Abstract
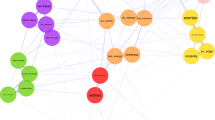
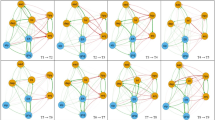
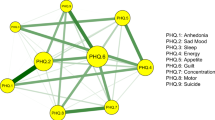
The network theory conceptualizes mental disorders as complex networks of symptoms influencing each other by creating feedback loops, leading to a self-sustained syndromic constellation. Symptoms central to the network have the greatest impact in sustaining the rest of symptoms. This analysis focused on the network structure of depressive symptoms in late-life because of their distinct etiologic factors, clinical presentation, and outcomes. We analyzed cross-sectional data from wave 2 of the 19 country Survey of Health, Ageing, and Retirement in Europe (SHARE) and included non-institutionalized adults aged 65 years or older (mean age 74 years, 59% females) endorsing at least one depressive symptom on the EURO-D scale for depression (N =8,557). We characterized the network structure of depressive symptoms in late-life and used indices of “strength”, “betweenness”, and “closeness” to identify symptoms central to the network. We used a case-dropping bootstrap procedure to assess network stability. Death wishes, depressed mood, loss of interest, and pessimism had the highest values of centrality. Insomnia, fatigue and appetite changes had lower centrality values. The identified network remained stable after dropping 74.5% of the sample. Sex or age did not significantly influence the network structure. In conclusion, death wishes, depressed mood, loss of interest, and pessimism constitute the “backbone” that sustains depressive symptoms in late-life. Symptoms central to the network of depressive symptoms may be used as targets for novel, focused interventions and in studies investigating neurobiological processes central to late-life depression.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Alexopoulos GS. Depression in the elderly. Lancet. 2005.;365:1961–70.
Kok RM, Reynolds CF. Management of depression in older adults. JAMA. 2017;317:2114.
Borsboom D. A network theory of mental disorders. World Psychiatry. 2017;16:5–13.
Cramer AO, van Borkulo CD, Giltay EJ, van der Maas HL, Kendler KS, Scheffer M, et al. Major depression as a complex dynamic system. PLoS ONE. 2016;11:e0167490.
Van Borkulo CD, Borsboom D, Epskamp S, Blanken TF, Boschloo L, Schoevers RA et al. A new method for constructing networks from binary data. Sci Rep. 2014;4. https://doi.org/10.1038/srep05918.
Borsboom D, Cramer AOJ. Network analysis: an integrative approach to the structure of psychopathology. Annu Rev Clin Psychol. 2013;9:91–121.
Epskamp S, Kruis J, Marsman M. Estimating psychopathological networks: Be careful what you wish for. PLoS ONE. 2017;12:e0179891. https://doi.org/10.1371/journal.pone.0179891.
Fried EI, Bockting C, Arjadi R, Borsboom D, Amshoff M, Cramer AOJ, et al. From loss to loneliness: The relationship between bereavement and depressive symptoms. J Abnorm Psychol. 2015;124:256–65.
Cramer AO, Waldorp LJ, van der Maas HL, Borsboom D. Comorbidity: a network perspective. BehavBrain Sci. 2010;33:137–50.
Cramer AO, Borsboom D, Aggen SH, Kendler KS. The pathoplasticity of dysphoric episodes: differential impact of stressful life events on the pattern of depressive symptom inter-correlations. Psychol Med. 2012;42:957–65.
Van Borkulo C, Boschloo L, Borsboom D, Penninx BWJH, Lourens JW, Schoevers RA. Association of symptom network structure with the course of longitudinal depression. JAMA Psychiatry. 2015;72:1219–26.
Snippe E, Viechtbauer W, Geschwind N, Klippel A, de Jonge P, Wichers M. The impact of treatments for depression on the dynamic network structure of mental states: two randomized controlled trials. Sci Rep. 2017;7:46523.
Boschloo L, Van Borkulo CD, Borsboom D, Schoevers RA. A prospective study on how symptoms in a network predict the onset of depression. Psychother Psychosom. 2016;85:183–4.
Naismith SL, Norrie LM, Mowszowski L, Hickie IB. The neurobiology of depression in later-life: clinical, neuropsychological, neuroimaging and pathophysiological features. ProgNeurobiol. 2012;98:99–143.
Alexopoulos GS, Hoptman MJ, Kanellopoulos D, Murphy CF, Lim KO, Gunning FM. Functional connectivity in the cognitive control network and the default mode network in late-life depression. J Affect Disord. 2012;139:56–65.
