Abstract
Background
Increasing evidence indicates an association between statins and reduced prostate cancer-specific mortality (PCSM). However, significant bias may exist in these studies. One particularly challenging bias to assess is the healthy user effect, which may be quantified by screening patterns. We aimed to evaluate the association between statin use, screening, and PCSM in a dataset with detailed longitudinal information.
Methods
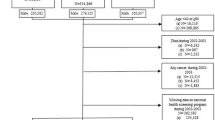
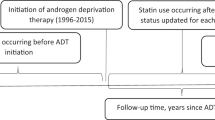
We used the Veterans Affairs Informatics and Computing Infrastructure to assemble a cohort of patients diagnosed with prostate cancer (PC) between 2000 and 2015. We collected patient-level demographic, comorbidity, and tumor data. We also assessed markers of preventive care utilization including cholesterol and prostate specific antigen (PSA) screening rates. Patients were considered prediagnosis statin users if they had at least one prescription one or more years prior to PC diagnosis. We evaluated PCSM using hierarchical Fine-Gray regression models and all-cause mortality (ACM) using a cox regression model.
Results
The final cohort contained 68,432 men including 40,772 (59.6%) prediagnosis statin users and 27,660 (40.4%) nonusers. Prediagnosis statin users had higher screening rates than nonusers for cholesterol (90 vs. 69%, p < 0.001) and PSA (76 vs. 67%, p < 0.001). In the model which excluded screening, prediagnosis statin users had improved PCSM (SHR 0.90, 95% CI 0.84–0.97; p = 0.004) and ACM (HR 0.96, 95% CI 0.93–0.99; p = 0.02). However, after including cholesterol and PSA screening rates, prediagnosis statin users and nonusers showed no differences in PCSM (SHR 0.98, 95% CI 0.91–1.06; p = 0.59) or ACM (HR 1.02, 95% CI 0.98–1.05; p = 0.25).
Conclusion
We found that statin users tend to have more screening than nonusers. When we considered screening utilization, we observed no relationship between statin use before a prostate cancer diagnosis and prostate cancer mortality.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 4 print issues and online access
$259.00 per year
only $64.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Nielsen SF, Nordestgaard BG, Bojesen SE. Statin use and reduced cancer-related mortality. N Engl J Med. 2012;367:1792–802. https://doi.org/10.1056/NEJMoa1201735.
Joentausta RM, Rannikko A, Murtola TJ. Prostate cancer survival among statin users after prostatectomy in a Finnish nationwide cohort. Prostate. 2019. https://doi.org/10.1002/pros.23768.
Larsen SB, Dehlendorff C, Skriver C, Dalton SO, Jespersen CG, Borre M, et al. Postdiagnosis statin use and mortality in danish patients with prostate cancer. J Clin Oncol. 2017;35:3290–7. https://doi.org/10.1200/JCO.2016.71.89814.
Boudreau DM, Yu O, Johnson J. Statin use and cancer risk: a comprehensive review. Expert Opin Drug Saf. 2010;9:603–21. https://doi.org/10.1517/14740331003662620.
Altwairgi AK. Statins are potential anticancerous agents (review). Oncol Rep. 2015;33:1019–39. https://doi.org/10.3892/or.2015.3741.
Chubak J, Boudreau DM, Wirtz HS, McKnight B, Weiss NS. Threats to validity of nonrandomized studies of postdiagnosis exposures on cancer recurrence and survival. J Natl Cancer Inst. 2013;105:1456–62. https://doi.org/10.1093/jnci/djt211.
Shrank WH, Patrick AR, Brookhart MA. Healthy user and related biases in observational studies of preventive interventions: a primer for physicians. J Gen Intern Med. 2011;26:546–50. https://doi.org/10.1007/s11606-010-1609-1.
Emilsson L, García-Albéniz X, Logan RW, Caniglia EC, Kalager M, Hernán MA. Examining bias in studies of statin treatment and survival in patients with cancer. JAMA Oncol. 2018;4:63. https://doi.org/10.1001/jamaoncol.2017.2752.
