Preface
Executive functions, learning, attention, and processing speed are imperative facets of cognitive performance, affected in neuropsychiatric disorders. In clinical studies on different patient groups, recombinant human (rh) erythropoietin (EPO) lastingly improved higher cognition and reduced brain matter loss. Correspondingly, rhEPO treatment of young rodents or EPO receptor (EPOR) overexpression in pyramidal neurons caused remarkable and enduring cognitive improvement, together with enhanced hippocampal long-term potentiation. The ‘brain hardware upgrade’, underlying these observations, includes an EPO induced ~20% increase in pyramidal neurons and oligodendrocytes in cornu ammonis hippocampi in the absence of elevated DNA synthesis. In parallel, EPO reduces microglia numbers and dampens their activity and metabolism as prerequisites for undisturbed EPO-driven differentiation of pre-existing local neuronal precursors. These processes depend on neuronal and microglial EPOR. This novel mechanism of powerful postnatal neurogenesis, outside the classical neurogenic niches, and on-demand delivery of new cells, paralleled by dendritic spine increase, let us hypothesize a physiological procognitive role of hypoxia-induced endogenous EPO in brain, which we imitate by rhEPO treatment. Here we delineate the brain EPO circle as working model explaining adaptive ‘brain hardware upgrade’ and improved performance. In this fundamental regulatory circle, neuronal networks, challenged by motor-cognitive tasks, drift into transient ‘functional hypoxia’, thereby triggering neuronal EPO/EPOR expression.
Similar content being viewed by others
The particular situation of contemporary research on erythropoietin
Recombinant human (rh) EPO has been an approved and safe drug for treating renal anemia for meanwhile over 35 years [1,2,3,4,5]. Over the last 25 years, roles of EPO and its receptor, EPOR, in brain became increasingly evident [6, 7], even though the existence of an endogenous brain EPO system has for long time remained a matter of dispute [8]. Explaining the multifaceted brain EPO system, however, will be pivotal to understand adaptive brain mechanisms and develop novel treatment strategies for brain diseases, exploiting both, rhEPO and hypoxia-induced brain EPO. This in turn faces several challenges.
The rhEPO market has always been highly lucrative, but patents expired around 2008. Industry, facing competition by biosimilar producers and fearing off-label use and emergence of new side effects, withdrew essentially all support of research on further rhEPO indications, while funding agencies keep sending applicants for clinical EPO projects to industry. Its name, derived from the original description in erythropoiesis and somewhat misleading for neuroscientists or reviewers, and its negative reputation as doping drug have not helped funding translational research on EPO. This is unfortunate considering that >300 preclinical studies since 1998 showed beneficial effects of high-dose rhEPO in a wide spectrum of brain disease models [6, 7, 9,10,11,12].
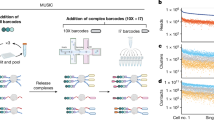
In fact, considerable upregulation of EPO/EPOR in brain occurs for instance upon brain injury [7, 13], which stimulated researchers early to explore the neuroprotective and neuroregenerative potential of this growth factor [9, 14]. Notwithstanding all this evidence, underlying mechanisms have remained widely obscure. Even though research on extra-hematopoietic, direct tissue-protective properties of rhEPO started in the nineties [9, 14,15,16], results were partly controversial [8, 13], owing to lack of necessary tools, e.g., specific antibodies or targeted genetic models. But also the extremely low brain expression of EPO/EPOR poses a huge problem (Fig. 1), with EPO undetectable by e.g., single cell RNA sequencing (scRNA-seq) - a so-called ‘drop-out effect’ across tissues - and EPOR even on ‘strongly expressing’ hematopoietic cells amounting to much less than 1000 molecules per cell [13, 17]. At the same time, this low expression reflects perfectly the incredible potency of this growth factor.
a Unbiased clustering of hippocampal cells from mice under normoxia (n = 2) or hypoxia (n = 2), represented in UMAP space, reveals 16 distinct cell populations across conditions [77]. b The extremely low expression of EPOR in these populations, compared to the abundant expression of renin receptor (c), illustrates the partial ‘dropout effect’ of scRNA-seq for EPOR. We note that EPO is not detectable at all using this method.
Unusual reverse translation in brain EPO research: Human trials first
Following own clinical observations as neurologist and psychiatrist (HE), starting over 30 years ago, and contrary to the usual translational methodologies in neuroscience, we started with investigator-initiated clinical trials on rhEPO already in 1998, including trials in ischemic stroke, multiple sclerosis, schizophrenia, major depression and bipolar disease [18,19,20,21,22,23]. This ‘human trials first’ approach led to the discovery of the highly reproducible neuroprotective and procognitive effects of rhEPO in humans, independent of hematopoiesis. In addition, it documented repeatedly a significant reduction of gray matter loss in brain disease upon rhEPO treatment [24,25,26]. Strikingly, in healthy humans, application of a single high-dose of rhEPO already increased the hippocampal response during memory retrieval [27].
Many effects of rhEPO treatment on cognition, neuroprotection, and neuroregeneration, however, have for a long time been difficult to persuasively separate from rhEPO effects on erythropoiesis/hematocrit. Acute anemia, for instance, affects human brain functions and respective neurophysiological measures like P300, while anemia correction or oxygen breathing results in prompt improvement [28].
Separating EPO effects on brain from hematopoiesis
An elegant study employing either transgenic mice with EPO overexpression exclusively in brain or wildtype mice receiving just one high-dose rhEPO injection showed convincingly that EPO in brain has remarkable effects on exercise performance in absence of any hematocrit changes [29]. This can for instance explain the intriguing brain effects of athletes upon EPO doping, e.g., increased drive and motivation [30]. Even though doping in sports is definitely not reinforced here, it represents one of the most convincing ‘field studies’, supporting the strong and enduring effects of rhEPO on brain performance.
Substantial additional evidence supports that EPO actions in brain are not related to hematopoiesis: (i) There was either no increase in hematocrit or no correlation between such increase and cognition. (ii) The effect on cognition by far outlasted any transient effect on hematocrit [18, 20, 22, 26, 31]. (iii) Even more compellingly, the above-cited study on transgenic EPO expression in brain [29] and (iv) non-hematopoietic EPO analogues [32,33,34,35,36,37] have been further key arguments for EPO actions on brain in absence of blood effects. (v) Moreover, boosted cognition and neuroplasticity of mice expressing constitutively active EPOR in glutamatergic pyramidal neurons [38], but not in GABAergic interneurons [39], suggested a central role of these neurons for EPO effects on cognition, independent of hematopoiesis.
