Abstract
Background
Excessive and inconsolable crying behavior in otherwise healthy infants (a condition called infant colic (IC)) is very distressing to parents, may lead to maternal depression, and in extreme cases, may result in shaken baby syndrome. Despite the high prevalence of this condition (20% of healthy infants), the underlying neural mechanisms of IC are still unknown.
Methods
By employing the latest magnetic resonance imaging (MRI) techniques in newborns, we prospectively investigated whether newborns’ early brain responses to a sensory stimulus (smell) is associated with a subsequent crying behavior.
Results
In our sample population of 21 healthy breastfed newborns, those who developed IC at 6 weeks exhibited brain activation and functional connectivity in primary and secondary olfactory brain areas that were distinct from those in babies that did not develop IC. Different activation in brain regions known to be involved in sensory integration was also observed in colicky babies. These responses measured shortly after birth were highly correlated with the mean crying time at 6 weeks of age.
Conclusions
Our results offer novel insights into IC pathophysiology by demonstrating that, shortly after birth, the central nervous system of babies developing IC has already greater reactivity to sensory stimuli than that of their noncolicky peers.
Impact
-
Shortly after birth, the central nervous system of colicky infants has a greater sensitivity to olfactory stimuli than that of their noncolicky peers. This early sensitivity explains as much as 48% of their subsequent crying behavior at 6 weeks of life.
-
Brain activation patterns to olfactory stimuli in colicky infants include not only primary olfactory areas but also brain regions involved in pain processing, emotional valence attribution, and self-regulation.
-
This study links earlier findings in fields as diverse as gastroenterology and behavioral psychology and has the potential of helping healthcare professionals to define strategies to advise families.
Similar content being viewed by others
Introduction
Why do some infants cry so much more than others? Crying is a part of typical infant behavior1,2 as it is a form of communication between caregivers and babies3. At 6 weeks of age, some babies cry very little and are easily soothed by their caregivers, but approximately 20% of infants cry for >3 h a day for multiple days4. Excessive crying in otherwise healthy infants (also called infant colic (IC)) is very distressing to parents, may lead to early weaning, maternal anxiety, and maternal depression; and in extreme cases, may result in shaken baby syndrome with severe consequences5,6. Health care professionals are frustrated by the lack of solutions they can offer7 as the etiology of this extreme behavior is largely unknown8.
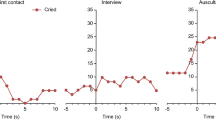
Different hypotheses have been proposed to explain why some babies cry so much more than their peers. Psychosocial, gastrointestinal, and neurological factors seem to contribute to the pathophysiology of IC. Stressed parents, maternal anxiety, and paternal depression have been linked to excessive crying behavior in different studies9. Literature also provides evidence for an interplay between IC and intestinal microbiota dysbiosis with specific microbial signature in infants with excessive crying behavior10, which could in turn lead to more gas production in the gut and/or cause gut inflammation. Other gastrointestinal factors such as a leaky gut barrier, altered hepatic bile acid production and regulation, enteric nervous system immaturity, and visceral hypersensitivity may also play a role11. Finally, some hypotheses suggest that excessive crying is simply the upper end of the spectrum of early developmental crying behavior and may be related to differences in the functioning of the central nervous system12. Central sensory integration may be a key element for the understanding of behavioral differences observed shortly after birth as sensory experiences and reactions to stimuli are essential elements regulating behavior13. St James-Roberts and colleagues confirmed this hypothesis by showing that babies who have increased reactivity after sensory stimuli (e.g., undressing, handling, and a heel prick) shortly after birth subsequently display longer episodes of crying14. Tauman and colleagues used a parental questionnaire and found that children with behavioral sleep and eating disorders during early childhood have hypersensitive profiles15. This finding led to the conclusion that children who are more sensitive or reactive to sensory stimulation may be more difficult to care for during their entire childhood, starting with excessive crying early in life. Being hyperreactive or hyporeactive to sensory stimulation depends on detection thresholds, self-regulation strategies16, variations in emotional valence attribution, and pain thresholds17.
Drawing on these hypotheses, we aimed to investigate whether infants with IC already have a different reactivity to sensory stimuli at birth. We therefore enrolled healthy full-term infants at birth and investigated their cerebral reactivity to olfactory stimuli with functional magnetic resonance imaging (fMRI) during their first week of life. Their daily crying time was measured at 6 weeks of age using parental diaries. We hypothesized that early brain response to olfactory odorants, which reflects early sensory reactivity, would be correlated to crying behavior after 6 weeks of age.
