Abstract
Objective
The latest genome-wide association studies of obesity-related traits have identified several genetic loci contributing to body composition (BC). These findings have not been robustly replicated in African populations, therefore, this study aimed to assess whether European BC-associated gene loci played a similar role in a South African black population.
Methods
A replication and fine-mapping study was performed in participants from the Birth to Twenty cohort (N = 1,926) using the Metabochip. Measurements included body mass index (BMI), waist and hip circumference, waist-to-hip ratio (WHR), total fat mass, total lean mass and percentage fat mass (PFM).
Results
SNPs in several gene loci, including SEC16B (Padj < 9.48 × 10−7), NEGR1 (Padj < 1.64 × 10−6), FTO (Padj < 2.91 × 10−5), TMEM18 (Padj < 2.27 × 10−5), and WARS2 (Padj < 3.25 × 10−5) were similarly associated (albeit not at array-wide signficance (P ≤ 6.7 × 10−7) with various phenotypes including fat mass, PFM, WHR linked to BC in this African cohort, however the associations were driven by different sentinel SNPs. More importantly, DXA-derived BC measures revealed stronger genetic associations than simple anthropometric measures. Association signals generated in this study were shared by European and African populations, as well as unique to this African cohort. Moreover, sophisticated estimates like DXA measures enabled an enhanced characterisation of genetic associations for BC traits.
Conclusion
Results from this study suggest that in-depth genomic studies in larger African cohorts may reveal novel SNPs for body composition and adiposity, which will provide greater insight into the aetiology of obesity.
Similar content being viewed by others
Introduction
It is well established that obesity, a partly heritable trait, is a key risk factor for many non-communicable diseases (NCDs), and that its global rise is leading to increases in morbidity and mortality1,2. The study of the genetic contribution to body composition traits have predominantly focused on body-mass index (BMI)3, and measures of overall adiposity, such as waist circumference (WC) and waist-to-hip ratio (WHR). BMI is a readily measurable proxy for body fat on a population-level, whereas WC and WHR as measures of abdominal obesity are both proxy indicators of visceral adipose tissue (VAT). VAT has been strongly correlated with cardiovascular disease and related pathologies, and therefore WC and WHR are good predictors of health risk, metabolic syndrome or cardiometabolic diseases4. Although BMI, WC and WHR are easily collected in large study cohorts and thus allow statistically well-powered meta-analyses, they represent heterogeneous phenotypes, and are not the best indicators of body adiposity5. In contrast, dual energy X-ray absorptiometry (DXA) is the preferred method of determining body composition by accurately quantifying fat-, fat-free-, and bone mass. This method allows for the resolution of total adipose tissue and soft tissue, and bone mineral content6, but is a costly measure to implement in large cohort studies.
Recent genome-wide association studies (GWAS) and meta-analyses have identified hundreds of genetic risk loci for obesity and body composition measures. For the most part, GWAS have been carried out in European or Asian study cohorts, with a paucity of research in African populations7. Studying complex trait genetics in African cohorts remain enticing, given the vast diversity in African genomes8 and the increased ability to pinpoint causal signals due to generally lower linkage disequilibrium (LD)9. Fine-mapping (i.e. genotyping additional SNPs in target regions, that were not included in the original genotyping platform) across populations of differing LD backgrounds is another powerful tool in gaining insight into the causal variants for polygenic obesity10,11. The Metabochip12, a genotyping array representing genomic loci associated with several anthropometric, cardiometabolic and atherosclerotic traits has successfully been used in several such fine-mapping experiments13,14. The aim of the present study was to use the Metabochip to identify genetic loci associated with common anthropometric measures of body size and body fat distribution, in a South African cohort. In addition, these genotypes were correlated to DXA-derived measures of body composition and adiposity.
Materials and methods
Ethics statement
The Human Research Ethics committee (Medical) of the University of the Witwatersrand endorsed clearance for data and DNA sample collection from the Birth to Twenty (Bt20) cohort under certificate number M010556. In addition, the use of DNA and data for the purpose of this study were allowed under certificate number M120647. All participants provided written informed consent for the collection of data and samples and subsequent analysis.