Back-translation of brain EPO research to mice: procognitive effects
With sophisticated higher cognition testing in normal mice, employing the Five Choice Serial Reaction Time Task [40, 41] or visual discrimination tasks in the Touch-Screen based operant system [42], we initiated targeted ‘back-translational’ work. We were able to document faster, more pronounced and lastingly improved attention, learning and memory, together with enhanced hippocampal long-term potentiation upon rhEPO application [43,44,45]. Similar cognitive improvement ensued from experiments using prolylhydroxylase inhibitors for stabilization of hypoxia-inducible factor (HIF). This HIF stabilization, leading to increased EPO expression in brain (and other tissues), provided first hints that endogenous EPO may be sufficient to improve cognition, but did not ultimately prove it, since vascular endothelial growth factor, for instance, also rises upon HIF stabilization [46, 47] and can enhance hippocampal learning and memory [48].
Brain EPO adds a new layer of complexity to postnatal neurogenesis
Some of the neuroprotective and neuroregenerative actions of rhEPO in disease models were speculated to be related to neurogenesis [49,50,51,52], but for a long time, no data were available to support this hypothesis or to discriminate between rhEPO effects on neural progenitor proliferation versus differentiation in postnatal brain [51]. In hematopoiesis, EPO is crucial for antiapoptotic effects on erythroid precursors and for their differentiation rather than for proliferation [53]. We therefore asked whether similar mechanisms apply for the brain. Based on our findings of EPO enhancing cognition and long-term potentiation [43], we initiated our recently published studies on healthy young mice, in which we investigated the effects of three-week administration of rhEPO, starting at the age of four weeks, on brain cell numbers [45, 54]. Entirely unexpected was the discovery that this treatment leads to an around 20% increase in numbers of pyramidal neurons in cornu ammonis (CA), in absence of any respectively altered cell proliferation or apoptosis [45]. Using nanoscopic secondary ion mass spectrometry (NanoSIMS), we found that in rhEPO-treated mice, fed with 15N-leucine diet, an equivalent ~20% of neurons revealed elevated 15N-leucine incorporation, reflecting high de-novo protein synthesis [45]. Under constant cognitive challenge (but not without), the discovered increase in neuron numbers persisted until over six months of age [45]. Reassuringly, the increase in pyramidal neuron numbers and dendritic spines is similarly observed when EPO treatment starts at older age, precluding a purely late developmental phenomenon [54]. We concluded that at any age, EPO most likely drives the differentiation of diverse non-dividing, pre-existing local precursors within neuronal lineages, i.e., in absence of elevated DNA synthesis. Uncovered by serendipity with rhEPO, our observations added a new layer of complexity to postnatal neurogenesis and neuroregeneration where brain expressed EPO appears to play a crucial role in the sense of a ‘neurogenesis fast track’. This novel role of brain EPO is best sketched with a circle including motor-cognitive challenge and ‘functional hypoxia’ (see below; Fig. 2).
Focusing on cornu ammonis (CA) pyramidal neurons, we delineate here a physiological circle of enduring neuroplasticity through enhanced dendritic spine density and swift generation of new functional neurons from diverse precursors without proliferation. Apparently, the entire precursor cell lineage in adult murine CA that is ready to differentiate towards pyramidal neurons remains ‘in flow’. In the proposed neuronal lineage progression, the EPO-responsive progenitor cells and immature neurons may never constitute abundant clusters in a cross-sectional steady-state analysis, but increases rather occur in transient waves with individual neurodifferentiation markers just rising at particular time windows. In this process, neuron-microglia counterbalance plays a pivotal role with both microglial and pyramidal neuronal EPOR being critical for neuronal differentiation upon EPO. Elimination of the pyramidal neuronal EPOR eradicates EPO-driven neurodifferentiation. Strikingly, also upon microglial EPOR deletion, the acceleration by EPO of neuronal differentiation is abolished. We note that the brain EPO circle can be entered anywhere, starting either with mild to moderate inspiratory hypoxia, with rhEPO treatment or with motor-cognitive challenge as inducer of functional hypoxia. Under all these circumstances, brain EPO (and EPOR) emerge as central players of a novel mechanism driving neuronal differentiation and lasting plasticity [54, 77, 105]. Note: In this sketch, the balance symbolizes cell numbers and activity, not weight, i.e., microglia numbers/activity go down while pyramidal neuron numbers go up [105].
Functional hypoxia as part of a novel model of neuroplasticity
Hypoxia is the term for reduced oxygen in cells/tissues, relative to ‘normal’. Earlier interpreted as principally pathological, e.g., upon cardiac arrest, hypoxia is increasingly recognized as strong driver of development including angiogenesis, hematopoiesis, or regeneration [55,56,57,58,59]. In perfect support, quite some literature deals with hypoxic/ischemic preconditioning, where sub-lethal insults induce protection against later fatal injuries by improving tolerance, e.g., through lasting or stand-by activation of hypoxia signaling pathways, anti-apoptosis, anti-excitotoxicity, and autophagy [60]. Noteworthy, hypoxia can be the ultimate consequence of various processes, including lower oxygen availability due to hypoxemia, anemia, perfusion impairment, or increased oxygen consumption (‘functional hypoxia’). Although the mere cellular responses to physiological and pathological hypoxia are similar, they are accompanied by different parallel mechanisms, potentially directing responses towards beneficial effects as observed upon mild to moderate inspiratory hypoxia or functional hypoxia (as discussed in this review) or adverse effects, e.g., occurring upon ischemia or dysregulation of cerebral perfusion [61].
