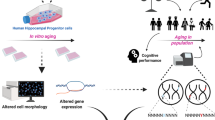
Abstract
Environmental factors like diet have been linked to depression and/or relapse risk in later life. This could be partially driven by the food metabolome, which communicates with the brain via the circulatory system and interacts with hippocampal neurogenesis (HN), a form of brain plasticity implicated in depression aetiology. Despite the associations between HN, diet and depression, human data further substantiating this hypothesis are largely missing. Here, we used an in vitro model of HN to test the effects of serum samples from a longitudinal ageing cohort of 373 participants, with or without depressive symptomology. 1% participant serum was applied to human fetal hippocampal progenitor cells, and changes in HN markers were related to the occurrence of depressive symptoms across a 12-year period. Key nutritional, metabolomic and lipidomic biomarkers (extracted from participant plasma and serum) were subsequently tested for their ability to modulate HN. In our assay, we found that reduced cell death and increased neuronal differentiation were associated with later life depressive symptomatology. Additionally, we found impairments in neuronal cell morphology in cells treated with serum from participants experiencing recurrent depressive symptoms across the 12-year period. Interestingly, we found that increased neuronal differentiation was modulated by increased serum levels of metabolite butyrylcarnitine and decreased glycerophospholipid, PC35:1(16:0/19:1), levels – both of which are closely linked to diet – all in the context of depressive symptomology. These findings potentially suggest that diet and altered HN could subsequently shape the trajectory of late-life depressive symptomology.
Similar content being viewed by others
Introduction
Major depressive disorder (MDD) is a debilitating condition that significantly impacts upon the physical, emotional and social wellbeing of individuals and their relatives [1]. Moreover, MDD is highly prevalent across all age ranges and consequently represents a major financial burden globally [2]. Given the devastating consequences of MDD, late-life depression, in particular, is an important public health concern, increasing the risk of morbidity and suicide, decreasing physical, cognitive and social functioning, and increasing self-neglect in later life - all of which are subsequently associated with increased mortality [3].
Importantly, late-life depression has also been consistently associated with an increased risk of cognitive decline (CD) and dementia [4, 5] both of which also significantly increase in risk in later life [6]. Furthermore, these conditions are often comorbid [7], and, therefore, treating one condition could consequently alleviate the associated symptoms of the other(s). Thus, late-life depression could also represent a target for preventing or alleviating CD and/or dementia [8].
Unfortunately, the development and implementation of effective pharmacological treatments for MDD is struggling to keep pace with the growth of its prevalence [9] and to better target MDD, we need to go beyond pharmacological intervention and seek other methods of modifying depression risk. One relevant avenue is environmental and lifestyle modification, in particular diet, which has been associated with depression in later life [10]. Indeed, several epidemiological studies have demonstrated how a higher adherence to the Mediterranean diet was associated with a reduced MDD prevalence in ageing populations [11, 12]. However, as yet it is unclear how exactly diet could influence depression outcomes on a biological level [13].
One relevant biological process associated with depression [14, 15] that is also modulated by diet [16, 17], is adult hippocampal neurogenesis (HN; the birth of new neurons derived from stem cells present in the hippocampus [18, 19]). Evidence to support an important role for HN in depression aetiology stems from research showing how chronic stress exposure (a risk factor for depression) supresses HN [20, 21], which, importantly, correlates with hippocampal volume and is notably required for antidepressant drugs to be effective in rodent models of depression [22, 23].
However, currently it is impossible to test the effects of diet on neurogenesis in live humans, and one option is to use an in vitro readout of human HN [24,25,26,27]. The main concept and relevance of this in vitro assay stems from the fact that the hippocampal neurogenic niche is in close vicinity to blood vessels, allowing direct communication with the systemic environment [28]. As such, HN is responsive to systemic and peripheral modulators like stress, inflammation and diet [16, 29] - all cues extrinsic to the brain and delivered via the blood. This idea is further supported from several lines of research. For example, Villeda and colleagues (2011), in their in vivo parabiosis model, demonstrate that ageing blood in young animals can indeed decrease HN [30, 31], while specific blood factors have been shown to transfer the beneficial effects of exercise on HN and cognition in rodents [32, 33]—all emphasising a role for modulation of HN by blood-borne factors.
Therefore, here we set out to study the effect of the systemic environment on the hippocampal neurogenic process in participants with and without depressive symptomology, using an in vitro cellular HN assay. Specifically, we used serum samples taken at inclusion of a longitudinal ageing cohort to: (i) determine whether changes in the neurogenic process are associated with depressive symptomology and chronicity across a 12-year period, (ii) explore the relationship between CD and depressive symptomology and the impact this may have on neurogenesis, and (iii) ascertain whether nutritional, metabolomic, and lipidomic biomarkers could modulate these HN outcomes.
Methods and materials
Cohort and study design
Serum samples were from participants of the Three-City (3C) cohort [34], specifically, from a case-control study on CD (n = 373) nested within the 3C-Bordeaux centre as described before [35]. Briefly, at baseline, fasting blood samples and sociodemographic, lifestyle and clinical measures were collected from all participants. Follow-up visits were performed every two to three years over 12 years during which depressive symptomology were assessed (Fig. 1A). The 3C study protocol was approved by the Consultative Committee for the Protection of Persons participating in Biomedical Research at Kremlin-Bicetre University Hospital (Paris, France). For further detail, see Table 1 and Supplementary Materials.
A Three City (3C) cohort and study design: The 3C cohort is a French population-based cohort that started in 1999–2000 and consists of male and female community dwellers aged >65 years (n = 9294). Participants from the 3C study were recruited from three French cities: Bordeaux (n = 2104), Dijon (n = 4931), and Montpellier (n = 2259), and specifically, a subsample nested within the 3C-Bordeaux cohort (n = 373) was used for this study. At baseline (0y), face-to-face interviews were conducted to collect sociodemographic and lifestyle characteristics, medical information, cognitive testing, blood pressure, and anthropometric measurements from all participants. Additionally, fasting blood samples were collected for constitution of a biobank; the serum samples of which were used for the metabolomics, lipidomics and the in vitro cellular assays, whereas the plasma samples were used to extract the nutritional biomarker data. Follow-up visits were performed every 2 to 3 years over a 12-year period and assessed depressive symptomology and cognitive decline. Cases were classified as all participants that reported high depressive symptomology (i.e., ≥17 in men and of ≥23 in women on the CES-D scale) at any timepoint (including at baseline) across the 12-year study period, whereas controls were all participants that did not report experiencing high depressive symptomology. In vitro neurogenesis cellular assays: B Proliferation assay: 24 h after seeding, cell medium was replaced with fresh medium containing 1% serum and 1:100 penicillin streptomycin (PenStrep; 10,000 U/mL) and was subsequently left to incubate for 72 h before being fixed in 4% paraformaldehyde (PFA), stained and proliferation specific markers quantified. C Differentiation assay: after 48 h of proliferation in the presence of 1% serum and 1:100 PenStrep (same as proliferation assay), cells were washed and treated with another serum supplementation, this time in medium absent of 4-hydroxytamoxifen (4-OHT) and growth factors: epidermal growth factor (EGF) and basic fibroblast growth factor (FGF), to allow cells to spontaneously differentiate. Serum-treated cells and were subsequently left to differentiate for a further 7 days before being fixed in 4% PFA, stained, and differentiation specific markers quantified. Cognitive decline status definition: Participants were classified as either cognitively stable or with accelerated cognitive decline based on their average performance in five neuropsychological tests (i.e., the Mini-Mental State Examination, the Benton Visual Retention Test, the Isaac’s Set Test, and the Trail-Making Test part A and part B) across five follow-up visits across the 12-year study duration. (1) Serum samples used for the metabolomics, lipidomics and in vitro assays are aliquots taken from the same batch. 3C three city, M male, F female, y years, h hours, 4-OHT 4-hydroxytamoxifen, CES-D Epidemiologic Studies Depression scale. Image created using BioRender software.