Studying the neural correlates of these high-level brain functions is challenging. Advanced neuroimaging techniques, especially fMRI, enable investigations of brain activity after the presentation of standardized sensory stimuli in a noninvasive manner and may therefore provide insight into what babies feel18,19.
Methods
Subjects
In total, 36 full-term newborns born between 37 and 42 gestational weeks without signs of neurological disorders, congenital abnormality, or illness since birth were prospectively enrolled in this study during their first 24–72 h of life, i.e., well before their excessive crying behavior (IC) started. All babies were exclusively breastfed at enrollment. The newborns underwent an fMRI between their first and sixth day after birth during natural sleep or quiet resting in the scanner, and no pharmacological sedation was used. The fMRI procedure is widely used, and no side effects have been described in healthy or sick babies20; thus fMRI is very unlikely to have caused crying. The study followed the Declaration of Helsinki’s guidelines. The local ethical committee (CER-approval number: 10–202) approved the study, and all parents provided written informed consent before enrollment.
Of the 36 infants enrolled in the study, 15 infants were excluded from the analysis due to technical difficulties (7 infants), excessive motion during the MRI (4 infants), health issues unrelated to the study (1 infant with meningitis), or incomplete crying diaries (3 infants). In total, 21 infants completed the study (see Table 1).
Crying behavior at 6 weeks
The parents kept a crying diary [adapted from Barr et al.21] for 14 days starting from week 5–6 of life. Each 24-h period was divided into 96 intervals of 15 min during which the parents noted whether their baby was awake and calm, crying/fussing, being fed, or sleeping. A baby was considered to have IC if the baby cried for >3 h a day for at least 3 days within a consecutive 7-day period (according to the Rome III criteria22). The mean crying time (MCT) was calculated over a 2-week recording period. In Barr’s original diary, each 24-h period was divided into 288 intervals of 5 min and time sucking was also being noted by parents. We chose to use a simplified diary as parents were asked to fill it for 14 consecutive days. As not all parents would fill it regularly during the day, we feared that some would not recall short bouts of crying behavior. We did not ask about sucking behavior as it was not part of our hypothesis.
At 6 weeks of life, a trained pediatric nurse visited all infants at home and registered any undercurrent illness appearance since birth. The feeding situation, growth, and medical data from the first month visit by a pediatrician were also observed and recorded. All infants had normal growth and clinical examination.
Stimulation protocol
As previously described by our group19, the following three olfactory stimuli were selected for the experiment: a rotten cabbage-like (dimethyl trisulfide) odor, banana-like (isoamyl acetate (IAA)) odor, and eucalyptus-like (eucalyptol (EU)) odor, which is a bimodal (olfactory and trigeminal) odor. All odorants were considered food grade and also natural for IAA and EU (Sigma-Aldrich, Flavours and Fragrances). Furthermore, the odorants needed to fulfill the following criteria: an airborne odorant not biologically relevant for newborns (different from breast milk, formula, or amniotic fluid); have a hedonic value, i.e., pleasant (banana) or unpleasant (rotten cabbage), or a trigeminal property (EU); have no absorption in the tube used in the delivery system; and have nonirritant compounds (for safety reasons). Each odorant was delivered using a homemade four-way odorant delivery system (three odorants and neutral stimulus) in continuous air flow.
The odorants were presented for 20 s in a pseudo-randomized order to minimize interaction effects between the substances. Each odorant stimulation was repeated 5 times per run and was separated by 20 s of odorless stimulation from a water flask containing sterile water (neutral condition). This block-design stimulation was preferred over an event-related design due to the rapid breathing of newborns. The stimulation protocol is described in detail in our previous study19.
MRI acquisition
All infants were fed immediately before testing to increase their chance of sleeping or staying quiet throughout the procedure. After the infants were fed and quiet, they were swaddled in a blanket with noise protection placed on their ears (adhesive earmuffs (Minimuffs; Natus Medical Inc., San Carlos, CA, USA)). Then the infants were positioned on a vacuum pillow (VacFix, Par Scientific, Odense, Denmark) longer than their bodies that surrounded the head to prevent movements and attenuate noise. The infants’ well-being and behavior during the experiments were monitored using pulse oxymetry, a camera, and a microphone, and a nurse was present during the entire MRI acquisition. If the infants showed signs of restlessness, scanning was immediately interrupted.