In 2019, W.G. Kaelin, P.J. Ratcliffe & G.L. Semenza jointly received the Nobel Prize in Physiology and Medicine for their discoveries of how cells sense and adapt to oxygen availability [55,56,57,58,59]. The hypoxia-induced transcriptional program is partly independent of [62,63,64] and partly controlled by HIF, binding to hypoxia-responsive elements to modulate gene expression, including EPO [6, 29, 46, 60, 63, 65,66,67,68,69]. This fundamental context, however, has not been systematically translated to normal brain functions, where it likely has a central, yet unheralded role. Extensive physical activity and cognitive challenge lead to widespread brain activation and improved global brain function including mood [70, 71]. Neurologists/psychiatrists encourage patients to improve functions by practicing: ‘Use-it-or-lose-it’. Hippocampal volume increases upon exercise in healthy or schizophrenic subjects, correlating with e.g., improved short-term memory [72]. We hypothesized that activity-induced, ‘functional hypoxia’ of neurons and brain-expressed EPO may play pivotal roles in all these circumstances. But this had still to be proven as detailed below. In perfect agreement with this concept, but without even considering functional hypoxia as the driving force, a recent elegant study on a mouse model of Rett syndrome showed that intensive physical training, beginning in the presymptomatic period, dramatically improves the performance of specific motor and memory tasks, and significantly delays the onset of symptoms. Task-specific neurons that are repeatedly activated during training were found to develop more dendritic arbors and to have better neurophysiological responses than those in untrained mice [73]. Rett syndrome is a progressive neurological disorder in which children develop normally for the first one or two years of life, before experiencing profound motor and cognitive decline. The results of this beautiful work strongly encourage novel therapeutic approaches in Rett syndrome but also in other neurodevelopmental conditions like many forms of intellectual disability or (syndromal) autism, as for instance in fragile X syndrome or SYNGAP mutations [74,75,76]. These novel therapeutic approaches likely build on functional hypoxia as pivotal driving force.
The brain EPO circle explaining adaptive brain hardware upgrade and enhanced performance
With a refined transgenic reporter approach, utilizing the oxygen-dependent degradation (ODD) domain of Hif-1α fused to CreERT2 recombinase, CAG-CreERT2-ODD::R26R-tdTomato mice [77, 78], we provided first clues that complex running wheel (CRW) exposure as voluntary motor-cognitive challenge leads to ‘relative oxygen deficiency’ in hippocampal pyramidal neurons, i.e., initially higher oxygen consumption than delivery, which we coined ‘functional hypoxia’. Figure 3 shows tdTomato+ hypoxic cells in representative mouse brain sections. We also spatially mapped these cells by light-sheet microscopy [77]. This three-dimensional view allowed to demonstrate hypoxia across essentially all brain areas. Amazingly, running on CRW causes hypoxic neurons all over, and particularly abundant in hippocampus. Here, the CRW-induced endogenous hypoxia of pyramidal neurons augments EPO and EPOR expression, as experimentally proven by in situ hybridization [54]. EPO and EPOR in turn prompt via auto/paracrine signaling the emergence of new pyramidal neurons and, in parallel, enhance dendritic spine densities of preexisting neurons. As a result, performance is improved, conveniently referring to ‘EPO brain doping’ [54].
Illustrative coronal brain sections of CAG-CreERT2-ODD::R26R-tdTomato mice under (a) normoxia and (b) voluntary complex running wheel performance (‘functional hypoxia’). Motor-cognitive challenge (over 5 consecutive days with daily tamoxifen injections, 5 in total) induces globally enhanced numbers/intensity of tdTomato+ cells in the brain with particular focus on hippocampus and cortex (pyramidal neurons) [77].
An explanation for the fast appearance of a substantial amount of new mature pyramidal neurons upon EPO in just 3–4 weeks was provided by scRNA-seq in CA1, revealing an increase in newly differentiating neurons already 6 h after a single intraperitoneal rhEPO injection. This means that we see the start of enhanced differentiation already at this early time point, as illustrated by a pseudotime presentation of the trajectory analysis of neuronal cells, performed in Monocle2 [54, 79]. In fact, the increase in the number of differentiating immature neurons starts at 6 h after the first EPO injection with an increase in T-box brain1 (Tbr1) positive neuronal precursors over the placebo condition (Fig. 2). Additional markers that characterize this early responding cluster include doublecortin (Dcx) and transducin-like enhancer family member4 (Tle4). At one week after EPO treatment start, we see an increase in a subsequent differentiation stage (Zbtb20 positive immature neurons). This EPO-induced differentiation flow is ultimately leading after 3–4 weeks to a 20% increase in mature pyramidal neurons with expression of the markers Ctip2/NeuN, while the other transcripts/proteins are no longer increased under EPO but have returned to control/placebo level. This rapid, wave-like drive of neurodifferentiation was similarly observed upon hypoxia-induced expression of EPO in brain. Exposure to moderate inspiratory hypoxia (12% O2) imitated the improved CRW performance as well as the enhanced neuron numbers and dendritic spines upon rhEPO, and inspiratory hypoxia in combination with CRW (add-on endogenous, functional hypoxia) even acted synergistically. All these effects depend on pyramidal neuronal expression of the EPOR gene [54].
Taken together, an intriguing novel model of neuroplasticity emerged, in which specific task-associated neuronal networks drift into transient functional hypoxia as a local as well as a brain-wide response comprising indirectly activated neurons and non-neuronal cells [77, 80]. This in turn triggers neuronal EPO/EPOR expression to mediate neuroplasticity via adaptive transcript regulation in the behaving brain, leading to substantial ‘hardware upgrade’ (Fig. 2).
Effects of pharmacological oxygen manipulations on brain function
We are just starting to understand the role of oxygen manipulations in the brain with respect to effects on brain performance and brain disease. Even though not directly related to the main topic of this perspective, we note that a whole array of different methods on modulating oxygen availability have been described to influence brain functions in health and disease models. Just examples are recent work on hyperbaric oxygen therapy that reported alleviation of vascular dysfunction and amyloid burden in an Alzheimer’s disease mouse model and also in elderly patients [81]. Similarly, intermittent hypoxic–hyperoxic training in geriatric subjects [82] and in patients with mild cognitive impairment [83] showed beneficial effects on cognition. In this context, the endogenous EPO system likely plays an important role. In fact, a coding single nucleotide polymorphism of EPO, the nonsynonymous rare variant SNP rs62483572, was identified to be protective in Alzheimer’s disease [84]. Moreover, human EPO and EPOR gain-of-function genotypes are associated with better cognition [85].
