Abstract
Background
Emergency department (ED) crowding may delay assessment and management and compromise outcomes. The association between the crowding metric time to physician initial assessment (PIA) and outcomes for children presenting for acute asthma is examined.
Methods
A population-based retrospective cohort of all presentations to 18 high-volume EDs during 2010–2014 in Alberta, Canada was created. Hourly, facility-specific median PIAs were calculated. Physician claims and hospitalizations data were linked for children (2–17 years) presenting for asthma.
Results
Twenty-five thousand three hundred and eighty-three presentations (16,053 children) were made for asthma. Crowding was common in all hospitals and affected PIA more for lower acuity presentations. For every 1-h increase in median facility PIA, the individual-level PIA increased by 13 min (95% CI: 12, 14) for high, 43 min (95% CI: 42, 44) for moderate, and 60 min (95% CI: 58, 61) for the low acuity groups, when adjusted by predictors. Similarly, length of stay increased by 6, 36, and 45 min for the high, moderate, and low acuity groups, respectively. Increased PIA resulted in more departures prior to completion of care for the lower acuity groups.
Conclusions
Crowding adversely affects short-term outcomes of less ill children more than those who are more ill. When EDs experience increased crowding, care to patients with asthma is delayed; effective strategies to reduce crowding and delays to care are urgently needed.
Impact
-
For children presenting to EDs for asthma, increased time to physician initial assessment adversely affects short-term outcomes of patients with less severe presentations to a greater extent compared to those who are most severe.
-
Times to physician initial assessment are below recommended benchmarks; however, delays in care exist that impact LOS, odds of admission, and premature patient departures.
-
Pediatric patients with severe asthma are seen quickly and their outcomes are excellent.
-
Since crowding adversely affects short-term outcomes of pediatric patients with asthma, efforts to reduce ED crowding and assess patients with asthma in a more timely manner are needed.
Similar content being viewed by others
Introduction
Emergency departments (EDs) are a critical component of healthcare systems and crowding is a common problem for health systems in high-income countries and high-volume medical centers. Crowding represents a state where the demand for emergency services surpasses the resources available for providing timely and quality care.1,2,3 Crowding can result in compromised care and delay therapies for time-sensitive conditions such as systemic corticosteroid administration for asthma;4 it has also been shown to increase hospital length of stay (LOS), patients leaving without completing care, and mortality.5,6
Asthma is the most common chronic condition in children7 and in Canada has a prevalence of 18% in boys and 13% in girls.8 Acute exacerbations often result in ED presentations with 750,000 presentations for children in the United States annually.9 Acute asthma requires timely care and can be life-threatening without proper management.10 Despite the importance of EDs for asthma care, there is limited literature on ED presentations and the effects of crowding on outcomes. Decreased timeliness and effectiveness of care for children with acute asthma was found to be associated with metrics ED occupancy and number waiting to see an attending-level physician.11 Few studies provide data from multiple sites across a defined region, examined over multiple years, with comprehensive information on outcomes and follow-up.
We used administrative data to explore the association between crowding in high-volume EDs in Alberta, Canada and outcomes for children presenting with asthma. We extracted all presentations for any condition from these facilities during a 5-year period and calculated the facility-specific hourly ED crowding metric of time to physician initial assessment (PIA). We investigated the impact of facility-specific ED crowding on important patient outcomes for children presenting with asthma.
Methods
Subjects
This retrospective cohort study used population-based health administrative databases from Alberta, Canada from April 1, 2010 to March 31, 2015. The study focused on Alberta’s 18 highest-volume EDs, classified into three categories: regional, urban (Calgary and Edmonton), and academic/teaching. The regional and urban hospitals assessed mixed pediatric–adult patient ages, whereas two academic/teaching EDs assessed only pediatric patients (ages ≤ 17 years) and three academic/teaching EDs are to assess only adult patients. The high-volume EDs have >30,000 visit annually with 57,307 as the median number of visits over study years for regional EDs (interquartile range [IQR] 51,737–60,753), 54,502 (IQR 50,221–71,218) for urban EDs, 72,404 (IQR 66,449–78,080) for academic/teaching EDs serving adult patients only, and 54,129 (IQR 41,294–70,793) for academic/teaching EDs serving pediatric patients only.