The acquisition was performed using a 3-T MRI (Siemens Magnetom Trio, Erlangen, Germany) with an 8-channel neohead coil (LMT medical systems, Lübeck, Germany). The total duration of the acquisition was between 30 and 50 min depending on the newborns’ compliance. Two runs of 350 functional images were acquired during the olfactory stimulation using a single-shot T2*-weighted gradient-echo echo planar imaging (EPI) sequence (repetition time (TR) = 1800 ms, echo time (TE) = 25 ms, flip angle = 85°, 30 slices, and voxel size = 2.2 × 2.2 × 3.5 mm3). A T2-weighted structural image was acquired for anatomical reference (TR = 4990 ms, TE = 160 ms, flip angle = 150°, 113 coronal slices, and voxel size = 0.78 × 0.78 × 1.2 mm3).
fMRI preprocessing
The preprocessing of the functional images was performed with SPM8 (Wellcome Department of Imaging Neuroscience, UCL, London, UK) and included (i) realignment, (ii) slice timing, (iii) rigid-body coregistration of functional images on the T2 structural image, (iv) normalization of subject anatomical T2 image (1 × 1 × 1 mm) and EPI (2 × 2 × 2 mm) to a T2 template of newborns created from 28 infants’ anatomical T2 images acquired in this study, and (v) spatial smoothing (full width at half maximum 6 mm).
To accommodate the high level of motion in the infants, images with framewise displacement >6 mm were excluded along with the previous and two following images23.
fMRI analysis
The functional time series were analyzed voxel by voxel with a general linear model (GLM). The six realignment parameters and their Volterra expansion24 were reduced using singular value decomposition (SVD). The NC (number of components) of first SVD components explaining at least 99% of the variance or the first six SVD components if NC > 6 were included in the GLM model as covariate regressors. This SVD reduction allows for the consideration of the 24 realignment parameters to remove any residual motion-related variance without greatly decreasing the number of degrees of freedom while ensuring the orthogonality of the model. The block stimulation design of each odor was convolved by the canonical hemodynamic response function and used as a regressor. Sessions without motion >6 mm including a minimum of 2 repetitions of each condition were used in the analysis, and regressors associated with the odorant stimulation and confounds were accordingly excluded. The low-frequency noise and signal drift were removed using a discrete cosine transform basis set with a filter cut-off period of 256 s.
The first-level contrast images of each of the 21 subjects were then entered into two second-level group analyses (random effects) using t test statistics and a linear regression. The significance threshold was set at p < 0.005 uncorrected with a minimum of 10 voxels extent to identify the regions involved in the processing of each odorant separately in contrast with the neutral condition (water) and their association with subsequent crying behavior.
To study the association between sensory (olfactory) reactivity at birth and subsequent crying behavior, we conducted the following two different analyses: first, we compared the brain responses between the groups (the babies were assigned to the group “colicky” or “noncolicky” depending on their total time of crying) using a two-sample t test analysis; and second, we assessed the correlation between each contrast of interest and the mean daily crying time (in minutes) of each baby.
Psychophysiological interaction (PPI) analysis
To further characterize cerebral responses to olfactory stimuli in newborns, we performed a PPI analysis25 that evaluated the modulation of functional connectivity. This seed-based method identifies regions whose activity becomes more closely related to the activity of a seed region (physiological aspect) under a specific condition or task (psychological aspect). In this analysis, we used the piriform cortex as a seed due to its well-documented role in olfaction26 and selected the Cabbage>Water contrast as it elicited the greatest cortical response. In addition to the seed time course and task regressor reflecting the contrast of interest, the model included an interaction term, which was calculated as an element-by-element multiplication of the seed and task regressors, and movement confounds as described in the previous session. The second-level analysis of the contribution of this interaction term to the model identifies regions whose functional connectivity with the seed is modulated by the experimental conditions. Continuous run segments without motion >6 mm were used for the analysis, and all regressors associated with the odorant stimulation or movement were accordingly excluded. The correlation between the strength of the PPI effect in each individual and the MCT was calculated used Pearson correlation coefficients.
Results
The crying time ranged from 0 (i.e., the parents reported no crying/fussing episodes lasting ≥15 min) to a maximum of 326.2 min/24 h. Eleven infants were considered to have excessive crying or IC at 6 weeks according to Rome III22 criteria. The MCT in the infants with colic was 175.8 ± 62.6 min/24 h, while the MCT in the infants without colic was 62.4 ± 43.9 min/24 h (mean ± SD, p = 0.001).
