Abstract
Background
Premature infants often develop enteric dysbiosis with a preponderance of Gammaproteobacteria, which has been related to adverse clinical outcomes. We investigated the relationship between increasing fecal Gammaproteobacteria and mucosal inflammation, measured by fecal calprotectin (FC).
Methods
Stool samples were collected from very-low-birth weight (VLBW) infants at ≤2, 3, and 4 weeks’ postnatal age. Fecal microbiome was surveyed using polymerase chain reaction amplification of the V4 region of 16S ribosomal RNA, and FC was measured by enzyme immunoassay.
Results
We enrolled 45 VLBW infants (gestation 27.9 ± 2.2 weeks, birth weight 1126 ± 208 g) and obtained stool samples at 9.9 ± 3, 20.7 ± 4.1, and 29.4 ± 4.9 days. FC was positively correlated with the genus Klebsiella (r = 0.207, p = 0.034) and its dominant amplicon sequence variant (r = 0.290, p = 0.003), but not with the relative abundance of total Gammaproteobacteria. Klebsiella colonized the gut in two distinct patterns: some infants started with low Klebsiella abundance and gained these bacteria over time, whereas others began with very high Klebsiella abundance.
Conclusion
In premature infants, FC correlated with relative abundance of a specific pathobiont, Klebsiella, and not with that of the class Gammaproteobacteria. These findings indicate a need to define dysbiosis at genera or higher levels of resolution.
Similar content being viewed by others
Introduction
In healthy, full-term neonates, the intestine is seeded by microbial inocula received from the birth canal, maternal skin, and milk, and the gut microbiome is dominated by Gram-positive Firmicutes such as Staphylococcus, Propionibacterium, Bifidobacterium, and Lactobacillus.1 Increasing pre-clinical and epidemiological information now acknowledges the positive influence of these bacteria on mucosal homeostasis, immunity, nutrient absorption, and energy regulation in the neonatal intestine.2,3 In contrast, in preterm infants, the intestinal microbiome may develop very differently.4 In these infants, the hospital microflora may contribute more to the gut microbiome, whereas the maternal influence may be curtailed due to shortened labor or a Cesarean birth, limited physical contact with the mother, and periods of enteral fasting. There may be additional selection pressures from broad-spectrum antibiotics, indwelling tubes and catheters, intestinal dysmotility, and immaturity of barriers such as gastric acid, secretory immunoglobulin A, and mucus.1 Not surprisingly, many preterm infants develop an enteric dysbiosis with a preponderance of Gram-negative bacteria of the class Gammaproteobacteria and its constituent families Enterobacteriaceae, Vibrionaceae, and Pseudomonadaceae.5,6,7,8 Emerging epidemiological data link such dysbiosis with adverse outcomes such as necrotizing enterocolitis (NEC), cholestasis, and developmental delay,4,6,7,9 but the mechanism(s) by which Gammaproteobacteria present in the bowel lumen may evoke inflammatory responses are not well understood. Intestinal epithelium and many resident immune cell lineages are normally tolerant of Gram-negative bacteria,10 and further study is needed to ascertain if dysbiosis secondary to a Gammaproteobacterial bloom may induce mucosal inflammation when the relative abundance of Gammaproteobacteria exceeds a critical threshold, or is associated with an increase in specific pathobionts in this class of bacteria.
In this prospective observational study, we investigated the relationship between fecal Gammaproteobacteria and mucosal inflammation in premature infants. We used fecal calprotectin (FC), which is derived from neutrophils and inflammatory macrophages present in the mucosa, as the inflammatory marker.11 Preterm infants tend to have greater variability in FC expression than older children and adults, but several studies now show FC to be a useful marker of intestinal inflammation and NEC when cut-off values between 200 and 300 µg/g of stool were used.11,12,13,14 We hypothesized that FC increases in preterm infants as a function of the relative abundance of Gammaproteobacteria in stool. To test this hypothesis, we recorded demographic and clinical information from a cohort of very-low-birth weight (VLBW) infants, surveyed their fecal microbiome, and measured FC at serial time-points during the neonatal period.