Study participants
This study utilised data and DNA samples collected from the longitudinal Bt20 cohort of Soweto, South Africa, described in detail elsewhere15 and in supplementary data (Body Composition in Africans_supplementary data). For this study we used phenotype data collected from cohort participants during the cohort year-17 collection (N = 1,240) and from their female caregivers during the year-13 collection (N = 1,033). This dataset included 972 caregiver–participant pairs, with 60 unrelated caregivers and 267 unrelated participants (described in Table 1).
Body measurements
Body weight, body height, age, WC, hip circumference (HC), sub-total fat mass (grams) and sub-total fat-free mass (grams) (excluding bone mineral content) were measured and recorded for all study participants and described in the supplementary data. Subsequently, BMI, WHR and PFM (percentage fat mass) were calculated from these measures. Whole body composition measures were obtained using dual energy X-ray absorptiometry (DXA) (Hologic, Malborough, MA, USA) as per the guidelines recommended by the International Society of Clinical Densitometry16. Sub-total body fat and fat-free (lean) mass (in grams) excluding the head was used given the high percentage of hair weaves used by female study participants. The PFM was calculated as fat mass (in grams) divided by total body mass (in grams).
Genotyping
Genotyping was performed using the Illumina Metabochip (Illumina, San Diego, California, USA) at the DNA Technologies Core of the University of California, Davis (California, USA). Genotypes were called using GenomeStudio vs.2011.1 (Illumina, San Diego, California, USA) based on a modified clustering manifest trained on the genotyping data.
Statistical analysis
Quality control
Genotype quality control (QC) was assessed according to standard published methods17 and is described in detail in the supplementary data. Quantile–quantile (QQ) plots were drawn in R vs.3.2.2 using the package qqman to visualise the distribution of the test-statistic for each of the phenotypes18 for post-analysis QC assessment. Furthermore, population structure was assessed and principle component analysis (PCA) was used to identify outliers and to assess genomic inflation as a result of population stratification (smartpca in EIGENSTRAT-vs.3.0; HelixSystems, USA). The Genesis software tool was used for PCA visualisation (http://www.bioinf.wits.ac.za/software/genesis/). Merging of the datasets in PLINK resulted in 1,926 individuals and 125,878 SNPs remaining for analysis.
Manual inspection of the intensity plots for all SNPs showing associations were performed using Evoker19. Every SNP was inspected in the dataset and the SNPs that passed both sets of evaluations described above were included (N = 125,878 SNPs remaining in the full sample set).
The power to detect associations was assessed using the software package Quanto (http://biostats.usc.edu/Quanto.html; Supplementary Tables S1-S7) and factored in multiple hypothesis testing using the array-wide significance level outlined below as alpha. In this study the Bonferroni correction was applied to adjust for multiple testing. The Bonferroni genome-wide (GW) significance level for Metabochip data was calculated by using only unlinked loci−0.05/number of independent markers: (0.05/74475) on the Metabochip, resulting in a P ≤ 6.7 × 10−7 cut-off (referred to as the array-wide significance level). The number of independent markers was calculated by performing linkage disequilibrium (LD)-based SNP pruning where a window of 50 SNPs was considered at a time, LD between each pair of SNPs in the window was calculated and one of a pair of SNPs was removed if the LD was greater than 0.5. To address the possible introduction of Type II errors through the application of this rigorous correction, we chose to present a second category of results where a cut-off of P ≤ 1 × 10−4 was met.
Association analysis
All statistical analyses were performed using either GCTA vs.1.2420 or PLINK v1.921. A mixed linear model association (MLMA) method incorporating a relatedness matrix (calculated by GCTA using the given genotypes) was employed to compensate for relatedness within the merged dataset, and age, sex and height were included as covariates where appropriate (reported as Padj in Table 2). In the analysis for BMI (where height is already compensated for in the derived measure) and WHR, only age and sex were used as covariates. We did not adjust for possible confounding from other body composition variables because of the problems of co-linearity and over-adjustment that may have arisen.
To exploit the disparate age and sex dynamic in this dataset, we also performed sex- (male vs. female) and age- (adolescents vs. adult) stratified analyses using linear regression under an additive model (results presented in the supplementary data). All analyses were adjusted for applicable covariates and were also reported as Padj. To ensure that population structure was controlled for, the genomic control method (GC) was flagged during the association analysis using PLINK v1.9 where the calculated genomic control GC inflation factor λ suggested no evidence of detectable population structure and/or genotyping error.