Presentations to the ED were extracted from the National Ambulatory Care Reporting System (NACRS), and linkages were made to the Cumulative Registry File (CRF) for demographic data, the Physician Claim File (PCF) for physician fee-for-service claims, and the Discharge Abstract Database (DAD) for hospitalization data. Statistics Canada 2006 census data provided neighborhood income quintiles and community size. The Health Research Ethics Board of the University of Alberta (Pro00056282) approved this study.
Children (2 ≤ age ≤ 17 years) residing in Alberta who presented to the high-volume EDs during the study period, with a primary or secondary diagnosis of asthma, defined as an International Classification of Diseases (ICD-10-CA)12 diagnostic code of J45.x (asthma all forms), formed the study population. Non-residents of Alberta were not included in the study (<1% of NACRS13).
Variables
The NACRS database provides the dates and times related to ED presentations, triage level, and disposition status. The date/time variables included registration, triage, PIA, disposition decision, and when the patient left the ED. The start of the ED presentation was set to be the minimum of the registration and triage dates and times. The start of the ED presentation was used to define fiscal year, month of year, weekday/weekend, and time of shift. Triage level represents the acuity and urgency of ED care required and is based on the Canadian Emergency Department Triage and Acuity Scale (CTAS).14,15 The triage levels were assigned by dedicated nursing staff and are defined as: resuscitation (CTAS 1), emergency (CTAS 2), urgent (CTAS 3), semi-urgent (CTAS 4), and non-urgent (CTAS 5), with corresponding timeliness of PIA (i.e., immediate, 15, 30, 60 and 120 min, respectively). Patients are assigned 1 of the 10 disposition codes according to the way in which they are released from ED, and we grouped these as discharges, admissions, transfers, deaths, and left without completion of care (e.g., patients who leave against medical advice or without being seen [LWBS]).
Demographic and geographic data were obtained from the CRF. Age is calculated as age at the date of ED presentation. Sex is coded as either male or female. The postal code and health zone of residence (North, Edmonton, Central, Calgary, South) are reported according to residence at fiscal year-end. The Postal Code Conversion File Plus16 links postal codes to census data to provide neighborhood income quintile16 and community size. Only area-level proxy of socio-economic status is available.
The PCF database provided the date a patient visited a physician and the physician type. Specialists of interest were categorized as respiratory medicine specialist and other specialists (internal medicine, pediatrician, and asthma educator). Physician claims (hereafter called follow-up visits) were extracted up to 183 days after an ED visit. The DAD database provided the date and time of the start and end of hospitalization.
Crowding metric
We used one of the recommended ED crowding metrics1 based on all presentations made by patients to a facility for any condition: time to PIA. An individual PIA was calculated as the time from ED presentation start (usually triage) to the first assessment by a physician for presentations that were not LWBS (set to 0 if PIA occurred before registration or triage in a critical situation17). For each facility, all ED visits that started within the same hour (e.g., 08:00–08:59) were used and hourly facility-specific medians for PIA were determined.
Outcome measures
Several outcomes were calculated for individual presentations. Some outcomes were only available for subsets of the data (i.e., admitted or discharged patients). In the ED, the outcomes included: disposition, ED LOS, and time from disposition decision to hospital admission. The total ED LOS depended on disposition (Canadian Institute for Health Information17). For discharged patients, ED LOS was calculated as the time from the start of ED presentation (usually triage) until the time of the disposition decision. For admitted patients, ED LOS was calculated as the time from the start of the ED presentation until time the patient left the ED. Hence, the time of the disposition decision reflects the end of the ED presentation for discharged patients, whereas the end of the ED presentation for admitted patients is when the patient left the ED. The outcomes examined outside of the ED included length of hospitalization for admitted patients. For discharged patients, outcomes were time from end of ED presentation to ED return (if appropriate), time to first follow-up visit with a physician and whether physician follow-up occurred within 7, 14, and 30 days of discharge, time to first follow-up with a respiratory medicine specialist and whether it occurred within 30 days of discharge, and time to first follow-up with other specialist and whether it occurred within 30 days of discharge.