Depressive symptomology outcomes
Depressive symptomatology was evaluated using the Centre for Epidemiologic Studies Depression (CES-D) scale [36, 37]. Scores of ≥17 in men and of ≥23 in women were used as indicators of clinically relevant depressive symptomatology [38]. Additionally, to assess symptom chronicity, cases were further categorised based on whether a high depressive symptomology was detected once (i.e., single occurrence) or multiple times (i.e., recurrent symptoms) across the study. To retain a maximum number of participants with depressive symptomology, participants that had symptoms at baseline were retained in all analyses, and baseline depressive symptomology was controlled for in all analyses. For further detail, see Supplementary Materials.
Nutritional variables
The concentrations of 23 nutritional biomarkers (i.e., 12 fatty acids, 6 carotenoids, 25(OH)D, alpha and gamma tocopherol, retinol, transthyretin) were determined in total plasma as previously described [39,40,41]. The metabolite and lipid data were extracted from serum using a large-scale, quantitative multi-metabolite platform and shotgun MS lipidomics, respectively, as described previously [42, 43]. For a full list of all nutritional variables, see Table 2.
Cell line and culture conditions
We used the immortalised human fetal hippocampal multipotent progenitor cell line HPC0A07/03 (HPC; ReNeuron Ltd, UK) as described before [27]. HPCs were cultured in medium (constitution as previously described [27]) and grown on tissue culture flasks, incubated at 37 °C, with 5% CO2 and saturated humidity. Cells were routinely passaged at 80% confluency before being plated for experiments. For further detail, see Supplementary Materials and Fig. S1.
In vitro neurogenesis assay
HPC0A07/03C cells were treated with participant serum during their proliferation and differentiation, as previously described [27]. As detailed in Fig. 1B, 1% serum was added to the cell culture during both proliferation (48 h) and differentiation (7 days) before being fixed in 4% paraformaldehyde and stained for proliferation and differentiation specific markers, respectively. For further detail, see Supplementary Materials.
Immunocytochemistry
Cell count, progenitor cell integrity, proliferation, cell death and differentiation were visualised using 4′,6-diamidino-2-phenylindole (DAPI), Nestin and SRY-Box Transcription Factor 2 (SOX2), Ki67, cleaved caspase-3 (CC3), doublecortin (DCX), and microtubule-associated protein 2 (MAP2) using immunocytochemistry, as previously described [27, 44]. For further detail, see Supplementary Materials and Fig. S2.
Image analysis
All immunostainings were quantified using the unbiased, semi-automated CellInsight NXT High Content Screening platform and Studio Cell Analysis Software (ThermoScientific), as previously described [27, 44]. For further detail, see Supplementary Materials.
Neurite outgrowth
To quantify the neurite outgrowth and branching of neuronal cells after differentiation, automated neurite outgrowth analyses were performed. Images were acquired using the CellInsight (as above) and analysis was performed using the web-based Columbus Analysis System (Perkin Elmer) and the CSIRO Neurite Analysis 2 method, as previously described [45]. For protocol details, see Supplementary Materials.
All experiments, immunocytochemistry, and image analyses were performed by an experimenter blinded to depressive status. All experiments were carried out in technical triplicates.
Statistical analysis
Data analyses were conducted using SPSS Statistics 26 and R software (version 3.6.3). Logistic and linear regression models were used to study the association between HN readouts and depressive symptomology, and nutrient, metabolomic, and lipidomic biomarkers, respectively. Additionally, mediation and moderation analyses were conducted using the PROCESS macro, as previously described [46], to (i) more fully explore the relationship between neurogenesis, diet and depressive symptomology, and (ii) determine (where relevant) how key risk factors (e.g., CD, hippocampal volume, stress and inflammation) may influence the relationship between neurogenesis and depressive symptomology. All models were primarily adjusted for age, gender, education, and CD status, and in case of association, further adjustment was performed by including baseline depression status and relevant potential confounders (Tables 1–2). False discovery rate correction was applied to account for multiple testing throughout and all models were bootstrapped enhanced to obtain robust estimates of standard errors. For further detail, see Supplementary Materials.
Results
Cohort characteristics
Table 1 details the characteristics of our sample. Specifically, participants were on average 76 years old at baseline, 66% were female and 29% had a secondary school education or higher.
Within our sample, 8% of participants reported depressive symptomology at baseline, which increased to 30% across the duration of the study. Of this 30%: 18% experienced symptoms at a single timepoint (2% at baseline only), while the remaining 12% repeatedly reported symptoms (5% including baseline).
To start, we determined the association between individual HN markers and depressive symptomology reported at any timepoint, irrespective of chronicity. Only altered apoptosis during proliferation (i.e., %CC3- and %Ki67/CC3-positive cells; highlighted in blue in Table 1) and neuronal differentiation (i.e., %MAP2-positive cells and associated morphology; all highlighted in purple in Table 1) were significantly associated with depressive symptoms.
A drive towards hippocampal stem cell differentiation may be associated with depressive symptomology
As depicted in Fig. 2A–C, decreased baseline levels of %Ki67/CC3-positive cells (i.e., dying proliferating cells; p = 0.02) and increased baseline levels of %MAP2-positive cells (i.e., young neurons; p = 0.002) were significantly associated with depressive symptomology within our sample across the 12-year period.
A Model 1: Association between baseline proliferative cell death (i.e., %Ki67/CC3) and neuronal differentiation (i.e., %MAP2) and depressive symptomology using logistic regression. Reduced baseline levels of %Ki67/CC3-positive cells (OR 0.23 [95% CI; 0.08 to 0.69]; p = 0.02) and increased %MAP2-positive cells (OR 1.06 [95% CI; 1.01 to 1.11]; p = 0.002) were both independently associated with depressive symptomology across the 12-year study period in a fully adjusted model. Model adjusted for age, gender, education, cognitive decline status, baseline depression, plasma glucose levels and total hippocampal volume. *p < 0.05; **p < 0.01. B (i) Baseline levels of %Ki67/CC3-positive cells stratified by caseness for depressive symptomology. Cases, i.e., those scoring positive for depressive symptomology at least once across the 12-year study (including at baseline), had significantly reduced levels of baseline levels of %Ki67/CC3-positive cells (M = 0.74 (0.05) vs. M = 0.56 (0.05)). Cellular readout expressed as a percentage relative to neural cell number. Cell line: HPC0A07/03; Passage number: P15-21; Technical replicates: n = 3; Data represents mean ± SEM. *p < 0.05. (ii) Representative immunostaining demonstrating %Ki67/CC3-positive cells for representative case and control. Images taken at x10 objective; scale bar represents 100 µm. C (i) Baseline levels of %MAP2-positive cells stratified by caseness for depressive symptomology. Cases had significantly increased levels of baseline %MAP2-positive cells (M = 44.3 (1.13) vs. M = 47.7 (1.09)). Cellular readout expressed as a percentage relative to neural cell number. Cell line: HPC0A07/03; Passage number: P15-21; Technical replicates: n = 3; Data represents mean ± SEM. **p < 0.01. (ii) Representative immunostaining demonstrating %MAP2-positive cells for representative case and control. Images taken at x10 objective; scale bar represents 100 µm. D (i) Baseline levels of %CC3-positive cells stratified by caseness for a single occurrence of depressive symptomology. Cases, i.e., those scoring positive for depressive symptomology only once across the 12-year study duration (including baseline), had significantly reduced levels of baseline levels of %CC3-positive cells (M = 1.02 (0.10) vs. M = 1.32 (0.06)). Cellular readout expressed as a percentage relative to neural cell number. Cell line: HPC0A07/03; Passage number: P15-21; Technical replicates: n = 3; Data represents mean ± SEM. *p < 0.05. (ii) Representative immunostaining demonstrating %CC3-positive cells during proliferation for representative case and control. Images taken at x10 objective; scale bar represents 100 µm. E (i) Baseline levels of %Ki67/CC3-positive cells stratified by caseness for a single occurrence of