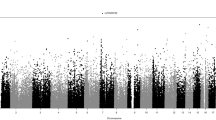
Post-analysis association results were visualised as Manhattan plots, drawn in R vs.3.2.2 using the package qqman18 and LocusZoom (regional) plots, drawn using LocusZoom vs.1.1.22.
Results
Characteristics of the study participants
Of the 2,273 participants enroled for this study, N = 1,926 (85%) passed genotyping quality control evaluation, and were included in further statistical analyses. Of these, 954 were adolescents (median age of 17.9 years, N = 505 males and N = 449 females) and 972 were adult female caregivers (median age 42.0 years). Detailed summary statistics relevant to the body size and composition measures of the cohort is presented in Table 1. Details of all quality control results are shown in Supplementary data (Figures S1-S4).
To further investigate population structure and the distinctions between different African populations, an intracontinental plot of available African datasets was generated. With respect to principal components 1 and 2, it is revealed that the majority of the participants from this study clustered together tightly with other Bt20 participants previously genotyped23, as well as with other south eastern Bantu-speakers (Fig. 1). The Bt20 cohort forms a distinct cluster away from other East- and West African groups.
Genetic variation associated with body size and composition
Table 2 shows the sentinel SNPs found to be associated with all traits tested, with genome-wide analysis visualised in Fig. 2 (body composition phenotypes i.e. fat mass, lean mass and PFM) and Fig. 3 (BMI and measures of body fat distribution). Variants with suggestive associations (approaching array-wide significance P ≤ 5 × 10−6) was observed between a locus upstream of BRINP2|SEC16B (lead SNP rs6664268) and both fat mass and percentage fat mass. Exploring other associations suggestive of significance reveals several interesting findings, including SNPs in SP110 associated with both lean mass and WC, and WARS2, associated with HC and WHR. The only association with FTO observed in the cohort was with an intronic SNP (intron 2- rs1861554) and WHR.
Regional plots for BRINP2|SEC16B (Fig. 4) were drawn to gain further insight into the underlying genomic complexity of the regions found to be associated with various traits. As observed in Fig. 4(a), the variants with suggestive associations have a lower LD with the lead SNP against an African LD background. In Fig. 4(b) the relationship of SNPs drawn against a European LD background, show that the cluster of associated SNPs are indistinguishable from one another, due to strong LD with the lead SNP. Figure 4(c) illustrates an intermediate effect of associated SNPs against an Asian LD background.
The strength of the LD with lead SNP (purple diamond) is indicated by r2 values, with each dot colour indicating an r2 value according to the key on the left-hand side of the LZ plot. A-The presence of variants that have a weaker correlation with the lead SNP is indicated by the blue dot (r2 = 0.4) and the yellow dot (r2 = 0.8) against an African LD background. B- The relationship of SNPs drawn against a European LD background, show that the cluster of associated SNPs are indistinguishable from one another, as reflected by their strong LD (red coloured dots) with the index SNP. C- illustrates an intermediate effect of correlated SNPs against an Asian LD background. The recombination hotspots are illustrated in blue peaks, with neighbouring genes shown beneath the plot
Sex- and age-specific correlations linked to body size and composition
Due to the unique composition of the cohort genotyped for this study, we were able to systematically search for genetic loci that may influence body composition in an age- or sex-specific manner. As such, 7 loci with sex-specific effects (supplementary Table S8) and 2 loci with age-specific effects (supplementary Table S9) reached either suggestive or array-wide significance. Highly significant associations were observed in the male subset for TRPM7, SLC17A1 and COBBL1 (across different measures), regardless of the smaller sample size. These cross-phenotype, sex- and age-specific associations are summarised in Table S10 in supplementary data.
