Abstract
Background
A growing body of evidence defines inflammation as a hallmark feature of disease pathogenesis of Duchenne muscular dystrophy. To tailor potential immune modulatory interventions, a better understanding of immune dysregulation in Duchenne muscular dystrophy is needed. We now asked whether dystrophin deficiency affects the cascade of leukocyte recruitment.
Methods
We performed intravital microscopy on the cremaster muscle of wild-type and dystrophin-deficient mdx mice. Recruitment was triggered by preparation alone (traumatic inflammation) or in combination with scrotal TNFα injections. Neutrophilic infiltration of the cremaster muscle was assessed on tissue sections. Integrin expression on circulating neutrophils and serum levels of pro-inflammatory cytokines were measured by flow cytometry.
Results
Mdx mice show increased rolling and adhesion at baseline (traumatic inflammation) and a more profound response upon TNFα injection compared with wild-type animals. In both models, neutrophilic infiltration of the cremaster muscle is increased. Upregulation of the integrins LFA-1 and Mac-1 on circulating leukocytes and pro-inflammatory cytokines IL-6 and CCL2 in the serum points toward systemically altered immune regulation in mdx mice.
Conclusion
We are the first to show exaggerated activation of the leukocyte recruitment cascade in a dystrophin-deficient organism in vivo.
Similar content being viewed by others
Introduction
Duchenne muscular dystrophy (DMD) is an X-linked recessive disorder that is characterized by a progressive and lethal muscle wasting in male children. It is caused by a mutation in the dystrophin gene that results in a dysfunctional dystrophin–glycoprotein complex (DGC). The DGC forms a structural bridge between the extra- and intracellular matrix of cells, but also interacts with multiple membrane-bound signaling proteins, such as ion channels and pumps, G protein-coupled receptors, NOS, as well as receptors for neurotransmitters.1,2,3 Loss of function of dystrophin results in membrane fragility, impaired calcium homeostasis, necrosis, inflammation, and progressive muscle wasting.4 Besides the general susceptibility of skeleton muscles to mechanical stress in DMD patients, other contributing factors are being discussed. Altered cellular signaling, that emerges from an impaired DGC composition, may result in impaired tissue regeneration, vascular adaptation, and especially in aberrant regulation of inflammation.5 Numerous studies have identified inflammatory changes like cytokine and chemokine signaling,6,7,8 leukocyte recruitment,4,9,10,11,12 and the induction of gene expression of inflammatory pathways13,14,15,16 as key features of DMD. Further, increased infiltration of macrophages, neutrophils, eosinophils, and mast cells was observed in the dystrophic muscle9 and discussed as mediators of disease pathogenesis. Anti-inflammatory drugs such as steroids (prednisolone), nonsteroidal anti-inflammatory drugs (aspirin, ibuprofen, and parecoxib), and anti-TNFα antibodies (Remicade) have been shown to dampen inflammation by reducing immune cell infiltration and expression of cellular adhesion molecules like P-selectin, L-selectin, and ICAM-1 in mdx mice.17,18,19,20
The dystrophin-deficient mdx mouse is a widely used model to study dystrophinopathies, as a point mutation results in a loss of the full-length dystrophin likewise to many DMD cases.21 Findings by Hodgetts et al. revealed that specific depletion of neutrophils reduces muscular necrosis and inflammation in mdx mice, highlighting the importance of innate immune cells in the mdx model of DMD.22 Neutrophil recruitment follows a well-defined cascade of events of leukocyte capture from the bloodstream to subsequent stages of rolling, along the endothelium of inflamed tissue, and ultimately adhesion and transmigration. We previously showed that the receptor of advanced glycation end products (RAGE) and intercellular adhesion molecule 1 (ICAM-1) with their natural binding partners macrophage-1 antigen (Mac-1, CD11b/CD18) and lymphocyte function-associated antigen 1 (LFA-1, CD11a/CD18) mediate and regulate neutrophil recruitment in vivo.23,24,25,26 Interestingly, dysregulation of RAGE and ICAM-1 was also reported in mdx mice.27,28 We have previously shown that targeted modulation of the neutrophil recruitment cascade can curb inflammation and improve outcome.29,30 Whether the leukocyte recruitment cascade is altered in the context of dystrophin deficiency has however not been addressed in vivo, yet. Using intravital microscopy in the mdx mouse model, this study intends to further characterize leukocyte recruitment in a preclinical model of DMD to set the stage for targeted interventional studies.
