinction as well as heart rate support a role in the pathophysiology of fear and anxiety.
Our observations complement a recent report that rs7194256 within the 3’UTR of SLC6A2 regulating binding of hsa-miR-19a-3p was associated with elevated anxiety measures, arterial noradrenaline levels, depression scores, larger left ventricular mass index, heart rate, as well as higher systolic and diastolic blood pressure levels in healthy controls and patients with affective (depression and PD) and cardiovascular disease57. While we failed to observe an association of rs7194256 with trait anxiety or PD, our results share the same direction of effects concerning PD, trait anxiety, and sympathetic noradrenergic endophenotypes for rs2910931 and hsa-miR-579-3p. They add to the observations of Marques and co-workers57 by providing evidence for parallel effects of microRNA regulation of SLC6A2 on central and peripheral sympathetic noradrenergic endophenotypes.
In conclusion, microRNA regulation of SLC6A2 may contribute to the pathophysiology of fear and anxiety not necessarily by increased basic pathological anxiety but rather by modulating reactions of fear and flight. These reactions are related to increased sympathetic noradrenergic activation, which may represent the common link between anxiety disorders and their cardiovascular symptoms as well as comorbid cardiovascular disease57,58,59,60,61. Future studies addressing mechanisms of hsa-miR-579-3p action and its role in clinical cohorts of anxiety and cardiovascular disorders including therapy studies have to further corroborate these hypotheses. As such, studies on microRNAs open up new perspectives on common mechanisms of comorbid disorders and novel therapeutic approaches.
References
Craske, M. G. & Stein, M. B. Anxiety. Lancet 388, 3048–3059 (2016).
Eley, T. C. et al. The intergenerational transmission of anxiety: a Children-of-Twins Study. Am. J. Psychiatry 172, 630–637 (2015).
Howe, A. S. et al. Candidate genes in panic disorder: meta-analyses of 23 common variants in major anxiogenic pathways. Mol. Psychiatry 21, 665–679 (2016).
Mineka, S. & Zinbarg, R. A contemporary learning theory perspective on the etiology of anxiety disorders: it’s not what you thought it was. Am. Psychol. 61, 10–26 (2006).
Kindt, M. A behavioural neuroscience perspective on the aetiology and treatment of anxiety disorders. Behav. Res. Ther. 62, 24–36 (2014).
Hamm, A. O. et al. Panic disorder with agoraphobia from a behavioral neuroscience perspective: Applying the research principles formulated by the Research Domain Criteria (RDoC) initiative. Psychophysiology 53, 312–322 (2016).
Davies, S. J. C., Esler, M. & Nutt, D. J. Anxiety--bridging the heart/mind divide. J. Psychopharmacol. 24, 633–638 (2010).
Alpers, G. W., Wilhelm, F. H. & Roth, W. T. Psychophysiological assessment during exposure in driving phobic patients. J. Abnorm. Psychol. 114, 126–139 (2005).
Richter, J. et al. Dynamics of defensive reactivity in patients with panic disorder and agoraphobia: implications for the etiology of panic disorder. Biol. Psychiatry 72, 512–520 (2012).
Bremner, J. D., Krystal, J. H., Southwick, S. M. & Charney, D. S. Noradrenergic mechanisms in stress and anxiety: I. Preclinical studies. Synapse 23, 28–38 (1996).
Bremner, J. D., Krystal, J. H., Southwick, S. M. & Charney, D. S. Noradrenergic mechanisms in stress and anxiety: II. Clinical studies. Synapse 23, 39–51 (1996).
Bandelow, B. et al. Urinary excretion of cortisol, norepinephrine, testosterone, and melatonin in panic disorder. Pharmacopsychiatry 30, 113–117 (1997).
Kalk, N. J., Nutt, D. J. & Lingford-Hughes, A. R. The role of central noradrenergic dysregulation in anxiety disorders: evidence from clinical studies. J. Psychopharmacol. 25, 3–16 (2011).
Charney, D. S. Neuroanatomical circuits modulating fear and anxiety behaviors. Acta Psychiatr. Scand. Suppl. 108, 38–50 (2003).
Fullana, M. A. et al. Neural signatures of human fear conditioning: an updated and extended meta-analysis of fMRI studies. Mol. Psychiatry 21, 500–508 (2016).