Discussion
The Metabochip has proved to be a useful tool in the discovery and replication of variants contributing to obesity-related traits10,13,14, but its use in sub-Saharan African (SSA) populations had yet to be tested. This current study follows on earlier replication studies, using candidate gene approaches, where genetic polymorphisms previously linked with BMI in non-African populations, were investigated in the Bt20 cohort24,25 as well as another study conducted in a Nigerian cohort26. The Metabochip has previously been used to densely genotype and evaluate 21 BMI loci identified in European GWAS in ~29,000 African Americans from the Population Architecture using Genomics and Epidemiology (PAGE) study10. They showed that eight of the 21 loci were associated with BMI (P = 5.8 × 10−5) and that for most of the loci, fewer variants were in LD (r2 > 0.5) with the most significant SNP in African American populations than European populations. Further, they also reported two new variants associated with BMI, BRE and DHX34 as well as a putative independent signal near GNPDA210. A GWAS of anthropometric traits including African American populations showed that 32 of the loci associated with BMI were directionally consistent with European populations albeit not at GW significance27. A similar Asian GWAS (cited in ref. 3 also confirmed the lack of reproducibility of GW significant signals in non-European populations. To date there has been one GWAS conducted in an African (Nigerian) cohort on anthropometric traits28. The current study is unique in that it investigates genetic associations of seven phenotypes related to body-size and composition in an African cohort, including three body composition traits derived from DXA measurements. Further to this, the ability to compare genetic associations across sex and ages (albeit with reduced power) is also a unique feature of this study.
Our study has replicated known body composition loci including SEC16B, FTO and NEGR1 and resulted in the discovery of new signals that may associate with an increased risk for obesity-related traits. All of the replicated loci showed stronger associations with neighbouring SNPs, than the previously reported index SNPs. This could be attributable to ascertainment bias given that most of the SNPs on the Metabochip were chosen from Eurocentric-based GWASs. Ten loci were found to be associated with more than one trait. The most recent GIANT meta-analysis13 together with a GWAS meta-analysis of percentage body fat29 highlighted that BMI-associated loci had significant across-phenotype effects on other metabolic phenotypes.
The most substantial association signal from this study was with fat mass and percentage fat mass at an intergenic region upstream of BRINP2|SEC16B. The lead SNP maps to the same LD block where variants (SNPs rs543874 or rs10913469) were observed to associate with BMI in several continental populations, including Europeans3,30,31, Asians (cited in ref. 13 and African Americans10 and in both adults and children30,32,33. More recently a meta-analysis reported across-phenotype associations between SEC16B variant rs543874 and increases in percentage body fat29. To our knowledge, SEC16B variants have not previously been examined in any African population in relation to body composition or obesity. The results from regional genomic plots suggest the possibility of multiple independent association signals with lead variants upstream of BRINP2|SEC16B. This is demonstrated by the presence of associated (albeit not at GW-significance) signals that are in low LD with the index SNP when viewed against and African LD background22. In contrast, these SEC16B variants are in stronger LD with one another against a European and Asian background, suggesting that it would be harder to tease out potential causal variants in these populations. These results demonstrate the value of using African genomic data in dissecting possible independent association signals and thus narrowing in on potential causal loci.
The lead variant in the BRINP2|SEC16B locus, rs6664269, is in an intergenic region with no current evidence for a functional impact on the Sec16 protein. However, SEC16B is an interesting biological candidate gene for obesity related traits as it encodes the long Sec16L and the short Sec16 proteins, which are required for the vesicular transport of secretory molecules from the endoplasmic reticulum (ER) to the Golgi apparatus34,35. Hotta and colleagues (2009) have postulated that the Sec16 protein, which is expressed in many tissues including the brain, plays a role in the transport of appetite-regulatory peptides such as neuropeptide Y and pro-opiomelanocortin35,36. However, a study comparing obesity-related genes in Zucker diabetic fatty rats to those of its lean normoglycaemic counterpart showed that SEC16B was one of the only obesity-risk variants (of those tested) that was not expressed in the hypothalamus, but rather in subcutaneous adipose tissue, implying a more peripheral role in the regulation of obesity37.
Other array-wide significant associations were observed between variants in for TRPM7 (waist and hip circumference), SLC17A1 (waist-to-hip-ratio) and COBBL1 (waist-to-hip ratio) albeit only in males (N = 505; assessed at age 18 years). A region intergenic to COBBL1 (COBBL1-GRB14) has recently been implicated in a GWAS as a novel locus that results in an increase in body fat percentage29. It has also been noted that variants in or near COBBL1-GRB14 have previously been associated with T2D risk, fasting insulin, triglycerides, HDL-cholesterol29, indicating cross phenotype associations. The variants in/near TRPM7 and SLC17A1 have been associated with WHR and BMI, respectively, albeit not as GW significance3,38. No association with any anthropometric variables were associated with TRPM7 in the merged dataset. This locus was also associated with BMI in the males, but the association did not reach array-wide significance. The association of these variants with WC and HC needs to be replicated in larger mixed sex cohorts to confirm that they are indeed showing a sex-specific effect on body fat distribution in males only. Fat distribution is strongly associated with sex and ethnicity. For instance, African women have been shown to have lower levels of VAT but higher subcutaneous fat mass than BMI-matched European women39 and it has also been suggested that the current anthropometric cut-points used to define obesity may not be suitable for African populations40,41.