Park HS, Schoenfeld JD, Mailhot RB, Shive M, Hartman RI, Ogembo R, et al. Statins and prostate cancer recurrence following radical prostatectomy or radiotherapy: a systematic review and meta-analysis. Ann Oncol. 2013;24:1427–34. https://doi.org/10.1093/annonc/mdt077.
Scosyrev E, Tobis S, Donsky H, Wu G, Joseph J, Rashid H, et al. Statin use and the risk of biochemical recurrence of prostate cancer after definitive local therapy: a meta-analysis of eight cohort studies. BJU Int. 2013;111:E71–7. https://doi.org/10.1111/j.1464-410X.2012.11527.x.
Aminsharifi A, Howard LE, Amling CL, Aronson WJ, Cooperberg MR, Kane CJ, et al. Statins are associated with increased biochemical recurrence after radical prostatectomy in diabetic men but no association was seen in men also taking metformin: results from the SEARCH database. Clin Genitourin Cancer. 2019;17:e140–9. https://doi.org/10.1016/j.clgc.2018.09.020.
Charlson ME, Pompei P, Ales KL, MacKenzie CR. A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis. 1987;40:373–83. http://www.ncbi.nlm.nih.gov/pubmed/3558716. Accessed 28 Jul 2019.
Quan H, Sundararajan V, Halfon P, Fong A, Burnand B, Luthi JC, et al. Coding algorithms for defining comorbidities in ICD-9-CM and ICD-10 administrative data. Med Care. 2005;43:1130–9. http://www.ncbi.nlm.nih.gov/pubmed/16224307. Accessed 28 Jul 2019.
Klabunde CN, Potosky AL, Legler JM, Warren JL. Development of a comorbidity index using physician claims data. J Clin Epidemiol. 2000;53:1258–67. http://www.ncbi.nlm.nih.gov/pubmed/11146273. Accessed 28 Jul 2019.
Anderson-Carter I, Posielski N, Liou J, Khemees T, Downs T, Abel J, et al. The impact of statins in combination with androgen deprivation therapyin patients with advanced prostate cancer: a large observational study. Urol Oncol. 2019;37:130–7. https://doi.org/10.1016/J.UROLONC.2018.11.017.
Mucci LA, Stampfer MJ. Mounting evidence for prediagnostic use of statins in reducing risk of lethal prostate cancer. J Clin Oncol. 2014;32:1–2. https://doi.org/10.1200/JCO.2013.53.2770.
Wu S-Y, Fang S-C, Shih H-J, Wen Y-C, Shao Y-HJ. Mortality associated with statins in men with advanced prostate cancer treated with androgen deprivation therapy. Eur J Cancer. 2019;112:109–17. https://doi.org/10.1016/j.ejca.2018.11.032.
Van Rompay MI, Solomon KR, Nickel JC, Ranganathan G, Kantoff PW, McKinlay JB. Prostate cancer incidence and mortality among men using statins and non-statin lipid-lowering medications. Eur J Cancer. 2019;112:118–26. https://doi.org/10.1016/j.ejca.2018.11.033.
Schisterman EF, Cole SR, Platt RW. Overadjustment bias and unnecessary adjustment in epidemiologic studies. Epidemiology. 2009;20:488–95. https://doi.org/10.1097/EDE.0b013e3181a819a1.
Fine JP, Gray RJ. A proportional hazards model for the subdistribution of a competing risk. J Am Stat Assoc. 1999;94:496–509. https://doi.org/10.1080/01621459.1999.10474144.
Brookhart MA, Patrick AR, Dormuth C, Avorn J, Shrank W, Cadarette SM, et al. Adherence to lipid-lowering therapy and the use of preventive health services: an investigation of the healthy user effect. Am J Epidemiol. 2007;166:348–54. https://doi.org/10.1093/aje/kwm070.
Dormuth CR, Patrick AR, Shrank WH, Wright JM, Glynn RJ, Sutherland J, et al. Statin adherence and risk of accidents: a cautionary tale. Circulation. 2009;119:2051–7. https://doi.org/10.1161/CIRCULATIONAHA.108.824151.