Methods
Demographic and clinical information
This study was performed at the University of South Florida and the affiliated Tampa General Hospital (TGH) under appropriate oversight from the Institutional Review Boards. The neonatal intensive care unit (NICU) at TGH is an academic regional referral center with a single-patient room floor plan. All eligible VLBW infants were enrolled during the period May 2012 to December 2013; inclusion criteria included birth weight <1500 g, availability of a stool sample in the first 2 weeks after birth, and parental informed consent. Infants with major congenital anomalies or lethal chromosomal disorders were excluded. Three stool samples were obtained from each infant at ≤2, 3rd, and the 4th week after birth and stored at −80 °C until the time of analysis. Biological samples were handled under uniform conditions per accepted guidelines (biospecimen reporting for improved study quality).15
Fecal DNA amplification
Total DNA was extracted from 100 to 250 mg of stool (MoBio PowerFecal DNA Kit, Qiagen, Carlsbad, CA,USA) and V4 region of bacterial 16S ribosomal RNA (rRNA) gene was amplified by polymerase chain reaction with modified 515F and 806R primers.16 Amplicons were sequenced according to Illumina MiSeq protocol (Illumina, San Diego, CA, USA) to generate about 15,000 of 250 base-pair paired-end reads per sample.
Metagenomic analysis
Demultiplexed DNA sequences were first uploaded to the CLC Biomedical Workbench 3.5.3 (Qiagen) and analyzed for bacterial classifications to the genus level. Bacterial operational taxonomic units (OTUs) were mapped to the Greengenes v13.8 reference database at 97% similarity, and their relative abundances (%) were computed. Diversity within samples (α-diversity) were measured and represented by the number of OTUs, phylodiversity, Chao 1, Simpson, and Shannon indices. To improve taxonomic resolution, we next used the Divisive Amplicon De-noising Algorithm 2 (DADA2) to characterize bacterial OTUs to amplicon sequence variants (ASVs). This two-step analysis provided information on OTUs to allow comparison with existing studies of the preterm microbiome,5,6,7,17,18,19 and allowed validation of our results with the DADA2 pipeline that relies on a different, model-based approach to minimize amplicon errors.
Changes in the abundance of individual OTUs were investigated using Gneiss (balance tree) analysis.20 Due to the compositional nature of 16S rRNA gene sequence data, the relative (proportional) abundance of a taxon could be altered either due to a change in its own numbers or due to a shift in the relative abundance of other taxa. Balance tree analysis circumvents this problem by leveraging the correlation between co-occurring taxa to infer meaningful properties of sub-communities, rather than individual taxa.
FC measurements
We used a commercially available enzyme immunoassay (PhiCal, Genova Diagnostics, Ashville, NC, USA). The linear range of measurement for this assay is 25–2500 μg/g stool.
Statistical analysis
Clinical and demographic data were analyzed using SPSS 25 (IBM, Armonk, NY, USA). Scalar variables were compared by Friedman’s test for repeated measures or the Mann–Whitney U test, and categorical variables by Fisher’s exact test. Linear mixed-effects models were used to identify determinants of FC and Klebsiella abundance. Small-for-gestational age, ethnicity, vaginal birth, antenatal steroids, magnesium sulfate, chorioamnionitis, gender, multiple births, postnatal age, enteral feedings (binary), respiratory distress syndrome, patency of ductus arteriosus, sepsis, red blood cell transfusions (binary), and Klebsiella abundance were defined as fixed effects as all possible levels of the variable were represented in the cohort. Maternal body mass index (BMI), birth weight, gestation, post-menstrual age at stool collection, duration of ruptured membranes, and days of antibiotic treatment were defined as random effects. Mixed-effects procedures were performed using the maximum likelihood method and an autoregressive covariance matrix (with heterogeneous variances) as the dependent variables were anticipated to diverge with time. Best-fitting models were identified by −2 log likelihood, Akaike’s information criterion, and Schwarz’s Bayesian criterion. Important independent variables were shortlisted using bootstrap bagging, where a bootstrap dataset was constructed by not sampling a third of all subjects and replacing these by an equal number of duplicated samples. The bootstrap sample was analyzed by logistic regression with entry criterion of p < 0.2. To avoid model overfitting, multivariable analyses were limited to biologically plausible associations, to main effects for baseline measures, and time-dependent covariates for longitudinal measures.