Materials and methods
Animals
Mdx mice (C57Bl/10-Dmdmdx) and the respective wild-type (wt) controls (C57BL/10ScSn-Dmdmdx/J) were used for experiments at the age of 8–16 weeks. All animals were housed and bred in barrier-controlled and specific pathogen-free conditions at the IBF (Interfakultäre Biomedizinische Forschungseinrichtung), Heidelberg. Animals were cared for using guidelines that comply with local regulations for the care and use of laboratory animals. All experiments conducted were approved by local authorities and the Regierungspraesidium Karlsruhe, Baden-Wuerttemberg, Germany (AZ 35-918581/G-118/12).
Surgical preparation
Surgical preparations of the cremaster muscle were performed, as described previously.31 All experiments were conducted under intraperitoneal bolus anesthesia using ketamine 125 mg/kg (KetanestS, Pfizer Pharma GmbH, Berlin) and xylazine 12.5 mg/kg (Xylavet, CP-Pharma GmbH, Burgdorf). In brief, the cremaster muscle was dissected, exteriorized, and spread on a glass stage by needle-pin fixation, giving access to the broad plane of the muscle tissue. In TNFα- (TNFSF1A, 410-MT, R&D Systems) stimulated experiments, 500 ng of TNFα dissolved in 0.2 ml of NaCl 0.9% was injected into the scrotum 2 h prior to surgical preparation.
Intravital microscopy
IVM experiments were performed using an upright microscope (Olympus BX51W1, Hamburg, Germany) and a 40-fold objective (Zeiss Achroplan 40 × /0.80 W, Oberkochen, Germany) as previously described.32 Measurements were conducted on post-capillary venules with a diameter of 20–40 µm under continuous super-perfusion of 35 °C bicarbonate-buffered saline. Recordings were performed over 60 s. Data analysis was conducted in ImSpector Pro software (4.0.469, Lavision Biotec GmbH, Bielefeld). The following parameters were measured as described previously:33 rolling flux (number of rolling cells/min), rolling flux fraction (rolling cells/total number of cells passing the vessel within 1 min), adhesion (number of cells adhesive to the vessel wall within the field of view over 60 s/vascular surface in mm2), vessel diameter and length, center line velocity in µm/s (center line leukocyte velocity obtained from frame-by-frame video analysis), and wall shear rate γw (estimated by the formula γw = 4.9 × (8×center line velocity×0.625/vessel diameter). For the determination of the center line velocity of freely flowing leukocytes, rhodamine staining (0.2 mg/kg body weight) with consecutive fluorescence microscopy was performed.
Systemic leukocyte count
Peripheral leukocyte blood cell counts were acquired under the light microscope from 10 µl of whole blood stained with 90 µl of Türk’s solution (Merck, Germany).
Whole-mount histology
Whole-mount histology with Giemsa staining (Giemsa Stain Modified Solution, Fluka Analytical) of the cremaster muscle tissue was performed as described before.34 Images were recorded by upright microscopy (Leica DM4000 B LED), using a 63 × 10-fold oil immersion objective from Leica, Germany. All neutrophils outside the vessel were counted and reported as the number of neutrophils per square millimeter. The view field had a circular diameter of 0.345 mm and was bisected by the blood vessel of interest.
Flow cytometry
The expression of LFA-1 and Mac-1 on circulating leukocytes was analyzed by flow cytometry. After lysis of red blood cells, leukocytes were collected by repeated centrifugation and resuspension in FACS buffer and incubated with the respective APC- conjugated antibodies (eBioscience) at concentrations of 1-µl antibody per 1 million cells: rat anti-mouse CD11a κ (REF 17-0111) and CD11b κ (REF 17-0112), as well as rat IgG2a κ and IgG2b κ iso-controls (REF 17-4321 and REF 17-4031). Measurements were performed by a LSR II cytometer (BD Biosciences) and analyzed by FACSDiva and FlowJo software.