Also upon chronic moderate hyperoxia, increased HIF accumulation and EPO expression in mouse brain have been reported [86], pointing to some overlap in downstream mechanisms of hypoxia and hyperoxia, reflected or mediated e.g., by excess reactive oxygen species (ROS, see below) [87,88,89]. On the other hand, contrasting effects of hypoxia versus hyperoxia were found in a mouse model of Friedreich’s ataxia where breathing of 11% O2 attenuated the progression of ataxia, whereas breathing 55% O2 hastened it [90]. We conclude here, that much work needs to be done to understand respective mechanisms and to further exploit them for the benefit of patients. Overall, however, we should keep in mind, that hyperoxia is never physiological, whereas (functional) hypoxia definitely represents a major driving force of neurodevelopmental processes and adaptive neuroplasticity. Using hypoxia or rhEPO as treatment strategies, we imitate physiology, whereas hyperoxia would constitute some other sort of a pharmacological therapy. Nevertheless, any approach that demonstrates clear benefit in thus far untreatable diseases or syndromes should be considered and encouraged to be pursued. Even in COVID-19, where oxygen treatment depicts a logical and important therapeutic contribution, rhEPO treatment as substitution therapy might help overcome the unexpected ‘hypoxia paradox’ in this condition [91, 92].
Also worth mentioning in this context is the tight regulation between oxidative stress and antioxidants relating to EPO pathways. Strong intermittent hypoxic conditions (nadir of 5% O2), for instance, induce increased ROS production, which activate HIF. Of note, this strong hypoxia may damage parvalbumin-expressing interneurons through ROS accumulation, which apparently can be ameliorated by environmental enrichment [93]. On the other hand, ROS and antioxidants were shown to play a role in neuronal and oligodendroglial differentiation [94,95,96]. Therefore, yet to be elucidated downstream mechanisms of hypoxia and EPO may involve some antioxidant compensation to balance ROS increase and to allow undisturbed cellular differentiation processes.
Delineating the multifaceted and multicellular brain EPO system
Importantly, effects of EPO on cognition and neuroregeneration comprise parallel effects on other cell types. In a mouse model of traumatic brain injury, we saw that early treatment with rhEPO prevented consequences of secondary neurodegeneration, i.e., progressive brain atrophy and cognitive decline [25, 97], reduced the increase in injury-induced microglia and dampened their motility [98, 99]. Reflecting the high - but still poorly understood - complexity of the brain EPO system, also interneurons [39, 100], oligodendrocytes, their precursors (OPC) [45], astrocytes, endothelial cells and pericytes express EPO and EPOR, at least in disease [6, 10], and EPO not only traverses the blood-brain-barrier (BBB), but influences BBB function, immune cell transmigration, angiogenesis, and cerebral blood flow [31, 101,102,103].
In fact, EPO effects on interneurons are still much less clear. EPO treatment decreases the structural complexity of certain interneuronal subpopulations and the density of inhibitory perisomatic puncta that surround pyramidal neurons (Curto et al, manuscript in preparation). In a transgenic mouse line that constitutively overexpresses neuronal EPO from early development on, stimulation of postnatal GABAergic maturation and an elevation of hippocampal GABA-immunoreactive neurons was reported, together with increase in interneurons expressing parvalbumin, somatostatin and neuropeptide Y [100]. Whereas constitutively active EPOR in GABAergic neurons changed hippocampal network properties, cognition was not affected, suggesting that the effect of EPO on cognition is dominated by its effect on the glutamatergic system [39]. Much more work is needed to fully understand the impact of EPO on the inhibitory circuitry.
In EPO-treated NG2-CreERT2 mice, we confirmed enhanced differentiation of pre-existing oligodendrocyte precursors (NG2+), again in absence of elevated DNA synthesis [45]. Completely unexpected was the observation that mice with lack of oligodendroglial EPOR apparently develop a mild dementia phenotype, as demonstrated in our IntelliCage test paradigm [104]. This paradigm allows cognitive, emotional and social phenotyping of mice in an observer-independent setting. The underlying mechanisms of this OPC/oligodendrocyte-related cognitive/intellectual disability are not yet understood and presently subject to extensive study in our laboratory.
An unforeseen involvement of resident microglia started with the discovery that stimulated neurodifferentiation, either by rhEPO, functional or inspiratory hypoxia, goes hand in hand with a decrease in microglia numbers. Obviously, during accelerating neuronal differentiation, EPO acts as regulator of the CSF1R-dependent microglia. Here, neuronally expressed IL-34 and microglial CSF1R are instrumental [105]. Surprisingly, EPO affects microglia in phases, initially by inducing apoptosis, later by reducing proliferation, and overall dampens microglia activity and metabolism, as verified by selective genetic targeting of either microglial or pyramidal neuronal EPOR. It turned out that EPOR on both cell types are critical for neuronal differentiation in CA upon EPO [105]. We note that the EPO effects on microglia are opposite to the effects on most other cell types, where this potent growth factor rather acts in a strong antiapoptotic fashion, enhances energy metabolism, and drives proliferation and/or differentiation. The deeper delineation of these contrasting cellular responses to the same ligand requires further study and may involve different EPORs or different EPOR properties as well as diverse downstream intracellular signaling.
Conclusions and outlook
In summary, powerful, hematopoiesis-independent effects of rhEPO on neuroprotection, neuroregeneration and cognition in humans and rodents suggest that endogenous EPO in brain serves fundamental, previously overlooked physiological functions. The here introduced brain EPO circle explains as convenient working model the adaptive ‘brain hardware upgrade’ and enhanced performance upon rhEPO or brain EPO induction by hypoxia. In this fundamental regulatory circle, neuronal networks when challenged by motor-cognitive tasks, drift into transient ‘functional hypoxia’, thereby triggering neuronal EPO and EPOR expression (Fig. 2).
In other words, strong motor-cognitive exercise leads to neuronal activation and functional hypoxia, inducing HIF activation, followed by EPO transcription (among other transcripts) in pyramidal neurons, which in turn grow more dendritic spines and simultaneously stimulate their neighboring cells, ready to become neurons, to differentiate within the hippocampus. All this then contributes to cognitive improvement. We note, however, that the brain EPO circle can be entered anywhere, starting either with mild to moderate inspiratory hypoxia, with rhEPO treatment or with the aforementioned motor-cognitive challenge as inducer of functional hypoxia, leaving plenty of possible ways for future therapeutic interventions.