depressive symptomology. Cases had significantly reduced levels of baseline levels of %Ki67/CC3-positive cells (M = 0.53 (0.07) vs. M = 0.70 (0.03)). Cellular readout expressed as a percentage relative to neural cell number. Cell line: HPC0A07/03; Passage number: P15-21; Technical replicates: n = 3; Data represents mean ± SEM. *p < 0.05. (ii) Representative immunostaining demonstrating %Ki67/CC3-positive cells during proliferation for representative case and control. Images taken at x10 objective; scale bar represents 100 µm. F Important risk factors for a single occurrence of depressive symptomology: Model 2: Effect of baseline overall cell death and proliferative cell death on a single occurrence of depressive symptomology using logistic regression. Baseline levels of %CC3-positive cells during proliferation (OR 0.72 [95% CI; 0.53 to 0.91]; p = 0.03) and %Ki67/CC3-positive cells (OR 0.60 [95% CI; 0.35 to 0.98]; p = 0.04) were both associated with a single occurrence of depressive symptomology across the study period in a partially adjusted model (controlling for age, gender, education, and cognitive decline). However, these neurogenesis readouts were no longer significant in a fully adjusted model (controlling for age, gender, education, cognitive decline status, baseline depression, hypercholesterolemia, antecedents of cardiovascular disease, total hippocampal volume, cortisol levels and vitamin D supplementation) and were confounded by hippocampal volume (OR 0.98 [95% CI; 0.98 to 0.99]; p = 0.04). *p < 0.05. G (i) Baseline levels of %Ki67-positive cells (during proliferation) stratified by caseness for recurrent depressive symptomology. Cases, i.e., those scoring positive for depressive symptomology repeatedly across the 12-year study period, had a trend for reduced levels of baseline levels of %Ki67-positive cells during differentiation (M = 79.5 (1.14) vs. M = 81.6 (0.44)). Cellular readout expressed as a percentage relative to neural cell number. Cell line: HPC0A07/03; Passage number: P15-21; Technical replicates: n = 3; Data represents mean ± SEM. *p < 0.05. (ii) Representative immunostaining demonstrating %Ki67-positive cells during proliferation for representative case and control. Images taken at x10 objective; scale bar represents 100 µm. H (i) Baseline levels of %MAP2-positive cells stratified by caseness for recurrent depressive symptomology. Cases had significantly increased levels of baseline %MAP2-positive cells (M = 50.3 (1.48) vs. M = 44.8 (0.70)) relative to controls. Cellular readout expressed as a percentage relative to neural cell number. Cell line: HPC0A07/03; Passage number: P15-21; Technical replicates: n = 3; Data represents mean ± SEM. *p < 0.05. (ii) Representative immunostaining demonstrating %MAP2-positive cells for representative case and control. Images taken at x10 objective; scale bar represents 100 µm. I %MAP2-positive cell density, as associated with recurrent depressive symptomology, was modified by cognitive decline. Model 3.A: There was a significant interaction between %MAP2 and cognitive decline in participants with recurrent depressive symptomology (OR 1.07 [95% CI; 1.004 to 1.03]; p = 0.01). Model3.B: Further analyses revealed that %MAP2 was only associated with recurrent depressive symptomology in participants that also had cognitive decline (OR 1.08 [95% CI; 1.01 to 1.14]; p = 0.02). Models 3.A-B adjusted for age, gender, education, baseline depression, glucose levels, IL6 plasma levels, and regular physical exercise. *p < 0.05. CC3 cleaved caspase 3, MAP2 microtubule-associated protein 2, IL interleukin, OR odds ratio, P passage, M mean.
Having found that a decrease in the apoptosis of proliferating cells and an increase in neuronal differentiation was associated with depressive symptomology overall, we next sought to determine whether these HN outcomes would change depending on symptom chronicity.
Reduced proliferative cell death is associated with a single occurrence of depressive symptomology but is confounded by hippocampal volume
As shown in Fig. 2D, participants classified as experiencing depressive symptoms at a single timepoint across the study had significantly reduced baseline levels of %CC3-positive cells during proliferation (i.e., overall cell death; p = 0.03), in addition to a specific reduction in %Ki67/CC3 (i.e., dying proliferating cells; p = 0.04; Fig. 2E). However, when controlling for hippocampal volume, these associations no longer held (Fig. 3F).
A Association between lipid and metabolite levels and cell death during proliferation. (i) Model 4: Association between lipid and metabolite levels and baseline levels of cell death during proliferation using linear regression. Baseline serum levels of lipid PEO34:3(16:1/18:2) (ß = −0.13 [95% CI; −0.41 to −0.04] 0.09; p = 0.02), and baseline serum levels of metabolite butyrylcarnitine (ß = 0.15 [95% CI; 0.01 to 0.06] 0.01; p = 0.007) were both associated with baseline %CC3-positive cell levels during proliferation in a fully adjusted model. Model adjusted for age, gender, education, cognitive decline status, baseline depression. (a) Increments are the estimates expressed as a 1-standard deviation increase. *p < 0.05; **p < 0.01. Scatterplot showing (ii) negative relationship between baseline serum levels of lipid PEO34:3(16:1/18:2) and %CC3-positive cells during proliferation at baseline (pink), and (iii) positive relationship between baseline serum levels of metabolite butyrylcarnitine and %CC3-positive cells during proliferation at baseline (purple). B Association between lipid levels and proliferative cell death. (i) Model 5: Association between lipid levels and baseline levels of proliferative cell death using linear regression. Baseline serum levels of lipid PEO34:3(16:1/18:2) (ß = −0.27 [95% CI; −0.49 to −0.07] 0.10; p = 0.008) were associated with baseline %Ki67/CC3-positive cell levels during proliferation in a fully adjusted model. Model adjusted for age, gender, education, cognitive decline status, baseline depression, hippocampal volume, and Mediterranean diet score. (a) Increments are the estimates expressed as a 1-standard deviation increase. **p < 0.01. Scatterplot showing (ii) negative relationship between baseline serum levels of lipid PEO34:3(16:1/18:2) and %Ki67/CC3-positive cells during proliferation at baseline (pink). C Association between nutritional biomarker levels and differentiation. (i) Model 6: Association between nutritional biomarker levels and baseline levels of neuronal cell differentiation using linear regression. Reduced plasma levels of transthyretin (ß = −0.22 [95% CI; −0.28 to −0.49] 0.01; p = 0.006) were associated with increased baseline %MAP2-positive cell levels in a fully adjusted model. Model adjusted for age, gender, education, cognitive decline status, baseline depression, zeaxanthin levels, arachidonic acid levels, retinol levels and cell passage number. (a) Increments are the estimates expressed as a 1-standard deviation increase. **p < 0.01. (ii) Scatterplot showing negative relationship between baseline plasma transthyretin levels and %MAP2-positive cells at baseline (pink). D Association between lipid levels and differentiation. (i) Model 7: Association between lipid levels and baseline levels of neuronal cell differentiation using linear regression. Reduced serum levels of lipid PC35:1(16:0/19:1) (ß = −2.77 [95% CI; −5.52 to −0.08] 0.01; p = 0.047) were associated with increased baseline %MAP2-positive cell levels in a fully adjusted model. Model adjusted for age, gender, education, cognitive decline status, baseline depression, PC32:2(14:0/18:2) levels, PC34:3(16:1/18:2) levels and cell passage number. (a) Increments are the estimates expressed as a 1-standard deviation increase. *p < 0.05. (ii) Scatterplot showing negative relationship between baseline serum levels of lipid PC35:1(16:0/19:1) and %MAP2-positive cells at baseline (pink). E There was a significant indirect effect of baseline serum levels of lipid PC35:1(16:0/19:1) on depressive symptomology through baseline %MAP2-positive cell levels (ab = −0.08 [−0.19; −0.001]). The mediator (i.e., %MAP2-positive levels) accounted for 24% of the total effect (PM = 0.24). F The association between metabolite butyrylcarnitine and depressive symptomology was modified by neuronal differentiation. (i) There was a significant interaction between serum levels of metabolite butyrylcarnitine and %MAP2-positive cell levels (b = 0.005; SE = 0.002; p = 0.04). (ii) Interaction plot revealing that the positive association between serum levels of metabolite butyrylcarnitine and depressive symptomology was only significant for participants that had %MAP2 levels greater than 47% in our sample (p = 0.02). CC3 cleaved caspase 3, MAP2 microtubule-associated protein 2.