The activation analysis demonstrates that colicky babies have more significant response in the bilateral piriform cortex, left amygdala, left anterior insula, middle cingulate gyrus, thalamus, caudate nucleus, putamen, and left superior parietal lobule during the processing of a cabbage-like odor compared to infants who did not develop IC (Fig. 1).
Newborns who develop IC at 6 weeks (n = 11) show a statistically significant difference in the activation of the bilateral piriform cortex, the left insula, the left amygdala, and the caudate nucleus (display threshold p < 0.005 uncorrected) when they smell a cabbage-like odor compared to newborns who do not develop IC (n = 10). Activations are overlaid on a T2-weighted newborn template. Color bar indicates the t values.
Furthermore, we observed a significant correlation (p < 0.005, uncorrected) between the MCT at 5–6 weeks and the cerebral reactivity to the cabbage-like odor stimulation in the newborn period at the level of (a) the primary and secondary olfactory cortices, including the right piriform cortex, left orbitofrontal cortex (OFC), and anterior cingulate cortex (ACC) and (b) other cortical regions, such as the left superior parietal lobule and a part of the precuneus (Fig. 2). This correlation indicates that the greater the degree of the activation of these cerebral areas at birth during exposure to an olfactory stimulus, the more the infants cry at week 5–6 of life. The correlation is strong in the right piriform cortex (r = 0.69, with an r2 of 0.48) and left OFC (r = 0.58, with an r2 of 0.34) (Fig. 2b). For example, the response measured in the piriform cortex at birth explains 48% of the crying behavior at week 5–6.
a Linear regression of the activated areas under the cabbage condition (n = 21) showing a significant positive correlation (p < 0.005, uncorrected) between the mean daily crying time and the level of activation in the right piriform cortex, the left orbitofrontal cortex (OFC), the anterior cingulate cortex (ACC), and the precuneus. Activations are overlaid on a T2-weighted newborn template. Color bar indicates the t values. b Plot of the correlation at the x y z position on the maximum value in the right piriform cortex (r = 0.69, p < 0.0005) (upper part) and the left OFC (r = 0.58, p < 0.005) (bottom part).
The PPI analysis shows that when the babies who subsequently develop IC were exposed to the cabbage-like odor, the activity in the piriform cortex and caudate nucleus became more closely related than that in the control infants (Fig. 3a). This measure of functional connectivity recorded shortly after birth is strongly correlated with the MCT at 6 weeks of age (r = 0.81, p < 0.001, see Fig. 3b).
Altered functional connectivity is present shortly after birth in babies who subsequently develop colic. a During the cabbage-like odor exposure, there is an increased correlation between the bilateral caudate nucleus’s and the seed (piriform cortex)’s activations compared to those during the exposure to the baseline odor (contrast cabbage>water). This effect is significantly higher in the babies who subsequently develop colic than in those who do not (contrast colicky>noncolicky). b The strength of this psychophysiological interaction effect identified shortly after birth is significantly correlated with the mean crying time at 6 weeks (r = 0.81, p < 0.001).
Discussion
In this study, we demonstrated that healthy newborn babies who develop IC at 6 weeks of life have a different brain reactivity to odorant stimuli during the first days of life than those who will not develop IC. fMRI showed involvement of the piriform cortex, amygdala, OFC, ACC, insula, thalamus, caudate nucleus, putamen, and the parietal cortex. Although these brain areas are involved in olfactory processing in infants19 and adults, their more pronounced activation in the infants who subsequently develop IC may reflect not only a difference in the detection threshold but also their implication in more complex cerebral processing of sensory stimulation linked to self-regulation strategies, emotional valence attribution, and pain processing.
The neural correlates of self-regulation in newborns are still vastly unknown, but Fjell and colleagues27 found a relationship between the development of self-control and the structural development of the ACC. Therefore, the more pronounced activation of the ACC at birth in babies who develop colic may represent a neural correlate of self-regulation difficulties described in behavioral studies investigating IC during the first months of life. Indeed, decreased self-regulation capacities have been found in infants with IC even though their level of autonomic and neuroendocrine stress was not higher28. Longitudinal studies have confirmed that, even if a majority of regulatory difficulties during early infancy are transient, a non-negligible minority of children exhibits persistent difficulties29,30.