There is certainly significant correlations of our findings with body composition and other cardiometabolic-related trait associations shown in European, Asian and African-American cohorts as eluded to earlier in the discussion. This was confirmed by a “look-up” of our top associated SNPs in the NHLBI GRASP catalogue, v2.0.0.042 and PhenoScanner43 databases, respectively. Confirmation of our findings were observed for several of the top-associated SNPS, albeit not at GW-significance. However we were able to confirm associations for variants (SNPs rs543874 or rs10913469) upstream of BRINP2|SEC16B which map to the same LD block as the lead SNP found in this study (rs6664268), thus illustrating evidence of replication of signals.
Several potentially functional intronic non-coding variants have been revealed from GWAS. Clarifying how these variants contribute to biological mechanisms resulting in disease remains a challenge. Recent endeavours such as ENCODE (Encyclopaedia of DNA elements) have contributed to a better understanding of the functional elements in the non-coding genome44. For instance, investigations of the well-known obesity gene, FTO, have demonstrated that polymorphisms in intronic regions can have long reaching effects on genes. Studies have shown that FTO variants influences gene expression regulation in both IRX3 and IRX5, several megabases away. Intronic variants have also been shown to contain regulators of alternative splicing and other regulatory elements entrenched within these regions45.
Our results suggest that GWAS-identified variants of body composition are tagged by different lead SNPs in an African cohort. This is in line with the expectation of observing some differences when replicating European tag SNPs in an African population. According to Lu and Loos46 the replication of loci rather than specific SNPs offers a more detailed analysis and takes into account differences in genetic LD backgrounds between populations of varying ancestries. In these studies, signals were shown to be localised to smaller haplotype blocks than when originally reported.
The lack of replication of previously reported associations with BMI in our study may be due to smaller LD blocks present in the African data, thereby decreasing the tagging efficiency of the array. These “dilution of effects”46,47,48 have been observed in other trans-ethnic GWAS10,47,49 investigations, specifically African American study cohorts47. Furthermore, varying allele frequencies of variants between European and African populations may have contributed to lower statistical power to detect associations in this study and it is possible that some variants may have been excluded during QC due to very low MAFs. The MalariaGEN consortium has stated that the lack of replication of GWAS signals in African populations questions the validity of previously reported associations, stating that real associations may fail to replicate due to overestimation of effect size (‘winner’s curse’), variation in frequency of effect allele between populations, variations in LD between the index SNP and causative SNP and the overall complexity of the disease (allelic heterogeneity or epistasis)48. It has been postulated that besides the difference in sample sizes influencing the ability to detect smaller effects, differences in environment, especially diet and physical activity, may attenuate the relationship between causative SNPs and obesity47. This may be plausible for differences in signals observed between African American and African populations, where although they share related ancestries, the environment (e.g. diet and physical activity) is very different47. However it is also important to bear in mind that African-American populations are admixed and therefore subject to differences in their genetic architecture compared to indigenous African populations9.
In this study we concentrated our efforts on replicating reported GWAS adiposity signals rather than the discovery of new loci. Given our small sample size (N = 1926) and the small to moderate effect sizes, we acknowledge that the study might not have been sufficiently powered to detect the very weak SNP effects on BMI and related phenotypes that have been reported in much larger studies3,13,29. Large meta-analyses are needed to detect the small effect sizes from surrogate measures of adiposity such as BMI. The latest GIANT consortium meta-analyses have combined sample sizes of 339,224 individuals in much larger studies3. A further limitation of this study is the inclusion of mother–child pairs and the possible issues of relatedness reducing the power to detect associations, even though it was adjusted for in the association analysis. Further, the adolescents in the study were a mix of both males and females, whilst the adults were females only. We did adjust for the necessary covariates in the analyses, however this disparity may have affected the ability to uncover further age- and sex-specific associations.