We also performed linear regression to identify predictors of FC at different time-points of stool collection. Independent variables were tested with entry at p < 0.2 and acceptance at p < 0.05, first using a one-step forced entry and then “stepwise” in the sequence of appearance during perinatal period. In addition to the variables listed above, duration of iron therapy was also tested. To identify highly correlated variables, multicollinearity diagnostics (tolerance values <0.2, variance inflation factors >10) were reviewed. Independence of variables was confirmed by the Durbin–Watson statistic (acceptable range 1.5–2.5). Scatterplots of standardized residuals vs. standardized predicted values were evaluated for homoscedasticity and non-linearity. Normality of residuals was confirmed by evaluation of histograms. To determine Klebsiella abundance levels associated with elevated FC, we computed receiver-operating characteristics (ROCs) by plotting sensitivity vs. 1-specificity and identified “cut-off” abundance values at the highest sum of sensitivity and specificity (Youden’s J statistic). Statistical tests were two-tailed and considered significant at p < 0.05.
Results
Demographic and clinical information
We enrolled 45 eligible VLBW infants admitted to our NICU between May 2012 and December 2013. The clinical characteristics of this cohort have been described in part, elsewhere.21 These infants were born at a gestation (mean ± standard deviation, SD) of 27.9 ± 2.2 weeks, with birth weight 1126 ± 208 g. Their clinical characteristics are summarized in Table 1 of our previous publication.22
Fecal calprotectin
Stool samples for the ≤2, 3rd, and 4th week time-points were collected at postnatal age (mean ± SD) 9.9 ± 3, 20.7 ± 4.1, and 29.4 ± 4.9 days; and post-menstrual age 29.8 ± 2.3, 31.2 ± 1.9, and 32.6 ± 1.9 weeks, respectively. FC levels remained stable over time (median (interquartile range/IQR): 161 (101–277), 187 (132–306), and 152 (102–311) µg/g stool in ≤2, 3rd, and 4th week, respectively; Friedman’s test; difference not significant (NS)).
Fecal microbiome
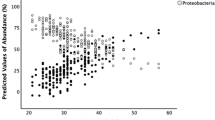
A total of 2,017,727 reads was obtained (mean ± SD 15,285 ± 7,139 sequences per sample). The α-diversity metrics (number of OTUs, phylodiversity, and Shannon, Chao 1, and Simpson indices) increased with postnatal age (Fig. 1). The relative abundance of Proteobacteria increased over time, comprising 46% (median; IQR = 0–90%) of all reads at ≤2 weeks, 83.5% (54.8–93.3%) in the 3rd week, and 77% (57–88.3%) in the 4th week (p < 0.001). Gammaproteobacteria accounted for 42.5% (0–90%) of all reads in ≤2 weeks, 69.7% (29.9–86.9%) in the 3rd, and 75.5% (54.5–86%) in the 4th week stool samples (p < 0.001). Klebsiella were the dominant Gammaproteobacterial genus: median (IQR) 44% (2–98%), 85% (0–98%), and 78.5% (11.3–97.5%) in the <2nd, 3rd, and 4th week stool samples, respectively, as summarized in Supplemental Table 3 of our previous publication.22 An ASV of Klebsiella accounted for nearly a third of all reads in weeks 3–4 (median 0.18% (IQR 0–65%) at ≤2 weeks, 24.6% (0–80%) in the 3rd, and 26.2% (0.1–66.9%) in the 4th week (NS)).
Predictors of FC
In bivariate analyses, FC was positively correlated with birth weight (Spearman’s r = 0.337, p < 0.001), particularly during the 3rd (r = 0.417, p = 0.009) and 4th weeks (r = 0.501, p = 0.005), but not with gestation or post-menstrual age. There was no correlation between FC and the relative abundance of Proteobacteria or its constituent Gammaproteobacteria (or the other major phyla, Firmicutes and Actinobacteria) in stool. Interestingly, FC was positively correlated with the genus Klebsiella (r = 0.207, p = 0.034), but not with other Gammaproteobacteria (Table 1). FC was also correlated with the Klebsiella ASV described above (r = 0.290, p = 0.003).
We used mixed-effects models to identify predictors of FC across the repeated measurements. The best-fitting, parsimonious model (Table 2) showed positive associations with vaginal birth (F = 83.29, p < 0.001), Hispanic ethnicity (F = 7.89, p = 0.006), and Klebsiella abundance (F = 4.54, p = 0.035). The association with the dominant ASV of Klebsiella was even stronger (F = 7.37, p = 0.008). We also performed linear regression to identify determinants of FC at different time-points of stool collection. At ≤2 weeks, the best-fitting model (r2 = 0.68, F = 35.76, p < 0.001) showed positive effects of maternal BMI (B = 6.08, t = 5.72, p < 0.001) and confirmed the association with vaginal birth (B = 157.62, t = 2.73, p = 0.01). During the 3rd week (r2 = 0.8, F = 40.77, p < 0.001), FC was associated with birth weight (B = 0.3, t = 7.29, p < 0.001) and Hispanic ethnicity (B = 256.19, t = 3.52, p = 0.001), but days of iron supplementation had a negative impact (B = −20.8, t = −3.39, p = 0.002). In the 4th week regression model (r2 = 0.61, F = 18.96, p < 0.001), the associations with birth weight (B = 0.2, t = 4.93, p < 0.001) and Hispanic ethnicity (B = 334.69, t = 2.08, p = 0.048) were still evident.
