Abstract
Background
Offspring born to mothers with pre-eclampsia (Pre-E) suffer higher risks of adult cardiovascular diseases, suggesting that exposure to an antiangiogenic environment in-utero has a lasting impact on the development of endothelial function. The goal of this study is to test the hypothesis that in-utero exposure to Pre-E results in alterations of angiogenic factors/cytokines that negatively impact vascular development during infancy.
Methods
Infants born from mothers with and without Pre-E were recruited and followed up at 6 months. Plasma cytokines, blood pressure, microvessel density, and vascular reactivity were assessed.
Results
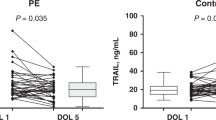
6-month-old infants born to mothers with Pre-E had unchanged blood pressure (p = 0.86) and microvessel density (p = 0.57). Vascular reactivity was decreased in infants born to mothers with Pre-E compared to infants born to healthy mothers (p = 0.0345). Interleukin 8 (IL-8) (p = 0.03) and Angiopoeitin-2 (Ang-2) (p = 0.04) were increased in infants born to mothers with Pre-E. We observed that higher IL-8 was associated with lower vascular reactivity (rho = −0.14, p < 0.0001).
Conclusion
At 6 months of age, infants born to mothers with Pre-E had impaired vascular reactivity and higher IL-8 and Ang-2, but similar blood pressure and microvessel density compared to infants born to non-Pre-E mothers.
Impact Statement
-
Changes in cord blood antiangiogenic factors are documented in infants of mothers with pre-eclampsia and may contribute to offspring risks of adult cardiovascular disease. How these factors evolve during early infancy and their correlation with offspring vascular development have not been studied.
-
This study found that 6-month-old infants born to mothers with pre-eclampsia had decreased vascular reactivity, which was correlated with higher IL-8.
-
These findings underscore the lasting impact of maternal pre-eclampsia on offspring vascular development and highlight the need for long-term follow-up in children born to mothers with pre-eclampsia.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 14 print issues and online access
$259.00 per year
only $18.50 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Boakye, E. et al. Nativity-related disparities in preeclampsia and cardiovascular disease risk among a racially diverse cohort of US Women. JAMA Netw. Open 4, e2139564 (2021).
Irgens, H. U., Reisæter, L., Irgens, L. M. & Lie, R. T. Long term mortality of mothers and fathers after pre-eclampsia: population based cohort study. BMJ 323, 1213–1217 (2001).
Yang, L. et al. Maternal hypertensive disorders during pregnancy and the risk of offspring diabetes mellitus in childhood, adolescence, and early adulthood: a nationwide population-based cohort study. BMC Med. 21, 59 (2023).
Hecht, J. L. et al. The pathology of eclampsia: An autopsy series. Hypertens. Pregnancy 36, 259–268 (2017).
Weel, I. C. et al. Association between placental lesions, cytokines and angiogenic factors in pregnant women with Preeclampsia. PLoS ONE 11, e0157584 (2016).
Clark, D. E. et al. A vascular endothelial growth factor antagonist is produced by the human placenta and released into the maternal circulation. Biol. Reprod. 59, 1540–1548 (1998).
Tangerås, L. H. et al. Distinct first trimester cytokine profiles for gestational hypertension and preeclampsia. Arterioscler. Thromb. Vasc. Biol. 35, 2478–2485 (2015).
Tomimatsu, T. et al. Preeclampsia: Maternal systemic vascular disorder caused by generalized endothelial dysfunction due to placental antiangiogenic factors. Int. J. Mol. Sci. 20, 4246 (2019).
Heath-Freudenthal, A. et al. Vascular disorders of pregnancy increase susceptibility to neonatal pulmonary hypertension in high-altitude populations. Hypertens. Dallas Tex. 1979 79, 1286–1296 (2022).
Vinayagam, V., Bobby, Z., Habeebullah, S., Chaturvedula, L. & Bharadwaj, S. K. Maternal and cord blood plasma sEng and TGF-β1 in patients with hypertensive disorders of pregnancy: a pilot study in a South. Indian Popul. J. Clin. Diagn. Res. JCDR 11, QC32–QC34 (2017).
Kim, D.-H., Shin, S. H., Kim, E.-K. & Kim, H.-S. Association of increased cord blood soluble endoglin with the development of bronchopulmonary dysplasia in preterm infants with maternal preeclampsia. Pregnancy Hypertens. 13, 148–153 (2018).