Remarkably, the bigger picture of the brain EPO system is still missing to date, despite supporting hints of hypoxia influencing cognition and of hypoxia-induced EPO [6, 7, 10]. All these hints are first fragments of a still concealed mosaic. Physiological conditions of brain EPO/EPOR expression, function and interplay of the different brain cell types with respect to the brain EPO system have remained widely unexplored. Published work on putatively different types of EPOR in brain is fragmentary and contradictory [106, 107]. Targeting EPO and hypoxia, the critical components of the here delineated regulatory brain circle, may yield promising innovative treatment approaches to neuropsychiatric diseases. But admittedly, for complete mechanistic understanding, much work still remains to be done.
References
Jelkmann W. Erythropoietin research, 80 years after the initial studies by Carnot and Deflandre. Respir Physiol. 1986;63:257–66.
Lodish HF. Translational control of protein synthesis: the early years. J Biol Chem. 2012;287:36528–35.
Lodish HF, Hilton DJ, Klingmüller U, Watowich SS, Wu H. The erythropoietin receptor: biogenesis, dimerization, and intracellular signal transduction. Cold Spring Harb Symp Quant Biol. 1995;60:93–104. https://doi.org/10.1101/sqb.1995.060.01.012.
Graber SE, Krantz S. Erythropoietin and the control of red cell production. Annu Rev Med. 1978;29:51–66.
Bauer C, Kurtz A. Oxygen sensing in the kidney and its relation to erythropoietin production. Annu Rev Physiol. 1989;51:845–56.
Brines M, Cerami A. Emerging biological roles for erythropoietin in the nervous system. Nat Rev Neurosci. 2005;6:484–94.
Sirén A-L, Faßhauer T, Bartels C, Ehrenreich H. Therapeutic potential of erythropoietin and its structural or functional variants in the nervous system. Neurotherapeutics. 2009;6:108–27.
Ghezzi P, Bernaudin M, Bianchi R, Blomgren K. Erythropoietin: not just about erythropoiesis (vol 375, pg 2142, 2010). Lancet. 2010;376:418–418.
Brines ML, Ghezzi P, Keenan S, Agnello D, De Lanerolle NC, Cerami C, et al. Erythropoietin crosses the blood–brain barrier to protect against experimental brain injury. Proc Natl Acad Sci. 2000;97:10526–31.
Sargin D, Friedrichs H, El-Kordi A, Ehrenreich H. Erythropoietin as neuroprotective and neuroregenerative treatment strategy: comprehensive overview of 12 years of preclinical and clinical research. Best Pract Res Clin Anaesthesiol. 2010;24:573–94.
Newton SS, Sathyanesan M. Erythropoietin and non-erythropoietic derivatives in cognition. Front Pharmacol. 2021;12:728725.
Dey S, Lee J, Noguchi CT. Erythropoietin non-hematopoietic tissue response and regulation of metabolism during diet induced obesity. Front Pharmacol. 2021;12:725734.
Ott C, Martens H, Hassouna I, Oliveira B, Erck C, Zafeiriou M-P, et al. Widespread expression of erythropoietin receptor in brain and its induction by injury. Mol Med. 2015;21:803–15.
Sakanaka M, Wen T-C, Matsuda S, Masuda S, Morishita E, Nagao M, et al. In vivo evidence that erythropoietin protects neurons from ischemic damage. Proc Natl Acad Sci. 1998;95:4635–40.
Juul SE, Anderson DK, Li Y, Christensen RD. Erythropoietin and erythropoietin receptor in the developing human central nervous system. Pediatr Res. 1998;43:40–49.
Marti HH, Wenger RH, Rivas LA, Straumann U, Oigicaylioglu M, Henn V, et al. Erythropoietin gene expression in human, monkey and murine brain. Eur J Neurosci. 1996;8:666–76.
Um M, Gross AW, Lodish HF. A “classical” homodimeric erythropoietin receptor is essential for the antiapoptotic effects of erythropoietin on differentiated neuroblastoma SH-SY5Y and pheochromocytoma PC-12 cells. Cell Signal. 2007;19:634–45.
Ehrenreich H, Fischer B, Norra C, Schellenberger F, Stender N, Stiefel M, et al. Exploring recombinant human erythropoietin in chronic progressive multiple sclerosis. Brain. 2007;130:2577–88.
Ehrenreich H, Hasselblatt M, Dembowski C, Cepek L, Lewczuk P, Stiefel M, et al. Erythropoietin therapy for acute stroke is both safe and beneficial. Mol Med. 2002;8:495–505.
Ehrenreich H, Hinze-Selch D, Stawicki S, Aust C, Knolle-Veentjer S, Wilms S, et al. Improvement of cognitive functions in chronic schizophrenic patients by recombinant human erythropoietin. Mol Psychiatry. 2007;12:206–20.
Ehrenreich H, Weissenborn K, Prange H, Schneider D, Weimar C, Wartenberg K, et al. Recombinant human erythropoietin in the treatment of acute ischemic stroke. Stroke. 2009;40:e647–e656.
Miskowiak KW, Ehrenreich H, Christensen EM, Kessing LV, Vinberg M. Recombinant human erythropoietin to target cognitive dysfunction in bipolar disorder: a double-blind, randomized, placebo-controlled phase 2 trial. J Clin psychiatry. 2014;75:0–0.
Miskowiak KW, Vinberg M, Christensen EM, Bukh JD, Harmer CJ, Ehrenreich H, et al. Recombinant human erythropoietin for treating treatment-resistant depression: a double-blind, randomized, placebo-controlled phase 2 trial. Neuropsychopharmacology. 2014;39:1399–408.
Miskowiak KW, Vinberg M, Macoveanu J, Ehrenreich H, Køster N, Inkster B, et al. Effects of erythropoietin on hippocampal volume and memory in mood disorders. Biol Psychiatry. 2015;78:270–7.
Sirén A-L, Radyushkin K, Boretius S, Kämmer D, Riechers C-C, Natt O, et al. Global brain atrophy after unilateral parietal lesion and its prevention by erythropoietin. Brain. 2006;129:480–9.
Wüstenberg T, Begemann M, Bartels C, Gefeller O, Stawicki S, Hinze-Selch D, et al. Recombinant human erythropoietin delays loss of gray matter in chronic schizophrenia. Mol Psychiatry. 2011;16:26–36.
Miskowiak K, O’Sullivan U, Harmer CJ. Erythropoietin enhances hippocampal response during memory retrieval in humans. J Neurosci. 2007;27:2788–92.