Alexopoulos GS, Arean P. A model for streamlining psychotherapy in the RDoC era: The example of ‘Engage’. Mol Psychiatry. 2014;19:14–19.
van Agtmaal MJM, Houben AJHM, Pouwer F, Stehouwer CDA, Schram MT. Association of Microvascular Dysfunction With Late-Life Depression: A Systematic Review and Meta-analysis. JAMA Psychiatry. 2017;74:729–39.
Taylor WD, Aizenstein HJ, Alexopoulos GS. The vascular depression hypothesis: mechanisms linking vascular disease with depression. Mol Psychiatry. 2013;18:963–74.
Alexopoulos GS, Morimoto SS. The inflammation hypothesis in geriatric depression. Int J Geriatr Psychiatry. 2011;26:1109–18.
Schaakxs R, Comijs HC, Lamers F, Beekman AT, Penninx BW. Age-related variability in the presentation of symptoms of major depressive disorder. Psychol Med. 2017;47:543–52.
Hegeman JM, Kok RM, van der Mast RC, Giltay EJ. Phenomenology of depression in older compared with younger adults: meta-analysis. Br J Psychiatry. 2012;200:275–81.
Fried EI, Nesse RM. Depression sum-scores don’t add up: Why analyzing specific depression symptoms is essential. BMC Med. 2015;13. https://doi.org/10.1186/s12916-015-0325-4.
Börsch-Supan A, Brandt M, Hunkler C, Kneip T, Korbmacher J, Malter F, et al. Data resource profile: The survey of health, ageing and retirement in Europe (share). Int J Epidemiol. 2013;42:992–1001.
Borsch-Supan A, Brugiavini A, Jorges H, Kapteyn A, Mackenbach J, Siegrist. et al. First results from the Survey of Health, Ageing and Retirement in Europe (2004–7). Starting the Longitudinal Dimension. Mannheim: Mannheim Research Institute for the Economics of Aging (MEA); 2008. http://www.share-project.org/fileadmin/pdf_documentation/FRB2/Table_of_contents.pdf.
Börsch-Supan. A survey of health, ageing and retirement in Europe (SHARE) Wave 2. 2016 Release version: 5.0.0. https://doi.org/10.6103/SHARE.w2.500.
Nelson B, McGorry PD, Wichers M, Wigman JTW, Hartmann JA. Moving from static to dynamic models of the onset of mental disorder: a review. JAMA Psychiatry. 2017;74:528–34.
Meeks TW, Vahia IV, Lavretsky H, Kulkarni G, Jeste DV. A tune in ‘a minor’ can ‘b major’: A review of epidemiology, illness course, and public health implications of subthreshold depression in older adults. J Affect Disord. 2011;129:126–42.
Kennedy GJ, Ceïde ME. Screening older adults for mental disorders. Clin Geriatr Med. 2018;34:69–79.
Steffens DC. Late-life depression and the prodromes of dementia. JAMA Psychiatry. 2017;74:673–4.
Pickett YR, Ghosh S, Rohs A, Kennedy GJ, Bruce ML, Lyness JM. Healthcare use among older primary care patients with minor depression. Am J Geriatr Psychiatry. 2014;22:207–10.
Rodríguez MR, Nuevo R, Chatterji S, Ayuso-Mateos JL. Definitions and factors associated with subthreshold depressive conditions: A systematic review. BMC Psychiatry. 2012;12. https://doi.org/10.1186/1471-244X-12-181.
Anderson TM, Slade T, Andrews G, Sachdev PS. DSM-IV major depressive episode in the elderly: The relationship between the number and the type of depressive symptoms and impairment. J Affect Disord. 2009;117:55–62.
Prince MJ, Beekman AT, Deeg DJ, Fuhrer R, Kivela SL, Lawlor BA, et al. Depression symptoms in late life assessed using the EURO-D scale. Effect of age, gender and marital status in 14 European centres. Br J Psychiatry. 1999;174:339–45.
Prince MJ, Reischies F, Beekman AT, Fuhrer R, Jonker C, Kivela SL, et al. Development of the EURO-D scale--a European, Union initiative to compare symptoms of depression in 14 European centres. Br J Psychiatry. 1999;174:330–8.
Griffiths-Jones HM. A computerized psychiatric diagnostic system and case nomenclature for elderly subjects: GMS and AGECAT. Psychol Med. 1986;16:89–99.
Gurland B, Golden RR, Teresi JA, Challop J. The SHORT-CARE: An efficient instrument for the assessment of depression, dementia and disability. J Gerontol. 1984;39:166–9.