Cytometric bead array (CBA)
Cytokine concentrations in mouse sera were analyzed by the use of the CBA mouse inflammation kit (BD Biosciences, San Jose). The cytokines interleukin-6 (IL-6), interleukin-10 (IL-10), monocyte chemoattractant protein-1 (MCP-1, also known as CCL2), interferon-γ (IFN-γ), tumor necrosis factor (TNF), and interleukin-12p70 (IL-12p70) are included in the kit. The CBA kit contains a mixture of six different capture beads with distinct fluorescence intensities. The different capture beads are conjugated with a specific antibody. Detector reagent containing PE-conjugated detection antibodies and the samples containing the analytes are incubated, forming sandwich complexes (capture bead + analyte + detection reagent) that can be analyzed by using flow cytometry. PE fluorescence intensity correlates with cytokine concentration. Measurements and settings were performed according to BD manual instructions, using a LSR II cytometer (BD Biosciences) and analyzed by FACSDiva and FCAP Array™ software.
Statistics
All statistics were performed using Prism software (version 5.01, GraphPad Software Inc.). Gaussian distribution was analyzed using D’Agostino & Pearson omnibus normality test. In the case of Gaussian distribution, the two-tailed, unpaired Student’s t test was used. In the case of non-Gaussian distribution, the nonparametric Mann–Whitney U test was used. Significance was set at p < 0.05. Data are presented as mean + SEM. For logarithmic data like mean fluorescent intensities (MFIs) from flow cytometry, geometric means were used for statistical analysis and data presentation.
Results
To assess leukocyte recruitment in dystrophin-deficient mdx mice, we performed IVM on post-capillary venules of the cremaster muscle and quantified leukocyte transmigration into the inflamed muscle tissue. Preparation of the tissue itself induces mild inflammation; however, this IVM method still reflects the inflammatory state at baseline as closely as technically possible. In the following, this preparation will be referred to as the “trauma” setting. TNFα injections are meant to mimic recruitment in a stage of immune activation. Figure 1 depicts the experimental setup for IVM experiments. Hemodynamic and microvascular parameters (shear rate, center line velocity, and vessel diameter), as well as peripheral leukocyte counts of mdx mice and wt mice, did not differ (Fig. 1c). Also, rolling velocities were comparable between wt and mdx mice (Supplemental Figure S1 (online)).
Introduction to IVM experiments. a Schematic drawing of a male mouse dissected for IVM measurements. Cremaster post-capillary venules were identified at the junction of two confluent vessels. Video recordings were performed with an upright microscope following offline analysis. b For each venule, the rolling flux fraction and the number of adherent cells was recorded. The number of transmigrated polymorphonuclear leukocytes (PMN) was determined after fixation and staining. c Hemodynamic and microvascular parameters like shear rate, center line velocity, and vessel diameter, as well as systemic leukocyte counts, did not differ between wt and mdx mice. In total, 83 venules were recorded in mdx mice and 76 venules in wt mice from five mice per group. All data are presented as mean + SEM, n.s. not significant
Leukocyte recruitment is enhanced in mdx mice
In the trauma model, mdx mice showed a higher (p < 0.0001) fraction of rolling leukocytes (26.6 ± 3.137%, mean ± SEM) compared with wt animals (7.993 ± 1.169%, mean ± SEM) (Fig. 2a). Within the same venule, leukocyte adhesion to the endothelial wall was analyzed as the number of leukocytes that did not move their position over 60 s. Mdx mice showed a higher (p < 0.0001) number of adherent leukocytes (679.3 ± 55.28 [n]/m2, mean ± SEM) compared with wt mice (383.5 ± 48.62 [n]/m2, mean ± SEM) (Fig. 2b). IVM data were acquired from 83 venules recorded in mdx and 76 recorded in wt mice taken from five animals per group.