Data analysis
Numerical summaries (e.g., means, standard deviations [SDs], IQR (represented as 25th percentile, 75th percentile]) and counts (percentages) describe data. Mixed-effects regression models assessed the association of the crowding metric with outcomes by three CTAS groups: high acuity defined as CTAS 1 or 2, moderate acuity defined as CTAS 3, and low acuity defined as CTAS 4 or 5. The few ED presentations with missing CTAS were removed from the data. The models were linear and Cox proportional hazards for duration outcomes without and with censoring, respectively, and generalized linear for categorical outcomes. Random effects accommodated the correlated data from the same patient and captured variation in the ED facility. For the time-to-event analyses, all times were censored at the March 31, 2015 study end date, except for follow-up visits, which were censored at 183 days.
The value of the crowding metric used as a covariate in the model corresponded to the same start hour and ED facility as a patient’s ED presentation. These base models provided unadjusted estimates. Predictor variables were added to the base models to obtain full models and adjusted estimates: age, sex, income quintile (1/2 vs. others), community size (≥100,000 vs. others), zone of residence, weekday/weekend, month of year, time of shift, fiscal year, and ED category. Full models assessed the effect of crowding metrics on outcomes when adjusting for important predictors. Estimates, odds ratios (ORs), and hazard ratios (HRs) were provided with 95% confidence intervals (CIs), and a p value < 0.05 was considered statistically significant. R18 and SAS19 were used for analyses.
Results
There were 764,775 presentations to the EDs by children for all conditions during the study; 25,388 (3.3%) were for children with asthma and were made by 16,056 unique children. Five presentations with missing triage levels were removed, yielding 25,383 ED presentations for asthma (16,053 unique children) for further analysis. The majority of ED presentations were made by boys (63.3%), with an average age of 7.4 years, from communities ≥100,000 (77.8%), who presented to academic/teaching hospitals (55.4%; Table 1). A small number of presentations for children occurred at adult only academic/teaching hospitals (376, 1.5%). Presentations most often occurred during the evening, were highest in the months of September and October, were lowest in the winter, and were stable across fiscal years. Presentations most commonly had an urgent (CTAS 3) triage level (13,290, 52.4%), and asthma presentations had disproportionally more resuscitation/emergency triage levels compared to children or adults presenting with any condition (Fig. 1). There were 244 (1.0%) and 7833 (30.9%) presentations that had resuscitation (CTAS 1) and emergency (CTAS 2) triage levels, respectively. Further, 3728 (14.7%) were semi-urgent presentations (CTAS 4) and 288 (1.1%) were non-urgent (CTAS 5) presentations. Of the 25,383 presentations for acute asthma, 87.2% (22,146) were discharged, 9.4% (2393) were admitted, 1.9% (494) were transferred, and 1.4% (346) left without completion of care. There was some variation by CTAS group; notably less acute patients were more likely to be discharged. While 95.7% of patients with low acuity presentations were discharged, the largest number of discharges occurred in children with moderate acuity (12,179 [55%]). Admissions resulted for 5.9% of presentations in the moderate acuity group. There were very few deaths (<10 patients), and data confidentiality agreements prevent further description.
The facility-specific hourly ED crowding metrics based on presentations for any condition and any age were calculated for all included EDs, for each hour and each day of their operation. The mean of the median PIA metric was 93 min (median = 79 min, IQR 48 min, 2 h 2 min) across all facilities and hours (Supplementary Table S1) and remained stable over the study period.