Weiskopf RB, Toy P, Hopf HW, Feiner J, Finlay HE, Takahashi M, et al. Acute isovolemic anemia impairs central processing as determined by P300 latency. Clin Neurophysiol. 2005;116:1028–32.
Schuler B, Vogel J, Grenacher B, Jacobs RA, Arras M, Gassmann M. Acute and chronic elevation of erythropoietin in the brain improves exercise performance in mice without inducing erythropoiesis. FASEB J. 2012;26:3884–90.
Ninot G, Connes P, Caillaud C. Effects of recombinant human erythropoietin injections on physical self in endurance athletes. J Sports Sci. 2006;24:383–91.
Ehrenreich H, Degner D, Meller J, Brines M, Behe M, Hasselblatt M, et al. Erythropoietin: a candidate compound for neuroprotection in schizophrenia. Mol Psychiatry. 2004;9:42–54.
Bürgi M, Aparicio GI, Dorella A, Kratje R, Scorticati C, Oggero M. Novel erythropoietin‐based therapeutic candidates with extra N‐glycan sites that block hematopoiesis but preserve neuroplasticity. Biotechnol J. 2021;16:2000455.
Brines M, Patel NS, Villa P, Brines C, Mennini T, De Paola M, et al. Nonerythropoietic, tissue-protective peptides derived from the tertiary structure of erythropoietin. Proc Natl Acad Sci. 2008;105:10925–30.
Bonnas C, Wüstefeld L, Winkler D, Kronstein-Wiedemann R, Dere E, Specht K, et al. EV-3, an endogenous human erythropoietin isoform with distinct functional relevance. Sci Rep. 2017;7:1–15.
Pankratova S, Kiryushko D, Sonn K, Soroka V, Køhler LB, Rathje M, et al. Neuroprotective properties of a novel, non-haematopoietic agonist of the erythropoietin receptor. Brain. 2010;133:2281–94.
Ehrenreich H. A boost for translational neuroscience. Science. 2004;305:184–5.
Leist M, Ghezzi P, Grasso G, Bianchi R, Villa P, Fratelli M, et al. Derivatives of erythropoietin that are tissue protective but not erythropoietic. Science. 2004;305:239–42.
Sargin D, El-Kordi A, Agarwal A, Müller M, Wojcik SM, Hassouna I, et al. Expression of constitutively active erythropoietin receptor in pyramidal neurons of cortex and hippocampus boosts higher cognitive functions in mice. BMC Biol. 2011;9:1–16.
Wüstefeld L, Winkler D, Janc OA, Hassouna I, Ronnenberg A, Ostmeier K, et al. Selective expression of a constitutively active erythropoietin receptor in GABA ergic neurons alters hippocampal network properties without affecting cognition. J Neurochem. 2016;136:698–705.
Carli M, Robbins T, Evenden J, Everitt B. Effects of lesions to ascending noradrenergic neurones on performance of a 5-choice serial reaction task in rats; implications for theories of dorsal noradrenergic bundle function based on selective attention and arousal. Behav Brain Res. 1983;9:361–80.
Humby T, Wilkinson L, Dawson G. Assaying aspects of attention and impulse control in mice using the 5‐choice serial reaction time task. Curr Protoc Neurosci. 2005;31:1–15.
Izquierdo A, Wiedholz LM, Millstein RA, Yang RJ, Bussey TJ, Saksida LM, et al. Genetic and dopaminergic modulation of reversal learning in a touchscreen-based operant procedure for mice. Behav Brain Res. 2006;171:181–8.
Adamcio B, Sargin D, Stradomska A, Medrihan L, Gertler C, Theis F, et al. Erythropoietin enhances hippocampal long-term potentiation and memory. BMC Biol. 2008;6:1–16.
El-Kordi A, Radyushkin K, Ehrenreich H. Erythropoietin improves operant conditioning and stability of cognitive performance in mice. BMC Biol. 2009;7:1–8.
Hassouna I, Ott C, Wüstefeld L, Offen N, Neher RA, Mitkovski M, et al. Revisiting adult neurogenesis and the role of erythropoietin for neuronal and oligodendroglial differentiation in the hippocampus. Mol Psychiatry. 2016;21:1752–67.
Adamcio B, Sperling S, Hagemeyer N, Walkinshaw G, Ehrenreich H. Hypoxia inducible factor stabilization leads to lasting improvement of hippocampal memory in healthy mice. Behav Brain Res. 2010;208:80–84.
Wenger RH, Gassmann M. Oxygen (es) and the hypoxia-inducible factor-1. Biol Chem. 1997;378:609–16.
Cao L, Jiao X, Zuzga DS, Liu Y, Fong DM, Young D, et al. VEGF links hippocampal activity with neurogenesis, learning and memory. Nat Genet. 2004;36:827–35.
Leconte C, Bihel E, Lepelletier F-X, Bouët V, Saulnier R, Petit E, et al. Comparison of the effects of erythropoietin and its carbamylated derivative on behaviour and hippocampal neurogenesis in mice. Neuropharmacology. 2011;60:354–64.
Ransome MI, Turnley AM. Systemically delivered Erythropoietin transiently enhances adult hippocampal neurogenesis. J Neurochem. 2007;102:1953–65.
Shingo T, Sorokan ST, Shimazaki T, Weiss S. Erythropoietin regulates the in vitro and in vivo production of neuronal progenitors by mammalian forebrain neural stem cells. J Neurosci. 2001;21:9733–43.
Tsai PT, Ohab JJ, Kertesz N, Groszer M, Matter C, Gao J, et al. A critical role of erythropoietin receptor in neurogenesis and post-stroke recovery. J Neurosci. 2006;26:1269–74.
Hattangadi SM, Wong P, Zhang L, Flygare J, Lodish HF. From stem cell to red cell: regulation of erythropoiesis at multiple levels by multiple proteins, RNAs, and chromatin modifications. Blood J Am Soc Hematol. 2011;118:6258–68.
Wakhloo D, Scharkowski F, Curto Y, Butt UJ, Bansal V, Steixner-Kumar AA, et al. Functional hypoxia drives neuroplasticity and neurogenesis via brain erythropoietin. Nat Commun. 2020;11:1–12.
Ivashkiv LB. The hypoxia–lactate axis tempers inflammation. Nat Rev Immunol. 2020;20:85–86.