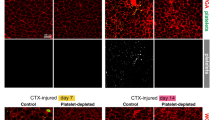
Mdx mice show enhanced leukocyte recruitment during trauma-induced inflammation. a Mdx mice show increased leukocyte rolling. For visualization, two representative image illustrations of IVM video recordings in wt and mdx mice were generated from stacked images with a temporal delay of 1 s. Spatial movement of rolling cells is illustrated by a red transparent shade. p < 0.0001, wt mice n = 5 (76 venules), and mdx mice n = 5 (83 venules). b Mdx mice show increased leukocyte adhesion. The same two image illustrations as in a were taken to display cell adhesion; the same vessels were analyzed as in a. Adherent cells are marked by a red circle. p < 0.0001. c Mdx mice show increased extravasation of PMN. Representative images are shown after tissue fixation and Giemsa staining. p < 0.05, wt mice n = 5 (29 vessels), and mdx mice n = 6 (36 vessels). All data are presented as mean + SEM. Asterisks indicate statistical significance, set at p < 0.05
Transmigration is enhanced in mdx mice
Leukocyte transmigration was assessed after tissue fixation and leukocyte staining. Each venule analyzed was placed to bisect the field of view at 630-fold magnification. The number of neutrophilic granulocytes outside the vessel per field of view was assessed. Mdx mice (1092 ± 214.7, mean ± SEM) showed a higher (p < 0.05) number of extravasated polymorphonuclear cells (PMN) compared with wt mice (589.5 ± 63.51, mean ± SEM) (Fig. 2c). In mdx mice, 36 image sections were analyzed, and 29 in wt mice taken from five animals per group.
TNFα-induced leukocyte recruitment
Local application of TNFα is a strong inducer of inflammation. As reported from other mice strains, TNFα enhances leukocyte arrest and subsequent transmigration.23,32 Wild-type controls showed the expected increase of leukocyte adhesion (647.0 ± 65.69, mean ± SEM) following local TNFα stimulation, compared with the respective data from the trauma model (p < 0.005). Further, mdx mice revealed a stimulus-dependent enhancement (p < 0.001) of leukocyte adhesion (1035 ± 93.40, mean ± SEM), which exceeded adhesion in wt animals (p < 0.001) (Fig. 3b). IVM data were acquired from 58 venules recorded in mdx and 66 recorded in wt mice taken from five animals per group.
Mdx mice show enhanced leukocyte recruitment during TNFα-induced inflammation. As an analog to Fig. 2, rolling flux fraction, cell adhesion, and transmigration were studied in TNFα-induced inflammation. a Rolling flux fraction is not statistically different between wt and mdx mice (p > 0.05). b Leukocyte adhesion is enhanced in mdx mice (p < 0.001), wt mice n = 5 (66 venules), and mdx mice n = 5 (58 venules). c Mdx mice show increased (p < 0.05) extravasation of PMN cells after TNFα-induced inflammation, wt mice n = 5 (36 vessels), and mdx mice n = 5 (45 vessels). All data are presented as mean + SEM. Asterisks indicate statistical significance, set at p < 0.05
Transmigration again was higher (p < 0.05) in mdx mice (997.6 ± 101.2, mean ± SEM). In mdx mice, 45 image sections were analyzed taken from five animals, and 36 in wt mice taken from four animals.
Integrin expression is enhanced in mdx mice
Leukocyte arrest is mediated through integrins like LFA-1 and Mac-1. As shown in Fig. 4, the expression of LFA-1 was higher (p < 0.05) in mdx mice (411.4 ± 21.17, geometric mean ± SEM, n = 14) compared with wt controls (282.5 ± 61.16, geometric mean ± SEM, n = 9). Also, the expression of Mac-1 was higher (p < 0.05) in mdx mice (477.2 ± 28.75, geometric mean ± SEM, n = 14) than in wt controls (328.8 ± 34.06, geometric mean ± SEM, n = 12). Taken together, mdx mice show enhanced integrin expression.