Correlates of the hedonic valence of sensory stimuli have been studied in adults and more recently in infants. In both populations, a greater activation of the piriform cortex and insula has been described after unpleasant odor processing19,31. In our study, the increased activation of the piriform cortex and insula in the colicky babies may represent an earlier labeling of the hedonic nature of odors (pleasant or unpleasant) or a negative overinterpretation of new odors. The ACC and insula are also involved in emotional integration32, and their more marked activation in the babies who subsequently develop IC may indicate an emotional labeling of a sensation experienced as “neutral” by others. In follow-up studies, Canivet et al. examined emotional valence attribution differences in children who had experienced IC. At 4 years of age, these children had a tendency to be more emotional and express more negative emotional and pain-related complaints33.
Pain may also lead to differences in sensory reactivity. The neural correlates of pain processing are currently well known in adults and infants. The ACC, insula, precuneus, and parietal lobe, which showed increased activity at birth in babies who subsequently develop colic, are involved in pain processing34,35. A misinterpretation of nonpainful stimuli as painful could explain this activation in our colicky population. Differences in functional connectivity between the piriform cortex and the caudate nucleus (a known relay station for emotional and cognitive processing systems) also confirm the high level of sensory integration at birth in this population.
Altered visceral sensation, especially stemming from digestion, has also been hypothesized to lead to IC36,37. This hypothesis is supported by a recent paper showing that the gut luminal contents from colicky infants trigger visceral hypersensitivity in normal mice and that hypersensitivity is correlated with crying time38. The present results may shed a different light on the link observed between the digestive tract and crying behavior and altered brain reactivity is a key element. Indeed, the insula, ACC, and thalamus, which are called the homeostatic afferent network, are activated in response to visceral, somatic, and sensory stimuli and are overactivated in newborns who subsequently develop IC. Thus babies with IC not only experience different stimuli from their digestive tract, due to early dysbiosis and/or gut physiology alterations, but also have altered brain reactivity to the information conveyed through the microbiota–gut–brain axis39.
The study has limitations. One of them is the small sample size, which is partly due to the challenge of studying the neural correlates of high-level brain functions in babies. One of these challenges is the sensitivity to infants’ motion when no sedation is used. Another difficulty is the challenge of recording behavioral reaction during a sensory stimulation in the scanner. Previous studies on infant olfactory perception have assessed perception by recording behavioral changes as oro-facial responses and head-turn duration. However, these behavioral measures cannot be assessed easily during MRI experiments. It is also very challenging to differentiate sleep and wake states in newborns inside the scanner but we are still confident in our results as it has been shown that the sleep states of newborns has no impact on their ability to process sensory information40. The high rate of reported colic in our subjects could be explained by the additional focus placed on crying behavior from birth as the parents were aware of their participation in a study investigating IC. Cerebral reactions to biologically relevant odorants and to other sensory modalities should also be investigated to better understand sensory integration in colicky infants at this early age.
Conclusion
Our results highlight a new link between brain activation and connectivity at the earliest stage of life and subsequent crying behavior. More specifically, we show that neonates who subsequently develop IC are more sensitive to odorous stimulus (smell of cabbage-like odor) immediately after birth. The brain activation patterns in these infants include not only primary olfactory areas but also brain regions involved in pain processing, emotional valence attribution, and self-regulation. Our study offers a new understanding of infants with IC by demonstrating that, at birth, their central nervous system has a potentially greater sensitivity to sensory stimuli than that of their noncolicky peers and that this early sensitivity explains as much as 48% of their subsequent crying behavior. This study further links earlier findings regarding babies with IC in fields as diverse as gastroenterology and behavioral psychology. Our results could help healthcare professionals explain babies’ excessive crying to their parents, which, in addition to providing immense relief, may also help them adapt their parenting approach to their child’s unique disposition and needs. Furthermore, if our findings are confirmed in a high number of colicky babies, early interventions could be developed to prevent the development of excessive crying behavior.
References
St James-Roberts, I. & Plewis, I. Individual differences, daily fluctuations, and developmental changes in amounts of infant waking, fussing, crying, feeding, and sleeping. Child Dev. 67, 2527–2540 (1996).
Wolke, D., Bilgin, A. & Samara, M. Systematic review and meta-analysis: fussing and crying durations and prevalence of colic in infants. J. Pediatr. 185, 55–61.e4 (2017).