We also computed ROCs of Klebsiella abundance to identify a cut-off value that predicted high FC levels similar to those recorded in infants with mucosal inflammation (>280 µg/g stool) 12. Klebsiella abundance ≥83% predicted FC >280 µg/g with 72% sensitivity and 60% specificity (area under the curve, AUC = 0.646, p = 0.028; Fig. 2a). In the 3rd week, Klebsiella abundance ≥76% predicted elevated FC with 89% sensitivity and 57% specificity (AUC = 0.722, p = 0.047; Fig. 2b).
Fecal Klebsiella predict FC expression: a Relative abundance of Klebsiella ≥83% in stool predicted high FC (>280 µg/g of stool) with 72% sensitivity and 60% specificity (area under curve, AUC = 0.646); b during the 3rd postnatal week, Klebsiella abundance ≥76% predicted high FC with 89% sensitivity and 57% specificity (AUC = 0.722)
Predictors of the relative abundance of Klebsiella in stool
Similar to the observed associations of FC, Klebsiella abundance was also related in mixed-effects models to vaginal birth (F = 5.68, p = 0.015) and Hispanic ethnicity (F = 124.33, p < 0.001). The dominant ASV of Klebsiella was also affected by the same clinical antecedents, vaginal birth (F = 13.46, p < 0.001), and Hispanic ethnicity (F = 57.81, p < 0.001).
Clustering of infants based on Klebsiella abundance at ≤2 weeks
To investigate whether the variability (range 0–98%) in Klebsiella abundance we observed in the ≤2-week stool samples indicated the presence of more than one distinct subgroups of infants in our cohort, we used agglomerative hierarchical and K-means clustering procedures. These analyses revealed two subgroups with distinct cluster centers (13 vs. 94% in clusters 1 and 2, respectively; F = 370.83, p < 0.001; analysis of variance; Fig. 3). In cluster 1 (n = 23), the relative abundance of Klebsiella (and its dominant ASV) started at low levels and increased over time (Friedman test, p = 0.009 and 0.021 for Klebsiella and its dominant ASV, respectively). In contrast, Klebsiella dominated the intestinal microbiome in cluster 2 (n = 21). There was minimal loss of Klebsiella abundance over time (p = 0.018; Table 3), but the Klebsiella ASV remained stable. Gneiss (balance tree analysis)20 confirmed that these cluster differences in Klebsiella abundance were significant and not merely due to decreased abundance of other taxa (Fig. 4). In support of these data, the accumulative ratios of major bacterial families vs. Klebsiella (Fig. 5) decreased over time in cluster 1, consistent with the acquisition of Klebsiella. Cluster 2 started with and maintained low ratios, indicating persistently high levels of Klebsiella compared to other taxa.
Longitudinal change in fecal Klebsiella abundance. Scatter dot plots summarize fecal Klebsiella abundance over time. Open and solid circles indicate the two subgroups of infants identified in our cohort by K-means clustering analysis of fecal Klebsiella abundance at ≤2 weeks. Cluster 1 (23 infants, open circles) started with low Klebsiella abundance and gained these bacteria over time (Friedman test, p = 0.009). Cluster 2 (21 infants, solid circles) showed high Klebsiella abundance with minor attrition in weeks 3 and 4 (p = 0.018)
Temporal change in bacterial abundances at the family level relative to Klebsiella in the two clusters. Top: Boxplots summarize accumulative ratios of major bacterial families vs. Klebsiella (natural log-transformed, Ln) in the two patient clusters. Bottom: Bar diagrams summarize the distribution of major bacterial taxa at the family level in the numerator and the denominator
The two clusters were similar in birth weight and gestational age (Fig. 3). Cluster 1 experienced a shorter duration of maternal ruptured membranes, but had more days on antibiotics. There was no difference in major neonatal morbidities, days to full enteral feeds (150 mL/kg), days on positive pressure respiratory support, Z-scores for weight on postnatal day 28 and at 36 weeks’ post-menstrual age (based on Fenton growth charts), and length of hospital stay. A summary of the clinical characteristics of the two clusters in Table 4.