Integrin expression on circulating neutrophils is enhanced in mdx mice. LFA-1 and Mac-1 expression levels on neutrophils from wt and mdx mice were measured by flow cytometry. a Representative histogram with the respective isotype controls for LFA-1 expression. Mdx neutrophils show increased expression of LFA-1 (n = 9–14 animals per group). b Representative histogram with the respective isotype controls for Mac-1 expression. Mdx neutrophils show increased expression of Mac-1 (n = 12–14 animals per group). All data are presented as geometric mean + SEM. Asterisks indicate statistical significance, set at p < 0.05
Cytokine expression is enhanced in mdx mice
We used a bead array with a known fluorescence concentration ratio to measure systemic cytokine levels in blood serum (Fig. 5). Mdx mice (2.150 ± 0.798, mean ± SEM) showed higher (p < 0.05) concentrations of IL-6 compared with wt mice (0.3377 ± 0.2772, mean ± SEM). We further found enhanced CCL2 expression (p < 0.05) in mdx mice (50.15 ± 8.066, mean ± SEM) compared with wt mice (25.35 ± 6.766, mean ± SEM). Data were acquired from 14 animals per group. Concentrations are presented as [pg/ml].
Mdx mice exhibit elevated systemic pro-inflammatory cytokines. The serum levels of pro-inflammatory cytokines IL-6 and CCL2 were analyzed via cytometric bead array. a Dotplots of fluorescent intensity of both IL-6 and CCL2 from a representative wt and mdx mouse. b Serum concentrations were calculated from standard measurements. Mdx mice show significant induction of both IL-6 and CCL2 in blood serum. Data are presented as mean + SEM from n = 14 animals per group. Asterisks indicate statistical significance, set at p < 0.05
The concentration of IL-10, IFN-γ, and IL-12p70 was below the detection threshold of the CBA kit in wt and mdx mice. For TNF, four versus three values above the threshold were detected, showing slightly higher levels in mdx mice (1.053 ± 0.4727, mean ± SEM) compared with wt mice (0.8550 ± 0.5476, mean ± SEM). Due to the small set of data and the majority of samples below the detection threshold, TNF results were not considered for statistical analysis.
Discussion
Despite substantial scientific progress, the exact pathogenesis of muscular dystrophy caused by dystrophin deficiency remains unclear. In addition to its structural importance as a linking element between intracellular actin filaments and the extracellular matrix, functional aspects of dystrophin and the DGP like signaling or ion channel stabilization have been highlighted lately3,5 and support a multifactorial pathogenesis. Inflammation has been shown to be a key feature of disease progression in early13,14 and the late clinical stages.35,36 Yet, little is known about individual aspects of inflammation like the innate immune response. Here, we provide novel insights into inflammatory regulation of leukocyte recruitment in the dystrophin-deficient mdx mouse.
We employed two standard models for the study of leukocyte recruitment on the cremaster muscle in vivo, and found enhanced recruitment of leukocytes in mdx mice. This core finding is in line with earlier reports of elevated numbers of neutrophils in dystrophin-deficient muscle tissue.4,9 Of note, it was shown that most intraluminal and perivascular leukocytes in the cremaster model are neutrophils.29 Importantly, cremaster muscle fibers of mdx mice are shown to be centrally nucleated,37 and abdominal wall muscle (representing the embryogenic origin of the cremaster muscle) was identified as fibrotic in mdx mice.38 These dystrophic tissue features of the cremaster muscle are important when extrapolating the significance of our findings to more relevant muscle groups in mdx mice and DMD patients, which are however technically difficult to study via IVM.
In the trauma setting, all stages of leukocyte recruitment—rolling, adherence, and transmigration—were activated in mdx mice. In the TNFα model, the rolling flux fraction was however not significantly elevated, which might be explained by the greater number of adherent neutrophils and a consequently reduced pool of circulating neutrophils. Considering comparable white blood cell counts, the actual rolling capacity might therefore be underestimated by a lack of available leukocytes. Interestingly, our baseline IVM data on wt animals differ from previously published results by our own group. Whereas adhesion in the trauma model has been robust between 420 and 550/mm2 and around 800/mm2 in the TNFα model,23,26 we now report lower values of the rolling flux fraction for both trauma and TNFα models in wt animals.