Increased neuronal differentiation and impaired neuronal cell morphology is associated with recurrent depressive symptomology but is modified by cognitive decline
Unlike a single occurrence of depressive symptomology, we found that increased baseline levels of %MAP2-positive cells were significantly associated with experiencing recurrent depressive symptoms across the course of the study (p = 0.02; Fig. 2H). Additionally, although not reaching statistical significance, we also observed a decrease in the level of %Ki67-positive cells (i.e., overall proliferation) for participants with recurrent depressive symptoms (p = 0.07; Fig. 2G). Moreover, although participants with recurrent depressive symptomology had more %MAP2-positive cells, morphological analyses revealed a significantly impaired morphology, such that these MAP2-positive cells had a reduced total neurite length (p = 0.003), fewer number of neurites (p = 0.005) and a less complex degree of neurite branching (p = 0.006) (Table 1).
Interestingly, in our fully adjusted model, we found a significant interaction between %MAP2 and CD amongst those with recurrent depressive symptoms (p = 0.01), revealing that these changes in %MAP2 were only associated with recurrent depressive symptomology in those also diagnosed with CD (p = 0.02; Fig. 2I).
Thus far, we have shown that a potential drive towards hippocampal stem cell differentiation may be associated with late-life depressive symptomology, and that CD can modify the association of %MAP2 in participants experiencing recurrent depressive symptoms. No differences in any other individual neurogenesis readout, i.e., %Nestin-, %SOX2-, %CC3-(during differentiation) or %DCX-positive cells, were observed between groups (Table 1). Moreover, we found no difference in the neurite morphology of %DCX- and %MAP2-positive cells between depressive symptomology (overall), or a single depressive episode, and controls (Table 1). Additionally, principal component analyses revealed no differences in the overall neurogenic profiles between groups (Supplementary Materials).
Next, as detailed in Table 2, we assessed whether nutritional status could modulate these changes in %CC3 (prol), %Ki67/CC3 and %MAP2.
Neuronal differentiation mediates the relationship between PC35:1(16:0/19:1) and depressive symptomology, while the association between metabolite butyrylcarnitine and depressive symptomology is modified by neural differentiation
As shown in Fig. 3, reduced serum levels of lipid PE034:3(16:1/18:2) (p = 0.02) and increased serum levels of metabolite butyrylcarnitine (p = 0.007) were both independently associated with increased baseline levels of %CC3-positive cells during proliferation in a fully adjusted model (Fig. 3A). Additionally, we also found a negative association between serum levels of lipid PE034:3(16:1/18:2) and baseline %Ki67/CC3 (p = 0.008; Fig. 3B). Moreover, reduced plasma levels of transthyretin (p = 0.006; Fig. 3C), and serum levels of glycerophospholipid, phosphatidylcholine [PC]35:1(16:0/19:1) (p = 0.047; Fig. 3D) were both independently associated with increased %MAP2.
While we found that several nutritional measures were associated with HN in our sample, only metabolite butyrylcarnitine and lipid PC35:1(16:0/19:1) were also associated with depressive symptomology. Specifically, we found a significant positive association between butyrylcarnitine levels (p = 0.049), and a negative association between PC35:1(16:0/19:1) levels (p = 0.045), and depressive symptoms.
To understand the relationship(s) more fully between this metabolite and phospholipid, our HN outcomes, and depressive symptomology, mediation analyses were subsequently performed. As depicted in Fig. 3E, we found a significant indirect effect of serum PC35:1(16:0/19:1) levels (ab = −0.08 [−0.19; −0.01]; p = 0.04) on depressive symptomology as mediated through %MAP2 levels.
While we found no significant indirect effect of butyrylcarnitine levels on depressive symptomology as mediated through %CC3, we did however find a significant interaction between %MAP2 and this metabolite (p = 0.04). Therefore, we performed a simple moderation analysis and found that those with higher levels of %MAP2 (i.e., <46%, p = 0.03; <58%, p = 0.01) and increased levels of butyrylcarnitine were more likely to have depressive symptoms (p = 0.005; Fig. 3F).
Discussion
Using serum samples from a longitudinal, population-based ageing cohort, we provide evidence to support that blood-borne factors, via the systemic milieu of participants, influence the fate of hippocampal progenitor cells in vitro, notably in association with late-life depressive symptomology. We demonstrate that both reduced baseline levels of apoptotic, proliferating cells (i.e., %Ki67/CC3-positive cells) and increased baseline differentiation (i.e., %MAP2-positive cells) are independently associated with the occurrence of depressive symptomology across a 12-year period in later life. Moreover, these neurogenesis outcomes appear to be context-specific regarding the chronicity and recurrence of depressive symptoms. For example, reduced proliferative cell apoptosis was uniquely associated with experiencing depressive symptomology at a single timepoint, whereas increased neuronal differentiation was a hallmark of recurrent symptomology within our cohort. Furthermore, we demonstrated that these alterations in neurogenesis were modulated by metabolomic and lipidomic biomarkers, i.e., butyrylcarnitine and PC35:1(16:0/19:1), and that diet could thus play an important role in regulating the neurogenic process in humans.
The hippocampus has been implicated in learning and memory [47, 48], stress responsivity [49, 50] and emotional regulation [51] factors all associated with, and often altered in, MDD [52, 53]. The hippocampus is also unique in that it contains one of the niches within the human brain where neurogenesis occurs [54]. Our present in vitro data suggest that depressive symptoms are not only associated with reduced hippocampal volume—one of the most replicated neuroimaging findings in MDD research [55], but also that HN may play a key role in the pathogenesis and/or progression of depression.
In the context of our work, we found a specific decrease in the number of dying proliferative cells during the earlier, proliferation phase of the neurogenic process, without a concomitant decrease in overall cell death. We also observed a subsequent increase in the number of neurons during differentiation, which may be a ‘knock-on’ effect of the changes occurring in the earlier stages of the neurogenic process. Taken together, this suggests that neuronal cells might be pushed towards differentiation in late-life depression, which, importantly, is not attributable to antidepressant medication here, as previously described [56,57,58]. Interestingly, an increase in peripheral levels of MAP2 in bipolar depression has recently been reported as well [59], while one post-mortem study also showed an increase in pyramidal neuronal density in the CA1 in chronic MDD [60]. However, it is notable that the literature predominately reports a reduction in all neurogenesis-associated readouts in depression [61], although, these findings primarily stem from end-stage tissue samples from young-to-middle aged MDD patients; therefore, it is difficult to extrapolate these results to that of our own.
Our most exciting finding is that despite our unique sample and study, with prominent differences in time (12-year follow-up), approach and measures (cellular changes vs. depressive symptomatology), some specificity persisted nevertheless between our HN outcomes and the chronicity and/or recurrent nature of depressive symptomology. For example, the observed drive towards neuronal differentiation was unique to experiencing recurrent depressive symptoms within our cohort. Moreover, although we observed an increase in MAP2 neurons in our in vitro assay from participants with recurrent symptoms, the morphology of these neurons was significantly impaired; they had fewer, shorter neurites and a less complex branching pattern—a finding that has previously been reported in stress models [62, 63], in older individuals with psychological distress [64], and in the context of late-life depression [65]. Furthermore, several clinical studies have reported synaptic dysfunction in MDD, albeit in the prefrontal cortex, which may be one functional biological consequence of these observed morphological changes [66], of which MAP2 plays a key role [67]. However, whether the increased number of differentiating cells is a causal or adaptive response to these morphological impairments requires further substantiation.
One of the potentially wider functional implications of the changes in HN observed for those with recurrent depressive symptomology could relate to cognitive capacity [68]. Indeed, while neurogenesis was associated with recurrent depressive symptoms in our sample, this was only found in a subset of these participants, i.e., those that subsequently developed CD, highlighting the complex relationship between CD and depression particularly in later life. Our data suggest that either recurrent depressive symptoms could here represent a consequence, or concomitant event, of CD (and altered HN), or that altered HN could potentially modulate cognitive reserve, or exacerbate cognitive impairment in, those already suffering with recurrent depressive symptoms. Pertinently, an association between altered HN and CD has consistently been reported in rodent models [69], in addition to the recognised overlap between depression, CD and dementia for which neurogenesis may be an important mediator [61].