The PIA time for patients with asthma was similar to the facility-specific PIA metric (Table 2). The median PIA was 50 min (IQR 27 min, 93 min), and more acute patients had shorter PIA than less acute patients. For presentations of asthma ending in discharge (n = 22,146, Table 3), 6.6% (1469) of presentations resulted in a return to the ED within 30 days for asthma, 26.8% (5939) had a physician follow-up within 7 days, 0.8% (172) had follow-up with a respiratory medicine specialist within 30 days, and 21.1% (4681) had a follow-up with another specialist (e.g., pediatrician, asthma educator) within 30 days. For presentations of asthma ending in admission (n = 2393, Table 4), the median time from the admission decision to admission was 1 h 53 min (IQR 61 min, 3 h 38 min), and the median length of hospitalization was 2 days (IQR 1.4, 3). The medians were similar across CTAS groups. The same summaries are provided for the children who presented for conditions other than asthma (Supplementary Table S2). Children presenting for asthma generally had shorter median PIA and longer median LOSs than the children who presented for other conditions.
Individual-level PIA for patients with asthma increased by acuity group as the median PIA facility-specific metric increased (Supplementary Table S3). For every 1-h increase in median facility PIA, the individual-level PIA increased by a small amount, 13 min (95% CI: 12, 14) for the high acuity group, by larger amounts for the moderate acuity group (43 min; 95% CI: 42, 44), and the low acuity group (60 min; 95% CI: 58, 61) when adjusted by other predictors. Similarly, for every 1-h increase in median facility PIA, the LOS increased by 6, 36, and 45 min for the high, moderate, and low acuity groups, respectively. Increased median PIA was also associated with increased odds of admission for the moderate acuity group when adjusted by other predictors (adjusted OR (aOR) = 1.29; 95% CI: 1.06–1.57) and increased odds of left without completion of care for the moderate acuity (aOR = 4.72; 95% CI: 3.09–7.21) and the low acuity (uOR = 2.37; 95% CI: 1.345–4.18) groups (Supplementary Fig. S1).
For presentations of asthma ending in discharge, increased median PIA was associated with longer times to ED return for the moderate (adjusted HR (aHR) = 0.96; 95% CI: 0.93–0.99) and low acuity (aHR = 0.92; 95% CI: 0.86–0.993) groups when adjusted by predictors. In adjusted models and for presentations for asthma ending in admission, a 1-h increase in median facility PIA was associated with increased time between admission decision and admission for the high acuity (16 min, 95% CI: 2–30) and moderate acuity (20 min, 95% CI: 3–37) groups (Fig. 2). Of those presentations that ended in left without completion of care, 5.2% (18/346) experienced a return ED visit within 3 days; 0.58% (2/346) required admission. Comparatively, of the presentations that ended in discharge, 3.0% (678/22,146) experienced a return ED visit within 3 days and 0.55% (122/22,146) required admission.
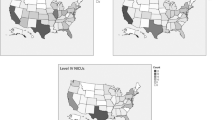
Estimates are adjusted for age, sex, income quintile, community size, patient’s zone of residence, weekday, month of year, time of shift, fiscal year, and ED category. Numerical values are provided in Supplementary Table S3. CTAS Canadian Triage and Acuity Scale, d days, ED emergency department, PIA physician initial assessment.
Discussion
This large population-based study examined individual patient-level outcomes associated with the facility-specific ED crowding metric of time to PIA for high-volume EDs during 5 consecutive years in Alberta. We have focused on the efficiency domain of medical care defined by the Institute of Medicine.20 Overall, the results have revealed several important observations. First, patients with asthma present with respiratory distress, and not surprisingly, their acuity is assessed more commonly as severe or urgent, and their PIAs are below the institutional averages for these ages. In mixed EDs seeing pediatric and adult patients, the treatment of adults did not contribute to delays in care for children. Second, despite severe crowding in these EDs, available crowding metrics remained stable over the study period, perhaps reflecting the difficulty in defining the issue from administrative data and the lack of progress addressing this issue in this province. Third, perhaps because of age and distress of patients and the anxiety of their parents, pediatric patients with asthma are seen quickly and their outcomes are excellent (<7% admission, <1% death). While any deaths are devastating and most admissions are preventable, the majority of patients respond to treatment (not detailed here), are discharged, and few relapse within the next 30 (6.6%) days. Longer times to ED return may suggest that increase PIA was a deterrent to return and/or patients have found other care options (i.e., was able to get an appointment with a family physician or ambulatory clinic).