In mixed-effects models, Klebsiella abundance in cluster 1 increased with postnatal age (F = 5.0, p = 0.028) and antenatal steroids (F = 5.8, p = 0.019), whereas antenatal magnesium sulfate (F = 8.5, p = 0.005) and chorioamniotitis (F = 5.2, p = 0.026) had a negative effect. The association with antenatal steroids was also detectable in cluster 2 (F = 5.3, p = 0.025). In cluster 1, Klebsiella ASV also increased with postnatal age (F = 5.8, p = 0.018), and decreased with antenatal magnesium sulfate (F = 8.1, p = 0.006) and chorioamnionitis (F = 4.6, p = 0.035). In cluster 2, Klebsiella ASV was associated with vaginal delivery (F = 6.6, p = 0.013).
Cluster 1 had lower FC levels overall than cluster 2 (median (IQR) 148 (99–215) in cluster 1 vs. 226 (112–362)µg/g in cluster 2, respectively; p = 0.011). FC values were the highest in cluster 2 at ≤2 weeks (median (IQR) 243 (121–331)µg/g in cluster 2 vs. 148 (83–199) in cluster 1; p = 0.04). Antenatal magnesium sulfate had a negative effect on FC in cluster 1 (F = 15.0, p < 0.001), but a positive effect was seen in cluster 2 (F = 5.8, p = 0.02). Antenatal steroids had a negative effect on FC in cluster 2 (F = 6.0, p = 0.018).
Discussion
We present a detailed investigation of the relationship between fecal colonization with Gammaproteobacteria in VLBW infants and FC, a biomarker of gut mucosal inflammation. In our cohort, Gammaproteobacteria abundance did not affect FC expression. Instead, we found FC to be associated specifically with the presence of Klebsiella, and even more strongly, with a particular ASV within this genus. We observed two distinct paths to enteric colonization with Klebsiella: infants in cluster 1 began with very low abundance and gained modest levels of these bacteria over time, whereas the gut microbiome in cluster 2 was completely dominated by Klebsiella. High FC in cluster 2 infants indicated ongoing host–microbial interaction and a measureable innate immune response to these luminal bacteria. Importantly, Klebsiella abundance ≥83% predicted elevated FC levels similar to those seen during intestinal inflammation and NEC. To our knowledge, this is the first study to evaluate enteric dysbiosis in preterm infants in the context of the host inflammatory response.
The association of FC with fecal Klebsiella in our study raises several scientific questions. First, our findings call into question the practice of evaluating Gammaproteobacteria en bloc in the preterm microbiome. In recent years, several studies show that premature infants with a diagnosis of NEC had developed enteric dysbiosis with increased Gammaproteobacteria for several days to weeks antedating NEC onset.5,6,7,8 However, the lack of correlation between Gammaproteobacteria abundance and FC in our cohort suggests that Gammaproteobacteria may be too diverse a group to consistently exert a net inflammatory effect, and indicates a need for defining dysbiosis at higher levels of resolution. Second, we recorded highest FC levels in cluster 2 during the early neonatal period, when Klebsiella dominated in a setting of low α-diversity. These findings are important in efforts to develop a clinically relevant definition for dysbiosis; further study is needed to clarify whether the relative abundance of a pathobiont is relevant in isolation, or if it needs to be interpreted in conjunction with the diversity indices. Third, further study is needed to determine whether the early appearance of Klebsiella in some premature infants was unique to our center or if it represents a universal phenomenon in these patients. The inflammatory effects of Klebsiella in the intestine are plausible, considering the presence of potent virulence factors such as cell wall components and enterotoxins.23,24 Klebsiella are recognized intestinal pathogens of preterm and term neonates, having been identified in diarrhea, ecchymotic colitis, bacteremia during NEC and short-bowel syndrome, and even in NEC outbreaks.25,26,27,28,29 The correlation between fecal Klebsiella and elevated FC has been previously noted in infantile colic.30 Early colonization with Klebsiella has been noted in other preterm cohorts,6,8 but the possibility of finding distinct inflammation-driving pathobiont(s) at other centers cannot be excluded. In our own cohort, the correlation between FC and Klebsiella was relatively modest (r = 0.21), and when clustering was attempted based on FC, subgroup differences in Klebsiella did not reach significance. Finally, even though current evidence supports dysbiosis as an inflammatory stimulus, we need to acknowledge that a reciprocal effect, where pre-existing inflammation in the intestinal mucosa may promote a Gammaproteobacterial bloom, also warrants exploration.