In this study we have shown that DXA-derived indicators of adiposity produced stronger SNP association signals (see Table 2, and supplementary Tables S8 and S9), with the exception of male-specific associations with measures of fat distribution. Most GWAS for obesity-risk variants have focussed on BMI as a measure of obesity; however BMI may not be the best measure of adiposity, as it cannot discriminate between fat mass and fat-free mass50. One of the strengths of the current study is that DXA was used to estimate body composition and this is known to be a better indicator of obesity50,51. It is well known that BMI (determined from twin and family studies) exhibits high heritability estimates ranging from 40–70% in European populations1 but the heritability of other body composition phenotypes are less well described. A study of 554 participants (492 European and 48 African-American sibling pairs) that assessed the heritability of body composition measures by DXA showed that fat mass, fat-free mass and PFM (0.71, 0.60 and 0.64, respectively) are heritable traits52. This suggests that these phenotypes have a strong genetic component and are well suited for genetic association studies.
In summary, 11 loci associated with body size and composition were observed in this study. These associations comprised both array-wide (P ≤ 6.7 × 10−7) and suggestive associations approaching array-wide significance (P ≤ 5 × 10−6) and included the merged as well as the sex- and age-stratified analyses. Most of the associated SNPs/loci reported in this study have not been previously associated with body composition measures elsewhere. Data from this study strongly motivates that more accurate measures of body composition, such as those generated by DXA, produce stronger SNP association signals than do composite variables like BMI. Age- and sex-specific genetic associations with anthropometric measures were also noted in the current study, however they need to be investigated further. Initiatives such as the Human, Health, Heredity (H3) Africa AWI-Gen collaborative study aims to address the disparity that exists in African genomic studies of factors that influence body composition, body fat distribution and cardiometabolic disease risk53. However, this current study offers a significant contribution to our current understanding of the role of genetic factors to body composition in an African population.
References
Bodurtha, J. N. et al. Genetic analysis of anthropometric measures in 11-year-old twins: the Medical College of Virginia Twin Study. Pediatr. Res. 28, 1–4 (1990).
Ng M. et al. Global, regional, and national prevalence of overweight and obesity in children and adults during 1980–2013: a systematic analysis for the Global Burden of Disease Study 2013. The Lancet. 384, 766–781 (2014).
Speliotes, E. K. et al. Association analyses of 249,796 individuals reveal 18 new loci associated with body mass index. Nat. Genet. 42, 937–48 (2010).
Müller, M., Bosy‐Westphal, A. & Krawczak, M. Genetic studies of common types of obesity: a critique of the current use of phenotypes. Obes. Rev. 11, 612–8 (2010).
Wells, J. C. Commentary: the paradox of body mass index in obesity assessment: not a good index of adiposity, but not a bad index of cardio-metabolic risk. Int. J. Epidemiol. 43, 672–4 (2014).
Duren, D. L. et al. Body composition methods: comparisons and interpretation. J. Diabetes Sci. Technol. 2, 1139–46 (2008).
Rotimi, C. et al. Research capacity. Enabling the genomic revolution in Africa. Science 344, 1346–8 (2014).
Gurdasani, D. et al. The African genome variation project shapes medical genetics in Africa. Nature 517, 327–32 (2015).
Teo, Y. Y., Small, K. S. & Kwiatkowski, D. P. Methodological challenges of genome-wide association analysis in Africa. Nat. Rev. Genet. 11, 149–60 (2010).
Gong, J. et al. Fine mapping and identification of BMI loci in African Americans. Am. J. Hum. Genet. 93, 661–71 (2013).
Liu C.-T. et al. Multi-ethnic fine-mapping of 14 central adiposity loci. Hum. Mol. Genet. 23, 4738–4744 (2014).
Voight, B. F. et al. The metabochip, a custom genotyping array for genetic studies of metabolic, cardiovascular, and anthropometric traits. PLoS. Genet. 8, e1002793 (2012).
Locke, A. E. et al. Genetic studies of body mass index yield new insights for obesity biology. Nature 518, 197–206 (2015).
Winkler, T. W. et al. The influence of age and sex on genetic associations with adult body size and shape: a large-scale genome-wide interaction study. PLoS. Genet. 11, e1005378 (2015).