These relevant baseline differences might be due to strain differences between previously used C57BL/6 and the currently used C57BL/10 mice, which to our knowledge, have not yet been studied by IVM. Of note, infiltration of the cremaster muscle is comparable between C57BL/632 and our wt C57BL/10 mice around 600/mm2 in the TNFα model.
Selectins and integrins play a central role in reducing the rolling velocity of leukocytes, leading to their arrest at the endothelial wall.32 Selectin-dependent rolling velocities were shown to be comparable between wt and mdx mice. Interestingly, ICAM-1 and RAGE, the two main endothelial integrin-binding receptors, have been shown to be upregulated in mdx mice, and a reduction of RAGE activity restrains inflammation and enhances muscle strength.27,28 We now report the upregulation of both LFA-1 and Mac-1 on circulating neutrophils in mdx mice, which might imply global activation of leukocyte recruitment. On a systemic level, pro-inflammatory cytokines govern leukocyte activation and recruitment. CCL2 is a central cytokine involved in the recruitment of immune cells to the side of inflammation, whereas IL-6 mediates chemotaxis of neutrophils. We found upregulation of both cytokines in the blood of mdx mice, which is in line with previously reported upregulation of pro-inflammatory cytokines in the context of dystrophin deficiency.6,12 Interestingly, the absolute IL-6 concentrations reported from DMD patients of 3.77 ± 2.71 pg/mL,6,39 are comparable with elevated murine levels in our hands (2.150 ± 0.798 pg/ml).
Our descriptive work does not allow for potential causative deductions. Also, interspecies translation should be critically evaluated, especially as a variety of mutations in the dystrophin gene are known to cause DMD in humans. It is however worth noting that global activation of leukocyte recruitment is likely to have consequences beyond the skeletal muscle in DMD. Interestingly, induction of inflammatory pathways was reported to precede muscle dysfunction in DMD patients.13,15 Also, Fujita et al. showed that chimeric mdx mice receiving wt bone marrow showed improved muscle function.40 Combined, these data might point toward a potential primary immune defect in dystrophin-deficient organisms, independent of muscular inflammation and wasting. To discriminate a potential primary origin of inflammation from secondary effects in DMD however warrants further investigation.
In conclusion, our results indicate that the cascade of leukocyte recruitment is altered in dystrophin-deficient mdx mice. A better understanding of this aspect of immune disruption seen in dystrophin-deficient organisms may provide alternative targets for supportive therapies in treating patients with DMD.
References
Knuesel, I. et al. Short communication: altered synaptic clustering of GABAA receptors in mice lacking dystrophin (mdx mice). Eur. J. Neurosci. 11, 4457–4462 (1999).
Brunig, I., Suter, A., Knuesel, I., Luscher, B. & Fritschy, J. M. GABAergic terminals are required for postsynaptic clustering of dystrophin but not of GABA(A) receptors and gephyrin. J. Neurosci. 22, 4805–4813 (2002).
Constantin, B. Dystrophin complex functions as a scaffold for signalling proteins. Biochim. Biophys. Acta 1838, 635–642 (2014).
Evans, N. P., Misyak, S. A., Robertson, J. L., Bassaganya-Riera, J. & Grange, R. W. Immune-mediated mechanisms potentially regulate the disease time-course of duchenne muscular dystrophy and provide targets for therapeutic intervention. PM R. 1, 755–768 (2009).
Deconinck, N. & Dan, B. Pathophysiology of duchenne muscular dystrophy: current hypotheses. Pediatr. Neurol. 36, 1–7 (2007).
De Paepe, B. & De Bleecker, J. L. Cytokines and chemokines as regulators of skeletal muscle inflammation: presenting the case of Duchenne muscular dystrophy. Mediat Inflamm. 2013, 540370 (2013).
Poston, R. N., Haskard, D. O., Coucher, J. R., Gall, N. P. & Johnson-Tidey, R. R. Expression of intercellular adhesion molecule-1 in atherosclerotic plaques. Am. J. Pathol. 140, 665–673 (1992).