Calprotectin is a 24 kDa dimer of the calcium-binding proteins calgranulin A/S100A8 and calgranulin B/S100A9, expressed in neutrophils and inflammatory monocytes.11,12,13,14 FC has found wide acceptance as a non-invasive marker of gut mucosal inflammation because it is strongly correlated with leukocyte infiltration in the mucosa, is stable in stool at room temperature for several days, and is easy to measure.31 Premature infants tend to have higher and more variable FC than adults, but higher cut-off values such as 280 µg/g stool have been correlated with intestinal inflammation and NEC.11,12,13,14 Treatment with non-steroidal anti-inflammatory drugs (NSAIDs) can increase FC,32 but in our cohort, the FC levels in the two infants who received indomethacin for treatment of patent ductus arteriosus were not higher than the rest.
Vaginal birth was an important determinant of the relative abundance of Klebsiella (and the dominant Klebsiella) in stool and of FC expression. These findings suggest that Klebsiella were likely acquired via vertical, mother-to-infant transmission. The near-total dominance of the gut microbiome in some infants (cluster 2) within the first 2 weeks after birth also lends credence to this possibility. However, the source of these bacteria is unclear. During pregnancy, the vaginal microbiome is dominated by Firmicutes.33,34 In women with vaginal dysbiosis, pathobionts such as Prevotella, Sneathia, Atopobium, Mycoplasma, and Gardnerella can be identified, but Klebsiella are infrequent.34 Perinatal exposure to maternal enteric flora during vaginal birth and to the microbiome of human milk, which contain Klebsiella,35,36 are two possible sources. Increased maternal BMI and diabetes have been previously associated with enrichment of Enterobacteriaceae, including Klebsiella, in both maternal and neonatal gut microbiome.37 Unfortunately, we are unable to investigate these findings further because we did not collect maternal samples in the present study.
We found higher Klebsiella abundance and FC in Hispanic infants. Although racial/ethnic differences in the enteric microbiome are possible,38 the type of feedings could have had a confounding influence: 8/9 (88.8%) Hispanic infants received only human milk vs. 17/36 (47.2%) infants of other ethnic groups (p = 0.03). The correlation between birth weight and FC likely reflects the maturational expansion of the mucosal leukocyte populations, and thus, the improving ability of the host to launch an innate immune response. Associations with antenatal steroids and magnesium sulfate may be more difficult to explain; steroids could influence the host–microbial cross-talk through altered leukocyte function and cytokine expression, and epigenetic changes in the mucosa.39 Perinatal exposure to magnesium sulfate can also alter gut motility and some immune responses,40 but the effects on fecal microbiome are unclear.
In conclusion, we show that FC expression in VLBW infants was specifically associated with the genus Klebsiella and a dominant ASV mapping to this genus, but not with the relative abundance of all Gammaproteobacteria in stool. These findings are important in the quest to develop a clinically relevant definition of enteric dysbiosis in premature infants. Major strengths of our study are repeated measurements of the gut microbiome and FC, and the single-patient room floor plan of our NICU, which now represents the layout in most of the newer NICUs in the United States. There are important limitations, such as the limited sample size and the single-center design. In our cohort, Klebsiella abundance affected FC but not the clinical outcome; we had only a single patient with NEC, which made it difficult to analyze the clinical effects of abnormal microbial colonization and mucosal inflammation. Further study is needed in a larger, multicenter cohort to validate our findings, particularly to confirm the dichotomous development of the gut microbiome and the importance of Klebsiella as a leading pathobiont in preterm infants.
References
Penders, J. et al. Factors influencing the composition of the intestinal microbiota in early infancy. Pediatrics 118, 511–521 (2006).
Turnbaugh, P. J. et al. A core gut microbiome in obese and lean twins. Nature 457, 480–484 (2009).
Sommer, F. & Backhed, F. The gut microbiota—masters of host development and physiology. Nat. Rev. Microbiol. 11, 227–238 (2013).
Stewart, C. J. et al. Longitudinal development of the gut microbiome and metabolome in preterm neonates with late onset sepsis and healthy controls. Microbiome 5, 75 (2017).