Sezer, S. D. et al. Comparison of angiogenic and anti-angiogenic factors in maternal and umbilical cord blood in early- and late-onset pre-eclampsia. Gynecol. Endocrinol. J. Int. Soc. Gynecol. Endocrinol. 28, 628–632 (2012).
Antonios, T. F. T. et al. Capillary remodeling in infants born to hypertensive pregnancy: pilot study. Am. J. Hypertens. 25, 848–853 (2012).
Varley, B. J. et al. Intrauterine exposure to preeclampsia does not impair vascular health in children. Front. Public Health 10, 1071304 (2022).
Nahum Sacks, K. et al. Prenatal exposure to preeclampsia as an independent risk factor for long-term cardiovascular morbidity of the offspring. Pregnancy Hypertens. 13, 181–186 (2018).
Ren, C. L. et al. Forced expiratory flows and diffusion capacity in infants born from mothers with pre-eclampsia. Pediatr. Pulmonol. 57, 2481–2490 (2022).
Kramer, M. S. et al. A new and improved population-based Canadian reference for birth weight for gestational age. Pediatrics 108, E35 (2001).
Acosta, J. C. et al. Gestational diabetes mellitus alters maternal and neonatal circulating endothelial progenitor cell subsets. Am. J. Obstet. Gynecol. 204, 254.e8–254.e15 (2011).
DiMeglio, L. A. et al. Endothelial abnormalities in adolescents with type 1 diabetes: a biomarker for vascular sequelae? J. Pediatr. 157, 540–546 (2010).
Martin, H., Gazelius, B. & Norman, M. Impaired acetylcholine-induced vascular relaxation in low birth weight infants: implications for adult hypertension? Pediatr. Res. 47, 457–462 (2000).
Krispinsky, L. T. et al. Endothelial-dependent vasomotor dysfunction in infants after cardiopulmonary bypass. Pediatr. Crit. Care Med. J. Soc. Crit. Care Med. World Fed. Pediatr. Intensive Crit. Care Soc. 21, 42–49 (2020).
Hubble, S. M. A., Kyte, H. L., Gooding, K. & Shore, A. C. Variability in sublingual microvessel density and flow measurements in healthy volunteers. Microcirculation 16, 183–191 (2009).
Bezemer, R. et al. Rapid automatic assessment of microvascular density in sidestream dark field images. Med. Biol. Eng. Comput. 49, 1269–1278 (2011).
Hypertension in Pregnancy: Executive Summary. Obstet. Gynecol. 122, 1122 (2013).
Källén, B., Finnström, O., Nygren, K.-G. & Olausson, P. O. Association between preterm birth and intrauterine growth retardation and child asthma. Eur. Respir. J. 41, 671–676 (2013).
Nakimuli, A. et al. Relative impact of pre-eclampsia on birth weight in a low resource setting: A prospective cohort study. Pregnancy Hypertens. 21, 1–6 (2020).
Xiong, X., Demianczuk, N. N., Saunders, L. D., Wang, F.-L. & Fraser, W. D. Impact of preeclampsia and gestational hypertension on birth weight by gestational age. Am. J. Epidemiol. 155, 203–209 (2002).
Liu, Y. et al. Impact of gestational hypertension and preeclampsia on low birthweight and small-for-gestational-age infants in China: A large prospective cohort study. J. Clin. Hypertens. 23, 835–842 (2021).
Yang, Y. et al. Preeclampsia prevalence, risk factors, and pregnancy outcomes in Sweden and China. JAMA Netw. Open 4, e218401 (2021).
Weil, B. R., Stauffer, B. L., Greiner, J. J. & DeSouza, C. A. Prehypertension is associated with impaired nitric oxide-mediated endothelium-dependent vasodilation in sedentary adults. Am. J. Hypertens. 24, 976–981 (2011).
Stockelman, K. A. et al. Negative influence of insufficient sleep on endothelial vasodilator and fibrinolytic function in hypertensive adults. Hypertension 78, 1829–1840 (2021).
Cemgil Arikan, D., Aral, M., Coskun, A. & Ozer, A. Plasma IL-4, IL-8, IL-12, interferon-γ and CRP levels in pregnant women with preeclampsia, and their relation with severity of disease and fetal birth weight. J. Matern. -Fetal Neonatal Med. J. Eur. Assoc. Perinat. Med. Fed. Asia Ocean. Perinat. Soc. Int. Soc. Perinat. Obstet. 25, 1569–1573 (2012).