In the context of a single episode of depressive symptomology, although we observed a negative association with proliferative cell death, this was confounded by hippocampal volume. More specifically, reduced hippocampal volume increased the risk of a single depressive episode—a finding consistently reported in the literature [55]. Interestingly, we also observed a positive relationship between total hippocampal volume and this HN-associated outcome, potentially representing a compensatory response to loss of volume. However, mediation analyses did not support that the relationship between hippocampal volume and a single depressive episode was modulated by reduced proliferative cell death in our sample, although we are mindful that insufficient power upon sample stratification may have limited these analyses [70]. Future work should seek to explore the relationship more fully given that our understanding of the molecular and cellular processes contributing to hippocampal volume loss (and the role that HN plays) are not well-established [71, 72] and that this may represent an important predictive biomarker for depression and its associated recovery [73].
Given that the strongest risk factors for late-life depression are related to environmental and/or sociodemographic characteristics [74], it is unsurprising that in the context of a single, possibly, acute depressive episode that demographic factors such as education (which attributed most to the outcome) would be more relevant. Alterations in neurogenesis, in the context of depression, may only be relevant under more chronic forms of exposure, and/or, more importantly, in the presence of other key risk factors for depression – as we have demonstrated in the context of recurrent depressive symptomology. Meaningfully, we did find a negative relationship between cortisol levels (a biomarker for depression [75]) and a single episode of depressive symptomology, although this does contradict the literature predominately supporting a positive association [76]. However, it is noteworthy that in community-dwelling older adults, both hypo- and hypercortisolism have been associated with increased depressive symptomology and that hypocortisolism was present only in those with more health problems [77]. In our cohort we observed a similar outcome: those with a single bout of depressive symptomology also presented poorer health outcomes (i.e., increased hypercholesterolemia and antecedents of cardiovascular disease, Table 1). Poorer health status may therefore represent an additional burden in this subgroup, possibly leading to chronic stress and a blunted stress response.
Based on our findings that specific HN markers are associated with depression, we next sought to determine whether nutritional, metabolomic and/or lipidomic biomarkers could be modulating these outcomes, given the association between diet and neurogenesis [16, 17]. Interestingly, not only did we find that both metabolite butyrylcarnitine (a member of the acylcarnitines) and glycerophospholipid, PC35:1(16:0/19:1), were associated with depressive symptomology – findings that have previously been reported in clinical populations [78, 79] but that they also specifically modulated neuronal differentiation within our sample. For example, we show that reduced levels of PC35:1(16:0/19:1) were associated with increased differentiation, which in turn increased the risk of late-life depressive symptoms. Moreover, we find that the positive association between butyrylcarnitine levels and depressive symptomology is modified by differentiation, such that those individuals with higher levels of both butyrylcarnitine and neuronal differentiation are at the greatest risk.
Importantly, PCs are major components of the cell membrane, are involved in cell signalling and metabolism, and play a critical role in neurotransmission and synaptic plasticity [80, 81], while acytylcarnitines are required for β-oxidation and tricarboxylic acid cycle activity [81, 82]. Indeed, several studies demonstrate that the transition from neural stem cell to a neuronal lineage is accompanied by increased mitochondrial biogenesis, and a downregulation of glycolysis and fatty acid oxidation [81]. Thus, β-oxidation and lipogenesis play a critical role in neurogenesis and the dysregulation of these metabolic pathways could significantly impair the process. Our findings potentially support that there may be a metabolic dysregulation of neurodifferentiation in the context of late-life depression, given that we observe alterations in both butyrylcarnitine and PC35:1(16:0/19:1). Furthermore, these endogenously derived factors are closely related to diet [83, 84]. For example, the precursor of butyrylcarnitine is butyric acid, a short chain fatty acid whose main source is the microbial fermentation of dietary fibres in the gut [83]. Therefore, dietary modification in later life could represent a potential therapeutic target for depression.
Additionally, we also found that plasma levels of transthyretin – a biomarker for malnutrition [85] was negatively associated with neuronal differentiation. Malnutrition has consistently been associated with depression [86, 87], cognitive decline and/or dementia [88, 89], and plays an important role in altering brain plasticity, particularly during early life [90]. Interestingly, malnutrition is associated with increased apoptosis and immune system activation [91, 92], which might represent the mechanism of action by which overall nutrient deficiency alters neurogenesis. Moreover, we found a negative association between cell death during proliferation and (PE0)34:3(16:1/18:2) – an ether phospholipid that forms a key component of the lipid membrane and lipid rafts [93]. Ether phospholipids, together with cell death, not only plays a critical role in neurotransmission and synaptic plasticity [80], but has also been implicated in the pathogenesis of depression [79]. However, the precise mechanisms involved in how these nutritional factors influence HN outcomes remain to be elucidated, falling outside the scope of this study. Moreover, we are mindful that in our sample, neither transthyretin or PE034:3(16:1/18:2) levels were significantly associated with depressive symptomology and more work is needed to substantiation these findings in the context of depression.
Of note, consistent with previous research [94, 95], we did find a positive association between inflammation (i.e., plasma levels of IL6) and recurrent depressive symptomology, which could potentially represent another mechanism of action for this particular subgroup. Given that cytokines, like IL6, are important regulators of HN [96], it is possible that increased neuronal differentiation (as a potential consequence of altered neuronal apoptosis) may be associated with immune system dysfunction in chronic instances of late-life depression. However, we found no statistical evidence to support that the relationship between neuronal differentiation and recurrent depression was modulated by IL6 levels in our sample.
The strength of our work lies in the use of a well-characterised prospective cohort to evaluate the impact of nutrition (including metabolomics and lipidomics) on in vitro neurogenesis measures in the trajectory of late-life depressive symptomology. However, our study also has limitations. First, our HN measures are only proxy measures of in vitro neurogenesis; therefore, might not mirror those in vivo. It is also unclear whether these observed HN changes are causal or adaptive, given that this was a cross-sectional evaluation of neurogenesis. Moreover, we recognise that our assay does not reconstitute the neurogenic niche in its entirety, and future work should expand the model to include other important HN regulators such as microglia [97], particularly given the important association between depression and (neuro)inflammation, which could ultimately affect the outcomes presented herein [95, 98]. Finally, it would be profitable for future research to also extend the assay’s duration to monitor synaptic formation and plasticity (considering our morphological findings), and to adopt a longitudinal approach and compare HN markers and overall neurogenic profiles at multiple time points to understand the impact of the hippocampal neurogenic process more fully across the trajectory of late-life depression.
In summary, given that there are currently no methods of quantifying HN in living humans, our assay presents a powerful tool to better understand the relationship between diet, neurogenesis, and depression. More work is now needed to more fully understand how these metabolites/lipids can modulate HN in the context of depression, but we have shown that HN, modulated by butyrylcarnitine and PC35:1(16:0/19:1), is associated with late-life depressive symptomology, and that we can distinguish between HN-associated outcomes and symptom chronicity. Our work is particularly important given that current treatment options for depression are often limited [99], and, thus, diet may represent a promising way via which the burden imposed by this debilitating condition could be alleviated.
References
Otte C, Gold SM, Penninx BW, Pariante CM, Etkin A, Fava M, et al. Major depressive disorder. Nat Rev Dis Prim. 2016;2:16065.
Mathers CD, Loncar D. Projections of global mortality and burden of disease from 2002 to 2030. PLOS Med. 2006;3:e442.
Fiske A, Wetherell JL, Gatz M. Depression in older adults. Annu Rev Clin Psychol. 2009;5:363–89.
Herbert J, Lucassen PJ. Depression as a risk factor for Alzheimer’s disease: Genes, steroids, cytokines and neurogenesis—What do we need to know? Front Neuroendocrinol. 2016;41:153–71.