Irrespective of the metric used to define crowding in this system, there are some important generalities in the findings. The effects of ED crowding were felt most for the less severe acuity groups (i.e., CTAS 3–5). When adjusted for other predictors, increases in median PIA increased an individual’s PIA and LOS, with lower acuity groups experiencing greater increases. These small effects are likely indicative of the ability of ED clinicians to detect patients with more severe asthma and initiate therapy quickly. It is clear that an individual’s PIA is a critical component of an individual’s total ED LOS.
The time to PIA is a portion of the overall patient ED LOS that likely reflects the impact of triage decisions on patients’ pathway and experience with ED care. The impact of ED crowding in pediatric outcomes such as asthma exacerbations has been seldom explored in the scientific literature; however, there is some evidence of delayed asthma treatment as a result of crowding.11,21
We found that a longer time to PIA increased the odds of leaving without completion of care among lower acuity patients (CTAS 3–5) compared to those classified as emergency cases at triage. Although leaving without completion of care has been proposed as an indicator of crowding and poor health outcomes,22 some evidence in adult populations indicates that patients who leave the ED without being assessed by a physician are not at a higher risk of admission within 7 days compared to those seen by physicians and discharged home after a prolonged ED LOS.23 The number of patients who leave without completion of care is closely correlated to waiting time to see a physician.24 As time to PIA increases, patient and parental satisfaction with ED care decreases25 and parents of low acuity patients with asthma may choose to leave while those with higher triage priority elect to stay in the ED until their children receive asthma care. Notably, our study shows that increases in median PIA lead to greater odds of left without completion of care. The database used for our study does not include comprehensive information on whether patients presenting really did require the level of care provided in the ED in the first place.
The admission of patients with moderate severity after a prolonged PIA can be a reflection of the impact of a poor ED flow on delays in ED treatment of time-sensitive conditions such as asthma in which delays in ED care of urgent/CTAS 3 patients may lead to worsening patient condition requiring hospitalization.
Strengths of our study include a large sample size from population-based data sources with standardized data reporting in a geographically large area of Canada. This study has several limitation that require discussion. First, there is considerable debate about the appropriate metrics to represent crowding; we use PIA, while others have used LOS. Second, every metric is a proxy for actual real-time data on the level of crowding. Since a standard measurement of crowding is not routinely recorded in most Canadian EDs, any alternative is a proxy for the conditions at the recorded time. Third, administrative data do not contain the level of detail that may better explain a direct connection between metrics and outcomes. In particular, data on procedures and medications are not available, and other measures representing the severity of the asthma in the patient are also not available. Thus we were not able to study timeliness, patient-centeredness, or equitability domains of care.20 Fourth, we have focused on relapse and follow-up, and we acknowledge that there are many other relevant short-term outcomes for children with asthma that are not available from the administrative data sources. Fifth, there may be errors or missing times; however, missing data were infrequent (<1%). Sixth, while there are effective interventions that could decrease ED presentations for asthma (e.g., action plans and asthma education), we were unable to determine who did and did not have access to either of these important asthma interventions. Finally, our results may not be generalizable to jurisdictions with different healthcare systems.
Notwithstanding the above concerns, strengths of this study included the large sample size from population-based data sources, standardized data reporting, and a geographically large area of Canada. In conclusion, the time to PIA crowding metric influenced patient outcomes during the ED presentation and showed mixed evidence of associations with longer-term outcomes. Delays in physician assessment contributed more to outcomes for less severe patients and perhaps PIA is the best metric for crowding in these patients.