Richter, L., Norris, S., Pettifor, J., Yach, D. & Cameron, N. Cohort profile: Mandela’s children: the 1990 birth to twenty study in South Africa. Int. J. Epidemiol. 36, 504–11 (2007).
Gordon, C. M. et al. Dual energy X-ray absorptiometry interpretation and reporting in children and adolescents: the 2007 ISCD pediatric official positions. J. Clin. Densitom. 11, 43–58 (2008).
Anderson, C. A. et al. Data quality control in genetic case-control association studies. Nat. Protoc. 5, 1564–73 (2010).
Team RC. R: a language and environment for statistical computing. R Foundation for Statistical Computing, Vienna, Austria. 2013.
Morris, J. A., Randall, J. C., Maller, J. B. & Barrett, J. C. Evoker: a visualization tool for genotype intensity data. Bioinformatics 26, 1786–7 (2010).
Yang, J., Lee, S. H., Goddard, M. E. & Visscher, P. M. GCTA: a tool for genome-wide complex trait analysis. Am. J. Hum. Genet. 88, 76–82 (2011).
Purcell S. et al. PLINK: a toolset for whole-genome association and population-based linkage analysis. Am. J. Hum. Genet. 81 (3), 559–575, 2007.
Pruim, R. J. et al. LocusZoom: regional visualization of genome-wide association scan results. Bioinformatics 26, 2336–7 (2010).
May, A. et al. Genetic diversity in black South Africans from Soweto. BMC Genom. 14, 644 (2013).
Lombard Z. et al. Appetite regulation genes are associated with body mass index in black South African adolescents: a genetic association study. BMJ Open. 2, e000873, 1–10 (2012).
Pillay, V. et al. Exploring genetic markers of adult obesity risk in black adolescent South Africans—the birth to twenty cohort. Nutr. Diabetes 5, e157 (2015).
Adeyemo, A. et al. FTO genetic variation and association with obesity in West Africans and African Americans. Diabetes 59, 1549–54 (2010).
Monda, K. L. et al. A meta-analysis identifies new loci associated with body mass index in individuals of African ancestry. Nat. Genet. 45, 690–6 (2013).
Kang, S. J. et al. Genome-wide association of anthropometric traits in African- and African-derived populations. Hum. Mol. Genet. 19, 2725–38 (2010).
Lu, Y. et al. New loci for body fat percentage reveal link between adiposity and cardiometabolic disease risk. Nat. Commun. 7, 10495 (2016).
Bradfield, J. P. et al. A genome-wide association meta-analysis identifies new childhood obesity loci. Nat. Genet. 44, 526–31 (2012).
Thorleifsson, G. et al. Genome-wide association yields new sequence variants at seven loci that associate with measures of obesity. Nat. Genet. 41, 18–24 (2009).
Wang, H.-J. et al. Association of common variants identified by recent genome-wide association studies with obesity in Chinese children: a case-control study. BMC Med. Genet. 17, 7 (2016).
Zhao, J. et al. The role of obesity‐associated loci identified in genome‐wide association studies in the determination of pediatric BMI. Obesity 17, 2254–7 (2009).
Budnik A., Heesom K. J., Stephens D. J. Characterization of human Sec16B: indications of specialized, non-redundant functions. Scientific Reports. 1, 77, 1–10 (2011).
Hotta, K. et al. Association between obesity and polymorphisms in SEC16B, TMEM18, GNPDA2, BDNF, FAIM2 and MC4R in a Japanese population. J. Hum. Genet. 54, 727–31 (2009).
Bhattacharyya, D. & Glick, B. S. Two mammalian Sec16 homologues have nonredundant functions in endoplasmic reticulum (ER) export and transitional ER organization. Mol. Biol. Cell 18, 839–49 (2007).
Schmid, P. M. et al. Expression of fourteen novel obesity-related genes in zucker diabetic fatty rats. Cardiovasc. Diabetol. 11, 48 (2012).
Heid, I. M. et al. Meta-analysis identifies 13 new loci associated with waist-hip ratio and reveals sexual dimorphism in the genetic basis of fat distribution. Nat. Genet. 42, 949–60 (2010).
Crowther, N. J. & Ferris, W. F. The impact of insulin resistance, gender, genes, glucocorticoids and ethnicity on body fat distribution. J. Endocrinol. Metab. Diabetes 15, 115–20 (2010).