Soltis, J. The signal functions of early infant crying. Behav. Brain Sci. 27, 443–458 (2004). Discussion 459–490.
Reijneveld, S. A., Brugman, E. & Hirasing, R. A. Excessive infant crying: the impact of varying definitions. Pediatrics 108, 893–897 (2001).
Hiscock, H. et al. Preventing early infant sleep and crying problems and postnatal depression: a randomized trial. Pediatrics 133, e346–e354 (2014).
Talvik, I., Alexander, R. C. & Talvik, T. Shaken baby syndrome and a baby’s cry. Acta Paediatr. 97, 782–785 (2008).
Biagioli, E. et al. Pain-relieving agents for infantile colic. Cochrane Database Syst. Rev. 9, CD009999 (2016).
Akhnikh, S. et al. The excessively crying infant: etiology and treatment. Pediatr. Ann. 43, e69–e75 (2014).
Petzoldt, J. Systematic review on maternal depression versus anxiety in relation to excessive infant crying: it is all about the timing. Arch. Womens Ment. Health 21, 15–30 (2018).
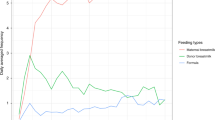
Savino, F. et al. Comparison of formula‐fed infants with and without colic revealed significant differences in total bacteria, Enterobacteriaceae and faecal ammonia. Acta Paediatr. 106, 573–578 (2017).
Zeevenhooven, J. et al. Infant colic: mechanisms and management. Nat. Rev. Gastroenterol. Hepatol. 15, 479–496 (2018).
Barr, R. G. Changing our understanding of infant colic. Arch. Pediatr. Adolesc. Med. 156, 1172–1174 (2002).
Dunn, W. The sensations of everyday life: empirical, theoretical, and pragmatic considerations. Am. J. Occup. Ther. 55, 608–620 (2001).
St James-Roberts, I. et al. Individual differences in responsivity to a neurobehavioural examination predict crying patterns of 1-week-old infants at home. Dev. Med. Child Neurol. 45, 400–407 (2003).
Tauman, R. et al. Sensory profile in infants and toddlers with behavioral insomnia and/or feeding disorders. Sleep Med. 32, 83–86 (2017).
Little, L. M., Dean, E., Tomchek, S. D. & Dunn, W. Classifying sensory profiles of children in the general population. Child Care Health Dev. 43, 81–88 (2017).
Liossi, C. & Howard, R. F. Pediatric chronic pain: biopsychosocial assessment and formulation. Pediatrics 138, e20160331 (2016).
Seghier, M. L., Lazeyras, F. & Huppi, P. S. Functional MRI of the newborn. Semin. Fetal Neonatal Med. 11, 479–488 (2006).
Adam-Darque, A. et al. fMRI-based neuronal response to new odorants in the newborn brain. Cereb. Cortex 28, 2901–2907 (2017).
Cawley, P. et al. Does magnetic resonance brain scanning at 3.0 Tesla pose a hyperthermic challenge to term neonates? J. Pediatr. 175, 228.e1–230.e1 (2016).
Barr, R. et al. Parental diary of infant cry and fuss behaviour. Arch. Dis. Child. 63, 380–387 (1988).
Hyman, P. E. et al. Childhood functional gastrointestinal disorders: neonate/toddler. Gastroenterology 130, 1519–1526 (2006).
Power, J. D. et al. Spurious but systematic correlations in functional connectivity MRI networks arise from subject motion. Neuroimage 59, 2142–2154 (2012).
Friston, K. J. et al. Movement‐related effects in fMRI time‐series. Magn. Reson. Med. 35, 346–355 (1996).
O’Reilly, J. X. et al. Tools of the trade: psychophysiological interactions and functional connectivity. Soc. Cogn. Affect. Neurosci. 7, 604–609 (2012).
Bensafi, M. The role of the piriform cortex in human olfactory perception: insights from functional neuroimaging studies. Chemosens. Percept. 5, 4–10 (2011).
Fjell, A. M. et al. Multimodal imaging of the self-regulating developing brain. Proc. Natl Acad. Sci. USA 109, 19620–19625 (2012).
White, B. P. et al. Behavioral and physiological responsivity, sleep, and patterns of daily cortisol production in infants with and without colic. Child Dev. 71, 862–877 (2000).
Hemmi, M. H., Wolke, D. & Schneider, S. Associations between problems with crying, sleeping and/or feeding in infancy and long-term behavioural outcomes in childhood: a meta-analysis. Arch. Dis. Child. Fetal Neonatal Ed. 96, 622–629 (2011).