Schröder FH, Hugosson J, Roobol MJ, Tammela TL, Zappa M, Nelen V, et al. Screening and prostate cancer mortality: results of the European Randomised Study of Screening for Prostate Cancer (ERSPC) at 13 years of follow-up. Lancet (Lond, Engl). 2014;384:2027–35. https://doi.org/10.1016/S0140-6736(14)60525-0.
Tsodikov A, Gulati R, Heijnsdijk EAM, Pinsky PF, Moss SM, Qiu S, et al. Reconciling the effects of screening on prostate cancer mortality in the ERSPC and PLCO trials. Ann Intern Med. 2017;167:449. https://doi.org/10.7326/M16-2586.
Crawford ED, Grubb R, Black A, Andriole GL, Chen MH, Izmirlian G, et al. Comorbidity and mortality results from a randomized prostate cancer screening trial. J Clin Oncol. 2011;29:355–61. https://doi.org/10.1200/JCO.2010.30.5979.
Telesca D, Etzioni R, Gulati R. Estimating lead time and overdiagnosis associated with PSA screening from prostate cancer incidence trends. Biometrics. 2008;64:10–9. https://doi.org/10.1111/j.1541-0420.2007.00825.x.
Draisma G, Boer R, Otto SJ, van der Cruijsen I, Damhuis R, Schröder FH, et al. Lead times and overdetection due to prostate-specific antigen screening: estimates from the European randomized study of screening for prostate cancer. J Natl Cancer Inst. 2003;95:868–78. https://doi.org/10.1093/jnci/95.12.868.
Alfaqih MA, Allott EH, Hamilton RJ, Freeman MR, Freedland SJ. The current evidence on statin use and prostate cancer prevention: are we there yet? Nat Rev Urol. 2017;14:107–19. https://doi.org/10.1038/nrurol.2016.199.
Yu O, Eberg M, Benayoun S, Aprikian A, Batist G, Suissa S, et al. Use of statins and the risk of death in patients with prostate cancer. J Clin Oncol. 2014;32:5–11. https://doi.org/10.1200/JCO.2013.49.4757.
Platz EA, Tangen CM, Goodman PJ, Till C, Parnes HL, Figg WD et al. Statin drug use is not associated with prostate cancer risk in men who are regularly screened. J Urol. 2014. https://doi.org/10.1016/j.juro.2014.01.095.
Murtola TJ, Syvälä H, Tolonen T, Helminen M, Riikonen J, Koskimäki J, et al. Atorvastatin versus placebo for prostate cancer before radical prostatectomy—a randomized, double-blind, placebo-controlled clinical trial. Eur Urol. 2018;74:697–701. https://doi.org/10.1016/J.EURURO.2018.06.037.
Penson DF, Albertsen PC, Nelson PS, Barry M, Stanford JL. Determining cause of death in prostate cancer: are death certificates valid? J Natl Cancer Inst. 2001;93:1822–3. https://doi.org/10.1093/jnci/93.23.1822.
Funding
The project described was partially supported by the National Institutes of Health, Grant TL1TR001443 (AK, PR, RRS, AKB). The content is solely the responsibility of the authors and does not necessarily represent the official views of the NIH.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
PR discloses previous salary support from Peptide Logic, LLC. AKB discloses consulting fees from Boston Consulting Group. RRS discloses consulting fees from Boston Consulting Group. AK discloses previous consulting fees from and ownership stake in Sympto Health. JDM disclose consulting fees from Boston Consulting Group and ownership stake in Sympto Health.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Kumar, A., Riviere, P., Luterstein, E. et al. Associations among statins, preventive care, and prostate cancer mortality. Prostate Cancer Prostatic Dis 23, 475–485 (2020). https://doi.org/10.1038/s41391-020-0207-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41391-020-0207-5
This article is cited by
-
Prostate cancer cell proliferation is influenced by LDL-cholesterol availability and cholesteryl ester turnover
Cancer & Metabolism (2022)
-
Population-wide impacts of aspirin, statins, and metformin use on prostate cancer incidence and mortality
Scientific Reports (2021)