Gallagher D, Kiss A, Lanctot K, Herrmann N. Depressive symptoms and cognitive decline: A longitudinal analysis of potentially modifiable risk factors in community dwelling older adults. J Affect Disord. 2016;190:235–40.
Cole JH, Marioni RE, Harris SE, Deary IJ. Brain age and other bodily ‘ages’: implications for neuropsychiatry. Mol Psychiatry. 2019;24:266–81.
Cherbuin N, Kim S, Anstey KJ. Dementia risk estimates associated with measures of depression: a systematic review and meta-analysis. BMJ Open. 2015;5:e008853.
Dafsari FS, Jessen F. Depression—an underrecognized target for prevention of dementia in Alzheimer’s disease. Transl Psychiatry. 2020;10:160.
Penn E, Tracy DK. The drugs don’t work? antidepressants and the current and future pharmacological management of depression. Ther Adv Psychopharmacol. 2012;2:179–88.
Sanchez-Villegas A, Martínez-González MADiet. a new target to prevent depression? BMC Med. 2013;11:3.
Vicinanza R, Bersani FS, D’Ottavio E, Murphy M, Bernardini S, Crisciotti F, et al. Adherence to Mediterranean diet moderates the association between multimorbidity and depressive symptoms in older adults. Arch Gerontol Geriatr. 2020;88:104022.
Masana MF, Haro JM, Mariolis A, Piscopo S, Valacchi G, Bountziouka V, et al. Mediterranean diet and depression among older individuals: The multinational MEDIS study. Exp Gerontol. 2018;110:67–72.
Marx W, Lane M, Hockey M, Aslam H, Berk M, Walder K, et al. Diet and depression: exploring the biological mechanisms of action. Mol Psychiatry. 2021;26:134–50.
Boldrini M, Galfalvy H, Dwork AJ, Rosoklija GB, Trencevska-Ivanovska I, Pavlovski G, et al. Resilience is associated with larger dentate gyrus, while suicide decedents with major depressive disorder have fewer granule neurons. Biol Psychiatry. 2019;85:850–62.
Micheli L, Ceccarelli M, D’Andrea G, Tirone F. Depression and adult neurogenesis: Positive effects of the antidepressant fluoxetine and of physical exercise. Brain Res Bull. 2018;143:181–93.
Stangl D, Thuret S. Impact of diet on adult hippocampal neurogenesis. Genes Nutr. 2009;4:271–82.
Murphy T, Dias GP, Thuret S. Effects of diet on brain plasticity in animal and human studies: mind the gap. Neural Plast. 2014;2014:563160.
Ernst A, Frisén J. Adult neurogenesis in humans- common and unique traits in mammals. PLoS Biol. 2015;13:e1002045–e1002045.
Spalding KL, Bergmann O, Alkass K, Bernard S, Salehpour M, Huttner HB, et al. Dynamics of hippocampal neurogenesis in adult humans. Cell 2013;153:1219–27.
Du Preez A, Onorato D, Eiben I, Musaelyan K, Egeland M, Zunszain PA, et al. Chronic stress followed by social isolation promotes depressive-like behaviour, alters microglial and astrocyte biology and reduces hippocampal neurogenesis in male mice. Brain Behav Immun. 2021;91:24–47.
Du Preez A, Law T, Onorato D, Lim YM, Eiben P, Musaelyan K, et al. The type of stress matters: repeated injection and permanent social isolation stress in male mice have a differential effect on anxiety- and depressive-like behaviours, and associated biological alterations. Transl Psychiatry. 2020;10:325.
Santarelli L, Saxe M, Gross C, Surget A, Battaglia F, Dulawa S, et al. Requirement of hippocampal neurogenesis for the behavioral effects of antidepressants. Science. 2003;301:805–9.
Planchez B, Surget A, Belzung C. Adult hippocampal neurogenesis and antidepressants effects. Curr Opin Pharm. 2020;50:88–95.
Maruszak A, Murphy T, Liu B, de Lucia C, Douiri A, Nevado AJ, et al. Cellular phenotyping of hippocampal progenitors exposed to patient serum predicts conversion to Alzheimer’s Disease. BioRxiv. 2017:175604.
de Lucia C, Murphy T, Steves CJ, Dobson RJB, Proitsi P, Thuret S. Lifestyle mediates the role of nutrient-sensing pathways in cognitive aging: cellular and epidemiological evidence. Commun Biol. 2020;3:1–17.
Borsini A, Pariante CM, Zunszain PA, Hepgul N, Russell A, Zajkowska Z, et al. The role of circulatory systemic environment in predicting interferon-alpha-induced depression: The neurogenic process as a potential mechanism. Brain Behav Immun. 2019;81:220–7.
Du Preez A, Lefèvre-Arbogast S, Houghton V, de Lucia C, Low DY, Helmer C, et al. The serum metabolome mediates the concert of diet, exercise, and neurogenesis, determining the risk for cognitive decline and dementia. Alzheimer’s Dement. 2021:18;1–22.
Murphy T, Thuret S. The systemic milieu as a mediator of dietary influence on stem cell function during ageing. Ageing Res Rev. 2015;19:53–64.
Lucassen PJ, Meerlo P, Naylor AS, van Dam AM, Dayer AG, Fuchs E, et al. Regulation of adult neurogenesis by stress, sleep disruption, exercise and inflammation: Implications for depression and antidepressant action. Eur Neuropsychopharmacol. 2010;20:1–17.
Yousef H, Czupalla CJ, Lee D, Chen MB, Burke AN, Zera KA, et al. Aged blood impairs hippocampal neural precursor activity and activates microglia via brain endothelial cell VCAM1. Nat Med. 2019;25:988–1000.
Villeda SA, Luo J, Mosher KI, Zou B, Britschgi M, Bieri G. et al. The ageing systemic milieu negatively regulates neurogenesis and cognitive function. Nature. 2011;477:90–4.
Leiter O, Seidemann S, Overall RW, Ramasz B, Rund N, Schallenberg S, et al. Exercise-induced activated platelets increase adult hippocampal precursor proliferation and promote neuronal differentiation. Stem Cell Rep. 2019;12:667–79.
Horowitz AM, Fan X, Bieri G, Smith LK, Sanchez-Diaz CI, Schroer AB. et al. Blood factors transfer beneficial effects of exercise on neurogenesis and cognition to the aged brain. Science. 2020;369:167–73.
3C Study Group. Vascular factors and risk of dementia: design of the Three-City Study and baseline characteristics of the study population. Neuroepidemiology. 2003;22:316–25.
Low DY, Lefèvre-Arbogast S, González-Domínguez R, Urpi-Sarda M, Micheau P, Petera M, et al. Diet-related metabolites associated with cognitive decline revealed by untargeted metabolomics in a prospective cohort. Mol Nutr Food Res. 2019;63:1–10.
Radloff LS. The CES-D scale: a self-report depression scale for research in the general population. Appl Psychol Meas. 1977;1:385–401.
Eaton WW, Muntaner C, Smith C, Tien A, Ybarra M. Center for Epidemiologic Studies Depression Scale: Review and revision (CESD and CESD-R). In: Maruish ME, ed. The use of psychological testing for treatment planning and outcomes assessment. 3rd ed. Mahwah, NJ: Lawrence Erlbaum; 2004:363–77.
Cosco TD, Lachance CC, Blodgett JM, Stubbs B, Co M, Veronese N, et al. Latent structure of the Centre for Epidemiologic Studies Depression Scale (CES-D) in older adult populations: a systematic review. Aging Ment Health. 2020;24:700–4.
Feart C, Letenneur L, Helmer C, Samieri C, Schalch W, Etheve S, et al. Plasma carotenoids are inversely associated with dementia risk in an elderly french cohort. J Gerontol Ser A. 2016;71:683–8.
Samieri C, Féart C, Letenneur L, Dartigues J-F, Pérès K, Auriacombe S, et al. Low plasma eicosapentaenoic acid and depressive symptomatology are independent predictors of dementia risk. Am J Clin Nutr. 2008;88:714–21.
Feart C, Helmer C, Merle B, Herrmann FR, Annweiler C, Dartigues J-F, et al. Associations of lower vitamin D concentrations with cognitive decline and long-term risk of dementia and Alzheimer’s disease in older adults. Alzheimer’s Dement. 2017;13:1207–16.