Åsberg ME, Perris CE, Schalling DE, Sedvall GE. CPRS: development and applications of a psychiatric rating scale. Acta Psychiatr Scand. 1978;57 Suppl 271:S5-69.
Radloff LS. The CES-D scale: A self-report depression scale for research in the general population. Appl Psychol Meas. 1977;1:385–401.
Zung WWK. A self-rating depression scale. Arch Gen Psychiatry. 1965;12:63–70.
Kendler KS. The genealogy of major depression: symptoms and signs of melancholia from 1880 to 1900. Mol Psychiatry. 2017;22:1539–53.
Pagán-Rodríguez R, Pérez S. Depression and self-reported disability among older people in Western Europe. J Aging Health. 2012;24:1131–56.
Guerra M, Ferri C, Llibre J, Prina AM, Prince M. Psychometric properties of EURO-D, a geriatric depression scale: a cross-cultural validation study. BMC Psychiatry. 2015;15:12.
Epskamp S, Borsboom D, Fried EI. Estimating psychological networks and their accuracy: a tutorial paper. Behav Res Methods. 2018;50:195–212.
Raue PJ, Morales KH, Post EP.Bogner HR, Have T Ten, Bruce ML. The Wish to die and 5-year mortality in elderly primary care patients. Am J Geriatr Psychiatry. 2010;18:341–50.
Conwell Y, Duberstein PR, Caine ED. Risk factors for suicide in later life. Biol Psychiatry. 2002;52:193–204.
Large M, Smith G, Sharma S, Nielssen O, Singh SP. Systematic review and meta-analysis of the clinical factors associated with the suicide of psychiatric in-patients. Acta Psychiatr Scand. 2011;124:18–19.
Bogers ICHM, Zuidersma M, Boshuisen ML, Comijs HC, Oude Voshaar RC. The influence of thoughts of death and suicidal ideation on the course of depression in older depressed patients. Int J Geriatr Psychiatry. 2017;32:882–91.
ICHM Bogers, Zuidersma M, Boshuisen ML, Comijs HC, Oude Voshaar RC. Determinants of thoughts of death or suicide in depressed older persons. Int Psychogeriatr. 2013;25:1775–82.
Pompili M, Belvederi Murri M, Patti S, Innamorati M, Lester D, Girardi P, et al. The communication of suicidal intentions: s meta-analysis. Psychol Med. 2016;46:2239–53.
Raue PJ, Sirey JA. NIH public access. Psychiatr Clin North Am. 2012;34:489–500.
Mellqvist Fässberg M, Östling S, Braam AW, Bäckman K, Copeland JRM, Fichter M, et al. Functional disability and death wishes in older Europeans: results from the EURODEP concerted action. Soc Psychiatry Psychiatr Epidemiol. 2014;49:1475–82.
Shah A, Hoxey K, Mayadunne V. Suicidal ideation in acutely medically ill elderly inpatients: prevalence, correlates and longitudinal stability. Int J Geriatr Psychiatry. 2000;15:162–9.
Sanna L, Stuart AL, Pasco JA, Kotowicz MA, Berk M, Girardi P, et al. Suicidal ideation and physical illness: does the link lie with depression? J Affect Disord. 2014;152–4:422–6.
Waern M, Rubenowitz E, Wilhelmson K. Predictors of suicide in the old elderly. Gerontology. 2003;49:328–34.
Palgi Y. Are ongoing cumulative chronic stressors associated with optimism and pessimism in the second half of life? Anxiety Stress Coping. 2013;26:674–89.
Nolen-Hoeksema S, Parker LE, Larson J. Ruminative coping with depressed mood following loss. J Pers Soc Psychol. 1994;67:92–104.
Aziz R, Steffens DC. What are the causes of late-life depression? Psychiatr Clin North Am. 2013;36:497–516.
Schaakxs R, Comijs HC, van der Mast RC, Schoevers RA, Beekman ATF. Penninx BWJH. risk factors for depression: differential across age? Am J Geriatr Psychiatry. 2017;25:966–77.
McKenzie DP, Clarke DM, Forbes AB, Sim MR. Pessimism, worthlessness, anhedonia, and thoughts of death identify DSM-IV major depression in hospitalized, medically ill patients. Psychosomatics. 2010;51:302–11.
Hirsch JK, Walker KL, Chang EC, Lyness JM. Illness burden and symptoms of anxiety in older adults: Optimism and pessimism as moderators. Int Psychogeriatr. 2012;24:1674–83.