Lueken, U. et al. Modulation of defensive reactivity by GLRB allelic variation: converging evidence from an intermediate phenotype approach. Transl. Psychiatry 7, e1227 (2017).
Tovote, P., Fadok, J. P. & Lüthi, A. Neuronal circuits for fear and anxiety. Nat. Rev. Neurosci. 16, 317–331 (2015).
Torres, G. E., Gainetdinov, R. R. & Caron, M. G. Plasma membrane monoamine transporters: structure, regulation and function. Nat. Rev. Neurosci. 4, 13–25 (2003).
Sand, P. G. et al. Norepinephrine transporter gene (NET) variants in patients with panic disorder. Neurosci. Lett. 333, 41–44 (2002).
Lee, Y. J. et al. Norepinephrine transporter (NET) promoter and 5’-UTR polymorphisms: association analysis in panic disorder. Neurosci. Lett. 377, 40–43 (2005).
Buttenschøn, H. N. et al. The norepinephrine transporter gene is a candidate gene for panic disorder. J. Neural Transm. 118, 969–976 (2011).
Stein, M. B. et al. Influence of RGS2 on sertraline treatment for social anxiety disorder. Neuropsychopharmacology 39, 1340–1346 (2014).
Schiele, M. A. & Domschke, K. Epigenetics at the crossroads between genes, environment and resilience in anxiety disorders. Genes Brain Behav. 4, e443 (2017).
Ambros, V. The functions of animal microRNAs. Nature 431, 350–355 (2004).
Lim, L. P. et al. Microarray analysis shows that some microRNAs downregulate large numbers of target mRNAs. Nature 433, 769–773 (2005).
Schratt, G. M. microRNAs at the synapse. Nat. Rev. Neurosci. 10, 842–849 (2009).
Volk, N. et al. MicroRNA-19b associates with Ago2 in the amygdala following chronic stress and regulates the adrenergic receptor beta 1. J. Neurosci. 34, 15070–15082 (2014).
Jovasevic, V. et al. GABAergic mechanisms regulated by miR-33 encode state-dependent fear. Nat. Neurosci. 18, 1265–1271 (2015).
Geaghan, M. & Cairns, M. J. MicroRNA and posttranscriptional dysregulation in psychiatry. Biol. Psychiatry 78, 231–239 (2015).
Issler, O. & Chen, A. Determining the role of microRNAs in psychiatric disorders. Nat. Rev. Neurosci. 16, 201–212 (2015).
Muiños-Gimeno, M. et al. Human microRNAs miR-22, miR-138-2, miR-148a, and miR-488 are associated with panic disorder and regulate several anxiety candidate genes and related pathways. Biol. Psychiatry 69, 526–533 (2011).
Hommers, L. G. et al. MicroRNA hsa-miR-4717-5p regulates RGS2 and may be a risk factor for anxiety-related traits. Am. J. Med. Genet. B Neuropsychiatr. Genet. 168B, 296–306 (2015).
Deckert, J. et al. GLRB allelic variation associated with agoraphobic cognitions, increased startle response and fear network activation: a potential neurogenetic pathway to panic disorder. Mol. Psychiatry 22, 1431–1439 (2017).
Grimson, A. et al. MicroRNA targeting specificity in mammals: determinants beyond seed pairing. Mol. Cell 27, 91–105 (2007).
Paraskevopoulou, M. D., et al. DIANA-microT web server v5.0: service integration into miRNA functional analysis workflows. Nucleic Acids Res. 41, W169–W173 (2013).
Wang, X. & Naqa, El. I. M. Prediction of both conserved and nonconserved microRNA targets in animals. Bioinformatics 24, 325–332 (2008).
Gloster, A. T. et al. Psychological treatment for panic disorder with agoraphobia: a randomized controlled trial to examine the role of therapist-guided exposure in situ in CBT. J. Consult. Clin. Psychol. 79, 406–420 (2011).
Wittchen, H.-U. & Pfister, H. DIA-X Interview (Swets & Zeitlinger, Frankfurt, 1997).
Sheehan, D. V. et al. The Mini-International Neuropsychiatric Interview (M.I.N.I.): the development and validation of a structured diagnostic psychiatric interview for DSM-IV and ICD-10. J. Clin. Psychiatry 59(Suppl 20), 22–33 (1998).