De Bleecker, J. L. & Engel, A. G. Expression of cell adhesion molecules in inflammatory myopathies and Duchenne dystrophy. J. Neuropathol. Exp. Neurol. 53, 369–376 (1994).
Spencer, M. J. & Tidball, J. G. Do immune cells promote the pathology of dystrophin-deficient myopathies? Neuromuscul. Disord. 11, 556–564 (2001).
Spencer, M. J., Montecino-Rodriguez, E., Dorshkind, K. & Tidball, J. G. Helper (CD4(+)) and cytotoxic (CD8(+)) T cells promote the pathology of dystrophin-deficient muscle. Clin. Immunol. 98, 235–243 (2001).
Madaro, L. & Bouche, M. From innate to adaptive immune response in muscular dystrophies and skeletal muscle regeneration: the role of lymphocytes. Biomed. Res. Int. 2014, 438675 (2014).
Porter, J. D. et al. Persistent over-expression of specific CC class chemokines correlates with macrophage and T-cell recruitment in mdx skeletal muscle. Neuromuscul. Disord. 13, 223–235 (2003).
Pescatori, M. et al. Gene expression profiling in the early phases of DMD: a constant molecular signature characterizes DMD muscle from early postnatal life throughout disease progression. FASEB J. 21, 1210–1226 (2007).
Chen, Y. W. et al. Early onset of inflammation and later involvement of TGFbeta in Duchenne muscular dystrophy. Neurology 65, 826–834 (2005).
Haslett, J. N. et al. Gene expression comparison of biopsies from Duchenne muscular dystrophy (DMD) and normal skeletal muscle. Proc. Natl Acad. Sci. USA 99, 15000–15005 (2002).
Acharyya, S. et al. Interplay of IKK/NF-kappaB signaling in macrophages and myofibers promotes muscle degeneration in Duchenne muscular dystrophy. J. Clin. Invest 117, 889–901 (2007).
Wehling-Henricks, M., Lee, J. J. & Tidball, J. G. Prednisolone decreases cellular adhesion molecules required for inflammatory cell infiltration in dystrophin-deficient skeletal muscle. Neuromuscul. Disord. 14, 483–490 (2004).
Granchelli, J. A., Pollina, C. & Hudecki, M. S. Pre-clinical screening of drugs using the mdx mouse. Neuromuscul. Disord. 10, 235–239 (2000).
Serra, F. et al. Inflammation in muscular dystrophy and the beneficial effects of non-steroidal anti-inflammatory drugs. Muscle Nerve 46, 773–784 (2012).
Grounds, M. D. & Torrisi, J. Anti-TNFalpha (Remicade) therapy protects dystrophic skeletal muscle from necrosis. FASEB J. 18, 676–682 (2004).
Sicinski, P. et al. The molecular basis of muscular dystrophy in the mdx mouse: a point mutation. Science 244, 1578–1580 (1989).
Hodgetts, S., Radley, H., Davies, M. & Grounds, M. D. Reduced necrosis of dystrophic muscle by depletion of host neutrophils, or blocking TNFalpha function with Etanercept in mdx mice. Neuromuscul. Disord. 16, 591–602 (2006).
Frommhold, D. et al. RAGE and ICAM-1 cooperate in mediating leukocyte recruitment during acute inflammation in vivo. Blood 116, 841–849 (2010).
Frommhold, D. et al. RAGE and ICAM-1 differentially control leukocyte recruitment during acute inflammation in a stimulus-dependent manner. BMC Immunol. 12, 56–68 (2011).
Braach, N. et al. Anti-inflammatory functions of protein C require RAGE and ICAM-1 in a stimulus-dependent manner. Mediat Inflamm. 2014, 743678 (2014).
Braach, N. et al. RAGE controls activation and anti-inflammatory signalling of protein C. PLoS ONE 9, e89422 (2014).
Sagheddu, R. et al. Targeting RAGE as a potential therapeutic approach to Duchenne muscular dystrophy. Hum. Mol. Genet 27, 3734–3746 (2018).