Wang, Y. et al. 16S rRNA gene-based analysis of fecal microbiota from preterm infants with and without necrotizing enterocolitis. ISME J. 3, 944–954 (2009).
Warner, B. B. et al. Gut bacteria dysbiosis and necrotising enterocolitis in very low birthweight infants: a prospective case–control study. Lancet 387, 1928–1936 (2016).
Pammi, M. et al. Intestinal dysbiosis in preterm infants preceding necrotizing enterocolitis: a systematic review and meta-analysis. Microbiome 5, 31 (2017).
Torrazza, R. M. et al. Intestinal microbial ecology and environmental factors affecting necrotizing enterocolitis. PLoS ONE 8, e83304 (2013).
Goyal, M. S., Venkatesh, S., Milbrandt, J., Gordon, J. I. & Raichle, M. E. Feeding the brain and nurturing the mind: linking nutrition and the gut microbiota to brain development. Proc. Natl Acad. Sci. USA 112, 14105–14112 (2015).
Smith, P. D. et al. Intestinal macrophages lack CD14 and CD89 and consequently are down-regulated for LPS- and IgA-mediated activities. J. Immunol. 167, 2651–2656 (2001).
MacQueen, B. C. et al. Elevated fecal calprotectin levels during necrotizing enterocolitis are associated with activated neutrophils extruding neutrophil extracellular traps. J. Perinatol. 36, 862–869 (2016).
Zhang, M., Zhang, X. & Zhang, J. Diagnostic value of fecal calprotectin in preterm infants with necrotizing enterocolitis. Clin. Lab. 62, 863–869 (2016).
Rouge, C. et al. Fecal calprotectin excretion in preterm infants during the neonatal period. PLoS ONE 5, e11083 (2010).
Albanna, E. A., Ahmed, H. S. & Awad, H. A. Stool calprotectin in necrotizing enterocolitis. J. Clin. Neonatol. 3, 16–19 (2014).
Moore, H. M., Kelly, A., McShane, L. M. & Vaught, J. Biospecimen Reporting for Improved Study Quality (BRISQ). Transfusion 53, e1 (2013).
Walters, W. et al. Improved bacterial 16S rRNA gene (V4 and V4–5) and fungal internal transcribed spacer marker gene primers for microbial community surveys. mSystems 1, e00009–15 (2016).
Torrazza, R. M., Li, N. & Neu, J. Decoding the enigma of necrotizing enterocolitis in premature infants. Pathophysiology 21, 21–27 (2014).
Fullerton, B. S. et al. Hospital transfers and patterns of mortality in very low birth weight neonates with surgical necrotizing enterocolitis. J. Pediatr. Surg. 51, 932–935 (2016).
Zhou, Y. et al. Longitudinal analysis of the premature infant intestinal microbiome prior to necrotizing enterocolitis: a case–control study. PLoS ONE 10, e0118632 (2015).
Morton, J. T. et al. Balance trees reveal microbial niche differentiation. mSystems 2, e00162–16 (2017).
Ho, T. B. T. et al. Dichotomous development of the gutmicrobiome in preterm infants. Microbiome in review 6, 157 (2018).
Ho, T. T. B. et al. Dichotomous development of the gut microbiome in preterm infants. Microbiome 6, 157 (2018).
Lu, M. C. et al. Colibactin contributes to the hypervirulence of pks(+) K1 CC23 Klebsiella pneumoniae in mouse meningitis infections. Front. Cell. Infect. Microbiol. 7, 103 (2017).
Straus, D. C., Lonon, M. K., Woods, D. E. & Garner, C. W. Production of an extracellular toxic complex by various strains of Pseudomonas cepacia. J. Med. Microbiol. 30, 17–22 (1989).
Gregersen, N. et al. Klebsiella pneumoniae with extended spectrum beta-lactamase activity associated with a necrotizing enterocolitis outbreak. Pediatr. Infect. Dis. J. 18, 963–967 (1999).
Hill, H. R., Hunt, C. E. & Matsen, J. M. Nosocomial colonization with Klebsiella, type 26, in a neonatal intensive-care unit associated with an outbreak of sepsis, meningitis, and necrotizing enterocolitis. J. Pediatr. 85, 415–419 (1974).
Boccia, D., Stolfi, I., Lana, S. & Moro, M. L. Nosocomial necrotising enterocolitis outbreaks: epidemiology and control measures. Eur. J. Pediatr. 160, 385–391 (2001).