Chambless, D. L., Caputo, G. C., Bright, P. & Gallagher, R. Assessment of fear of fear in agoraphobics: the body sensations questionnaire and the agoraphobic cognitions questionnaire. J. Consult. Clin. Psychol. 52, 1090–1097 (1984).
Reiss, S., Peterson, R. A., Gursky, D. M. & McNally, R. J. Anxiety sensitivity, anxiety frequency and the prediction of fearfulness. Behav. Res. Ther. 24, 1–8 (1986).
Kircher, T. et al. Effect of cognitive-behavioral therapy on neural correlates of fear conditioning in panic disorder. Biol. Psychiatry 73, 93–101 (2013).
Büchel, C., Morris, J., Dolan, R. J. & Friston, K. J. Brain systems mediating aversive conditioning: an event-related fMRI study. Neuron 20, 947–957 (1998).
Menashe, I., Rosenberg, P. S. & Chen, B. E. PGA: power calculator for case-control genetic association analyses. BMC Genet. 9, 36 (2008).
Slotnick, S. D., Moo, L. R., Segal, J. B. & Hart, J. Distinct prefrontal cortex activity associated with item memory and source memory for visual shapes. Brain Res. Cogn. Brain Res. 17, 75–82 (2003).
Tzourio-Mazoyer, N. et al. Automated anatomical labeling of activations in SPM using a macroscopic anatomical parcellation of the MNI MRI single-subject brain. Neuroimage 15, 273–289 (2002).
Xu, Z. & Taylor, J. A. SNPinfo: integrating GWAS and candidate gene information into functional SNP selection for genetic association studies. Nucleic Acids Res. 37, W600–W605 (2009).
Domschke, K. et al. Chromosome 4q31-34 panic disorder risk locus: association of neuropeptide Y Y5 receptor variants. Am. J. Med. Genet. B Neuropsychiatr. Genet. 147B, 510–516 (2008).
Maron, E., Hettema, J. M. & Shlik, J. Advances in molecular genetics of panic disorder. Mol. Psychiatry 15, 681–701 (2010).
Mobbs, D. et al. From threat to fear: the neural organization of defensive fear systems in humans. J. Neurosci. 29, 12236–12243 (2009).
Milad, M. R. & Quirk, G. J. Neurons in medial prefrontal cortex signal memory for fear extinction. Nature 420, 70–74 (2002).
Zhao, Z. et al. Dysregulated miR1254 and miR579 for cardiotoxicity in patients treated with bevacizumab in colorectal cancer. Tumour Biol. 35, 5227–5235 (2014).
Ziats, M. N. & Rennert, O. M. Identification of differentially expressed microRNAs across the developing human brain. Mol. Psychiatry 19, 848–852 (2014).
Huan, T. et al. Genome-wide identification of microRNA expression quantitative trait loci. Nat. Commun. 6, 6601 (2015).
Pazin, M. J. Using the ENCODE resource for functional annotation of genetic variants. Cold Spring Harb. Protoc. 2015, 522–536 (2015).
Hinske, L. C. et al. Alternative polyadenylation allows differential negative feedback of human miRNA miR-579 on its host gene ZFR. PLoS ONE 10, e0121507 (2015).
Marques, F. Z. et al. A polymorphism in the norepinephrine transporter gene is associated with affective and cardiovascular disease through a microRNA mechanism. Mol. Psychiatry 22, 134–141 (2017).
Tully, P. J., Harrison, N. J., Cheung, P. & Cosh, S. Anxiety and cardiovascular disease risk: a review. Curr. Cardiol. Rep. 18, 120 (2016).
Meuret, A. E., Kroll, J. & Ritz, T. Panic disorder comorbidity with medical conditions and treatment implications. Annu. Rev. Clin. Psychol. 13, 209–240 (2017).
Esler, M. & Kaye, D. Sympathetic nervous system activation in essential hypertension, cardiac failure and psychosomatic heart disease. J. Cardiovasc. Pharmacol. 35, S1–S7 (2000).