Torres-Palsa, M. J. et al. Expression of intercellular adhesion molecule-1 by myofibers in mdx mice. Muscle Nerve 52, 795–802 (2015).
Frommhold, D. et al. Protein C concentrate controls leukocyte recruitment during inflammation and improves survival during endotoxemia after efficient in vivo activation. Am. J. Pathol. 179, 2637–2650 (2011).
Buschmann, K. et al. The olive oil-based lipid clinoleic blocks leukocyte recruitment and improves survival during systemic inflammation: a comparative in vivo study of different parenteral lipid emulsions. Mediat. Inflamm. 2015, 757059 (2015).
Sperandio, M. et al. Alpha 2,3-sialyltransferase-IV is essential for L-selectin ligand function in inflammation. Eur. J. Immunol. 36, 3207–3215 (2006).
Frommhold, D. et al. Sialyltransferase ST3Gal-IV controls CXCR2-mediated firm leukocyte arrest during inflammation. J. Exp. Med. 205, 1435–1446 (2008).
Sperandio, M., Pickard, J., Unnikrishnan, S., Acton, S. T. & Ley, K. Analysis of leukocyte rolling in vivo and in vitro. Methods Enzym. 416, 346–371 (2006).
Forlow, S. B. & Ley, K. Selectin-independent leukocyte rolling and adhesion in mice deficient in E-, P-, and L-selectin and ICAM-1. Am. J. Physiol. Heart Circ. Physiol. 280, H634–H641 (2001).
Villalta, S. A., Rosenberg, A. S. & Bluestone, J. A. The immune system in Duchenne muscular dystrophy: Friend or foe. Rare Dis. 3, e1010966 (2015).
Kastenschmidt, J. M., Avetyan, I. & Villalta, S. A. Characterization of the inflammatory response in dystrophic muscle using flow cytometry. Methods Mol. Biol. 1687, 43–56 (2018).
Sato, K., Yokota, T., Ichioka, S., Shibata, M. & Takeda, S. Vasodilation of intramuscular arterioles under shear stress in dystrophin-deficient skeletal muscle is impaired through decreased nNOS expression. Acta Myol. 27, 30–36 (2008).
Gardner, B. B., Swaggart, K. A., Kim, G., Watson, S. & McNally, E. M. Cardiac function in muscular dystrophy associates with abdominal muscle pathology. J. Neuromuscul. Dis. 2, 39–49 (2015).
Rufo, A. et al. Mechanisms inducing low bone density in Duchenne muscular dystrophy in mice and humans. J. Bone Min. Res. 26, 1891–1903 (2011).
Fujita, R. et al. Endogenous mesenchymal stromal cells in bone marrow are required to preserve muscle function in mdx mice. Stem Cells 33, 962–975 (2015).
Acknowledgements
We are grateful to Britta Heckmann, Silvia Pezer, and Melitta Weissinger for excellent technical and experimental assistance. This study was supported by grants from the German Federal Ministry of Education and Research (BMBF) 01GL1746E as part of the PRIMAL Consortium and from the German Research Foundation (DFG) FR3068/4-1.
Author information
Authors and Affiliations
Contributions
All authors have met the Pediatric Research authorship requirements. S.K. designed experiments, acquired, analyzed, and interpreted data and wrote the paper. R.T., M.B., C.P., and J.P. interpreted data and revised the paper. D.F. designed experiments, interpreted data, and revised the paper. H.H. designed experiments, interpreted data, and wrote the paper. All authors read and approved the final version to be published.
Corresponding author
Ethics declarations
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Kranig, S., Tschada, R., Braun, M. et al. Dystrophin deficiency promotes leukocyte recruitment in mdx mice. Pediatr Res 86, 188–194 (2019). https://doi.org/10.1038/s41390-019-0427-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41390-019-0427-3
This article is cited by
-
The linkage between inflammation and fibrosis in muscular dystrophies: The axis autotaxin–lysophosphatidic acid as a new therapeutic target?
Journal of Cell Communication and Signaling (2021)