Crowther, N. J. & Norris, S. A. The current waist circumference cut point used for the diagnosis of metabolic syndrome in sub-Saharan African women is not appropriate. PLoS ONE 7, e48883 (2012).
Murphy, G. A. et al. The use of anthropometric measures for cardiometabolic risk identification in a rural African population. Diabetes Care 37, e64–5 (2014).
Leslie, R., O’Donnell, C. J. & Johnson, A. D. GRASP: analysis of genotype–phenotype results from 1390 genome-wide association studies and corresponding open access database. Bioinformatics 30, i185–i94 (2014).
Staley, J. R. et al. PhenoScanner: a database of human genotype–phenotype associations. Bioinformatics 32, 3207–9 (2016).
Consortium EP. An integrated encyclopedia of DNA elements in the human genome. Nature 489, 57–74 (2012).
Cooper, D. N. Functional intronic polymorphisms: buried treasure awaiting discovery within our genes. Hum. Genom. 4, 1 (2010).
Lu, Y. & Loos, R. J. Obesity genomics: assessing the transferability of susceptibility loci across diverse populations. Genome Med. 5, 55 (2013).
Adeyemo A. A. et al. Evaluation of genome wide association study associated type 2 diabetes susceptibility loci in sub Saharan Africans. Front. Genet. 6, 335, 1–8 (2015).
Jallow, M. et al. Genome-wide and fine-resolution association analysis of malaria in West Africa. Nat. Genet. 41, 657–65 (2009).
Ng, M. C. et al. Genome-wide association of BMI in African Americans. Obesity 20, 622–7 (2012).
Tan, L. J. et al. Replication of 6 obesity genes in a meta-analysis of genome-wide association studies from diverse ancestries. PLoS ONE 9, e96149 (2014).
Comuzzie, A. G. et al. Novel genetic loci identified for the pathophysiology of childhood obesity in the Hispanic population. PLoS ONE 7, e51954 (2012).
Hsu, F. C. et al. Heritability of body composition measured by DXA in the diabetes heart study. Obes. Res. 13, 312–9 (2005).
Ramsay M. et al. H3Africa AWI-Gen Collaborative Centre: a resource to study the interplay between genomic and environmental risk factors for cardiometabolic diseases in four sub-Saharan African countries. Glob. Health Epidemiol Genom. e20, 1-13 (2016).
Acknowledgements
The authors wish to thank Phelelani Mpangase for his assistance with bioinformatics and data analysis support. The authors are also grateful to the participants of the Birth to Twenty study. The AWI-Gen Collaborative Centre is funded by the National Institutes of Health (U54HG006938) as part of the H3Africa Consortium. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health. The work is also based on the research supported in part by the Thuthuka Programme of the National Research Foundation (NRF) of South Africa for the grant, Unique Grant No. 94007 & 80702. V.S. is supported by the Wits/NIH Non-Communicable Diseases Leadership Programme, funded through the Fogarty International Centre of the NIH Millennium Promise Awards: Noncommunicable Chronic Diseases Research Training Programme (D43), Grant Number: D43TW008330-01A1. Birth to Twenty is funded by the University of the Witwatersrand, Johannesburg, South African Medical Research Council, and the Wellcome Trust (UK) (grant number 092097/Z/10/Z). R.J.M. and S.A.N. are supported by the DST-NRF Centre of Excellence in Human Development at the University of the Witwatersrand, Johannesburg.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Sahibdeen, V., Crowther, N.J., Soodyall, H. et al. Genetic variants in SEC16B are associated with body composition in black South Africans. Nutr & Diabetes 8, 43 (2018). https://doi.org/10.1038/s41387-018-0050-0
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41387-018-0050-0
This article is cited by
-
Genetic variation in NOTCH1 is associated with overweight and obesity in Brazilian elderly
Scientific Reports (2024)
-
Assessing efficiency of fine-mapping obesity-associated variants through leveraging ancestry architecture and functional annotation using PAGE and UKBB cohorts
Human Genetics (2023)
-
QTL-mapping in the obese Berlin Fat Mouse identifies additional candidate genes for obesity and fatty liver disease
Scientific Reports (2022)
-
Parent-of-Origin inference for biobanks
Nature Communications (2022)
-
Transcriptional regulation of the ER stress-inducible gene Sec16B in Neuro2a cells
Molecular and Cellular Biochemistry (2021)