Kullmann JA, Trivedi N, Howell D, Laumonnerie C, Nguyen V, Banerjee SS, et al. Oxygen tension and the VHL-Hif1α pathway determine onset of neuronal polarization and cerebellar germinal zone exit. Neuron. 2020;106:607–23. e605.
Kaelin WG Jr, Ratcliffe PJ. Oxygen sensing by metazoans: the central role of the HIF hydroxylase pathway. Mol Cell. 2008;30:393–402.
Ratcliffe PJ. Oxygen sensing and hypoxia signalling pathways in animals: the implications of physiology for cancer. J Physiol. 2013;591:2027–42.
Semenza GL. Targeting HIF-1 for cancer therapy. Nat Rev Cancer. 2003;3:721–32.
Liu J, Gu Y, Guo M, Ji X. Neuroprotective effects and mechanisms of ischemic/hypoxic preconditioning on neurological diseases. CNS Neurosci Ther. 2021;27:869–82.
Marmarelis VZ, Shin DC, Zhang R. The dynamic relationship between cortical oxygenation and endtidal CO2 transient changes is impaired in MCI patients. Front Physiol. 2021;12:772456.
Jain IH, Calvo SE, Markhard AL, Skinner OS, To T-L, Ast T, et al. Genetic screen for cell fitness in high or low oxygen highlights mitochondrial and lipid metabolism. Cell. 2020;181:716–27. e711.
Lee P, Chandel NS, Simon MC. Cellular adaptation to hypoxia through hypoxia inducible factors and beyond. Nat Rev Mol cell Biol. 2020;21:268–83.
Yuen TJ, Silbereis JC, Griveau A, Chang SM, Daneman R, Fancy SP, et al. Oligodendrocyte-encoded HIF function couples postnatal myelination and white matter angiogenesis. Cell. 2014;158:383–96.
Jelkmann W. Erythropoietin: structure, control of production, and function. Physiol Rev. 1992;72:449–89.
Kenneth NS, Rocha S. Regulation of gene expression by hypoxia. Biochem J. 2008;414:19–29.
Marti HH. Erythropoietin and the hypoxic brain. J Exp Biol. 2004;207:3233–42.
Suresh S, Rajvanshi PK, Noguchi CT. The many facets of erythropoietin physiologic and metabolic response. Front Physiol. 2020;10:1534.
Lewczuk P, Hasselblatt M, Kamrowski-Kruck H, Heyer A, Unzicker C, Sirén A-L, et al. Survival of hippocampal neurons in culture upon hypoxia: effect of erythropoietin. Neuroreport. 2000;11:3485–8.
Kramer AF, Erickson KI. Capitalizing on cortical plasticity: influence of physical activity on cognition and brain function. Trends Cogn Sci. 2007;11:342–8.
Erickson KI, Hillman CH, Kramer AF. Physical activity, brain, and cognition. Curr Opin Behav Sci. 2015;4:27–32.
Pajonk F-G, Wobrock T, Gruber O, Scherk H, Berner D, Kaizl I, et al. Hippocampal plasticity in response to exercise in schizophrenia. Arch Gen Psychiatry. 2010;67:133–43.
Achilly NP, Wang W, Zoghbi HY. Presymptomatic training mitigates functional deficits in a mouse model of Rett syndrome. Nature. 2021;592:596–600.
Agarwal M, Johnston MV, Stafstrom CE. SYNGAP1 mutations: Clinical, genetic, and pathophysiological features. Int J Dev Neurosci. 2019;78:65–76.
Gamache TR, Araki Y, Huganir RL. Twenty years of SynGAP research: from synapses to cognition. J Neurosci. 2020;40:1596–605.
Garber KB, Visootsak J, Warren ST. Fragile X syndrome. Eur J Hum Genet. 2008;16:666–72.
Butt UJ, Steixner-Kumar AA, Depp C, Sun T, Hassouna I, Wüstefeld L, et al. Hippocampal neurons respond to brain activity with functional hypoxia. Mol Psychiatry 2021:1–18.
Kimura W, Xiao F, Canseco DC, Muralidhar S, Thet S, Zhang HM, et al. Hypoxia fate mapping identifies cycling cardiomyocytes in the adult heart. Nature. 2015;523:226–30.
Qiu X, Mao Q, Tang Y, Wang L, Chawla R, Pliner HA, et al. Reversed graph embedding resolves complex single-cell trajectories. Nat methods. 2017;14:979–82.
Butt UJ, Hassouna I, Fernandez Garcia-Agudo L, Steixner-Kumar AA, Depp C, Barnkothe N, et al. CaMKIIα Expressing Neurons to Report Activity-Related Endogenous Hypoxia upon Motor-Cognitive Challenge. Int J Mol Sci. 2021;22:3164.
Shapira R, Gdalyahu A, Gottfried I, Sasson E, Hadanny A, Efrati S, et al. Hyperbaric oxygen therapy alleviates vascular dysfunction and amyloid burden in an Alzheimer’s disease mouse model and in elderly patients. Aging (Albany N. Y). 2021;13:20935.
Bayer U, Likar R, Pinter G, Stettner H, Demschar S, Trummer B, et al. Intermittent hypoxic–hyperoxic training on cognitive performance in geriatric patients. Alzheimer’s Dement Transl Res Clin Interventions. 2017;3:114–22.
Serebrovska ZO, Serebrovska TV, Kholin VA, Tumanovska LV, Shysh AM, Pashevin DA, et al. Intermittent hypoxia-hyperoxia training improves cognitive function and decreases circulating biomarkers of Alzheimer’s disease in patients with mild cognitive impairment: a pilot study. Int J Mol Sci. 2019;20:5405.
Katsumata Y, Nelson PT, Estus S, Fardo DW. Initiative AsDN. Translating Alzheimer’s disease–associated polymorphisms into functional candidates: a survey of IGAP genes and SNPs. Neurobiol Aging. 2019;74:135–46.
Kästner A, Grube S, El-Kordi A, Stepniak B, Friedrichs H, Sargin D, et al. Common variants of the genes encoding erythropoietin and its receptor modulate cognitive performance in schizophrenia. Mol Med. 2012;18:1029–40.
Benderro GF, Sun X, Kuang Y, LaManna JC. Decreased VEGF expression and microvascular density, but increased HIF-1 and 2α accumulation and EPO expression in chronic moderate hyperoxia in the mouse brain. Brain Res. 2012;1471:46–55.