Stone, H. H., Kolb, L. D. & Geheber, C. E. Bacteriologic considerations in perforated necrotizing enterocolitis. South. Med. J. 72, 1540–1544 (1979).
Canioni, D. et al. Histopathology and microbiology of isolated rectal bleeding in neonates: the so-called “ecchymotic colitis”. Histopathology 30, 472–477 (1997).
Rhoads, J. M. et al. Altered fecal microflora and increased fecal calprotectin in infants with colic. J. Pediatr. 155, 823–828 e1 (2009).
Roseth, A. G., Schmidt, P. N. & Fagerhol, M. K. Correlation between faecal excretion of indium-111-labelled granulocytes and calprotectin, a granulocyte marker protein, in patients with inflammatory bowel disease. Scand. J. Gastroenterol. 34, 50–54 (1999).
Gisbert, J. P. & McNicholl, A. G. Questions and answers on the role of faecal calprotectin as a biological marker in inflammatory bowel disease. Dig. Liver Dis. 41, 56–66 (2009).
Stout, M. J. et al. Early pregnancy vaginal microbiome trends and preterm birth. Am. J. Obstet Gynecol 217, 356.e1–356.e18 (2017).
Kindinger, L. M. et al. The interaction between vaginal microbiota, cervical length, and vaginal progesterone treatment for preterm birth risk. Microbiome 5, 6 (2017).
Urbaniak, C., Angelini, M., Gloor, G. B. & Reid, G. Human milk microbiota profiles in relation to birthing method, gestation and infant gender. Microbiome 4, 1 (2016).
Patel, S. H. et al. Culture independent assessment of human milk microbial community in lactational mastitis. Sci. Rep. 7, 7804 (2017).
Verdam, F. J. et al. Human intestinal microbiota composition is associated with local and systemic inflammation inobesity. Obesity (Silver Spring). 21, E607–E615 (2013).
Gupta, V. K., Paul, S. & Dutta, C. Geography, ethnicity or subsistence-specific variations in human microbiome composition and diversity. Front. Microbiol. 8, 1162 (2017).
Cortese, R., Lu, L., Yu, Y., Ruden, D. & Claud, E. C. Epigenome-microbiome crosstalk: a potential new paradigm influencing neonatal susceptibility to disease. Epigenetics 11, 205–215 (2016).
Ghidini, A., Espada, R. A. & Spong, C. Y. Does exposure to magnesium sulfate in utero decrease the risk of necrotizing enterocolitis in premature infants? Acta Obstet. Gynecol. Scand. 80, 126–129 (2001).
Acknowledgments
This research was funded by National Institutes of Health awards NR015446 (M.W.G.), HL124078 (A.M.), and HL133022 (A.M.), and T32GM007281 (A.L.Y.). We thank the research nurses, Judy Zaritt and Marcia Kneusel, for identification of eligible infants, and collection of clinical information and stool samples. We are also indebted to the nursing staff at the NICU at TGH for their constant support.
Author contributions
T.T.B.H. collected and analyzed the data and wrote the manuscript. M.W.G. supervised laboratory process and advised on content of the manuscript. B.K. performed laboratory analysis and advised on laboratory techniques. A.L.Y. analyzed 16S rRNA data. B.A.T. advised on the content of the manuscript. J.A.G. supervised the analysis of 16S rRNA data and advised on the manuscript content. A.M. supervised the data analysis and wrote the manuscript. All authors edited the manuscript and approved the final draft.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ho, T.T.B., Groer, M.W., Kane, B. et al. Enteric dysbiosis and fecal calprotectin expression in premature infants. Pediatr Res 85, 361–368 (2019). https://doi.org/10.1038/s41390-018-0254-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41390-018-0254-y
This article is cited by
-
Supplemental N-acyl homoserine lactonase alleviates intestinal disruption and improves gut microbiota in broilers challenged by Salmonella Typhimurium
Journal of Animal Science and Biotechnology (2023)
-
Incomplete resection of necrotic bowel may increase mortality in infants with necrotizing enterocolitis
Pediatric Research (2021)
-
Role of platelets in neonatal necrotizing enterocolitis
Pediatric Research (2021)
-
The development of intestinal dysbiosis in anemic preterm infants
Journal of Perinatology (2020)
-
Colonization by B. infantis EVC001 modulates enteric inflammation in exclusively breastfed infants
Pediatric Research (2019)