References
Affleck, A., Parks, P., Drummond, A., Rowe, B. & Ovens, H. Emergency department overcrowding and access block. Can. J. Emerg. Med. 15, 59–37 (2013).
Asplin, B. R. et al. A conceptual model of emergency department crowding. Ann. Emerg. Med. 42, 173–180 (2003).
Pines, J., Hollander, J., Localio, A. R. & Metlay, J. The association between Emergency Department crowding and hospital performance on antibiotic timing for pneumonia and percutaneous intervention for myocardial infarction. Acad. Emerg. Med. 13, 873–878 (2006).
Bekmezian, A., Fee, C., Bekmezian, S., Maselli, J. H. & Weber, E. Emergency department crowding and younger age are associated with delayed corticosteroid administration to children with acute asthma. Pediatr. Emerg. Care 29, 1075–1081 (2013).
Bernstein, S. L. et al. The effect of emergency department crowding on clinically oriented outcomes. Acad. Emerg. Med. 16, 1–10 (2009).
Carter, E. J., Pouch, S. M. & Larson, E. L. The relationship between emergency department crowding and patient outcomes: a systematic review. J. Nurs. Scholarsh. 46, 106–115 (2014).
World Health Organization. Asthma. https://www.who.int/news-room/q-a-detail/asthma (2018).
Public Health Agency of Canada. Report from the Canadian Chronic Disease Surveillance System: Asthma and Chronic Obstructive Pulmonary Disease (COPD) in Canada, 2018 (Public Health Agency of Canada, Ottawa, ON, 2018).
Moorman, J. E. et al. National surveillance of asthma: United States, 2001-2010. National Center for Health Statistics. Vital Health Stat. Ser. 3 3, 1–58 (2012).
Camargo, C. A. Jr, Rachelefsky, G. & Schatz, M. Managing asthma exacerbations in the emergency department. Proc. Am. Thorac. Soc. 6, 357–366 (2009).
Sills, M. R., Fairclough, D., Ranade, D. & Kahn, M. G. Emergency department crowding is associated with decreased quality of care for children with acute asthma. Ann. Emerg. Med. 57, 191.e2007–200.e2007 (2011).
Canadian Institute of Health Information. The Canadian Enhancement of ICD-10 (International Statistical Classification of Diseases and Related Health Problems, Tenth Revision) (Canadian Institute of Health Information, Ottawa, ON, 2001).
Alberta Health and Wellness Data Disclosure Handbook (Alberta Health and Wellness, Edmonton, AB, 2003).
Bullard, M. J., Unger, B., Spence, J., Grafstein, E. & CTAS National Working Group. Revisions to the Canadian Emergency Department Triage and Acuity Scale (CTAS) adult guidelines. Can. J. Emerg. Med. 10, 136–151 (2008).
Gravel, J., Manzano, S. & Arsenault, M. Validity of the Canadian Paediatric Triage and Acuity Scale in a tertiary care hospital. Can. J. Emerg. Med. 11, 23–28 (2009).
Wilkins, R, Peters, P. A. PCCF+ Version 5K* User’s Guide. Automated Geographic Coding Based on the Statistics Canada Postal Code Conversion Files, Including Postal Codes through May 2011. Catalogue 82F0086-XDB. Health Analysis Division, Statistics Canada, Ottawa, July 2012
Canadian Institute for Health Information. eNACRS Reports: Emergency Department Wait Time Indicators (Canadian Institute for Health Information, Ottawa, ON, 2020).
R Core Team. R: A Language and Environment for Statistical Computing (R Foundation for Statistical Computing, Vienna, 2018).
SAS Institute Inc. SAS 9.4 (SAS Institute Inc, Cary, NC, 2014).