Guzy RD, Schumacker PT. Oxygen sensing by mitochondria at complex III: the paradox of increased reactive oxygen species during hypoxia. Exp Physiol. 2006;91:807–19.
Semenza GL. Life with oxygen. Science. 2007;318:62–64.
Hadanny A, Efrati S. The hyperoxic-hypoxic paradox. Biomolecules. 2020;10:958.
Ast T, Meisel JD, Patra S, Wang H, Grange RM, Kim SH, et al. Hypoxia rescues frataxin loss by restoring iron sulfur cluster biogenesis. Cell. 2019;177:1507–21. e1516.
Begemann M, Gross O, Wincewicz D, Hardeland R, Daguano Gastaldi V, Vieta E, et al. Addressing the ‘hypoxia paradox’ in severe COVID-19: literature review and report of four cases treated with erythropoietin analogues. Mol Med. 2021;27:1–11.
Ehrenreich H, Weissenborn K, Begemann M, Busch M, Vieta E, Miskowiak KW. Erythropoietin as candidate for supportive treatment of severe COVID-19. Mol Med. 2020;26:1–9.
Zhang M, Wu J, Huo L, Luo L, Song X, Fan F, et al. Environmental enrichment prevent the juvenile hypoxia-induced developmental loss of parvalbumin-immunoreactive cells in the prefrontal cortex and neurobehavioral alterations through inhibition of NADPH oxidase-2-derived oxidative stress. Mol Neurobiol. 2016;53:7341–50.
Le Belle JE, Orozco NM, Paucar AA, Saxe JP, Mottahedeh J, Pyle AD, et al. Proliferative neural stem cells have high endogenous ROS levels that regulate self-renewal and neurogenesis in a PI3K/Akt-dependant manner. cell stem cell. 2011;8:59–71.
Monin A, Baumann P, Griffa A, Xin L, Mekle R, Fournier M, et al. Glutathione deficit impairs myelin maturation: relevance for white matter integrity in schizophrenia patients. Mol Psychiatry. 2015;20:827–38.
Ostrakhovitch E, Semenikhin O. The role of redox environment in neurogenic development. Arch Biochem Biophys. 2013;534:44–54.
Sargin D, Hassouna I, Sperling S, Sirén AL, Ehrenreich H. Uncoupling of neurodegeneration and gliosis in a murine model of juvenile cortical lesion. Glia. 2009;57:693–702.
Mitkovski M, Dahm L, Heinrich R, Monnheimer M, Gerhart S, Stegmüller J, et al. Erythropoietin dampens injury-induced microglial motility. J Cereb Blood Flow Metab. 2015;35:1233–6.
Poggi G, Boretius S, Möbius W, Moschny N, Baudewig J, Ruhwedel T, et al. Cortical network dysfunction caused by a subtle defect of myelination. Glia. 2016;64:2025–40.
Khalid K, Frei J, Aboouf MA, Koester-Hegmann C, Gassmann M, Fritschy J-M, et al. Erythropoietin stimulates GABAergic maturation in the mouse hippocampus. Eneuro. 2021;8:1–20.
Castillo‐Gomez E, Kästner A, Steiner J, Schneider A, Hettling B, Poggi G, et al. The brain as immunoprecipitator of serum autoantibodies against N‐Methyl‐D‐aspartate receptor subunit NR1. Ann Neurol. 2016;79:144–51.
Hammer C, Stepniak B, Schneider A, Papiol S, Tantra M, Begemann M, et al. Neuropsychiatric disease relevance of circulating anti-NMDA receptor autoantibodies depends on blood–brain barrier integrity. Mol Psychiatry. 2014;19:1143–9.
Montagne A, Barnes SR, Sweeney MD, Halliday MR, Sagare AP, Zhao Z, et al. Blood-brain barrier breakdown in the aging human hippocampus. Neuron. 2015;85:296–302.
Dere E, Ronnenberg A, Tampe B, Arinrad S, Schmidt M, Zeisberg E, et al. Cognitive, emotional and social phenotyping of mice in an observer-independent setting. Neurobiol Learn Mem. 2018;150:136–50.
Garcia-Agudo LF, Steixner-Kumar AA, Curto Y, Barnkothe N, Hassouna I, Jähne S, et al. Brain erythropoietin fine-tunes a counterbalance between neurodifferentiation and microglia in the adult hippocampus. Cell Rep. 2021;36:109548.
Brines M, Grasso G, Fiordaliso F, Sfacteria A, Ghezzi P, Fratelli M, et al. Erythropoietin mediates tissue protection through an erythropoietin and common β-subunit heteroreceptor. Proc Natl Acad Sci. 2004;101:14907–12.
Sanchez PE, Navarro FP, Fares RP, Nadam J, Georges B, Moulin C, et al. Erythropoietin receptor expression is concordant with erythropoietin but not with common β chain expression in the rat brain throughout the life span. J Comp Neurol. 2009;514:403–14.
Acknowledgements
The authors are grateful to Prof. Klaus-Armin Nave, MPIEM (now MPI-NAT), for his constant support and encouragement over the past 20 years. This work was continuously funded by the Max Planck Society, the Deutsche Forschungsgemeinschaft (DFG, German Research Foundation), including the DFG Research Center for Nanoscale Microscopy & Molecular Physiology of the Brain (CNMPB) and the TRR 274/1 2020 - 408885537.
Funding
Open Access funding enabled and organized by Projekt DEAL.
Author information
Authors and Affiliations
Contributions
Concept, design and drafting manuscript: HE Drafting display items: HE, LF, AAS, JBHW and UJB. All authors read and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Ehrenreich, H., Garcia-Agudo, L.F., Steixner-Kumar, A.A. et al. Introducing the brain erythropoietin circle to explain adaptive brain hardware upgrade and improved performance. Mol Psychiatry 27, 2372–2379 (2022). https://doi.org/10.1038/s41380-022-01551-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41380-022-01551-5
This article is cited by
-
Erythropoietin restrains the inhibitory potential of interneurons in the mouse hippocampus
Molecular Psychiatry (2024)
-
EPO regulates neuronal differentiation of adult human neural-crest derived stem cells in a sex-specific manner
BMC Neuroscience (2023)
-
Erythropoietin re-wires cognition-associated transcriptional networks
Nature Communications (2023)