Alvarenga, M. E., Richards, J. C., Lambert, G. & Esler, M. D. Psychophysiological mechanisms in panic disorder: a correlative analysis of noradrenaline spillover, neuronal noradrenaline reuptake, power spectral analysis of heart rate variability, and psychological variables. Psychosom. Med. 68, 8–16 (2006).
Acknowledgements
We are grateful to all individuals who participated in this study either as part of the CRC-TRR-58 Mega study wave 1 and 2 or the German PanicNet wave 1 (multicenter trial ‘Mechanisms of Action in CBT (MAC)’) or wave 2 studies. We are grateful for the excellent technical help provided by Alexandra Bohl, Inge Reck, and Birgit Thur. The study was supported by the Interdisciplinary Center of Clinical Research Würzburg N-258 to L.G.H. and by DFG CRC-TRR-58 grants Z02 to J.D., A.R., M.R., and P.P., B01 to P.P., B03 to C.B., B06 to A.R. and C.B., and C02 to K.D. and J.D. B.S. is supported by DFG grant STR 1146/8-1. This work is part of the German multicenter trial “Mechanisms of Action in CBT (MAC)”. The study was funded by the German Federal Ministry of Education and Research (BMBF; project no. 01GV0615) as part of the BMBF Psychotherapy Research Funding Initiative. Principal investigators (PI) with respective areas of responsibility in the MAC study are V. Arolt (Münster: Overall MAC Program Coordination), H.U. Wittchen (Dresden: Principal. Investigator (PI) for the Randomized Clinical Trial and Manual Development), A. Hamm (Greifswald: PI for Psychophysiology), A.L. Gerlach (Münster: PI for Psychophysiology and Panic subtypes), A. Ströhle (Berlin: PI for Experimental Pharmacology), T. Kircher (Marburg: PI for functional neuroimaging), and J. Deckert (Würzburg: PI for Genetics). Additional site directors in the RCT component of the program are G.W. Alpers (Würzburg), T. Fydrich and L. Fehm (Berlin-Adlershof), and T. Lang (Bremen). Acknowledgements and staff members by site: Greifswald (coordinating site for Psychophysiology): Christiane Pané-Farré, Jan Richter, Susan Richter, Matthias von Rad; Berlin-Charité (coordinating Center for Experimental Pharmacology): Harald Bruhn, Anja Siegmund, Meline Stoy, André Wittmann; Berlin-Adlershof: Irene Schulz; Münster (Overall MAC Program Coordination, Genetics and Functional Neuroimaging): Andreas Behnken, Katharina Domschke, Adrianna Ewert, Carsten Konrad, Bettina Pfleiderer, Christina Uhlmann, Peter Zwanzger; Münster (coordinating site for psychophysiology and subtyping): Judith Eidecker, Swantje Koller, Fred Rist, Anna Vossbeck-Elsebusch; Marburg/Aachen (coordinating center for functional neuroimaging): Barbara Drüke, Sonja Eskens, Thomas Forkmann, Siegfried Gauggel, Susan Gruber, Andreas Jansen, Thilo Kellermann, Isabelle Reinhardt, Nina Vercamer-Fabri; Dresden (coordinating site for data collection, analysis, and the RCT): Franziska Einsle, Christine Froehlich, Andrew T. Gloster, Christina Hauke, Simone Heinze, Michael Hoefler, Ulrike Lueken, Peter Neudeck, Stephanie Preiß, Dorte Westphal; Würzburg Psychiatry Department (coordinating center for genetics): Andreas Reif, Caro Gagel; Würzburg Psychology Department: Julia Duerner, Hedwig Eisenbarth, Antje B. M. Gerdes, Harald Krebs, Paul Pauli, Silvia Schad, Nina Steinhäuser; Bremen: Veronika Bamann, Sylvia Helbig-Lang, Anne Kordt, Pia Ley, Franz Petermann, Eva-Maria Schroeder. Additional support was provided by the coordinating center for clinical studies in Dresden (KKS Dresden): Xina Graehlert and Marko Käppler. This work is also part of the German multicenter trial: Mechanisms of CBT-treatment effects in patients with panic disorder and panic disorder with AG: The role of interoceptive exposure and fear augmentation (MCBT-PDAS). The study is funded by the German Federal Ministry of Education and Research (BMBF, 01GV0614) as part of the larger BMBF Psychotherapy Research Funding Initiative Improving the