Abstract
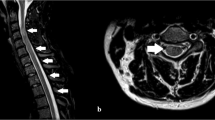
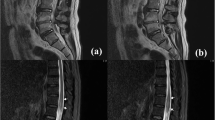
This is a case of acute onset unilateral Bell’s Palsy during COVID-19 illness, coinciding with development of progressive leg pain, weakness, and sensation change. The patient was ultimately found to have a large B-cell lymphoma mass invading the sciatic nerve, lumbosacral plexus and the spinal canal with compression of cauda equina consistent with neurolymphomatosis. Although COVID-19 infection has been associated with Bell’s palsy, Bell’s palsy has also been reported with lymphoid malignancy. We review current literature on the association of Bell’s palsy with COVID-19 infection and lymphoid malignancy, as well as review the diagnostic challenges of neurolymphomatosis. Providers should be aware of the possible association of Bell’s palsy as harbinger of lymphoid malignancy.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 1 print issues and online access
We are sorry, but there is no personal subscription option available for your country.
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Baugh RF, Basura GJ, Ishii LE, Schwartz SR, Drumheller CM, Burkholder R, et al. Clinical practice guideline: Bell’s palsy. Otolaryngol Neck Surg. 2013;149:S1–27.
Tamaki A, Cabrera CI, Li S, Rabbani C, Thuener JE, Rezaee RP, et al. Incidence of Bell palsy in patients with COVID-19. JAMA Otolaryngol Head Neck Surg. 2021;147:767–8. http://www.ncbi.nlm.nih.gov/pubmed/34165518.
Baden LR, El Sahly HM, Essink B, Kotloff K, Frey S, Novak R, et al. Efficacy and safety of the mRNA-1273 SARS-CoV-2 vaccine. N Engl J Med. 2021;384:403–16. http://www.nejm.org/doi/10.1056/NEJMoa2035389.
Gupta S, Jawanda MK, Taneja N, Taneja T. A systematic review of Bell’s Palsy as the only major neurological manifestation in COVID-19 patients. J Clin Neurosci. 2021;90:284–92.
Neo WL, Ng JCF, Iyer NG. The great pretender-Bell’s palsy secondary to SARS-CoV-2? Clin Case Rep. 2021;9:1175–7. https://pubmed.ncbi.nlm.nih.gov/33768805.
Islamoglu Y, Celik B, Kiris M. Facial paralysis as the only symptom of COVID-19: a prospective study. Am J Otolaryngol. 2021;42:102956.
Egilmez OK, Gündoğan ME, Yılmaz MS, Güven M. Can COVID-19 cause peripheral facial nerve palsy? SN Compr Clin Med. 2021;1–7. http://www.ncbi.nlm.nih.gov/pubmed/34056546.
Mutlu A, Kalcioglu MT, Gunduz AY, Bakici B, Yilmaz U, Cag Y. Does the SARS-CoV-2 pandemic really increase the frequency of peripheral facial palsy? Am J Otolaryngol. 2020;42:103032. http://www.ncbi.nlm.nih.gov/pubmed/33857779.
Martin-Villares C, Alba JR, Gonzalez-Gimeno MJ. Data from 235 cases of Bell’s palsy during COVID-19 pandemic: were there clusters of facial palsy? Neuroepidemiology. 2021;55:495–6. http://www.ncbi.nlm.nih.gov/pubmed/34515163.
Cartwright RA, Boddy J, Barnard D, Bernard S, Bird CC, Roberts BE, et al. Association between Bell’s palsy and lymphoid malignancies. Leuk Res. 1985;9:31–3.
Corringham RET, Ho AD. Bell’s palsy as a sign of Burkitt’s lymphoma in children. Blood. 1995;86:2052.
Bilavsky E, Scheuerman O, Marcus N, Hoffer V, Garty BZ. Facial paralysis as a presenting symptom of leukemia. Pediatr Neurol. 2006;34:502–4.
Walsh PS, Gray JM, Ramgopal S, Lipshaw MJ. Risk of malignancy following emergency department Bell’s palsy diagnosis in children. Am J Emerg Med. 2021;53:63–7. http://www.ncbi.nlm.nih.gov/pubmed/34992025.
Cheng J, Hashem MA, Barabé F, Cloutier S, Xi L, Raffeld M, et al. CCND1 genomic rearrangement as a secondary event in high grade B-cell lymphoma. HemaSphere. 2021;5:e505.
Grisariu S, Avni B, Batchelor TT, van den Bent MJ, Bokstein F, Schiff D, et al. Neurolymphomatosis: an International Primary CNS Lymphoma Collaborative Group report. Blood. 2010;115:5005–11. http://www.ncbi.nlm.nih.gov/pubmed/20368468.
Avila JD, Vivar C. Neurolymphomatosis: a review of 82 cases (P5.141). Neurology. 2017;88:P5.141.
Gan HK, Azad A, Cher L, Mitchell PLR. Neurolymphomatosis: diagnosis, management, and outcomes in patients treated with rituximab. Neuro Oncol. 2010;12:212–5.
Campagnolo M, Cacciavillani M, Cavallaro T, Ferrari S, Gasparotti R, Zambello R, et al. Neurolymphomatosis, a rare manifestation of peripheral nerve involvement in lymphomas: Suggestive features and diagnostic challenges. J Peripher Nerv Syst. 2020;25:312–5. http://www.ncbi.nlm.nih.gov/pubmed/32627254.
Jeong J, Kim SW, Sung DH. Neurolymphomatosis: a single-center experience of neuromuscular manifestations, treatments, and outcomes. J Neurol. 2021;268:851–9. http://www.ncbi.nlm.nih.gov/pubmed/33098033.
DeVries AH, Howe BM, Spinner RJ, Broski SM. B-cell peripheral neurolymphomatosis: MRI and 18F-FDG PET/CT imaging characteristics. Skelet Radio. 2019;48:1043–50. http://www.ncbi.nlm.nih.gov/pubmed/30666391.
Shree R, Goyal MK, Modi M, Gaspar BL, Radotra BD, Ahuja CK, et al. The diagnostic dilemma of neurolymphomatosis. J Clin Neurol. 2016;12:274–81.
Abe Y, Usui Y, Narita K, Takeuchi M, Matsue K. Clinical features, diagnosis, and prognosis of 14 cases of neurolymphomatosis: single institutional experience over 10 years. Blood. 2016;128:3042.
Author information
Authors and Affiliations
Contributions
ZP contributed to idea, patient work-up and evaluation, initial write-up, editing and final submission, SO contributed to chart review, literature review, write-up, creation of figure and table, editing and final submission.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ong, S., Petrin, Z. COVID-19 associated Bell’s Palsy and lumbosacral neurolymphomatosis in a patient with B-cell lymphoma—Case Report. Spinal Cord Ser Cases 9, 21 (2023). https://doi.org/10.1038/s41394-023-00580-8
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41394-023-00580-8