Institute of Medicine. Crossing the Quality Chasm: A New Health System for the 21st Century (The National Academies Press, Washington, DC, 2001).
Sills, M. R., Fairclough, D., Ranade, D. & Kahn, M. G. Emergency department crowding is associated with decreased quality of care for children. Pediatr. Emerg. Care 27, 837–845 (2011).
Morley, C., Unwin, M., Peterson, G. M., Stankovich, J. & Kinsman, L. Emergency department crowding: a systematic review of causes, consequences and solutions. PLoS ONE 13, e0203316 (2018).
Guttmann, A., Schull, M. J., Vermeulen, M. J. & Stukel, T. A. Association between waiting times and short term mortality and hospital admission after departure from emergency department: population based cohort study from Ontario, Canada. BMJ 342, d2983 (2011).
Kyriacou, D. N., Ricketts, V., Dyne, P. L., McCollough, M. D. & Talan, D. A. A 5-year time study analysis of emergency department patient care efficiency. Ann. Emerg. Med. 34, 326–335 (1999).
Preyde, M., Crawford, K. & Mullins, L. Patients’ satisfaction and wait times at Guelph General Hospital Emergency Department before and after implementation of a process improvement project. Can. J. Emerg. Med. 14, 157–168 (2012).
Acknowledgements
The authors thank Meng Lin of the Alberta SPOR data platform and AHS Research Data Services for providing health datasets. The authors also thank Jeffrey Bachman, MSc for accessing and preparing the Statistics Canada data and Larry Laliberte at the University of Alberta for providing the Statistics Canada data. This study was partially supported by summer student research awards to S.S. by Alberta Innovates-Health Solutions and the Women & Children’s Health Research Institute. This research has been funded by the generous support of the Stollery Children’s Hospital Foundation through the Women and Children’s Health Research Institute. This study was also supported by a grant from Alberta Health (AHW FP12-784). At the time of this project, B.H.R. was supported by Tier I Canada Research Chair in Evidence-based Emergency Medicine from the Canadian Institutes of Health Research (CIHR; Ottawa, Canada). The funding sources had no direct involvement in the study design, analysis, interpretation, or decision to submit this work.
Author information
Authors and Affiliations
Contributions
S.S. obtained summer student funding, performed initial analyses, provided an initial draft of the manuscript, and critically reviewed the manuscript for important intellectual content. B.H.R. conceptualized and designed the study, obtained funding, interpreted results, and reviewed and revised the manuscript. M.B.O. contributed to study conceptualization, results interpretation, manuscript writing, and critically reviewed the manuscript for important intellectual content. R.J.R. conceptualized and designed the study, coordinated and supervised data extraction, obtained summer student funding, directed statistical analyses, performed modeling analyses, interpreted results, and reviewed and revised the manuscript. All authors approved the final manuscript as submitted and agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Competing interests
B.H.R. received salary support from the Canadian Institutes of Health Research (CIHR; Ottawa, Canada). M.B.O., B.H.R., and R.J.R. are employees of the University of Alberta. The authors have no financial relationships with any organizations that might have an interest in the submitted work in the previous 3 years and no other relationship or activities that could appear to have influenced the submitted work. The authors have no financial relationships relevant to this article to disclose.
Ethics
The Health Research Ethics Board of the University of Alberta (Pro00056282) approved this study and patient consent was not required.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Sagaidak, S., Rowe, B.H., Ospina, M.B. et al. Emergency department crowding negatively influences outcomes for children presenting with asthma: a population-based retrospective cohort study. Pediatr Res 89, 679–685 (2021). https://doi.org/10.1038/s41390-020-0918-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41390-020-0918-2
This article is cited by
-
Emergency department crowding negatively influences outcomes for adults presenting for chronic obstructive pulmonary disease
Canadian Journal of Emergency Medicine (2023)
-
Evaluating the transitions in care for children presenting with acute asthma to emergency departments: a retrospective cohort study
BMC Emergency Medicine (2021)