Lefèvre-Arbogast S, Hejblum BP, Helmer C, Klose C, Manach C, Low DY, et al. Early signature in the blood lipidome associated with subsequent cognitive decline in the elderly: A case-control analysis nested within the Three-City cohort study. EBioMedicine. 2021;64:103216.
González-Domínguez R, Urpi-Sarda M, Jáuregui O, Needs PW, Kroon PA, Andrés-Lacueva C. Quantitative dietary fingerprinting (QDF)—A novel tool for comprehensive dietary assessment based on urinary nutrimetabolomics. J Agric Food Chem. 2020;68:1851–61.
Houghton V, Du Preez A, Lefèvre-Arbogast S, de Lucia C, Low DY, Urpi-Sarda M, et al. Caffeine compromises proliferation of human hippocampal progenitor cells. Front Cell Dev Biol. 2020;8:806.
Smeeth DM, Kourouzidou I, Duarte RRR, Powell TR, Thuret S Prolactin. Estradiol and testosterone differentially impact human hippocampal neurogenesis in an in vitro model. Neuroscience. 2020:454;1–25.
Hayes AF, Rockwood NJ. Regression-based statistical mediation and moderation analysis in clinical research: Observations, recommendations, and implementation. Behav Res Ther. 2017;98:39–57.
Clelland CD, Choi M, Romberg C, Clemenson GD, Fragniere A, Tyers P, et al. A functional role for adult hippocampal neurogenesis in spatial pattern separation. Science. 2009;325:210 LP–213.
Snyder JS, Hong NS, McDonald RJ, Wojtowicz JM. A role for adult neurogenesis in spatial long-term memory. Neuroscience. 2005;130:843–52.
Levone BR, Cryan JF, O’Leary OF. Role of adult hippocampal neurogenesis in stress resilience. Neurobiol Stress. 2015;1:147–55.
Snyder JS, Soumier A, Brewer M, Pickel J, Cameron HA. Adult hippocampal neurogenesis buffers stress responses and depressive behaviour. Nature. 2011;476:458–61.
Zhu Y, Gao H, Tong L, Li Z, Wang L, Zhang C, et al. Emotion regulation of hippocampus using real-time fmri neurofeedback in healthy human. Front Hum Neurosci. 2019;13:242.
Lucassen PJ, Oomen CA, Schouten M, Encinas JM, Fitzsimons CP. Chapter 8 - Adult Neurogenesis, Chronic Stress and Depression. In: Canales JJBT-AN in the H, editor. San Diego: Academic Press; 2016. p. 177–206.
Sheline YI, Liston C, McEwen BS. Parsing the hippocampus in depression: chronic stress, hippocampal volume, and major depressive disorder. Biol Psychiatry. 2019;85:436–8.
Lucassen PJ, Fitzsimons CP, Salta E, Maletic-Savatic M. Adult neurogenesis, human after all (again): Classic, optimized, and future approaches. Behav Brain Res. 2020;381:112458.
Cole J, Costafreda SG, McGuffin P, Fu CHY. Hippocampal atrophy in first episode depression: A meta-analysis of magnetic resonance imaging studies. J Affect Disord. 2011;134:483–7.
Boldrini M, Hen R, Underwood MD, Rosoklija GB, Dwork AJ, Mann JJ, et al. Hippocampal angiogenesis and progenitor cell proliferation are increased with antidepressant use in major depression. Biol Psychiatry. 2012;72:562–71.
Powell TR, Murphy T, de Jong S, Lee SH, Tansey KE, Hodgson K, et al. The genome-wide expression effects of escitalopram and its relationship to neurogenesis, hippocampal volume, and antidepressant response. Am J Med Genet Part B Neuropsychiatr Genet. 2017;174:427–34.
Boldrini M, Underwood MD, Hen R, Rosoklija GB, Dwork AJ, John Mann J, et al. Antidepressants increase neural progenitor cells in the human hippocampus. Neuropsychopharmacology. 2009;34:2376–89.
Daftary S, Yon J-M, Choi E-K, Kim Y-B, Bice C, Kulikova A, et al. Microtubule associated protein 2 in bipolar depression: Impact of pregnenolone. J Affect Disord. 2017;218:49–52.
Cobb JA, Simpson J, Mahajan GJ, Overholser JC, Jurjus GJ, Dieter L, et al. Hippocampal volume and total cell numbers in major depressive disorder. J Psychiatr Res. 2013;47:299–306.
Berger T, Lee H, Young AH, Aarsland D, Thuret S. Adult hippocampal neurogenesis in major depressive disorder and Alzheimer’s disease. Trends Mol Med. 2020;26:803–18.
McEwen BS, Nasca C, Gray JD. Stress effects on neuronal structure: hippocampus, amygdala, and prefrontal cortex. Neuropsychopharmacol Publ Am Coll Neuropsychopharmacol. 2016;41:3–23.
McEwen BS. Stress-induced remodeling of hippocampal CA3 pyramidal neurons. Brain Res. 2016;1645:50–4.
Soetanto A, Wilson RS, Talbot K, Un A, Schneider JA, Sobiesk M, et al. Association of anxiety and depression with microtubule-associated protein 2- and synaptopodin-immunolabeled dendrite and spine densities in hippocampal CA3 of older humans. Arch Gen Psychiatry. 2010;67:448–57.
Kang HJ, Voleti B, Hajszan T, Rajkowska G, Stockmeier CA, Licznerski P, et al. Decreased expression of synapse-related genes and loss of synapses in major depressive disorder. Nat Med. 2012;18:1413–7.
Chklovskii DB. Synaptic connectivity and neuronal morphology: two sides of the same coin. Neuron. 2004;43:609–17.
Kelliher MT, Saunders HAJ, Wildonger J. Microtubule control of functional architecture in neurons. Curr Opin Neurobiol. 2019;57:39–45.
Perera TD, Park S, Nemirovskaya Y. Cognitive role of neurogenesis in depression and antidepressant treatment. Neurosci. 2008;14:326–38.
Toda T, Parylak SL, Linker SB, Gage FH. The role of adult hippocampal neurogenesis in brain health and disease. Mol Psychiatry. 2019;24:67–87.
Fritz MS, Mackinnon DP. Required sample size to detect the mediated effect. Psychol Sci. 2007;18:233–9.
Ho NF, Hooker JM, Sahay A, Holt DJ, Roffman JL. In vivo imaging of adult human hippocampal neurogenesis: progress, pitfalls and promise. Mol Psychiatry. 2013;18:404–16.
Czéh B, Lucassen PJ. What causes the hippocampal volume decrease in depression? Eur Arch Psychiatry Clin Neurosci. 2007;257:250–60.
Nogovitsyn N, Muller M, Souza R, Hassel S, Arnott SR, Davis AD, et al. Hippocampal tail volume as a predictive biomarker of antidepressant treatment outcomes in patients with major depressive disorder: a CAN-BIND report. Neuropsychopharmacology. 2020;45:283–91.
Vyas CM, Okereke OI. Late-life depression: a narrative review on risk factors and prevention. Harv Rev Psychiatry. 2020;28:72–99.
Kennis M, Gerritsen L, van Dalen M, Williams A, Cuijpers P, Bockting C. Prospective biomarkers of major depressive disorder: a systematic review and meta-analysis. Mol Psychiatry. 2020;25:321–38.
Rothe N, Steffen J, Penz M, Kirschbaum C, Walther A. Examination of peripheral basal and reactive cortisol levels in major depressive disorder and the burnout syndrome: A systematic review. Neurosci Biobehav Rev. 2020;114:232–70.
Penninx BWJH, Beekman ATF, Bandinelli S, Corsi AM, Bremmer M, Hoogendijk WJ, et al. Late-life depressive symptoms are associated with both hyperactivity and hypoactivity of the hypothalamo-pituitary-adrenal axis. Am J Geriatr Psychiatry. 2007;15:522–9.