Haigh EAP, Bogucki OE, Sigmon ST, Blazer DG. Depression among older adults: a 20-year update on five common myths and misconceptions. Am J Geriatr Psychiatry. 2018;26:107–22.
Gleason OC, Pierce AM, Walker AE, Warnock JK. The two-way relationship between medical illness and late-life depression. Psychiatr Clin North Am. 2013;36:533–44.
Abi Zeid Daou M, Boyd BD, Donahue MJ, Albert K, Taylor WD. Frontocingulate cerebral blood flow and cerebrovascular reactivity associated with antidepressant response in late-life depression. J Affect Disord. 2017;215:103–10.
Morimoto SS, Alexopoulos GS. Cognitive deficits in geriatric depression. clinical correlates and implications for current and future treatment. Psychiatr Clin North Am. 2013;36:517–31.
Diniz BS, Reynolds CF, Sibille E, Lin CW, Tseng G, Lotrich F, et al. Enhanced molecular aging in late-life depression: the senescent-associated secretory phenotype. Am J Geriatr Psychiatry. 2017;25:64–72.
Rutherford BR, Taylor WD, Brown PJ, Sneed JR, Roose SP. Biological aging and the future of geriatric psychiatry. J Gerontol - Ser A Biol Sci Med Sci. 2016;72:343–52.
Belvederi Murri M, Pariante C, Mondelli V, Masotti M, Atti AR, Mellacqua Z, et al. HPA axis and aging in depression: systematic review and meta-analysis. Psychoneuroendocrinology. 2014;41:46–62.
Gordon JA. On being a circuit psychiatrist. Nat Neurosci. 2016;19:1385–6.
Rizvi SJ, Pizzagalli DA, Sproule BA, Kennedy SH. Assessing anhedonia in depression: potentials and pitfalls. Neurosci Biobehav Rev. 2016;65:21–35.
van Stockert S, Haslbeck JMB, Lamers F, BWJH Penninx, Schoevers RA, Fried EI. Depression and (no) inflammation? Using network analysis to examine links between individual depressive symptoms and inflammatory markers. PsyArXiv. 2018. https://doi.org/10.17605/OSF.IO/84SKE.
Kiosses DN, Leon AC, Arean PA. Psychosocial interventions for late-life major depression: evidence-based treatments, predictors of treatment outcomes, and moderators of treatment effects. Psychiatr Clin North Am. 2011;34:377–401.
Fried EI, Epskamp S, Nesse RM, Tuerlinckx F, Borsboom D. What are 'good' depression symptoms? Comparing the centrality of DSM and non-DSM symptoms of depression in a network analysis. J Affect Disord. 2016;189:314-20.
Acknowledgements
The SHARE data collection has been primarily funded by the European Commission through FP5 (QLK6-CT-2001–00360), FP6 (SHARE-I3: RII-CT-2006–062193, COMPARE: CIT5-CT-2005–028857, SHARELIFE: CIT4-CT-2006–028812) and FP7 (SHARE-PREP: N°211909, SHARE-LEAP: N°227822, SHARE M4: N°261982). Additional funding from the German Ministry of Education and Research, the Max Planck Society for the Advancement of Science, the U.S. National Institute of Mental Health (P50 MH113838), National Institute on Aging (U01_AG09740–13S2, P01_AG005842, P01_AG08291, P30_AG12815, R21_AG025169, Y1-AG-4553–01, IAG_BSR06–11, OGHA_04–064, HHSN271201300071C) and from various national funding sources is gratefully acknowledged (see www.share-project.org).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
GSA has been on the speakers’ bureaus of Lundbeck, Otsuka, and Allergan. The other authors declare that they have no conflict of interest.
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Belvederi Murri, M., Amore, M., Respino, M. et al. The symptom network structure of depressive symptoms in late-life: Results from a European population study. Mol Psychiatry 25, 1447–1456 (2020). https://doi.org/10.1038/s41380-018-0232-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41380-018-0232-0
This article is cited by
-
Impact of depressive symptoms on medication adherence in older adults with chronic neurological diseases
BMC Psychiatry (2024)
-
Psychopathological network for early-onset post-stroke depression symptoms
BMC Psychiatry (2023)
-
Maintenance in relationships, satisfaction, jealousy, and violence in young couples: a network analysis
BMC Psychology (2023)
-
The development of depressive symptoms in older adults from a network perspective in the English Longitudinal Study of Ageing
Translational Psychiatry (2023)
-
Associations of the serotonin transporter gene polymorphism, 5-HTTLPR, and adverse life events with late life depression in the elderly Lithuanian population
Scientific Reports (2023)