Abstract
Background
Newborns are at high risk of sepsis. At present there is no definitive “rule in” blood test for sepsis at the point of clinical concern. A positive blood culture remains the gold standard test for neonatal sepsis, however laboratory markers that correlate prospectively with culture positive sepsis could aid clinicians in making decisions regarding administration of empiric antibiotic therapies.
Methods
This multi-site, prospective observational study will take place in two neonatal intensive care units (National Maternity Hospital and Rotunda Hospital, Dublin). Neonates born at less than 34 weeks will be enroled and informed consent obtained prior to late onset sepsis work up. If at any point subsequently during their neonatal intensive care stay they develop signs and symptoms of possible sepsis requiring blood culture, an additional sodium citrate sample will be obtained. Infants will be categorised into three groups as follows: (i) culture positive sepsis, (ii) culture negative sepsis where an infant receives 5 days of antibiotics (iii) non sepsis. Our primary outcome is to establish if differential platelet/endothelial activation can prospectively identify neonatal culture positive late onset sepsis.
Trial registration number
NCT05530330
Impact
-
Preterm infants are a high risk group for the development of sepsis which is a major cause of mortality in this population.
-
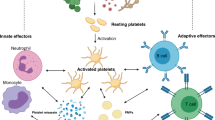
Platelets have been associated with host response to invasive bacterial infections both in animal models and translational work.
-
A positive blood culture is the gold standard test for neonatal sepsis but can be unreliable due to limited blood sampling in the very low birth weight population.
-
This study hopes to establish if platelet/endothelial associated plasma proteins can prospectively identify late onset neonatal sepsis.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 14 print issues and online access
$259.00 per year
only $18.50 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
Data availability
Nil data generated to date. On completion of the study, anonymised data available on request and within the limitations of General Data Protection Regulation (GDPR) useage.
References
Fleischmann-Struzek, C. et al. The global burden of paediatric and neonatal sepsis: A systematic review. Lancet Respir. Med 6, 223–230 (2018).
Mitre, E. et al. Association between use of acid-suppressive medications and antibiotics during infancy and allergic diseases in early childhood. JAMA Pediatrics 172, e180315–e180315 (2018).
Nogacka, A. M. et al. Early microbiota, antibiotics and health. Cell Mol. Life Sci. 75, 83–91 (2018).
Eck, A. et al. Neonatal microbiota development and the effect of early life antibiotics are determined by two distinct settler types. PLOS ONE 15, e0228133 (2020).
Esmaeilizand, R. et al. Antibiotic exposure and development of necrotizing enterocolitis in very preterm neonates. Paediatr. Child Health 23, e56–e61 (2017).
Patel, S. J. & Saiman, L. Antibiotic resistance in neonatal intensive care unit pathogens: Mechanisms, clinical impact, and prevention including antibiotic stewardship. Clin. Perinatol. 37, 547–563 (2010).
Schlapbach, L. J. & Kissoon, N. Defining pediatric sepsis. JAMA Pediatr. 172, 313–314 (2018).
Qazi, S. A. & Stoll, B. J. Neonatal sepsis: A major global public health challenge. Pediatr. Infect. Dis. J. 28, S1–S2 (2009).
Alshaikh, B., Yusuf, K. & Sauve, R. Neurodevelopmental outcomes of very low birth weight infants with neonatal sepsis: Systematic review and meta-analysis. J. Perinatol. 33, 558–564 (2013).
Singer, M. et al. The third international consensus definitions for sepsis and septic shock (sepsis-3). JAMA 315, 801–810 (2016).
Aziz, K. B. et al. Maximum vasoactive-inotropic score and mortality in extremely premature, extremely low birth weight infants. J. Perinatol. 41, 2337–2344 (2021).
Wynn, J. L. & Polin, R. A. A neonatal sequential organ failure assessment score predicts mortality to late-onset sepsis in preterm very low birth weight infants. Pediatr. Res 88, 85–90 (2020).
Vazzalwar, R., Pina-Rodrigues, E., Puppala, B. L., Angst, D. B. & Schweig, L. Procalcitonin as a screening test for late-onset sepsis in preterm very low birth weight infants. J. Perinatol. 25, 397–402 (2005).
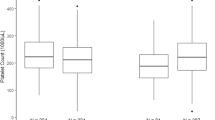
Guida, J. D., Kunig, A. M., Leef, K. H., McKenzie, S. E. & Paul, D. A. Platelet count and sepsis in very low birth weight neonates: Is there an organism-specific response? Pediatrics 111, 1411–1415 (2003).
Sola-Visner, M., Sallmon, H. & Brown, R. New insights into the mechanisms of nonimmune thrombocytopenia in neonates. Semin Perinatol. 33, 43–51 (2009).
McDonald, B. et al. Platelets and neutrophil extracellular traps collaborate to promote intravascular coagulation during sepsis in mice. Blood 129, 1357–1367 (2017).
O’Reilly, D. et al. Platelets in pediatric and neonatal sepsis: Novel mediators of the inflammatory cascade. Pediatr. Res. 91, 359–367 (2021).
Nyamundanda, G., Gormley, I. C., Fan, Y., Gallagher, W. M. & Brennan, L. Metsizer: Selecting the optimal sample size for metabolomic studies using an analysis based approach. BMC Bioinforma. 14, 338 (2013).
Köstlin-Gille, N. et al. Epidemiology of early and late onset neonatal sepsis in very low birthweight infants: Data from the german neonatal network. Pediatr. Infect. Dis. J. 40, 255–259 (2021).
Cantey, J. B. & Prusakov, P. A proposed framework for the clinical management of neonatal "Culture-Negative" sepsis. J. Pediatr. 244, 203–211 (2022).
Murphy, C. A. et al. The effect of platelets on thrombin generation in cord blood and peripheral neonatal blood in the premature infant; the event study. Blood 138, 3188 (2021).
Richardson, D. K., Corcoran, J. D., Escobar, G. J. & Lee, S. K. Snap-Ii and Snappe-Ii: Simplified newborn illness severity and mortality risk scores. J. Pediatr. 138, 92–100 (2001).
Parsons, M. E. M. et al. Platelet releasate proteome profiling reveals a core set of proteins with low variance between healthy adults. Proteomics 18, 1800219 (2018).
Maguire, P. B. et al. Proteomic analysis reveals a strong association of Β-catenin with cadherin adherens junctions in resting human platelets. Proteomics 18, 1700419 (2018).
Acknowledgements
We would like to acknowledge the contribution of Ms.Mandy Daly (Irish Neonatal Health Alliance) for her assistance and input with regard to patient-public involvement.
Funding
DOR has been awarded the Irish Clinical Academic Training (ICAT) Programme, supported by the Wellcome Trust and the Health Research Board (grant number 203930/B/16/Z), the Health Service Executive, National Doctors Training and Planning, and the Health and Social Care, Research and Development Division, Northern Ireland.
Author information
Authors and Affiliations
Contributions
Study designed by D.O.R., C.A.M., N.M.c.C., A.C. and P.M.. Statistical plan developed by I.C.G. and D.O.R.. Clinical protocol developed by D.O.R., C.A.M., C.M.M., F.N.A., N.M.c.C. and A.C.. Experimental design by D.O.R., C.N.M., P.M.. All authors reviewed this manuscript prior to submission.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
O’Reilly, D., Murphy, C.A., Moore, C.M. et al. Markers of platelet activation foR identification of late onset sEpsis in infaNTs: PARENT study protocol. Pediatr Res 95, 852–856 (2024). https://doi.org/10.1038/s41390-023-02812-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41390-023-02812-x