Hyde, R. et al. Long-term outcomes of infant behavioral dysregulation. Pediatrics 130, e1243–e1251 (2012).
Bensafi, M., Sobel, N. & Khan, R. M. Hedonic-specific activity in piriform cortex during odor imagery mimics that during odor perception. J. Neurophysiol. 98, 3254–3262 (2007).
Morita, T. et al. The anterior insular and anterior cingulate cortices in emotional processing for self-face recognition. Soc. Cogn. Affect. Neurosci. 9, 570–579 (2014).
Canivet, C., Jakobsson, I. & Hagander, B. Infantile colic. Follow-up at four years of age: still more “emotional”. Acta Paediatr. 89, 13–17 (2000).
Lee, M. C., Mouraux, A. & Iannetti, G. D. Characterizing the cortical activity through which pain emerges from nociception. J. Neurosci. 29, 7909–7916 (2009).
Goksan, S. et al. fMRI reveals neural activity overlap between adult and infant pain. eLife 4, e06356 (2015).
Savino, F. et al. Ghrelin and motilin concentration in colicky infants. Acta Paediatr. 95, 738–741 (2006).
Sung, V. et al. Treating infant colic with the probiotic Lactobacillus reuteri: double blind, placebo controlled randomised trial. BMJ 348, g2107 (2014).
Eutamene, H. et al. Luminal contents from the gut of colicky infants induce visceral hypersensitivity in mice. Neurogastroenterol. Motil. 29, e12994 (2017).
Mayer, E. A., Naliboff, B. D. & Craig, A. D. Neuroimaging of the brain-gut axis: from basic understanding to treatment of functional GI disorders. Gastroenterology 131, 1925–1942 (2006).
Fifer, W. P. et al. Newborn infants learn during sleep. Proc. Natl Acad. Sci. USA 107, 10320–10323 (2010).
Acknowledgements
The authors thank all parents and babies and the Plateforme de Recherche de Pédiatrie, the Centre for Biomedical Imaging (CIBM) of the University Hospital of Geneva, and the Clinical Development Unit of Nestlé Research for their support. We thank N. Gons for her editorial help. This project was partly funded by Nestlé Research, Lausanne, Switzerland (Société des Produits Nestlé SA). R.H.-V.L. was supported by the Swiss National Science Fundation (SNF) grant numbers: 33CM30–124101 (P.I.: P.S.H.) and 33CM30_140334 (P.I.: P.S.H.). A.A.-D. was supported by the SNF grant numbers: 33CM30–124101 and 33CM30_140334 and by Nestlé Research (Société des Produits Nestlé SA), Lausanne, Switzerland. L.F. was supported by the SNF grant number 324730_163084 (P.I.: P.S.H.).
Author information
Authors and Affiliations
Contributions
R.H.-V.L. and P.S.H. conceived the study. G.B. and C.L.G.-R. participated to the conceptualization of the study. P.S.H., R.H.-V.L., A.A.-D., F.L., F.G., P.P., G.B., and C.L.G.-R. contributed to the experimental design. A.A.-D. was in charge of the recruitment, the MRI data collection, and the main MRI analyses. A.A.-D., L.F., and J.S. did the data analysis, supported by F.G., and D.V.D.V., R.H.-V.L., P.S.H., A.A.-D., and F.G. contributed to the interpretation of data. A.A.-D. and R.H.-V.L. wrote the first draft of the manuscript. R.H.-V.L., P.S.H., A.A.-D., F.G., L.F., C.L.G.-R., and G.B. critically revised the manuscript. P.S.H. supervised the study. All authors had full access to all the data in the study.
Corresponding author
Ethics declarations
Competing interests
P.P., J.S., C.L.G.-R., and G.B. are employed by Nestlé Research (Société des Produits Nestlé). No other disclosures are reported.
Patient consent
All parents provided written informed consent before enrollment.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Adam-Darque, A., Freitas, L., Grouiller, F. et al. Shedding light on excessive crying in babies. Pediatr Res 89, 1239–1244 (2021). https://doi.org/10.1038/s41390-020-1048-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41390-020-1048-6
This article is cited by
-
Early regulatory problems and parenting: life-long risk, vulnerability or susceptibility for attention, internalizing and externalizing outcomes?
European Child & Adolescent Psychiatry (2021)