Ahmed AT, MahmoudianDehkordi S, Bhattacharyya S, Arnold M, Liu D, Neavin D, et al. Acylcarnitine metabolomic profiles inform clinically-defined major depressive phenotypes. J Affect Disord. 2020;264:90–7.
Walther A, Cannistraci CV, Simons K, Durán C, Gerl MJ, Wehrli S, et al. Lipidomics in major depressive disorder. Front Psychiatry. 2018;9:459.
Sebastião AM, Colino-Oliveira M, Assaife-Lopes N, Dias RB, Ribeiro JA. Lipid rafts, synaptic transmission and plasticity: Impact in age-related neurodegenerative diseases. Neuropharmacology. 2013;64:97–107.
Maffezzini C, Calvo-Garrido J, Wredenberg A, Freyer C. Metabolic regulation of neurodifferentiation in the adult brain. Cell Mol Life Sci. 2020;77:2483–96.
Ferreira GC, McKenna MC. L-carnitine and acetyl-L-carnitine roles and neuroprotection in developing brain. Neurochem Res. 2017;42:1661–75.
Akagawa S, Akagawa Y, Nakai Y, Yamagishi M, Yamanouchi S, Kimata T, et al. Fiber-rich barley increases butyric acid-producing bacteria in the human gut microbiota. Metabolites. 2021;11:559.
Reddan JM, White DJ, Macpherson H, Scholey A, Pipingas A. Glycerophospholipid supplementation as a potential intervention for supporting cerebral structure in older adults. Front Aging Neurosci. 2018;10:49.
Keller U. Nutritional laboratory markers in malnutrition. J Clin Med. 2019;8:775.
Cabrera MAS, Mesas AE, Garcia ARL, de Andrade SM. Malnutrition and depression among community-dwelling elderly people. J Am Med Dir Assoc. 2007;8:582–4.
Vafaei Z, Mokhtari H, Sadooghi Z, Meamar R, Chitsaz A, Moeini M. Malnutrition is associated with depression in rural elderly population. J Res Med Sci. 2013;18:S15–9.
Sanders C, Behrens S, Schwartz S, Wengreen H, Corcoran CD, Lyketsos CG, et al. Nutritional status is associated with faster cognitive decline and worse functional impairment in the progression of dementia: the cache county dementia progression study 1. J Alzheimer’s Dis. 2016;52:33–42.
Orsitto G, Fulvio F, Tria D, Turi V, Venezia A, Manca C. Nutritional status in hospitalized elderly patients with mild cognitive impairment. Clin Nutr. 2009;28:100–2.
Guerrini I, Thomson AD, Gurling HD. The importance of alcohol misuse, malnutrition and genetic susceptibility on brain growth and plasticity. Neurosci Biobehav Rev. 2007;31:212–20.
Ortiz R, Cortés L, Cortés E, Medina H. Malnutrition alters the rates of apoptosis in splenocytes and thymocyte subpopulations of rats. Clin Exp Immunol. 2009;155:96–106.
Rivadeneira DE, Grobmyer SR, Naama HA, Mackrell PJ, Mestre JR, Stapleton PP, et al. Malnutrition-induced macrophage apoptosis. Surgery. 2001;129:617–25.
Dean JM, Lodhi IJ. Structural and functional roles of ether lipids. Protein Cell. 2018;9:196–206.
Ting EY-C, Yang AC, Tsai S-J. Role of interleukin-6 in depressive disorder. Int J Mol Sci. 2020;21:2194.
Mac Giollabhui N, Ng TH, Ellman LM, Alloy LB. The longitudinal associations of inflammatory biomarkers and depression revisited: systematic review, meta-analysis, and meta-regression. Mol Psychiatry. 2021;26:3302–14.
Borsini A, Zunszain PA, Thuret S, Pariante CM. The role of inflammatory cytokines as key modulators of neurogenesis. Trends Neurosci. 2015;38:145–57.
Gemma C, Bachstetter AD. The role of microglia in adult hippocampal neurogenesis. Front Cell Neurosci. 2013;7:1–5.
Troubat R, Barone P, Leman S, Desmidt T, Cressant A, Atanasova B, et al. Neuroinflammation and depression: A review. Eur J Neurosci. 2021;53:151–71.
Cosci F, Mansueto G, Fava GA. Relapse prevention in recurrent major depressive disorder. A comparison of different treatment options based on clinical experience and a critical review of the literature. Int J Psychiatry Clin Pract. 2020:24;1–8.
Voorrips LE, Ravelli AC, Dongelmans PC, Deurenberg P, Van, Staveren WA. A physical activity questionnaire for the elderly. Med Sci Sports Exerc. 1991;23:974–9.
Dupré C, Bongue B, Helmer C, Dartigues JF, Hupin D, Roche F, et al. Physical activity types and risk of dementia in community-dwelling older people: the Three-City cohort. BMC Geriatr. 2020;20:132.
Féart C, Samieri C, Barberger-Gateau P. Mediterranean diet and cognitive function in older adults. Curr Opin Clin Nutr Metab Care. 2010;13:14–18.
Acknowledgements
This project was part of the EU consortium DCogPlast “Diet Cognition and Plasticity” funded by JPI-HDHL (Medical Research Council UK: MR/N030087/1; French National Research Agency ANR-15-HDHL-0002-05; PCIN-2015-229- MINECO; CiberFES- Cofund by FEDER Program from EU, 2017SGR1546 & ICREA 2018 Academia Award from the Generalitat de Catalunya), the BMWFW under BMWFW-10.420/0009-WF/V/3c/2015.
Funding
PJL and AK are supported by Alzheimer Nederland and the NWO Food & Cognition program, PJL is supported by the Urban Mental Health program of the University of Amsterdam. SLA was part of the University Research school (Ecole Universitaire de Recherche, EUR) Digital Public Health PhD program, supported within the framework of the French National Research Agency (ANR) “Programme d’Investissement d’Avenir” (Investment for the Future) PIA3 (17-EURE-0019). The Three-City Study was conducted under a partnership agreement between the Institut National de la Santé et de la Recherche Médicale (INSERM), the Institut de Santé Publique et Développement of the Victor Segalen Bordeaux 2 University and Sanofi-Aventis. The Fondation pour la Recherche Médicale funded the preparation and initiation of the study. The 3C Study was also supported by the Caisse Nationale Maladie des Travailleurs Salariés, Direction Générale de la Santé, Mutuelle Générale de l’Education Nationale, Institut de la Longévité, Regional Governments of Aquitaine and Bourgogne, Fondation de France, Ministry of Research-INSERM Programme “Cohortes et collections de données biologiques”, French National Research Agency COGINUT ANR-06-PNRA-005, the Fondation Plan Alzheimer (FCS 2009–2012), and the Caisse Nationale pour la Solidarité et l’Autonomie (CNSA).
Author information
Authors and Affiliations
Contributions
ADP designed and conceptualised study; data collection; statistical analysis; data interpretation; drafted and revised the manuscript for intellectual content; SFL statistical analysis; data interpretation; revised the manuscript for intellectual content; RGD metabolomic data collection; data interpretation; revised the manuscript for intellectual content; VH, CdL, DYL, CH, CF, CD, CPL, MP, ASP, MUS, SRR, BA, LA, PJL, AK, CM, CAL data interpretation; revised the manuscript for intellectual content; CS statistical analysis; data interpretation; revised the manuscript for intellectual content; ST designed and conceptualised study; statistical analysis; interpreted the data; drafted and revised the manuscript for intellectual content. Correspondence to ST.
Corresponding author
Ethics declarations
Competing interests
All authors declare no potential conflicts of interest with respect to the research, authorship, and/or publication of this article. For the purpose of open access, the author has applied a Creative Commons Attribution (CC BY) licence to any Author Accepted Manuscript version arising.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Du Preez, A., Lefèvre-Arbogast, S., González-Domínguez, R. et al. Impaired hippocampal neurogenesis in vitro is modulated by dietary-related endogenous factors and associated with depression in a longitudinal ageing cohort study. Mol Psychiatry 27, 3425–3440 (2022). https://doi.org/10.1038/s41380-022-01644-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41380-022-01644-1