Treatment of Panic Disorder. Principal investigators (PI) with respective areas of concentration of the MCBT-PDAS are Alfons Hamm (Greifswald: PI Psychophysiology); Thomas Lang (Bremen: Study Director for the Randomized Clinical Trial (RCT) and Manual Development); Alexander L. Gerlach (Münster: PI Panic subtypes); Georg W. Alpers (Mannheim: PI Ambulatory assessment); Christiane Pané-Farré (Greifswald: PI Psychophysiology and Panic Disorder); Tilo Kircher (Marburg: PI for functional neuroimaging), and Jürgen Deckert (Würzburg: PI for Genetics). Additional site directors in the RCT component of the program are Winfried Rief (Marburg), and Paul Pauli (Würzburg). Centers of the Research Network: Volker Arolt (Münster: Overall Network Coordination), Hans-Ulrich Wittchen (Dresden), Andreas Ströhle (Berlin). Acknowledgements and staff members by site: Bremen (coordinating center for the multicenter trial): Veronika Bamann, Sandra Cammin, Sarah Czilwik, Kira Geisler, Sylvia Helbig-Lang, Kirsten Helmes, Anne Kordt, Tanja Leonhard, Mila Plett-Perelshteyn, Christian Soltau, Juliane Sülz, Maxie von Auer; Greifswald (coordinating site for psychophysiology): Anett Hoffmann, Jan Richter; Mannheim (coordinating center for ambulatory assessment): Christoph Biwer, Elisabeth Borgmann, Antje Gerdes, Otto Martin, Kristina Steinbach, Bettina Stemmler, Andrew White; Marburg (coordinating center for functional neuroimaging): Tobias Fehlinger, Andreas Jansen, Nikita Jegan, Carsten Konrad, Marion Mickeler, Silke Rusch, Katrin Schlötterer, Benjamin Straube, Mareike Stumpenhorst, Katrin Wambach, Yunbo Yang; Münster (coordinating site for panic subtypes): Susanne Kettler, Anna Vossbeck-Elsebusch; Würzburg Psychiatry Department (coordinating center for genetics): Carola Gagel, Andreas Reif, Heike Weber; Würzburg Psychology Department: Almut Friedl-Huber, Harald Krebs, Caroline Ott, Nina Steinhäuser; Additional support was provided by the coordinating center for clinical studies in Dresden (KKS Dresden): Marko Käppler. The study was registered with the NCT01323556.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
T.K. received fees for educational programs from Janssen-Cilag, Eli Lilly, Servier, Lundbeck, Bristol Myers Squibb, Pfizer, and Astra-Zeneca; travel support/sponsorship for congresses from Servier; speaker’s honoraria from Janssen-Cilag; and research grants from Pfizer and Lundbeck. H.-U.W. has been a member of advisory boards of several pharmaceutical companies. He received travel reimbursements and research grant support from Essex Pharma, Sanofi, Pfizer, Organon, Servier, Novartis, Lundbeck, and Glaxo Smith Kline. V.A. is a member of advisory boards and/or gave presentations for the following companies: Astra-Zeneca, Janssen-Organon, Lilly, Lundbeck, Servier, Pfizer, and Wyeth. He also received research grants from Astra-Zeneca, Lundbeck, and Servier. He chaired the committee for the “Wyeth Research Award Depression and Anxiety”. A.S. received research from Lundbeck and speaker honoraria from AstraZeneca, Boehringer Ingelheim, Eli Lilly & Co, Lundbeck, Pfizer, Wyeth, and UCB. Educational grants were given by the Boehringer Ingelheim Fonds and the Eli Lilly International Foundation. A.R. has received a research grant from Medice and speaker’s honoraria from Medice and neuraxpharm. The other authors declare that they have no conflict of interest.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Hommers, L.G., Richter, J., Yang, Y. et al. A functional genetic variation of SLC6A2 repressor hsa-miR-579-3p upregulates sympathetic noradrenergic processes of fear and anxiety. Transl Psychiatry 8, 226 (2018). https://doi.org/10.1038/s41398-018-0278-4
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41398-018-0278-4
This article is cited by
-
Regulation of the Glycine Transporter GLYT1 by microRNAs
Neurochemical Research (2022)