Han, S. Y., Jun, J. K., Lee, C.-H., Park, J. S. & Syn, H. C. Angiopoietin-2: a promising indicator for the occurrence of severe preeclampsia. Hypertens. Pregnancy 31, 189–199 (2012).
Yue, T. L. et al. Interleukin-8. A mitogen and chemoattractant for vascular smooth muscle cells. Circ. Res. 75, 1–7 (1994).
Li, A., Dubey, S., Varney, M. L., Dave, B. J. & Singh, R. K. IL-8 directly enhanced endothelial cell survival, proliferation, and matrix metalloproteinases production and regulated Angiogenesis1. J. Immunol. 170, 3369–3376 (2003).
Boekholdt, S. M. et al. IL-8 plasma concentrations and the risk of future coronary artery disease in apparently healthy men and women. Arterioscler. Thromb. Vasc. Biol. 24, 1503–1508 (2004).
Szarka, A., Rigó, J., Lázár, L., Bekő, G. & Molvarec, A. Circulating cytokines, chemokines and adhesion molecules in normal pregnancy and preeclampsia determined by multiplex suspension array. BMC Immunol. 11, 1–9 (2010).
Ambalavanan, N. et al. Cytokines associated with bronchopulmonary dysplasia or death in extremely low birth weight infants. Pediatrics 123, 1132–1141 (2009).
Akwii, R. G., Sajib, M. S., Zahra, F. T. & Mikelis, C. M. Role of Angiopoietin-2 in vascular physiology and pathophysiology. Cells 8, 471 (2019).
Patel, J. V., Lim, H. S., Varughese, G. I., Hughes, E. A. & Lip, G. Y. H. Angiopoietin-2 levels as a biomarker of cardiovascular risk in patients with hypertension. Ann. Med. 40, 215–222 (2008).
Medvedeva, T. A. & Kushnarenko, N. N. Angiopoietin-2 is a new predictor of arterial stiffness and diastolic heart failure in gouty patients with arterial hypertension. Atherosclerosis 331, e229 (2021).
Aghai, Z. H. et al. Angiopoietin 2 concentrations in infants developing bronchopulmonary dysplasia: attenuation by dexamethasone. J. Perinatol. J. Calif. Perinat. Assoc. 28, 149–155 (2008).
Dionne, J. M., Abitbol, C. L. & Flynn, J. T. Hypertension in infancy: diagnosis, management and outcome. Pediatr. Nephrol. Berl. Ger. 27, 17–32 (2012).
Flynn, J. T. et al. Clinical practice guideline for screening and management of high blood pressure in children and adolescents. Pediatrics 140, e20171904 (2017).
van den Berg, V. J. et al. Reproducibility of microvascular vessel density analysis in Sidestream dark-field-derived images of healthy term newborns. Microcirc. N. Y. N. 1994 22, 37–43 (2015).
van Elteren, H. A., Ince, C., Tibboel, D., Reiss, I. K. M. & de Jonge, R. C. J. Cutaneous microcirculation in preterm neonates: comparison between sidestream dark field (SDF) and incident dark field (IDF) imaging. J. Clin. Monit. Comput. 29, 543–548 (2015).
Acknowledgements
The authors thank the Multiplex Analysis Core at the Indiana University Melvin and Bren Simon Comprehensive Cancer Center for providing support in analyzing samples and interpretation of data.
Funding
This study is supported by R01HL122215 (R.S.T, L.S.H), K08HD109636 (K.L.K), March of Dimes Basil O’Connor Award (K.L.K).
Author information
Authors and Affiliations
Contributions
K.L.K was responsible for the data analysis and interpretation and wrote the initial and final drafts. E.R. was responsible for data collection, data analysis and interpretation, and wrote the initial and final drafts. J.E.S was responsible for the data analysis and interpretation and revised the manuscript. S.E was responsible for data collection and revised the manuscript. D.M.H was responsible for study design and revising the manuscript C.L.R was responsible for data interpretation and revising manuscript. C.T and J.B were responsible for data collection and revising manuscript. D.M.H, L.S.H, and R.S.T were responsible for study design, data analysis and interpretation, and revising manuscript. All authors approved the final version of manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Consent statement Patient consent was obtained prior to enrollment as described in methods section.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kua, K.L., Rhoads, E., Slaven, J.E. et al. Decreased vascular reactivity associated with increased IL-8 in 6-month-old infants of mothers with pre-eclampsia. Pediatr Res (2024). https://doi.org/10.1038/s41390-024-03132-4
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41390-024-03132-4